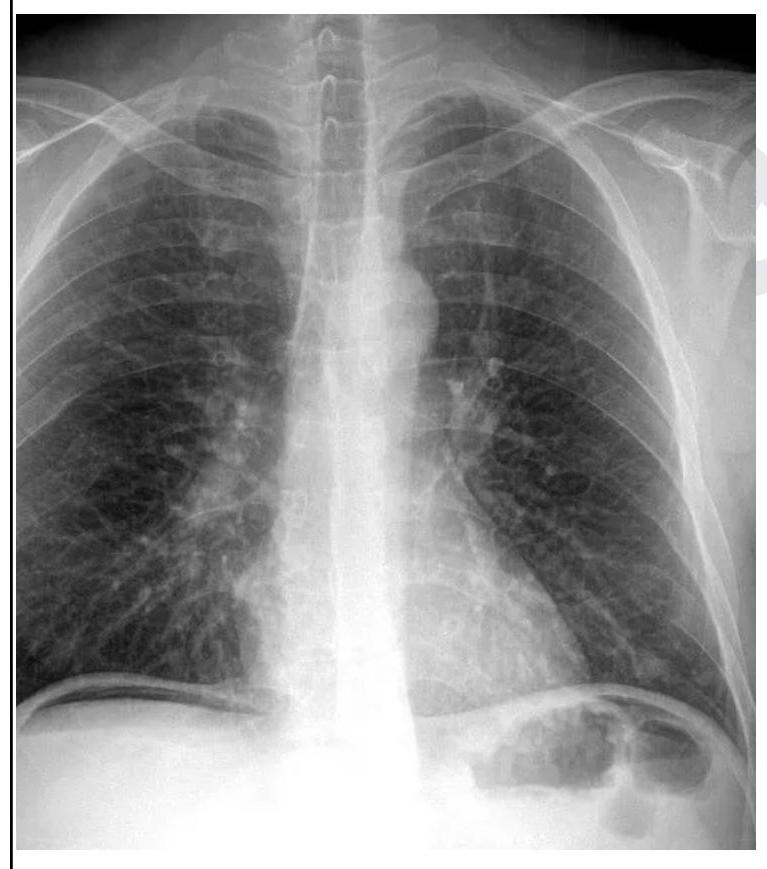
A patient after a road traffic accident presents to the emergency room with difficulty in swallowing and slurred speech. Investigations reveal fractures in the occipitotemporal region. Which of the following areas should be tested in order to find the nerve which is involved?
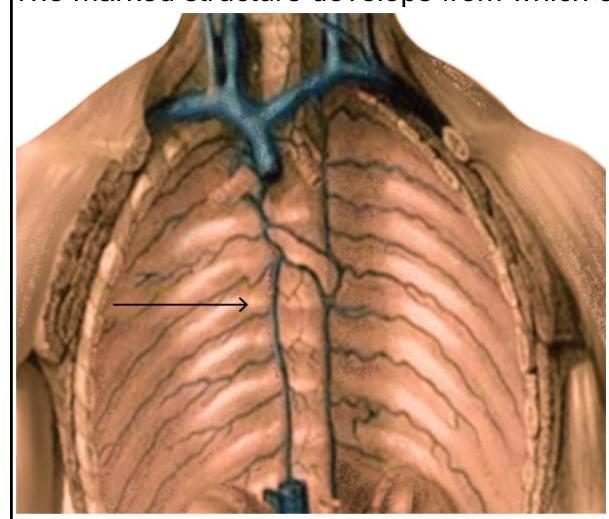
The marked structure develops from which of the following structures?
Inferior thyroid artery supplies which of the following structures? 1. Thyroid 2. Parathyroid 3. Esophagus 4. Thymus