INI-CET 2021 — Anesthesiology
4 Previous Year Questions with Answers & Explanations
In conventional oxygen therapy, which device will deliver the highest FiO2?
A 60 year old male patient was undergoing laparoscopic cholecystectomy. During the surgery, a sudden drop in EtCO2 to 8 mmHg was noted. His SpO2 became 90%, his blood pressure dropped to 80/50 mmHg, and peak airway pressure was 18 cm of H2O. What is the diagnosis?
Which nerve is targeted in the nasociliary nerve block?
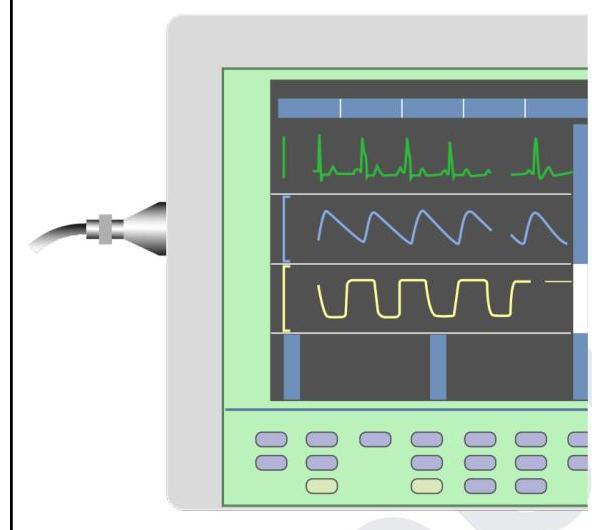
You are in the operating room and notice the tracing in yellow colour on this device. What does it indicate?
INI-CET 2021 - Anesthesiology INI-CET Practice Questions and MCQs
Question 1: In conventional oxygen therapy, which device will deliver the highest FiO2?
- A. Hudson mask
- B. Venturi mask
- C. Non rebreathing mask (Correct Answer)
- D. Nasal cannula
Explanation: **Non rebreathing mask** - This device features a **one-way valve** between the mask and the reservoir bag, preventing exhaled air from mixing with fresh oxygen. This allows for the delivery of the **highest possible FiO2** among conventional oxygen therapy devices, often up to 90-100%. - The **reservoir bag** ensures a continuous supply of high-concentration oxygen during inspiration, maximizing the amount of oxygen inhaled. *Hudson mask* - Also known as a **simple face mask**, it delivers a moderate FiO2 (40-60%) at flow rates of 5-10 L/min. - The open ports on the sides allow for mixing of room air with oxygen, making it less efficient for delivering very high oxygen concentrations. *Venturi mask* - This device uses the Venturi principle to deliver a **precise and consistent FiO2** by entraining room air with oxygen. - While it provides controlled oxygen delivery, its maximum FiO2 typically ranges from 24-60%, which is lower than a non-rebreathing mask. *Nasal cannula* - The nasal cannula delivers a relatively low FiO2 (24-44%) at flow rates of 1-6 L/min. - It is designed for **low-flow oxygen delivery** and is not suitable for patients requiring high concentrations of oxygen.
Question 2: A 60 year old male patient was undergoing laparoscopic cholecystectomy. During the surgery, a sudden drop in EtCO2 to 8 mmHg was noted. His SpO2 became 90%, his blood pressure dropped to 80/50 mmHg, and peak airway pressure was 18 cm of H2O. What is the diagnosis?
- A. Anaphylaxis
- B. Malignant hyperthermia
- C. Gas embolism (Correct Answer)
- D. Pneumothorax
Explanation: ***Gas embolism*** - A sudden drop in **EtCO2** to 8 mmHg, **hypotension**, and **hypoxemia** during laparoscopic surgery are classic signs of a gas embolism, often from insufflated CO2 entering the bloodstream. - The drop in EtCO2 is due to a sudden decrease in pulmonary blood flow, preventing CO2 from reaching the lungs for exhalation. *Anaphylaxis* - While anaphylaxis can cause hypotension and hypoxemia, it typically presents with **bronchospasm** (increased peak airway pressure), **tachycardia**, and skin manifestations like **urticaria** or angioedema, which are not explicitly mentioned. - Anaphylaxis does not typically cause a drastic, sudden drop in EtCO2 to such low levels as seen with a gas embolism. *Malignant hyperthermia* - This condition is characterized by a rapid and sustained increase in **EtCO2**, **tachycardia**, muscle rigidity, and hyperthermia, which is the opposite of the EtCO2 findings here. - Malignant hyperthermia would lead to a significant elevation in metabolic CO2 production, not a sudden drop in EtCO2. *Pneumothorax* - A pneumothorax would typically present with **increased peak airway pressures**, **hypoxia**, and **hypotension**, but the EtCO2 would likely initially rise or remain stable before dropping due to decreased ventilation, not an acute drop to 8 mmHg. - The primary physiological issue in pneumothorax is lung collapse, leading to ventilation-perfusion mismatch, but not directly causing a sudden near-absence of exhaled CO2 in this manner.
Question 3: Which nerve is targeted in the nasociliary nerve block?
- A. Greater palatine nerve
- B. Sphenopalatine nerve
- C. Anterior ethmoidal nerve
- D. Nasociliary nerve (Correct Answer)
Explanation: ***Nasociliary nerve*** - A nasociliary nerve block specifically targets the **nasociliary nerve** itself. - This block is used to anesthetize the sensory innervation of structures supplied by the nasociliary nerve, such as parts of the **nasal cavity**, **eyeball**, and **skin of the nose**. *Greater palatine nerve* - The **greater palatine nerve** supplies sensation to the posterior hard palate and is targeted in a **greater palatine nerve block**. - This nerve is a branch of the **maxillary nerve** and is primarily involved in dental and palatal anesthesia. *Sphenopalatine nerve* - The **sphenopalatine nerve**, or pterygopalatine ganglion, contains sensory fibers for the nasal cavity, palate, and pharynx, and its block is distinct from a nasociliary block. - A **sphenopalatine ganglion block** is mainly used for conditions like cluster headaches and facial pain, not for direct eyeball sensation. *Anterior ethmoidal nerve* - The **anterior ethmoidal nerve** is a branch of the nasociliary nerve, but a nasociliary nerve block targets the main trunk, which includes all its branches. - While the anterior ethmoidal nerve supplies the anterior part of the nasal septum and lateral wall, it is a **component** of the nasociliary innervation rather than the sole target.
Question 4: You are in the operating room and notice the tracing in yellow colour on this device. What does it indicate?
- A. O2 pressure in exhaled air
- B. Capnography (Correct Answer)
- C. O2 pressure in inhaled air
- D. Airway pressure
Explanation: ***Capnography*** - The yellow tracing displays a waveform that is characteristic of a **capnogram**, which measures the concentration of **carbon dioxide (CO2)** in the expired breath over time. - The rectangular shape with a sudden rise, plateau, and rapid fall is typical of the **CO2 waveform** during a respiratory cycle. *O2 pressure in exhaled air* - While oxygen levels can be monitored, the characteristic waveform shown with its distinct plateau phase is specific to **carbon dioxide** measurement. - Oxygen monitoring provides different types of waveforms or numerical values, such as **pulsus oximetry**, which shows oxygen saturation. *O2 pressure in inhaled air* - Monitoring devices typically display **inspired oxygen concentration (FiO2)** as a numerical value rather than a waveform. - The waveform shown is indicative of gas exchange dynamics during **exhalation**, not inhalation. *Airway pressure* - Airway pressure tracings typically show a waveform that correlates with the **inspiratory and expiratory phases** of breathing, indicating the pressure within the airway. - However, the specific shape and plateau of the waveform in yellow are distinct from typical **airway pressure** curves and are characteristic of CO2.