INI-CET 2021 — Internal Medicine
16 Previous Year Questions with Answers & Explanations
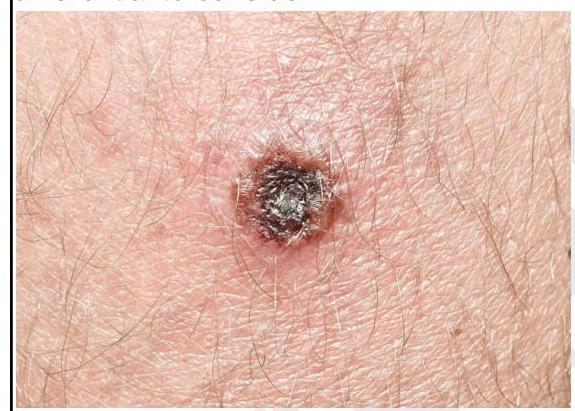
A forest officer develops the lesion as shown in the image. Which of the following is not a differential to consider?
An elderly woman presented with confusion, thirst, and abdominal pain symptoms. On examination, she had pallor and thoracic spine tenderness. X-ray spine showed osteolytic lesions. Her lab investigations showed the following findings. What is the most likely diagnosis? - Hb - 6.9 g/dl
An elderly woman presented with confusion, thirst, and abdominal pain symptoms. On examination, she had pallor and thoracic spine tenderness. X-ray spine showed osteolytic lesions. Her lab investigations showed the following findings. What is the most likely diagnosis? - Hb - 69 g/dl - WBC 4000/cm3 with normal differential count - Serum calcium 13 mg/dl - Creatinine 2.3 mg/dl - Total protein 9 g/dl - Albumin 2.4 g/dl
During the discharge of a COVID patient treated with steroids and remdesivir, which of the following will you inform him about? 1. Repeat RT-PCR after 7 days of discharge 2. Watch for the persistence of Anosmia 3. Watch for headache and nasal discharge 4. Monitor glucose levels 5. Watch for Sinusitis symptoms
A 50-year-old man suddenly developed right-sided weakness and aphasia within 2 hours. His BP recorded was 160/110mmHg and NCCT was clear. What is the next step in management?
Which of the following is not true about syndrome of inappropriate antidiuretic hormone secretion (SIADH)?
Treatment of choice for an acute attack of cluster headache is:
A 35-year-old female patient with class II pulmonary hypertension presents with a negative vasoreactive test. Which of the following is used in the next step of management?
Which of the following drugs is preferred in the management of primary progressive multiple sclerosis?
A 60-year-old male patient with critical mitral stenosis presented with atrial fibrillation. He has a history of multiple episodes of transient ischemic attacks. Which of the following are true regarding preventing stroke in this patient? 1. Only aspirin is given 2. Warfarin is given 3. Direct oral anticoagulants are not indicated 4. Mitral valvotomy should be recommended
INI-CET 2021 - Internal Medicine INI-CET Practice Questions and MCQs
Question 1: A forest officer develops the lesion as shown in the image. Which of the following is not a differential to consider?
- A. Cutaneous anthrax
- B. KFD (Correct Answer)
- C. Scrub typhus
- D. Healing brown recluse spider bite
Explanation: ***KFD*** - **Kyasanur Forest Disease** (KFD) is a viral hemorrhagic fever, but it does **not** typically present with a **skin lesion** or eschar like the one shown. - KFD is characterized by fever, headache, myalgia, and gastrointestinal symptoms, with hemorrhagic manifestations in severe cases, but not a primary cutaneous lesion. *Cutaneous anthrax* - **Cutaneous anthrax** commonly presents as an **eschar**, often with surrounding edema and vesicles, which can resemble the lesion in the image. - Exposure through handling infected animal products or contact with contaminated soil is common, aligning with a forest officer's occupation. *Scrub typhus* - **Scrub typhus** characteristically causes an **eschar** (tache noire) at the bite site of the chigger mite. - The lesion in the image, an ulcer with a central black crust, is highly suggestive of such an eschar seen in rickettsial infections. *Healing brown recluse spider bite* - A **brown recluse spider bite** can cause a **necrotic ulcer** with a central dark eschar as the wound heals, fitting the appearance of the lesion. - The profession of a forest officer increases the likelihood of exposure to spiders in their natural habitat.
Question 2: An elderly woman presented with confusion, thirst, and abdominal pain symptoms. On examination, she had pallor and thoracic spine tenderness. X-ray spine showed osteolytic lesions. Her lab investigations showed the following findings. What is the most likely diagnosis? - Hb - 6.9 g/dl
- A. Vertebral compression fracture
- B. Metastatic carcinoma
- C. Osteoporosis
- D. Multiple myeloma (Correct Answer)
Explanation: ***Multiple myeloma*** - The combination of **osteolytic lesions** (bone pain, tenderness), **hypercalcemia** (confusion, thirst), **anemia** (Hb 69 g/dl, pallor), and **renal insufficiency** (confusion, thirst from dehydration) is highly suggestive of **multiple myeloma** [1]. - This plasma cell malignancy leads to excessive production of monoclonal antibodies and bone destruction [1]. *Vertebral compression fracture* - While **thoracic spine tenderness** and osteolytic lesions could be a component, it doesn't fully explain the systemic symptoms such as **anemia**, **confusion**, and **hypercalcemia**. - A simple compression fracture would not account for the profound **anemia** (Hb 69 g/dl) seen in this patient. *Metastatic carcinoma* - While metastatic carcinoma can cause **osteolytic lesions**, **anemia**, and sometimes **hypercalcemia**, the specific constellation of symptoms, particularly the severity of anemia and rapid progression, makes **multiple myeloma** a more fitting diagnosis. - Absence of primary tumor indicates that it is not a metastatic disease [1]. *Osteoporosis* - **Osteoporosis** can cause vertebral fractures and bone pain but typically does not lead to **osteolytic lesions**, **severe anemia**, or **hypercalcemia** [2]. - The bone changes in osteoporosis are primarily due to decreased bone density, not destructive lesions [2].
Question 3: An elderly woman presented with confusion, thirst, and abdominal pain symptoms. On examination, she had pallor and thoracic spine tenderness. X-ray spine showed osteolytic lesions. Her lab investigations showed the following findings. What is the most likely diagnosis? - Hb - 69 g/dl - WBC 4000/cm3 with normal differential count - Serum calcium 13 mg/dl - Creatinine 2.3 mg/dl - Total protein 9 g/dl - Albumin 2.4 g/dl
- A. Milk alkali syndrome
- B. Metastatic breast cancer
- C. Multiple myeloma (Correct Answer)
- D. Primary hyperparathyroidism
Explanation: ***Multiple myeloma*** - The combination of **anemia** (Hb - 69 g/dl), **renal insufficiency** (creatinine 2.3 mg/dl), **hypercalcemia** (serum calcium 13 mg/dl), and **osteolytic lesions** on X-ray spine is highly characteristic of multiple myeloma, often remembered by the acronym **CRAB** (Calcium elevation, Renal failure, Anemia, Bone lesions) [1]. - The **elevated total protein** (9 g/dl) with a relatively low albumin (2.4 g/dl) suggests a **paraproteinemia**, a hallmark of multiple myeloma caused by the overproduction of monoclonal antibodies [1]. *Milk alkali syndrome* - This syndrome is characterized by **hypercalcemia**, **metabolic alkalosis**, and **renal insufficiency**, usually due to excessive intake of calcium and absorbable alkali. While hypercalcemia and renal dysfunction are present, the absence of metabolic alkalosis and the presence of osteolytic lesions make this less likely. - It does not typically cause **anemia** or **osteolytic lesions**, and the high total protein is not a feature. *Metastatic breast cancer* - While metastatic breast cancer can cause **osteolytic lesions** and **hypercalcemia**, it typically presents with a primary breast mass or a history of breast cancer [2]. - The **elevated total protein** with a narrowed albumin-globulin gap is not a characteristic feature of metastatic breast cancer unless it also involves multiple myeloma, which is less common. *Primary hyperparathyroidism* - This condition is characterized by **elevated parathyroid hormone (PTH)** leading to **hypercalcemia** and, in severe cases, bone disease (osteitis fibrosa cystica). - Unlike the patient's presentation, primary hyperparathyroidism typically does not cause **anemia** or such pronounced **renal failure** (though kidney stones are common), nor does it lead to significantly elevated total protein with a low albumin.
Question 4: During the discharge of a COVID patient treated with steroids and remdesivir, which of the following will you inform him about? 1. Repeat RT-PCR after 7 days of discharge 2. Watch for the persistence of Anosmia 3. Watch for headache and nasal discharge 4. Monitor glucose levels 5. Watch for Sinusitis symptoms
- A. 1,3 and 4
- B. 3,4 and 5 (Correct Answer)
- C. 2,3 and 4
- D. 1,2,3,4 and 5
Explanation: **3, 4, and 5** - For patients treated with **steroids**, it is crucial to monitor **glucose levels** due to the potential for steroid-induced hyperglycemia [1]. - Symptoms like **headache** and **nasal discharge** (and by extension **sinusitis symptoms**) could indicate conditions like **mucormycosis**, a serious fungal infection seen in immunocompromised COVID-19 patients, especially those having received steroids. *1, 3, and 4* - A **repeat RT-PCR after 7 days** of discharge is generally not recommended as per current guidelines, as viral shedding can persist without infectivity. - While monitoring for headache, nasal discharge, and glucose levels is appropriate, omitting the direct vigilance for **sinusitis symptoms** is less comprehensive. *2, 3, and 4* - While **anosmia** (loss of smell) can persist post-COVID, it is primarily a lingering symptom of the infection itself and typically resolves spontaneously, not usually requiring specific discharge instructions for monitoring its persistence to prevent complications. - The focus should be on new or worsening symptoms that might indicate post-COVID complications or secondary infections. *1, 2, 3, 4, and 5* - Including **repeat RT-PCR** and solely "watch for the persistence of Anosmia" without emphasizing resolution or specific actions makes this option less pertinent for discharge advice. - The priority for discharge instructions should be preventable complications and warning signs of serious conditions.
Question 5: A 50-year-old man suddenly developed right-sided weakness and aphasia within 2 hours. His BP recorded was 160/110mmHg and NCCT was clear. What is the next step in management?
- A. IV thrombolysis (Correct Answer)
- B. MRI Brain
- C. Antihypertensive therapy
- D. CT Angiography
Explanation: ***IV thrombolysis*** - This patient presents with **acute ischemic stroke** symptoms (right-sided weakness and aphasia) with an onset within 4.5 hours of symptom onset, making them a candidate for **IV thrombolysis** [1]. - A **clear NCCT** of the head within this timeframe rules out **hemorrhage**, confirming the safety profile for thrombolytic administration under appropriate blood pressure control [1]. *MRI Brain* - While an MRI brain is highly sensitive for **detecting acute ischemic changes**, it is typically not the initial emergent imaging choice in suspected stroke due to its longer acquisition time and limited availability compared to CT [1]. - The primary goal in acute stroke evaluation is to **rule out hemorrhage** quickly to determine eligibility for thrombolytics, which NCCT achieves effectively [1]. *Antihypertensive therapy* - While the patient's **blood pressure is elevated**, aggressive lowering is generally avoided in acute ischemic stroke unless it exceeds 220/120 mmHg (for non-thrombolysis candidates) or 185/110 mmHg (for thrombolysis candidates). - Rapidly lowering blood pressure can **reduce cerebral perfusion pressure** and worsen ischemic injury in the acute setting due to impaired autoregulation. *CT Angiography* - **CT angiography** can help identify large vessel occlusions that might be amenable to **endovascular thrombectomy** [1]. - However, the immediate priority after a clear NCCT and within the narrow time window is to initiate IV thrombolysis if no contraindications exist, as it provides systemic thrombolysis. CTA is usually performed concurrently or immediately after initial thrombolysis consideration/initiation if endovascular therapy is also being considered [1].
Question 6: Which of the following is not true about syndrome of inappropriate antidiuretic hormone secretion (SIADH)?
- A. Patient can be clinically euvolemic to hypovolemic
- B. Urine osmolality >100 mOsm/kg
- C. Urinary sodium <20 mEq/L (Correct Answer)
- D. Serum sodium <135 mEq/L
Explanation: ***Urinary sodium <20 mEq/L*** - In **SIADH**, the inappropriate secretion of ADH leads to increased water reabsorption, causing **dilutional hyponatremia**. [1] - The kidneys respond by trying to excrete excess water and dilute the urine, leading to **increased urinary sodium concentration**, typically *greater than* 20 mEq/L. *Patient can be clinically euvolemic to hypovolemic* - Patients with **SIADH** are typically **euvolemic** because the excess water is retained intracellularly and extracellularly in balanced proportions, without significant edema or dehydration. [1] - While fluid retention occurs, it's not enough to cause significant clinical volume overload, and they are never truly hypovolemic. *Urine osmolality >100 mOsm/kg* - In **SIADH**, the continued action of **ADH** despite hypotonicity results in the reabsorption of water, leading to the production of **concentrated urine**. [1] - This elevated urine osmolality, typically **greater than 100 mOsm/kg**, indicates an inability to adequately excrete free water. [1] *Serum sodium <135 mEq/L* - **SIADH** is defined by **hyponatremia**, a serum sodium concentration **below 135 mEq/L**, due to the excessive retention of water. - This dilutes the extracellular fluid, leading to a reduction in the relative concentration of sodium.
Question 7: Treatment of choice for an acute attack of cluster headache is:
- A. Subcutaneous sumatriptan
- B. 100 % oxygen at 6 L / minute (Correct Answer)
- C. Oral sumatriptan
- D. Prophylactic verapamil
Explanation: The treatment of choice for an acute attack of cluster headache is 100% oxygen at 6 L / minute. High-flow 100% oxygen delivered via a non-rebreather mask for 15-20 minutes is a highly effective and rapid treatment for acute cluster headache attacks [1]. Its mechanism of action is thought to involve cerebral vasoconstriction, which helps to alleviate the pain. While subcutaneous sumatriptan is effective for acute cluster headache [1], its use is limited to 2 injections per 24 hours due to the risk of coronary vasoconstriction. Oxygen therapy is generally preferred as a first-line acute treatment due to its rapid onset and favorable side-effect profile. Oral sumatriptan has a slower onset of action compared to subcutaneous administration and oxygen, making it less suitable for the rapid relief required for an acute cluster headache attack. The rapid and severe nature of cluster headache pain necessitates treatments with a quick therapeutic effect [1]. Verapamil is a calcium channel blocker used as a prophylactic treatment to prevent cluster headache attacks [1], not to treat an acute attack. Prophylactic medications are taken regularly to reduce the frequency and severity of attacks, whereas abortive treatments are used during an attack.
Question 8: A 35-year-old female patient with class II pulmonary hypertension presents with a negative vasoreactive test. Which of the following is used in the next step of management?
- A. Epoprostenol
- B. Nifedipine
- C. Iloprost
- D. Ambrisentan (Correct Answer)
Explanation: ***Ambrisentan*** - For patients with **Class II pulmonary hypertension** and a **negative vasoreactive test**, initial management typically involves **endothelin receptor antagonists (ERAs)**, phosphodiesterase-5 inhibitors (PDE5i), or guanylate cyclase stimulators (GCS). - **Ambrisentan** is an ERA that improves exercise capacity and delays clinical worsening in these patients. *Epoprostenol* - This is a **parenteral prostacyclin analog** reserved for patients with more severe pulmonary hypertension (WHO Class III or IV) or those who fail initial oral therapy. - Due to its continuous intravenous infusion, **high cost**, and side effects, it is not a first-line treatment for Class II PH. *Nifedipine* - **Calcium channel blockers (CCBs)** like nifedipine are only indicated for patients with a **positive vasoreactive test**, as they selectively dilate pulmonary arteries in these individuals. - For patients with a negative vasoreactive test, CCBs are **ineffective** and can be harmful due to systemic vasodilation causing hypotension. *Iloprost* - **Iloprost** is an inhaled prostacyclin analog used for patients with moderate to severe pulmonary hypertension (WHO Class III or IV), often in combination with other therapies. [1] - Its **inhalation route** and frequent dosing make it less practical for initial management of Class II disease compared to oral agents.
Question 9: Which of the following drugs is preferred in the management of primary progressive multiple sclerosis?
- A. Natalizumab
- B. Ocrelizumab (Correct Answer)
- C. Alemtuzumab
- D. Fingolimod
Explanation: ***Ocrelizumab*** - **Ocrelizumab** is the first and only FDA-approved disease-modifying therapy for **primary progressive multiple sclerosis (PPMS)**, demonstrating a reduction in disability progression. - It is a **monoclonal antibody** that selectively targets CD20-positive B cells, believed to play a critical role in the pathogenesis of MS. *Natalizumab* - **Natalizumab** is approved for **relapsing-remitting multiple sclerosis (RRMS)**, not primary progressive MS [1]. - It works by blocking the migration of immune cells into the **central nervous system**, but carries a risk of **progressive multifocal leukoencephalopathy (PML)**. *Alemtuzumab* - **Alemtuzumab** is used for **relapsing forms of MS**, particularly in patients who have had an inadequate response to other MS drugs [1]. - It is known for its durable efficacy but also its significant side effects, including **autoimmune conditions** and **infusion reactions**. *Fingolimod* - **Fingolimod** is an oral medication approved for **relapsing forms of MS**, but not for primary progressive MS [1]. - It acts by trapping lymphocytes in the **lymph nodes**, preventing them from entering the central nervous system.
Question 10: A 60-year-old male patient with critical mitral stenosis presented with atrial fibrillation. He has a history of multiple episodes of transient ischemic attacks. Which of the following are true regarding preventing stroke in this patient? 1. Only aspirin is given 2. Warfarin is given 3. Direct oral anticoagulants are not indicated 4. Mitral valvotomy should be recommended
- A. 1 only
- B. 1,2,3 and 4
- C. 2,3 and 4
- D. 2 and 3 (Correct Answer)
Explanation: ***2 and 3*** - In patients with **mitral stenosis** and **atrial fibrillation**, **warfarin** is the recommended anticoagulant for stroke prevention due to its efficacy in preventing thrombus formation in the left atrium [1]. - **Direct oral anticoagulants (DOACs)** are generally **contraindicated** in patients with moderate to severe mitral stenosis, as their effectiveness and safety in this specific population have not been established. *1 only* - **Aspirin monotherapy** is insufficient for stroke prevention in patients with **atrial fibrillation** and **mitral stenosis**, as their risk of thromboembolism is significantly higher [1]. - Aspirin has a lower efficacy compared to warfarin in preventing cardioembolic strokes originating from left atrial thrombi in this demographic. *1,2,3 and 4* - While warfarin is indicated and DOACs are not, recommending **mitral valvotomy** should be considered in conjunction with anticoagulation, but it is not the sole or primary measure for acute stroke prevention [2]. - The combination of all four statements is incorrect because DOACs are contraindicated, and aspirin alone is inadequate. *2,3 and 4* - Although **warfarin** is indicated and **DOACs** are not, recommending **mitral valvotomy** is a therapeutic intervention for the underlying structural heart disease, not a direct acute stroke prevention medication [2]. - Valvotomy improves hemodynamics and may reduce future thrombus risk, but immediate stroke prevention heavily relies on effective anticoagulation [2].