INI-CET 2021 — Ophthalmology
3 Previous Year Questions with Answers & Explanations
A 30-year-old female presents with redness and pain in the eye. Examination revealed 38 mm of Hg on IOP, aqueous flare, and corneal precipitates. Which of the following drugs must be avoided for her?
What is the most common route of the spread of retinoblastoma?
Identify the surgical step shown in the image given below
INI-CET 2021 - Ophthalmology INI-CET Practice Questions and MCQs
Question 1: A 30-year-old female presents with redness and pain in the eye. Examination revealed 38 mm of Hg on IOP, aqueous flare, and corneal precipitates. Which of the following drugs must be avoided for her?
- A. Carbonic anhydrase inhibitors
- B. Prostaglandin analogs (Correct Answer)
- C. Mannitol
- D. Beta-blockers
Explanation: ***Prostaglandin analogs*** - **Prostaglandin analogs** are **contraindicated in anterior uveitis** because they can significantly worsen inflammation. - They increase the risk of **cystoid macular edema (CME)** in patients with intraocular inflammation. - Can exacerbate existing **uveitis** and compromise treatment outcomes. - While they effectively lower IOP in non-inflammatory conditions, their pro-inflammatory effects make them unsuitable when aqueous flare and KPs are present. *Carbonic anhydrase inhibitors* - These drugs work by decreasing **aqueous humor production** and are safe and effective for reducing **IOP** in **uveitis**. - They do not exacerbate inflammation and are commonly used in the management of **uveitic glaucoma**. - Available in topical (dorzolamide, brinzolamide) and systemic (acetazolamide) formulations. *Mannitol* - **Mannitol** is an osmotic diuretic used for acute, severe elevations in **IOP**. - It rapidly reduces **IOP** by drawing fluid out of the vitreous and is safe to use in uveitis with elevated pressure. - Its use is typically for short-term, urgent IOP control. *Beta-blockers* - **Beta-blockers** (timolol, betaxolol) reduce **IOP** by decreasing **aqueous humor production**. - They are safe and commonly used to manage **elevated IOP** in uveitic patients. - They do not exacerbate inflammation and are first-line agents for IOP control.
Question 2: What is the most common route of the spread of retinoblastoma?
- A. Hematogenous (Correct Answer)
- B. Optic nerve invasion
- C. Direct invasion
- D. Lymphatic spread
Explanation: ***Correct: Hematogenous*** - **Hematogenous spread** is the most common route of metastatic dissemination in retinoblastoma, occurring when tumor cells invade choroidal blood vessels. - This leads to distant metastases in **bone marrow, bones, liver, and brain** through bloodstream circulation. - Studies of metastatic retinoblastoma show hematogenous spread accounts for the majority of extraocular dissemination patterns. *Incorrect: Optic nerve invasion* - While optic nerve invasion is the **most clinically significant** prognostic factor and provides direct CNS access, it is not the most common route statistically. - Occurs in approximately 20-30% of enucleated eyes and is a critical indicator for adjuvant therapy. - When present, it dramatically worsens prognosis due to leptomeningeal spread potential. *Incorrect: Lymphatic spread* - The globe lacks true lymphatic drainage, making lymphatic spread extremely rare. - Lymphatic involvement only occurs if tumor extends beyond the eye into orbital tissues with lymphatic channels. - Not a primary route of retinoblastoma dissemination. *Incorrect: Direct invasion* - Direct orbital invasion occurs with advanced intraocular tumors breaking through the sclera. - This is a local extension rather than a route of distant metastatic spread. - While serious, it represents local progression rather than the most common dissemination pathway.
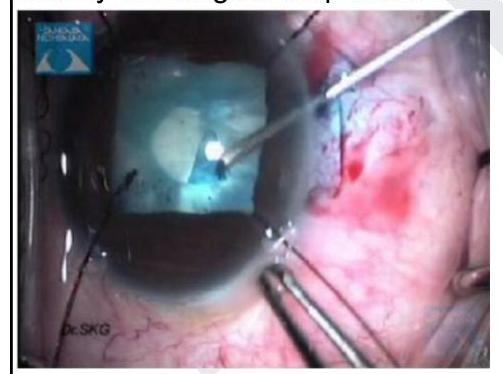
Question 3: Identify the surgical step shown in the image given below
- A. Capsulorrhexis
- B. Hydrodissection
- C. Intraocular lens implantation
- D. Lens aspiration (Correct Answer)
Explanation: ***Lens aspiration*** - The image shows a **phacoemulsification handpiece** (the instrument with the shining tip and central bore tube) actively fragmenting and aspirating the lens material, indicated by the cloudy material being removed. - This step is part of cataract surgery where the cataractous lens material is removed from the eye. *Capsulorrhexis* - This involves creating a **continuous curvilinear tear** in the anterior lens capsule, typically done at the beginning of cataract surgery. - The image does not show a tearing or incising action on the capsule; instead, it depicts material removal. *Hydrodissection* - This step involves injecting a **fluid wave** between the lens capsule and the lens cortex to separate them, facilitating nuclear rotation and removal. - The image depicts the removal of lens material, not the injection of fluid to separate layers. *Intraocular lens implantation* - This step involves inserting the **artificial lens** into the capsular bag after the cataractous lens has been removed. - The visual cues in the image indicate material removal and emulsification, not the insertion of a new lens.