Which of the following can be prevented by transfusing irradiated RBCs?
Which of the following is not likely to be seen in a patient with Paroxysmal Nocturnal Hemoglobinuria (PNH)?
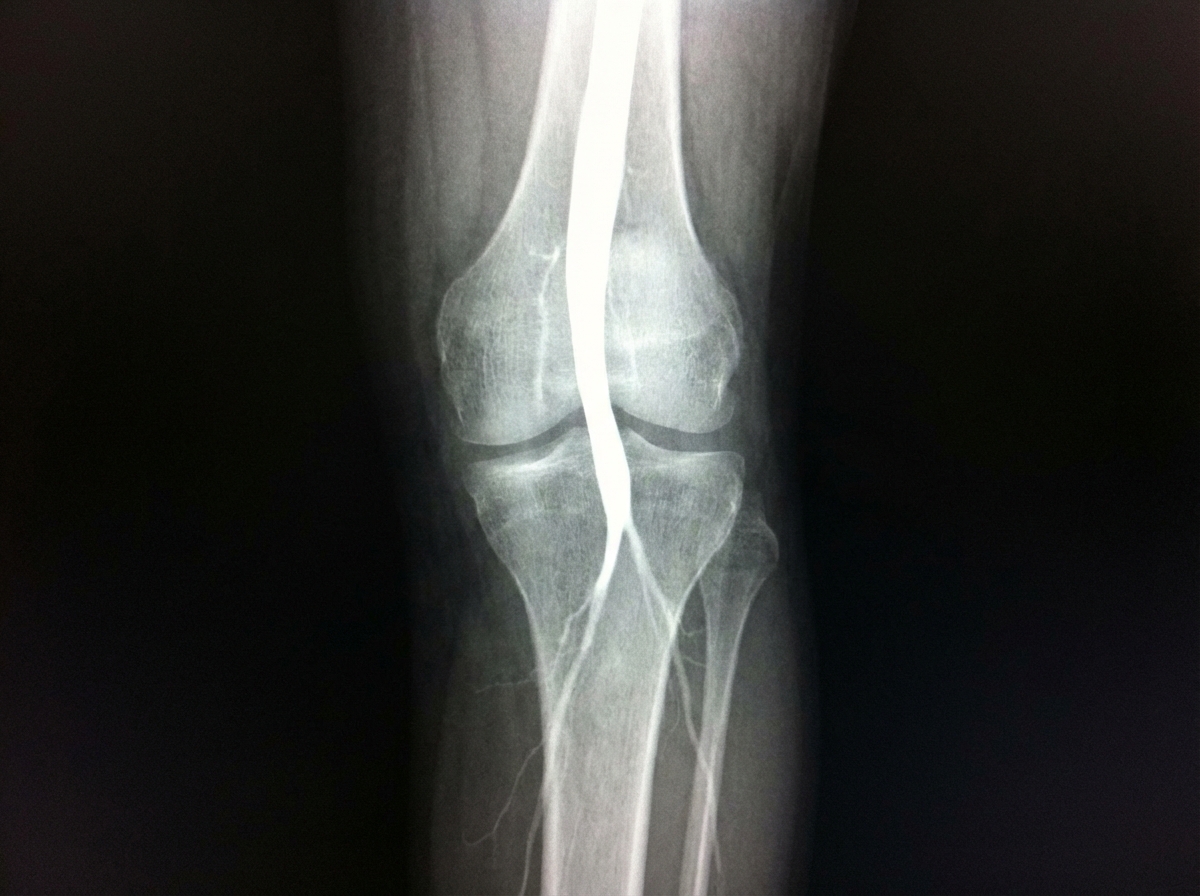
An HIV positive woman on ART was prescribed ergotamine for a migraine attack 4 days back. She presented with complaints that she is unable to feel her legs from the mid - thigh to her toes, for the past two days. The angiography image is given below. What is the likely diagnosis?
A patient admitted after a road traffic accident is put on mechanical ventilation. He opens his eyes on verbal command and moves all four limbs spontaneously. Calculate his GCS.
A 45-year-old male patient presented with a history of bilateral lower limb weakness, which progressed to his upper limbs in a year. On examination, he had weakness in both lower limbs and wasting in the left upper limb. Babinski sign was positive and the deep tendon reflexes were hyperactive. He has no sensory loss or any autonomic dysfunction. What is the likely diagnosis?
A 62-year-old male patient with heart failure is scheduled for a heart transplant. His renal function test is deranged, and haemoglobin is $6 \mathrm{gm} \%$. The physician ordered 2 units of whole blood. Four hours after transfusion, he developed severe respiratory distress. On examination, he is hypoxemic, has tachycardia and his mean arterial pressure is elevated. Which of the following are the best investigations for the above scenario? 1. Chest X-ray 2. Brain natriuretic peptide (BNP) level 3. Absolute neutrophil count 4. Leucocyte antibodies 5. Platelets