FMGE 2018 — Pediatrics
9 Previous Year Questions with Answers & Explanations
Most common cardiac abnormality in Noonan syndrome is:-
Compression ventilation ratio in case of Neonatal CPR:
A 6-year-old child presents with hepatosplenomegaly and generalized lymphadenopathy along with fever. The child developed a rash after being administered ampicillin. What could be the possible diagnosis?
Most common cause of bacterial meningitis in post-neonatal period:
Dose of vitamin A for an 18 month old baby, with keratomalacia, weighing 10 kg is?
Most common cause of cholestatic jaundice in newborn is
A 6-year-old child is brought with high fever with rigors for 5 days with pain in right hypochondrium. On examination, the patient is anicteric and tenderness is noted in right upper quadrant. What is the best investigation for this case?
A newborn loses maximum heat from:
A 6-year-old child is brought with the following lesion. He can develop lesions in which organ in future?
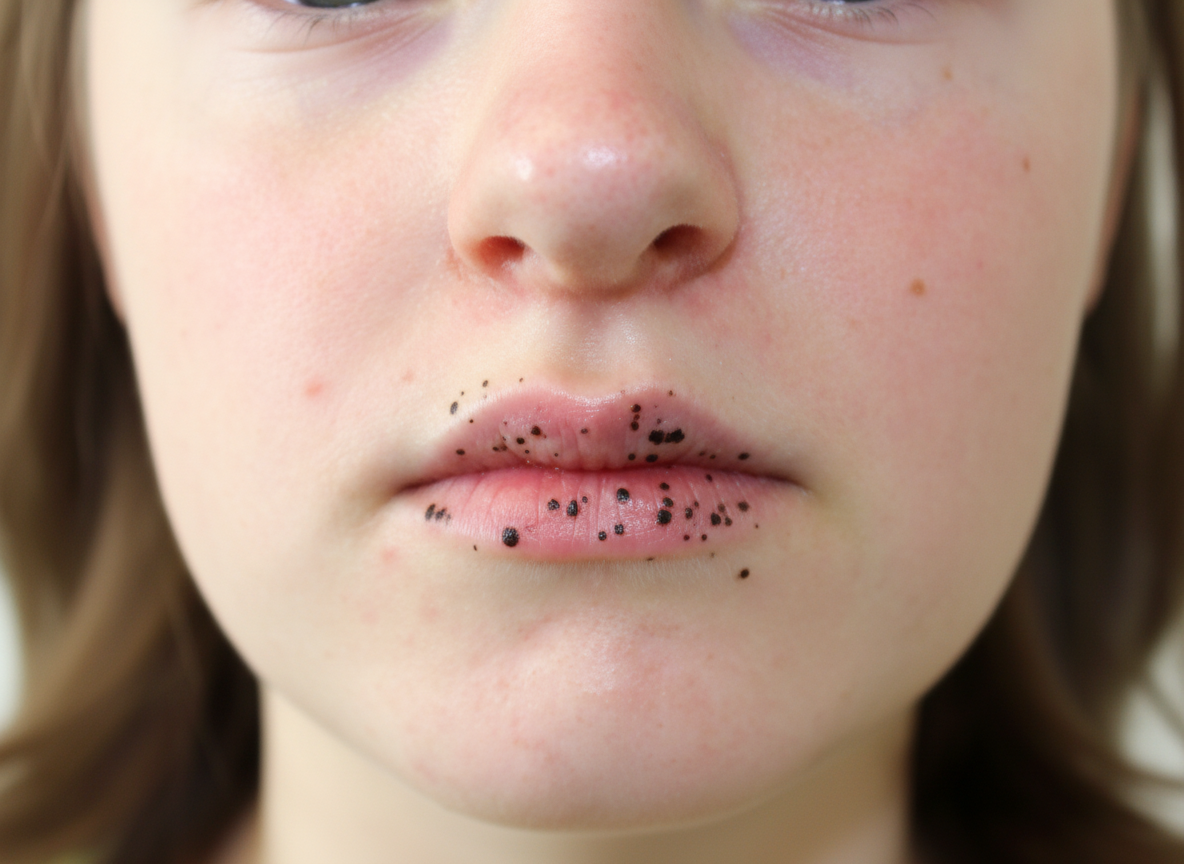
FMGE 2018 - Pediatrics FMGE Practice Questions and MCQs
Question 1: Most common cardiac abnormality in Noonan syndrome is:-
- A. Pulmonary stenosis (Correct Answer)
- B. Atrial septal defect
- C. Tetralogy of Fallot
- D. Ventricular septal defect
Explanation: ***Pulmonary stenosis*** - **Valvular pulmonary stenosis**, particularly a dysplastic pulmonary valve, is the **most common cardiac defect** found in individuals with Noonan syndrome. - This condition can lead to an obstruction of blood flow from the right ventricle into the **pulmonary artery**. *Atrial septal defect* - While **atrial septal defects (ASDs)** can occur in Noonan syndrome, they are less common than pulmonary stenosis. - ASDs are characterized by a hole in the septum separating the two upper chambers of the heart. *Tetralogy of Fallot* - **Tetralogy of Fallot** is a complex congenital heart defect involving four specific abnormalities, which is not the most common cardiac finding in Noonan syndrome. - It is typically associated with a different set of genetic syndromes or occurs sporadically. *Ventricular septal defect* - **Ventricular septal defects (VSDs)** are also observed in some cases of Noonan syndrome but are less prevalent than pulmonary stenosis. - VSDs involve a hole in the wall separating the heart's lower two chambers.
Question 2: Compression ventilation ratio in case of Neonatal CPR:
- A. 30:2
- B. 100:8
- C. 3:1 (Correct Answer)
- D. 15:2
Explanation: ***3:1*** - In **neonatal CPR**, a compression to ventilation ratio of **3 compressions per 1 breath** is recommended. This ratio prioritizes ventilation due to the most common cause of cardiac arrest in neonates being **hypoxia**. - This ratio aims to deliver sufficient oxygen while maintaining adequate cardiac output for the unique physiology of newborns. *30:2* - A 30:2 ratio is generally recommended for **adult CPR** when a single rescuer is present, as adults often have initial cardiac etiologies. - This ratio would provide insufficient ventilations for a neonate whose primary arrest cause is typically respiratory. *100:8* - This ratio is not a standard recommendation for any age group in Cardiopulmonary Resuscitation guidelines. - It would lead to an imbalance, offering a disproportionately high number of compressions relative to ventilations, which is not optimal for neonatal resuscitation. *15:2* - A 15:2 ratio is typically recommended for **pediatric CPR** when two or more rescuers are present. - While closer to the neonatal requirement for ventilation, it still does not provide the immediate and frequent ventilations needed for neonates.
Question 3: A 6-year-old child presents with hepatosplenomegaly and generalized lymphadenopathy along with fever. The child developed a rash after being administered ampicillin. What could be the possible diagnosis?
- A. Kawasaki disease
- B. Scarlet fever
- C. Infectious mononucleosis (Correct Answer)
- D. HIV infection
Explanation: ***Infectious mononucleosis*** - The combination of **hepatosplenomegaly**, **generalized lymphadenopathy**, and fever in a child is highly suggestive of infectious mononucleosis, typically caused by the **Epstein-Barr virus (EBV)**. - A characteristic feature is the development of a **maculopapular rash** following the administration of ampicillin or amoxicillin. *Kawasaki disease* - Characterized by **fever**, generalized rash, lymphadenopathy, and mucocutaneous inflammation, but typically does not involve significant **hepatosplenomegaly**. - The rash in Kawasaki disease is not typically triggered by **ampicillin**. *Scarlet fever* - Caused by a **Streptococcus pyogenes** infection and presents with a characteristic **sandpaper-like rash**, **strawberry tongue**, and fever. - It usually does not involve significant **hepatosplenomegaly** or a rash specifically induced by ampicillin. *HIV infection* - While HIV can cause **generalized lymphadenopathy** and **hepatosplenomegaly**, especially in children, the sudden onset of a rash specifically after ampicillin administration is not a hallmark of acute or chronic HIV infection. - Other opportunistic infections and **growth failure** would likely be present in advanced HIV.
Question 4: Most common cause of bacterial meningitis in post-neonatal period:
- A. Mycobacterium tuberculosis
- B. Staphylococcus aureus
- C. Streptococcus pneumoniae (Correct Answer)
- D. Klebsiella
Explanation: ***Streptococcus pneumoniae*** - *S. pneumoniae* is the most common cause of **bacterial meningitis** in the post-neonatal period (1 month to 1 year of age), particularly in regions with high vaccination rates against Hib. - Its polysaccharide capsule and ability to evade the immune system contribute to its virulence in causing **central nervous system infections**. - Accounts for approximately 40-50% of bacterial meningitis cases in this age group. *Mycobacterium tuberculosis* - While it can cause **tuberculous meningitis**, this is a less common form of meningitis, typically with a more **insidious onset** and often associated with immunosuppression or endemic areas. - Represents a chronic form of meningitis rather than acute bacterial meningitis. *Staphylococcus aureus* - *S. aureus* meningitis typically occurs in specific contexts such as **post-neurosurgery**, following head trauma, or in patients with indwelling catheters or bacteremia. - It is not the most frequent pathogen in community-acquired meningitis in infants. *Klebsiella* - **Klebsiella pneumoniae** can cause meningitis, especially in **neonates** (first 28 days of life), immunocompromised individuals, or patients with healthcare-associated infections. - However, it is not the most common cause of meningitis in the post-neonatal period.
Question 5: Dose of vitamin A for an 18 month old baby, with keratomalacia, weighing 10 kg is?
- A. 1,00,000 IU
- B. 50,000 IU
- C. 5,00,000 IU
- D. 2,00,000 IU (Correct Answer)
Explanation: **2,00,000 IU** - For children 12 months of age and older with **keratomalacia** due to vitamin A deficiency, the recommended dose is **200,000 IU** orally, given immediately. - This dose should be repeated the next day and again after four weeks to replenish stores and prevent recurrence. *1,00,000 IU* - This dose is typically recommended for infants **aged 6 to 11 months** with **clinical vitamin A deficiency**, including keratomalacia. - It is insufficient for an 18-month-old child with active keratomalacia. *50,000 IU* - This dose is usually given to infants **under 6 months** of age with clinical signs of **vitamin A deficiency**. - It is too low for an 18-month-old baby with keratomalacia. *5,00,000 IU* - This dose is excessively high and potentially toxic for an 18-month-old child. - Vitamin A toxicity can lead to adverse effects, including **increased intracranial pressure** and liver damage.
Question 6: Most common cause of cholestatic jaundice in newborn is
- A. Neonatal hepatitis
- B. Physiological
- C. Choledochal cyst
- D. Biliary atresia (Correct Answer)
Explanation: ***Biliary atresia*** - This is the **most common cause of cholestatic jaundice** requiring surgical intervention in otherwise healthy full-term newborns. - It involves the **progressive obliteration or absence of extrahepatic bile ducts**, leading to bile flow obstruction, conjugated hyperbilirubinemia, and ultimately liver damage if untreated. - Incidence is approximately **1 in 10,000-15,000 live births**, and early diagnosis (before 60 days of age) is critical for optimal surgical outcomes with Kasai portoenterostomy. *Neonatal hepatitis* - While it can cause **cholestatic jaundice** in newborns, biliary atresia remains the leading **surgical cause** requiring urgent intervention. - It describes a diverse group of conditions leading to inflammation of the liver, which can be **idiopathic** or caused by infections (TORCH), metabolic disorders, or genetic conditions. - Unlike biliary atresia, neonatal hepatitis may improve with supportive care and treatment of underlying causes. *Physiological* - **Physiological jaundice** is characterized by **unconjugated hyperbilirubinemia** and is typically transient, resolving without intervention. - It does not cause cholestatic jaundice, which involves **conjugated hyperbilirubinemia** and indicates an underlying pathological process. *Choledochal cyst* - A **choledochal cyst** is a congenital dilation of the bile ducts and can cause cholestatic jaundice, but it is a **rarer cause** compared to biliary atresia. - Symptoms often include an **abdominal mass**, pain, and recurrent cholangitis, which may differ from the typical presentation of early biliary atresia.
Question 7: A 6-year-old child is brought with high fever with rigors for 5 days with pain in right hypochondrium. On examination, the patient is anicteric and tenderness is noted in right upper quadrant. What is the best investigation for this case?
- A. SGOT/LFT
- B. CECT
- C. Serology
- D. USG (Correct Answer)
Explanation: ***USG*** - A **ultrasound** is the preferred initial investigation, especially in children, for evaluating abdominal pain in the **right hypochondrium** with fever. - It can effectively identify common causes like **cholecystitis**, **hepatitis**, or **liver abscess**, which fit the clinical presentation. *SGOT/LFT* - **Liver function tests (LFTs)** like SGOT/AST and SGPT/ALT provide information about liver inflammation or damage but do not help localize the pathology. - They are useful for assessing liver function but are not the primary diagnostic tool to identify the cause of the pain or fever. *CECT* - **Contrast-enhanced computed tomography (CECT)** is a more advanced imaging technique, often used after initial screening or when ultrasound findings are inconclusive. - It involves radiation exposure and contrast risks, making it less suitable as a first-line investigation for a child with these symptoms. *Serology* - **Serological tests** detect antibodies or antigens related to specific infections (e.g., viral hepatitis) but do not provide immediate anatomical information. - While they can confirm an infectious cause, they cannot identify the source of the pain or rule out other non-infectious pathologies immediately.
Question 8: A newborn loses maximum heat from:
- A. Head (Correct Answer)
- B. Abdomen
- C. Neck
- D. Palms & soles
Explanation: ***Head*** - Newborns have a **relatively large head surface area** compared to their total body surface area. - The head also has a rich **blood supply** and lacks subcutaneous fat for insulation, contributing to significant heat loss through **convection and radiation**. *Abdomen* - While the abdomen contributes to heat loss, it is covered by clothing and has a more proportionate surface area to mass ratio compared to the head, making it a **less significant site for maximal heat loss**. - Heat loss from the abdomen is not as pronounced as from the head due to its **central location** and typically greater insulation. *Neck* - The neck's surface area is comparably small, and it is often covered or in close proximity to the body, which helps to **reduce heat loss**. - It does not possess the same combination of large surface area and lack of insulating fat as the head. *Palms & soles* - While palms and soles have a high density of **sweat glands** and can contribute to heat loss through evaporation, their **total surface area is relatively small** in a newborn. - These areas are less significant for overall maximal heat loss compared to the head due to their limited size.
Question 9: A 6-year-old child is brought with the following lesion. He can develop lesions in which organ in future?
- A. Esophagus
- B. Small intestine (Correct Answer)
- C. Colon (Large Intestine)
- D. Stomach
Explanation: ***Small intestine*** - The image shows **perioral melanotic macules**, specifically around the mouth, which are classic cutaneous manifestations of **Peutz-Jeghers syndrome**. - Peutz-Jeghers syndrome is an **autosomal dominant disorder** characterized by these mucocutaneous pigmentations and an increased risk of developing **hamartomatous polyps** in the gastrointestinal tract. - The **small intestine** is the **most commonly affected site** for polyps in Peutz-Jeghers syndrome, with **60-90% of patients** developing small bowel polyps, particularly in the **jejunum**. - These polyps can cause complications including **intussusception**, bleeding, and obstruction. - Patients also have an increased risk of **malignancies** in the small intestine and other organs (breast, ovary, pancreas, colon). *Colon (Large Intestine)* - While colonic polyps do occur in Peutz-Jeghers syndrome (**20-30% of cases**), they are **less frequent** than small intestinal polyps. - The colon is a secondary site of involvement compared to the small intestine. - Increased risk of colorectal cancer exists but the predominant polyp site remains the small bowel. *Stomach* - Gastric polyps occur in **approximately 25% of patients** with Peutz-Jeghers syndrome. - While gastric involvement can occur, it is **less common** than small intestinal involvement. - The stomach is a secondary site compared to the small intestine. *Esophagus* - Esophageal involvement with polyps in Peutz-Jeghers syndrome is **very rare**. - The typical distribution of hamartomatous polyps extends from stomach to rectum, with minimal esophageal involvement. - Esophagus is the least commonly affected GI organ in this syndrome.