INI-CET 2021
151 Previous Year Questions with Answers & Explanations
Anesthesiology
2 questionsIn conventional oxygen therapy, which device will deliver the highest FiO2?
A 60 year old male patient was undergoing laparoscopic cholecystectomy. During the surgery, a sudden drop in EtCO2 to 8 mmHg was noted. His SpO2 became 90%, his blood pressure dropped to 80/50 mmHg, and peak airway pressure was 18 cm of H2O. What is the diagnosis?
INI-CET 2021 - Anesthesiology INI-CET Practice Questions and MCQs
Question 1: In conventional oxygen therapy, which device will deliver the highest FiO2?
- A. Hudson mask
- B. Venturi mask
- C. Non rebreathing mask (Correct Answer)
- D. Nasal cannula
Explanation: **Non rebreathing mask** - This device features a **one-way valve** between the mask and the reservoir bag, preventing exhaled air from mixing with fresh oxygen. This allows for the delivery of the **highest possible FiO2** among conventional oxygen therapy devices, often up to 90-100%. - The **reservoir bag** ensures a continuous supply of high-concentration oxygen during inspiration, maximizing the amount of oxygen inhaled. *Hudson mask* - Also known as a **simple face mask**, it delivers a moderate FiO2 (40-60%) at flow rates of 5-10 L/min. - The open ports on the sides allow for mixing of room air with oxygen, making it less efficient for delivering very high oxygen concentrations. *Venturi mask* - This device uses the Venturi principle to deliver a **precise and consistent FiO2** by entraining room air with oxygen. - While it provides controlled oxygen delivery, its maximum FiO2 typically ranges from 24-60%, which is lower than a non-rebreathing mask. *Nasal cannula* - The nasal cannula delivers a relatively low FiO2 (24-44%) at flow rates of 1-6 L/min. - It is designed for **low-flow oxygen delivery** and is not suitable for patients requiring high concentrations of oxygen.
Question 2: A 60 year old male patient was undergoing laparoscopic cholecystectomy. During the surgery, a sudden drop in EtCO2 to 8 mmHg was noted. His SpO2 became 90%, his blood pressure dropped to 80/50 mmHg, and peak airway pressure was 18 cm of H2O. What is the diagnosis?
- A. Anaphylaxis
- B. Malignant hyperthermia
- C. Gas embolism (Correct Answer)
- D. Pneumothorax
Explanation: ***Gas embolism*** - A sudden drop in **EtCO2** to 8 mmHg, **hypotension**, and **hypoxemia** during laparoscopic surgery are classic signs of a gas embolism, often from insufflated CO2 entering the bloodstream. - The drop in EtCO2 is due to a sudden decrease in pulmonary blood flow, preventing CO2 from reaching the lungs for exhalation. *Anaphylaxis* - While anaphylaxis can cause hypotension and hypoxemia, it typically presents with **bronchospasm** (increased peak airway pressure), **tachycardia**, and skin manifestations like **urticaria** or angioedema, which are not explicitly mentioned. - Anaphylaxis does not typically cause a drastic, sudden drop in EtCO2 to such low levels as seen with a gas embolism. *Malignant hyperthermia* - This condition is characterized by a rapid and sustained increase in **EtCO2**, **tachycardia**, muscle rigidity, and hyperthermia, which is the opposite of the EtCO2 findings here. - Malignant hyperthermia would lead to a significant elevation in metabolic CO2 production, not a sudden drop in EtCO2. *Pneumothorax* - A pneumothorax would typically present with **increased peak airway pressures**, **hypoxia**, and **hypotension**, but the EtCO2 would likely initially rise or remain stable before dropping due to decreased ventilation, not an acute drop to 8 mmHg. - The primary physiological issue in pneumothorax is lung collapse, leading to ventilation-perfusion mismatch, but not directly causing a sudden near-absence of exhaled CO2 in this manner.
Biochemistry
7 questionsMethyl-tetrahydrofolate (5-methyl-THF) gets accumulated in deficiency of which of the following?
Which of the following molecular analysis methods is used to detect RNA?
Glycated hemoglobin (HbA1c) is best measured using?
Which of the following options is false in a patient with advanced liver disease?
Which of the following is not a substrate for glucose formation?
What is the repair mechanism associated with CRISPR-cas9?
Which of the following is not amphipathic?
INI-CET 2021 - Biochemistry INI-CET Practice Questions and MCQs
Question 1: Methyl-tetrahydrofolate (5-methyl-THF) gets accumulated in deficiency of which of the following?
- A. Vitamin B12 (Cobalamin) (Correct Answer)
- B. Vitamin B2 (Riboflavin)
- C. Vitamin B1 (Thiamine)
- D. Vitamin B6 (Pyridoxine)
Explanation: ***Vitamin B12 (Cobalamin)*** - A deficiency in **Vitamin B12** (cobalamin) leads to the accumulation of **5-methyl-tetrahydrofolate (5-methyl-THF)** due to the **"folate trap"** hypothesis. - This occurs because B12 is a cofactor for **methionine synthase**, which converts 5-methyl-THF back to tetrahydrofolate (THF), a necessary step for DNA synthesis and other one-carbon metabolism reactions. - Without B12, folate remains trapped in the methyl form and cannot be utilized for other essential reactions. *Vitamin B2 (Riboflavin)* - **Vitamin B2** (riboflavin) is a precursor for **FAD** and **FMN**, essential coenzymes in various redox reactions in the electron transport chain and other metabolic pathways. - Its deficiency typically presents as **cheilosis**, glossitis, and angular stomatitis, but does not cause methyl-THF accumulation. *Vitamin B1 (Thiamine)* - **Vitamin B1** (thiamine) is a cofactor for enzymes like **pyruvate dehydrogenase** and **alpha-ketoglutarate dehydrogenase** in carbohydrate metabolism. - Its deficiency causes **Beriberi** (wet, dry, or Wernicke-Korsakoff syndrome), affecting the cardiovascular and nervous systems, but does not affect folate metabolism. *Vitamin B6 (Pyridoxine)* - **Vitamin B6** (pyridoxine) is a coenzyme for many metabolic reactions, particularly in amino acid metabolism and neurotransmitter synthesis. - Deficiency can lead to **sideroblastic anemia**, neurological symptoms, and dermatitis, but does not cause methyl-THF accumulation.
Question 2: Which of the following molecular analysis methods is used to detect RNA?
- A. Western blot
- B. G banding
- C. RT-PCR (Correct Answer)
- D. Sanger's method
Explanation: ***RT-PCR*** - **Reverse transcriptase polymerase chain reaction (RT-PCR)** is a molecular method that first converts **RNA into complementary DNA (cDNA)** using reverse transcriptase before amplification via PCR. - This technique is commonly used to detect and quantify specific **RNA sequences**, such as viral RNA or gene expression levels. *Western blot* - **Western blot** is a laboratory technique used to detect specific **proteins** in a sample. - It involves separating proteins by size using gel electrophoresis, transferring them to a membrane, and then detecting the target protein using specific antibodies. *G banding* - **G banding** is a cytogenetic technique used to produce a visible **karyotype** by staining condensed chromosomes. - This method is primarily used to detect large-scale structural changes in chromosomes, not to detect RNA. *Sanger's method* - **Sanger's method**, also known as **dideoxy sequencing**, is a DNA sequencing technique. - It is used to determine the exact order of **nucleotides within a DNA molecule**, not to detect RNA directly.
Question 3: Glycated hemoglobin (HbA1c) is best measured using?
- A. Isoelectric focusing
- B. Affinity chromatography
- C. Electrophoresis
- D. Ion exchange chromatography (Correct Answer)
Explanation: ***Ion exchange chromatography*** - This method separates hemoglobin variants based on their **charge differences** due to the glucose molecule attached to HbA1c. - It is a highly sensitive and specific method for quantifying HbA1c, widely used in clinical laboratories. *Isoelectric focusing* - This technique separates molecules based on their **isoelectric point (pI)**, the pH at which they have no net charge. - While it can differentiate some hemoglobin variants, it is generally **less efficient and more complex** for routine HbA1c measurement compared to ion exchange chromatography. *Affinity chromatography* - This method separates molecules based on their **specific binding affinity** to a ligand immobilized on a stationary phase. - While it has been explored for HbA1c measurement, it is **not the most commonly used** or preferred method due to potential interferences and cost compared to ion exchange chromatography. *Electrophoresis* - This technique separates molecules based on their **charge and size** in an electric field. - While it can separate major hemoglobin variants, it has **lower resolution and accuracy** for routine HbA1c quantification compared to more specialized chromatographic methods, making it less ideal for precise measurement.
Question 4: Which of the following options is false in a patient with advanced liver disease?
- A. Decreased ATP synthesis
- B. Hyperammonemia
- C. Increased synthesis of glutamine and glutamate from alpha-ketoglutarate
- D. Increased oxidative decarboxylation of alpha-ketoglutarate (Correct Answer)
Explanation: ***Increased oxidative decarboxylation of alpha-ketoglutarate*** - In advanced liver disease, **hepatic encephalopathy** is a common complication due to the liver's inability to detoxify **ammonia**. - Alpha-ketoglutarate is crucial for detoxifying ammonia into glutamate and then glutamine, processes that involve reductive amination and **ATP consumption**, not increased oxidative decarboxylation. *Decreased ATP synthesis* - Advanced liver disease impairs various metabolic functions, including those of the **mitochondria**, leading to decreased ATP production. - This reduction in **energy reserves** affects numerous cellular processes and organ functions. *Hyperammonemia* - The liver is responsible for detoxifying **ammonia** into urea via the **urea cycle**. - In advanced liver disease, the impaired function of the liver leads to a buildup of ammonia in the blood, resulting in **hyperammonemia**. *Increased synthesis of glutamine and glutamate from alpha-ketoglutarate* - In the brain, when the liver fails to detoxify ammonia, **astrocytes** attempt to convert excess ammonia into **glutamine** using **alpha-ketoglutarate**. - This process is a compensatory mechanism to reduce ammonia toxicity, but it depletes alpha-ketoglutarate, which is a key intermediate in the **Krebs cycle**, leading to **cerebral energy deficits**.
Question 5: Which of the following is not a substrate for glucose formation?
- A. Lactate
- B. Glycerol
- C. Alanine
- D. Acetyl coenzyme A (Correct Answer)
Explanation: ***Acetyl coenzyme A*** - **Acetyl CoA** cannot be converted to glucose because the two carbons from the acetyl group are lost as carbon dioxide in the **Krebs cycle**, making a net synthesis of glucose impossible. - The irreversible nature of the **pyruvate dehydrogenase complex** prevents the conversion of Acetyl CoA back to **pyruvate**, which is a crucial step for gluconeogenesis. *Lactate* - **Lactate** is a major substrate for gluconeogenesis, particularly during exercise and fasting, via the **Cori cycle**. - **Lactate dehydrogenase** converts lactate to **pyruvate**, which can then enter the gluconeogenic pathway. *Glycerol* - **Glycerol**, derived from triglyceride breakdown, enters gluconeogenesis by being converted to **glycerol-3-phosphate** and then to **dihydroxyacetone phosphate (DHAP)**. - DHAP is an intermediate in glycolysis and gluconeogenesis, allowing for its conversion to glucose. *Alanine* - **Alanine** is a **glucogenic amino acid** that can be transaminated to **pyruvate**. - **Pyruvate** can then proceed through the gluconeogenic pathway to synthesize glucose, especially during prolonged fasting.
Question 6: What is the repair mechanism associated with CRISPR-cas9?
- A. Mismatch repair
- B. Non-homologous end joining (Correct Answer)
- C. Nucleotide excision repair
- D. Base excision repair
Explanation: ***Non-homologous end joining*** - **CRISPR-Cas9** creates a **double-strand break (DSB)** in DNA, which is primarily repaired by **non-homologous end joining (NHEJ)**. - **NHEJ** is the **predominant repair pathway** in most cells, accounting for 60-90% of DSB repairs. - **NHEJ** is an error-prone repair mechanism that ligates the broken ends directly, often leading to small **insertions or deletions (indels)** causing gene knockout. - Note: **Homology-directed repair (HDR)** is another CRISPR-associated mechanism used for precise editing when a donor template is provided, but **NHEJ is the primary endogenous repair pathway**. *Mismatch repair* - This mechanism corrects errors that arise during **DNA replication**, such as incorrect base pairing. - It does not repair **double-strand breaks** induced by CRISPR-Cas9. *Nucleotide excision repair* - This pathway removes **bulky DNA adducts** and lesions, such as those caused by UV radiation. - It is not involved in repairing **CRISPR-Cas9 induced double-strand breaks**. *Base excision repair* - This mechanism corrects **damaged or modified bases**, typically single base changes, without affecting the sugar-phosphate backbone significantly. - It handles different types of DNA damage than the **double-strand breaks** generated by CRISPR-Cas9.
Question 7: Which of the following is not amphipathic?
- A. Triglycerides (Correct Answer)
- B. Sphingolipids
- C. Glycolipids
- D. Phosphoglycerol
Explanation: ***Triglycerides*** - Triglycerides are composed of a **glycerol backbone** esterified to three fatty acids, making them entirely **hydrophobic** and thus not amphipathic. - They serve primarily as **energy storage** molecules and do not form membranes because they lack a polar head group. *Sphingolipids* - Sphingolipids are amphipathic because they contain a **hydrophilic polar head group** (e.g., phosphocholine or a sugar) and two **hydrophobic tails** derived from a fatty acid and the sphingosine backbone. - This dual nature allows them to be fundamental components of **cell membranes**. *Glycolipids* - Glycolipids are characterized by a **carbohydrate head group** attached to a lipid moiety, rendering them amphipathic. - The sugar portion is **hydrophilic**, while the lipid portion (e.g., ceramide) is **hydrophobic**, enabling them to participate in cell recognition and membrane stability. *Phosphoglycerol* - Phosphoglycerol (more commonly referred to as **glycerophospholipids**) are amphipathic, consisting of a **glycerol backbone**, two fatty acid tails, and a **phosphate group** often linked to an alcohol. - The **phosphate and alcohol group** form the hydrophilic head, and the **fatty acid tails** form the hydrophobic region, making them crucial for lipid bilayers.
Internal Medicine
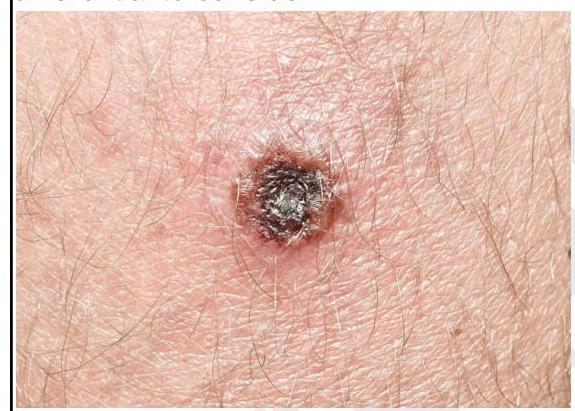
1 questionsA forest officer develops the lesion as shown in the image. Which of the following is not a differential to consider?
INI-CET 2021 - Internal Medicine INI-CET Practice Questions and MCQs
Question 1: A forest officer develops the lesion as shown in the image. Which of the following is not a differential to consider?
- A. Cutaneous anthrax
- B. KFD (Correct Answer)
- C. Scrub typhus
- D. Healing brown recluse spider bite
Explanation: ***KFD*** - **Kyasanur Forest Disease** (KFD) is a viral hemorrhagic fever, but it does **not** typically present with a **skin lesion** or eschar like the one shown. - KFD is characterized by fever, headache, myalgia, and gastrointestinal symptoms, with hemorrhagic manifestations in severe cases, but not a primary cutaneous lesion. *Cutaneous anthrax* - **Cutaneous anthrax** commonly presents as an **eschar**, often with surrounding edema and vesicles, which can resemble the lesion in the image. - Exposure through handling infected animal products or contact with contaminated soil is common, aligning with a forest officer's occupation. *Scrub typhus* - **Scrub typhus** characteristically causes an **eschar** (tache noire) at the bite site of the chigger mite. - The lesion in the image, an ulcer with a central black crust, is highly suggestive of such an eschar seen in rickettsial infections. *Healing brown recluse spider bite* - A **brown recluse spider bite** can cause a **necrotic ulcer** with a central dark eschar as the wound heals, fitting the appearance of the lesion. - The profession of a forest officer increases the likelihood of exposure to spiders in their natural habitat.
About INI-CET 2021 Questions
This page contains 151 questions from the INI-CET 2021 paper, organised across 19 subjects for focused practice. Every question comes with the correct answer and a detailed explanation to help you understand the underlying concept. Subject-wise organisation lets you target specific areas and identify which topics carried the most weight in this particular year.
Practising year-wise papers is essential for understanding how the INI-CET exam evolves — you can spot trending topics, gauge difficulty shifts, and benchmark your readiness against a real paper. To take your preparation further, download the Oncourse app for AI-driven performance insights, spaced repetition of questions you got wrong, and a personalised study plan built around your INI-CET goals.