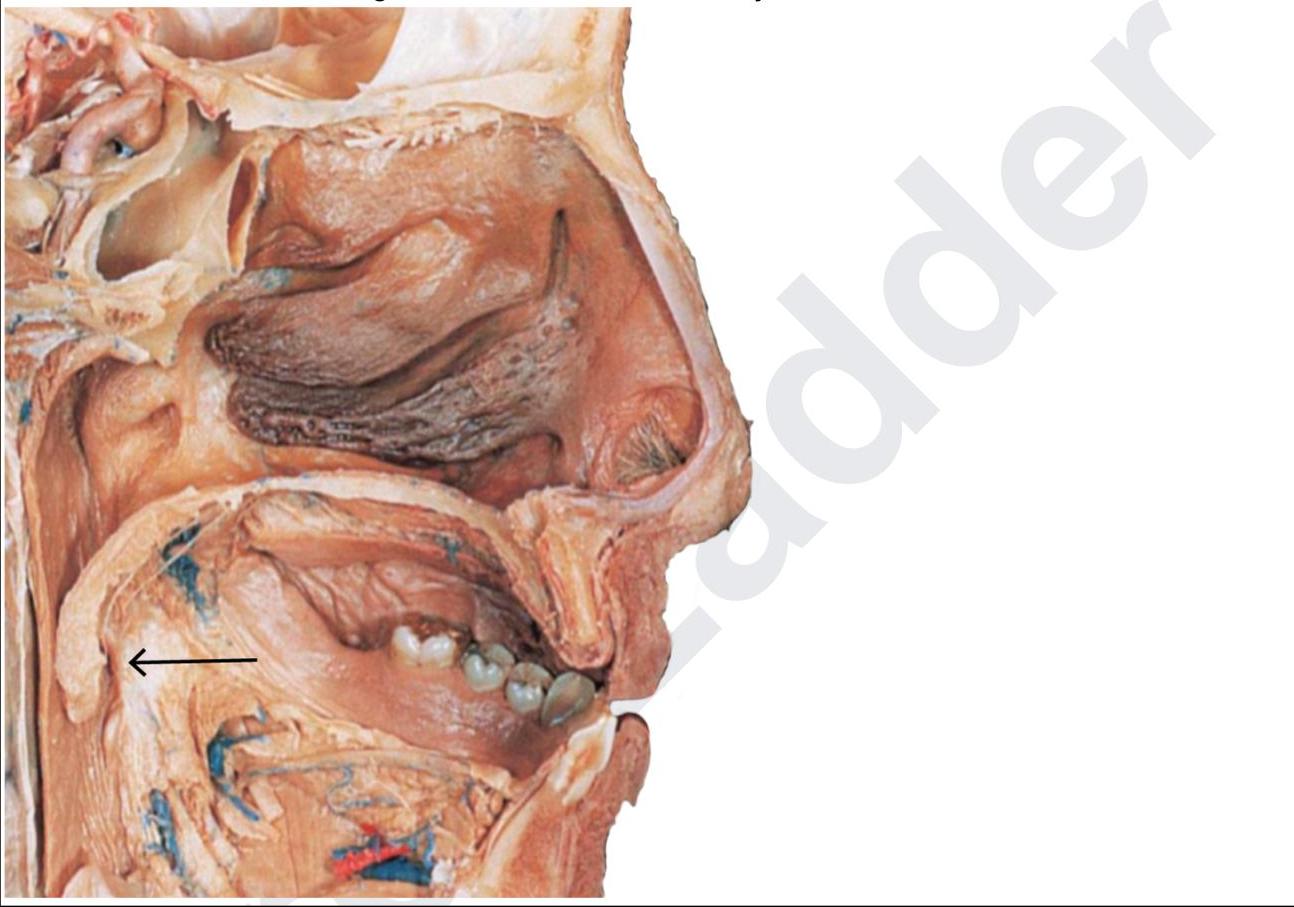
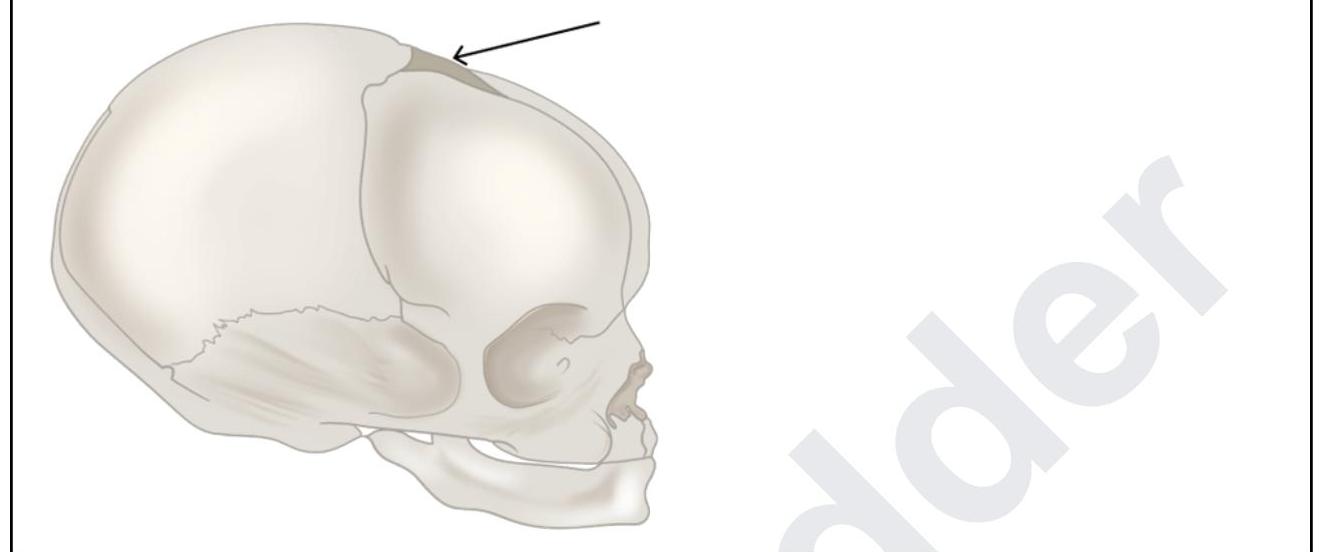
A 6-month-old boy was brought to the casualty with seizures. The pediatrician tries to do CSF sampling. What are the structures punctured by the pediatrician while piercing through the marked structure?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
A 6-month-old boy was brought to the casualty with seizures. The pediatrician tries to do CSF sampling. What are the structures punctured by the pediatrician while piercing through the marked structure?

An HIV positive woman on ART was prescribed ergotamine for a migraine attack 4 days back. She presented with complaints that she is unable to feel her legs from the mid - thigh to her toes, for the past two days. The angiography image is given below. What is the likely diagnosis?
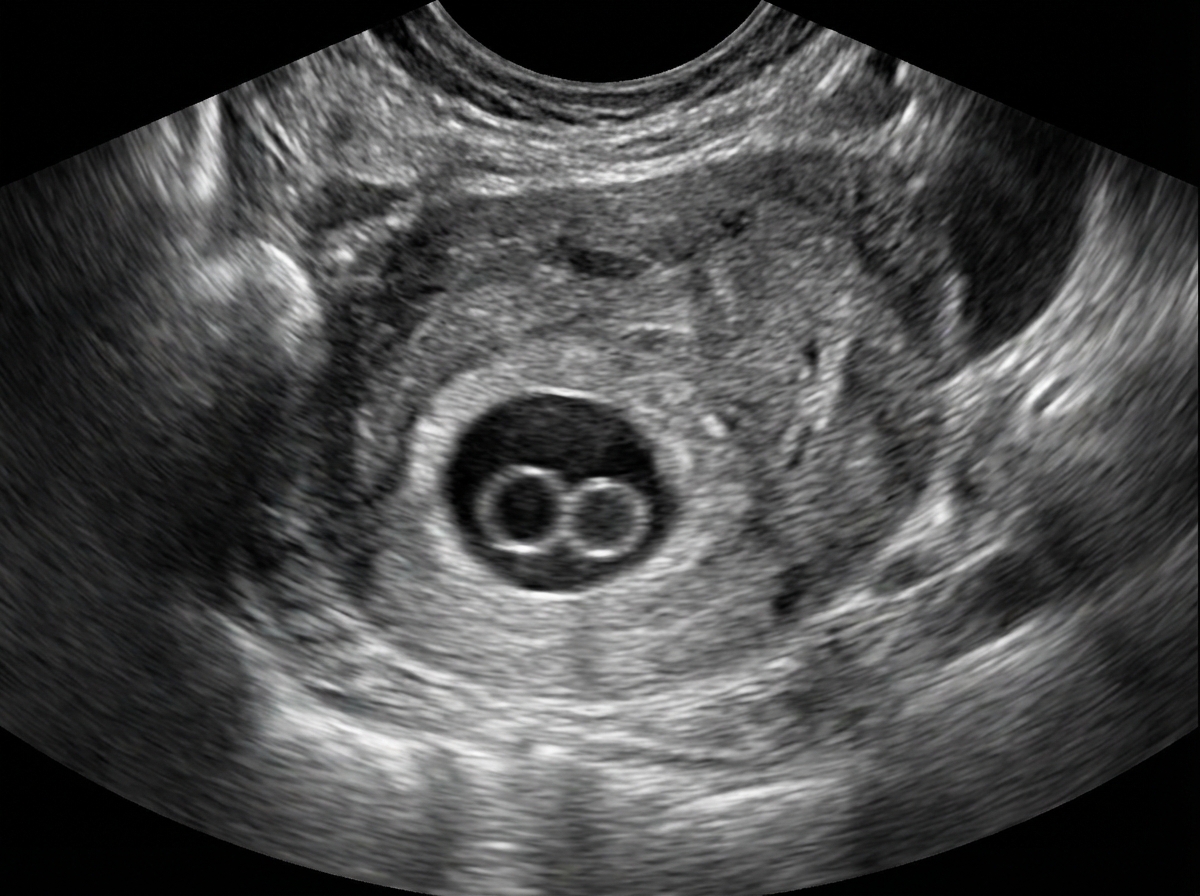
Double bleb sign seen in early pregnancy is due to?
Match the following 1. Hirschsprung's disease 2. Posterior urethral valve 3. Choledochal cyst 4. Intussusception A. Jaundice B. Currant jelly stools C. Distended abdomen D. Oligohydramnios
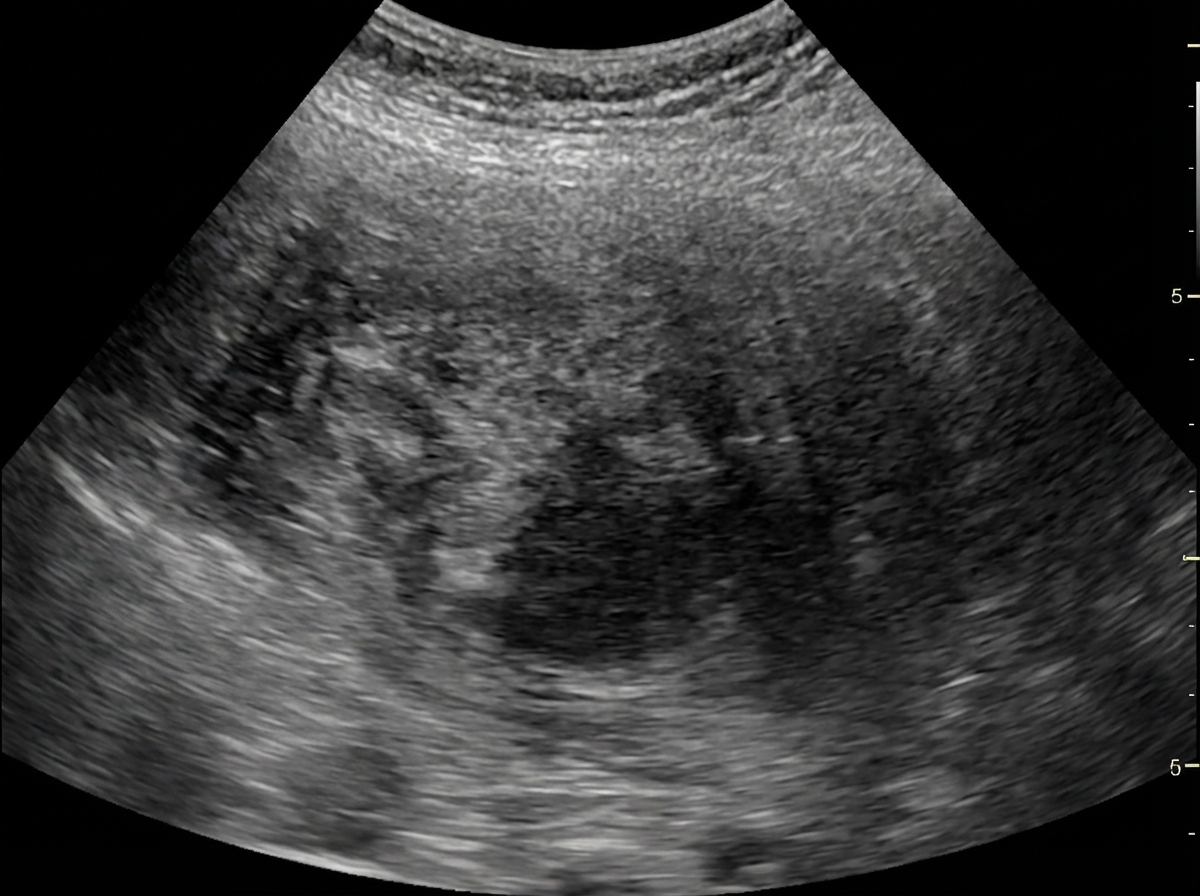
A mother notices a swelling in the abdomen of her 3-year-old child while bathing him. He had a history of hematuria two weeks back, which resolved spontaneously. On examination, a right-sided reniform ballotable mass was found. What is the most appropriate initial investigative approach?
Which of the following is false about the selection of essential drugs?
A patient who was diagnosed with epilepsy was put on retigabine TDS. Now phenytoin is being added. Which of the following changes should be made to retigabine?
A patient with history of ischemic stroke was started on clopidogrel. However, she had another attack of stroke after 6 months. Which of the following is likely to be responsible for the failure of clopidogrel in this patient?
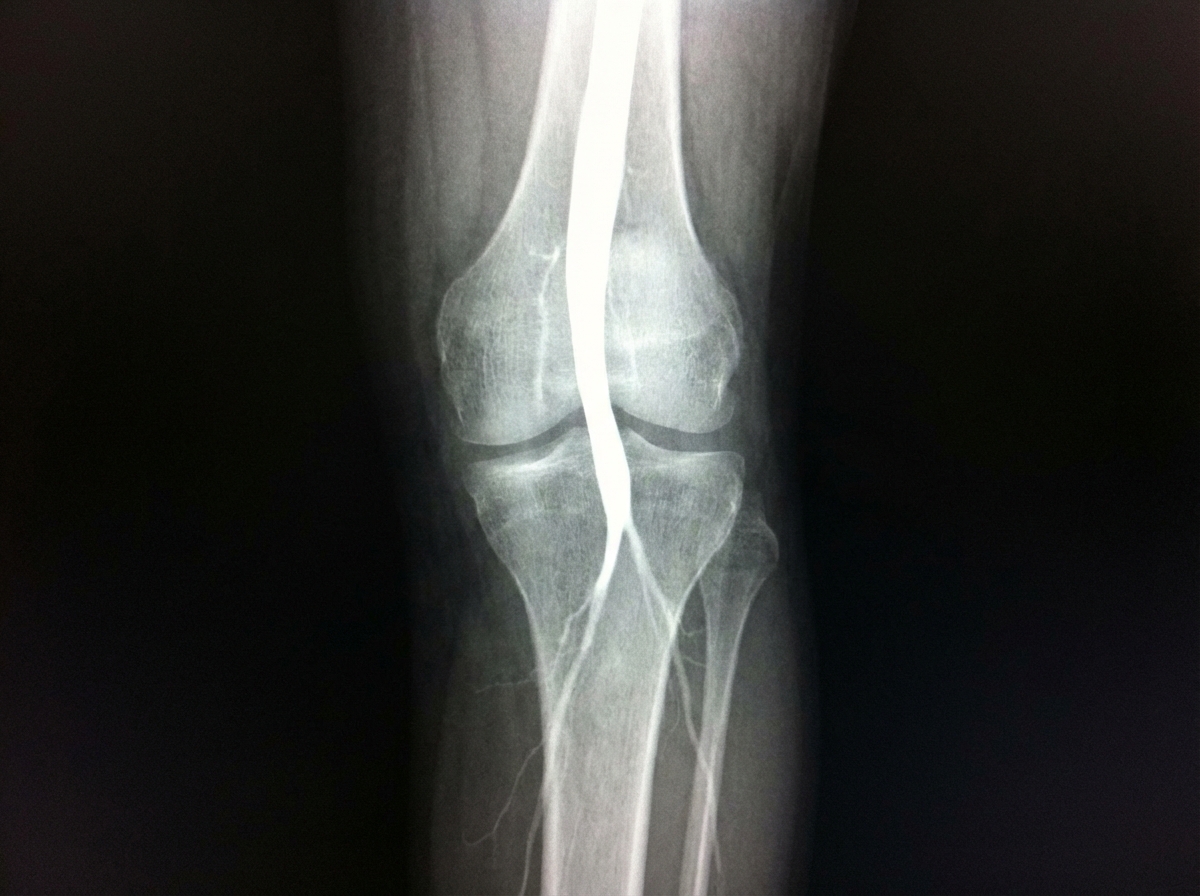
Identify the imaging modality given below.
A 12-year-old presented with fever and difficulty swallowing. He had swelling in the marked region and was advised to undergo tonsillectomy. Post-surgery the gauze continued to soak with blood. Which of the following vessels must have been injured?