Anatomy
2 questionsWhich bone attaches the sternum to the scapula?
Which branch of the facial nerve supplies the muscles of the lower lip?
FMGE 2018 - Anatomy FMGE Practice Questions and MCQs
Question 211: Which bone attaches the sternum to the scapula?
- A. Manubrium
- B. Clavicle (Correct Answer)
- C. First rib
- D. Second rib
Explanation: **Explanation:** The **Clavicle** (collarbone) is the correct answer because it serves as the only bony attachment between the upper limb and the axial skeleton. This connection is formed through two primary joints: 1. **Sternoclavicular (SC) Joint:** The medial end of the clavicle articulates with the manubrium of the sternum. 2. **Acromiovicular (AC) Joint:** The lateral end of the clavicle articulates with the acromion process of the scapula. By bridging these two points, the clavicle acts as a "strut," holding the scapula and humerus away from the thorax to allow for maximum range of motion. **Why other options are incorrect:** * **Manubrium:** This is the superior part of the sternum itself. While it provides the site for clavicular attachment, it does not directly reach or attach to the scapula. * **First Rib:** It lies inferior to the clavicle and articulates with the manubrium and the T1 vertebra. It does not articulate with the scapula (the scapula "glides" over the ribs via the physiological scapulothoracic joint, but there is no bony attachment). * **Second Rib:** It articulates with the sternal angle (Angle of Louis) and the T2 vertebra, playing no role in connecting the sternum to the scapula. **High-Yield NEET-PG Pearls:** * **First bone to ossify:** The clavicle is the first bone in the body to begin ossification (5th–6th week of fetal life). * **Ossification type:** It is the only long bone that undergoes **intramembranous ossification** (though its ends undergo endochondral ossification). * **Fracture Site:** The most common site of fracture is the junction of the medial two-thirds and lateral one-third. * **Clinical Sign:** In clavicular fractures, the medial fragment is elevated by the **Sternocleidomastoid** muscle.
Question 212: Which branch of the facial nerve supplies the muscles of the lower lip?
- A. Temporal
- B. Cervical
- C. Buccal
- D. Mandibular (Correct Answer)
Explanation: The facial nerve (CN VII) exits the stylomastoid foramen and enters the parotid gland, where it divides into five terminal branches that provide motor innervation to the muscles of facial expression. **1. Why Mandibular is Correct:** The **Marginal Mandibular branch** emerges from the lower part of the parotid gland and runs along or just below the lower border of the mandible. It supplies the muscles of the lower lip and chin, specifically the **depressor anguli oris, depressor labii inferioris, and mentalis**. Damage to this branch results in an asymmetrical smile due to the inability to depress the corner of the mouth on the affected side. **2. Why Other Options are Incorrect:** * **Temporal:** Supplies the muscles above the eye, including the frontalis, orbicularis oculi (upper part), and corrugator supercilii. * **Cervical:** Runs downward to supply the **platysma** muscle in the neck. * **Buccal:** Supplies the muscles of the cheek (**buccinator**) and the upper lip (orbicularis oris, levator labii superioris). While it contributes to the mouth area, the specific innervation for *lower lip depression* is mandibular. **3. High-Yield Clinical Pearls for NEET-PG:** * **Pes Anserinus:** The "goose's foot" pattern formed by the five terminal branches (Temporal, Zygomatic, Buccal, Mandibular, Cervical) within the parotid gland. * **Danger Zone:** The marginal mandibular nerve is vulnerable during submandibular gland surgery as it can dip up to 1–2 cm below the inferior border of the mandible. * **Buccinator Paradox:** The buccinator is a muscle of facial expression (supplied by the Buccal branch of CN VII) but is often confused with muscles of mastication (supplied by CN V3).
Dermatology
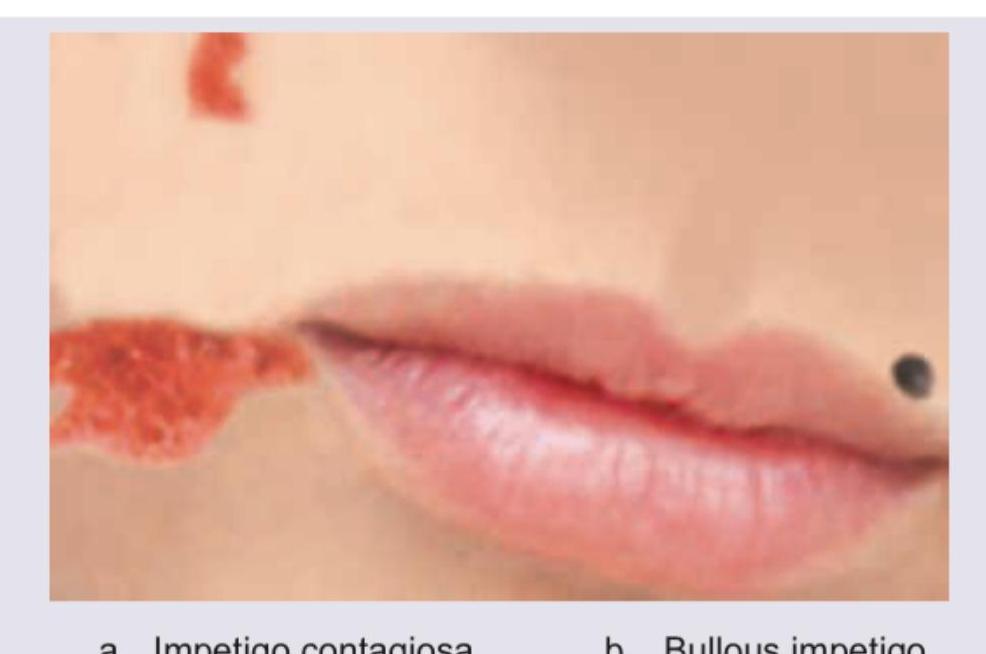
1 questionsA child presents with the skin lesions shown in the image. The most likely diagnosis is:
FMGE 2018 - Dermatology FMGE Practice Questions and MCQs
Question 211: A child presents with the skin lesions shown in the image. The most likely diagnosis is:
- A. Impetigo contagiosa (Correct Answer)
- B. Bullous impetigo
- C. Ritter disease
- D. Ecthyma
Explanation: ***Impetigo contagiosa*** - The image shows **honey-colored crusted lesions** around the mouth, which are highly characteristic of **impetigo contagiosa (non-bullous impetigo)**. - This form of impetigo is typically caused by *Staphylococcus aureus* or *Streptococcus pyogenes* and primarily affects superficial layers of the epidermis. *Bullous impetigo* - Characterized by **flaccid bullae** (blisters) that rupture to leave a thin, varnish-like crust, rather than the thick honey-colored crusts seen here. - It is exclusively caused by **Staphylococcus aureus** strains producing exfoliative toxins. *Ritter disease* - Also known as **Staphylococcal Scalded Skin Syndrome (SSSS)**, this condition involves widespread **erythema and exfoliation** resembling a burn. - It is a severe, systemic illness with widespread skin involvement, not localized crusted lesions like those pictured. *Ecthyma* - This is a more **deep-seated skin infection** that penetrates into the dermis, characterized by **"punched-out" ulcers** with thick, adherent crusts and often leaves scars. - While also caused by *Staphylococcus aureus* and/or *Streptococcus pyogenes*, its lesions are typically more severe and destructive than what is depicted.
Forensic Medicine
1 questionsThe most reliable criterion in Gustafson's criteria is:
FMGE 2018 - Forensic Medicine FMGE Practice Questions and MCQs
Question 211: The most reliable criterion in Gustafson's criteria is:
- A. Attrition
- B. Root resorption
- C. Transparency of root (Correct Answer)
- D. Periodontosis
Explanation: ***Transparency of root*** - This criterion, specifically **dentinal translucency**, is considered the most reliable age indicator in **Gustafson's criteria** due to its continuous and predictable increase with age. - The **translucency** results from the deposition of **secondary dentin** and obliteration of dentinal tubules, progressing from the apex towards the crown. *Attrition* - **Attrition** refers to the wear of tooth surfaces, which is highly variable and depends on diet, habits, and dental health, making it an unreliable age indicator. - While it generally increases with age, its rate is subject to many confounding factors. *Root resorption* - **Root resorption** is the progressive loss of tooth structure from the root and can be caused by various factors like trauma, infection, or orthodontic treatment, not solely age. - It is an unpredictable process and not a consistent age-related change. *Periodontosis* - **Periodontosis**, or **periodontal disease**, is inflammation and infection of the supporting structures around the teeth, influenced by oral hygiene and genetics. - While its prevalence may increase with age, it's not a direct and reliable physiological age marker for individuals.
Internal Medicine
1 questionsA 35-year-old lady who presented with a 6-month painless fluctuant, non-transilluminant swelling with a thin watery discharge. Clinical diagnosis is?
FMGE 2018 - Internal Medicine FMGE Practice Questions and MCQs
Question 211: A 35-year-old lady who presented with a 6-month painless fluctuant, non-transilluminant swelling with a thin watery discharge. Clinical diagnosis is?
- A. Brachial cyst
- B. Secondaries
- C. Lymphoma
- D. TB (Correct Answer)
Explanation: ***TB*** - **Tuberculosis (TB)** lymphadenopathy often presents as a **painless, fluctuant, non-transilluminant cervical swelling** (scrofula) with possible **thin, watery discharge** from a sinus tract [1]. - The 6-month duration indicates a **chronic process**, consistent with the indolent nature of TB infection [1]. *Brachial cyst* - A **branchial cleft cyst** typically presents as a **smooth, movable, and sometimes fluctuant neck mass**, but it is usually **transilluminant** unless infected. - While it can discharge, the fluid is often mucoid, and the discharge is less commonly described as thin and watery; also it typically develops during childhood or early adulthood. *Secondaries* - **Metastatic lymph nodes (secondaries)** are generally **firm, non-fluctuant, and non-tender**, and do not typically discharge thin watery fluid unless there is necrosis or ulceration of the overlying skin. - The absence of associated primary malignancy symptoms also makes this less likely. *Lymphoma* - **Lymphoma** presents as often **painless rubbery, firm, and non-fluctuant lymph node enlargement**, and discharge is not a typical feature unless there is skin involvement or ulceration in advanced stages. - The described fluctuance and watery discharge are not characteristic of simple lymphoma.
Ophthalmology
1 questionsAverage hypermetropia in a newborn is
FMGE 2018 - Ophthalmology FMGE Practice Questions and MCQs
Question 211: Average hypermetropia in a newborn is
- A. + 2.5 D (Correct Answer)
- B. + 10 D
- C. + 1 D
- D. + 5 D
Explanation: ***+ 2.5 D*** - Most **newborns** are **hypermetropic** (farsighted) due to a shorter axial length of the eye. - The average hypermetropic correction needed at birth is approximately **+2.5 diopters (D)**. *+ 10 D* - A hyperopia of **+10 D** would represent a very significant degree of **hypermetropia**, far exceeding the typical physiological range for a newborn. - Such high hyperopia in a newborn might suggest an **ocular anomaly** or a condition like **microphthalmia**. *+ 1 D* - A hyperopia of **+1 D** is a mild degree of hypermetropia, which is less than the average physiological hyperopia found in **newborns**. - While within a normal range for some infants, it does not represent the typical average for **newborns**. *+ 5 D* - A hyperopia of **+5 D** is a higher degree of hypermetropia than the average seen in **newborns**. - While possible, it is not the most common or average refractive error at birth, which is typically around **+2.5 D**.
Orthopaedics
1 questionsMost common complication of extra capsular fracture of neck of femur is:
FMGE 2018 - Orthopaedics FMGE Practice Questions and MCQs
Question 211: Most common complication of extra capsular fracture of neck of femur is:
- A. Malunion
- B. Ischemic necrosis
- C. Pulmonary complications
- D. Non union (Correct Answer)
Explanation: ***Non union*** - **Non-union** is a common complication in extracapsular femoral neck fractures due to the **disrupted blood supply** and mechanical forces across the fracture site. - The **fracture fragments** may fail to heal properly, leading to persistent pain, instability, and functional impairment. *Malunion* - **Malunion** occurs when the fracture heals in an **unacceptable anatomical position**, causing deformity or altered biomechanics. - While it can be a complication, **non-union** is generally more prevalent and problematic in extracapsular femoral neck fractures. *Ischemic necrosis* - **Ischemic necrosis** (or avascular necrosis) is less common in extracapsular femoral neck fractures compared to intracapsular fractures. - This is because the **extracapsular location** often spares the crucial blood supply to the femoral head, which is frequently compromised in intracapsular injuries. *Pulmonary complications* - **Pulmonary complications** (e.g., pneumonia, pulmonary embolism) are significant risks in elderly patients with hip fractures due to prolonged immobility and surgery. - However, direct fracture-related complications like **non-union** are distinct and represent issues specifically with bone healing.
Pathology
1 questionsVirchow's triad includes all except:-
FMGE 2018 - Pathology FMGE Practice Questions and MCQs
Question 211: Virchow's triad includes all except:-
- A. Stasis of blood flow
- B. Endothelial injury
- C. Platelet thrombus (Correct Answer)
- D. Hypercoagulability
Explanation: ***Platelet thrombus*** - Virchow's triad describes the three primary categories of factors that are thought to contribute to **thrombosis**, but it does not specifically include a formed **thrombus** itself. [1] - While **platelet thrombus** formation is an outcome of an imbalance in these factors, it is not one of the predisposing conditions identified by Virchow's triad. *Stasis of blood flow* - **Stasis** refers to a reduction in the rate of blood flow, which allows clotting factors to accumulate and endothelial cells to become hypoxic, increasing the risk of **thrombosis**. [1] - This is a well-established component of Virchow's triad, explaining why factors like immobility or venous insufficiency predispose to clot formation. *Endothelial injury* - **Endothelial injury** or dysfunction exposes the subendothelial collagen, leading to platelet adhesion and activation, and the initiation of the coagulation cascade. [1] - It is a critical component of Virchow's triad, often seen in conditions like **atherosclerosis** or trauma, which directly promotes thrombus formation. [2] *Hypercoagulability* - **Hypercoagulability**, or thrombophilia, refers to an increased propensity for coagulation due to genetic or acquired abnormalities in clotting factors. [1] - This imbalance in the coagulation system is a central part of Virchow's triad, leading to an exaggerated thrombotic response even in the absence of significant stasis or injury. [2] **References:** [1] Kumar V, Abbas AK, et al.. Robbins and Cotran Pathologic Basis of Disease. 9th ed. Hemodynamic Disorders, Thromboembolic Disease, and Shock, pp. 132-133. [2] Cross SS. Underwood's Pathology: A Clinical Approach. 6th ed. (Basic Pathology) introduces the student to key general principles of pathology, both as a medical science and as a clinical activity with a vital role in patient care. Part 2 (Disease Mechanisms) provides fundamental knowledge about the cellular and molecular processes involved in diseases, providing the rationale for their treatment. Part 3 (Systematic Pathology) deals in detail with specific diseases, with emphasis on the clinically important aspects., pp. 142-143.
Pediatrics
1 questionsA 6-year-old child is brought with the following lesion. He can develop lesions in which organ in future?
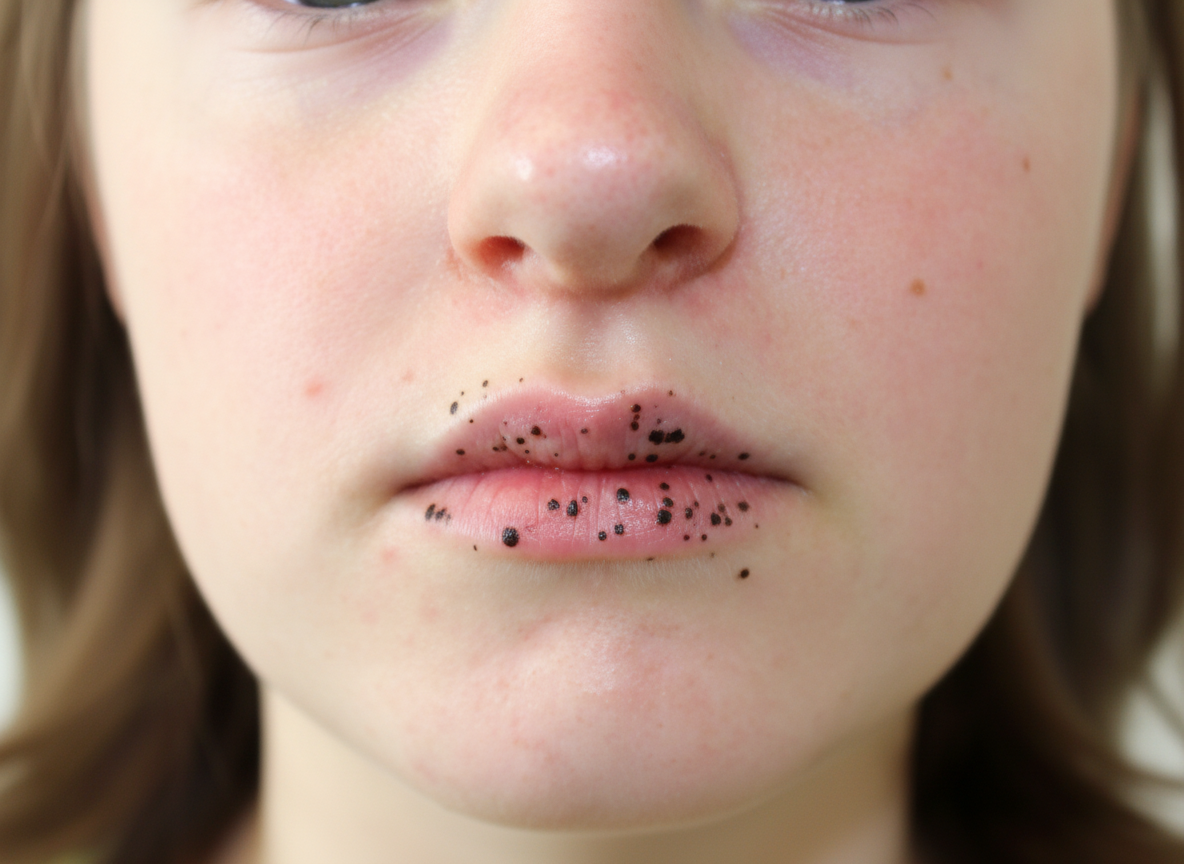
FMGE 2018 - Pediatrics FMGE Practice Questions and MCQs
Question 211: A 6-year-old child is brought with the following lesion. He can develop lesions in which organ in future?
- A. Esophagus
- B. Small intestine (Correct Answer)
- C. Colon (Large Intestine)
- D. Stomach
Explanation: ***Small intestine*** - The image shows **perioral melanotic macules**, specifically around the mouth, which are classic cutaneous manifestations of **Peutz-Jeghers syndrome**. - Peutz-Jeghers syndrome is an **autosomal dominant disorder** characterized by these mucocutaneous pigmentations and an increased risk of developing **hamartomatous polyps** in the gastrointestinal tract. - The **small intestine** is the **most commonly affected site** for polyps in Peutz-Jeghers syndrome, with **60-90% of patients** developing small bowel polyps, particularly in the **jejunum**. - These polyps can cause complications including **intussusception**, bleeding, and obstruction. - Patients also have an increased risk of **malignancies** in the small intestine and other organs (breast, ovary, pancreas, colon). *Colon (Large Intestine)* - While colonic polyps do occur in Peutz-Jeghers syndrome (**20-30% of cases**), they are **less frequent** than small intestinal polyps. - The colon is a secondary site of involvement compared to the small intestine. - Increased risk of colorectal cancer exists but the predominant polyp site remains the small bowel. *Stomach* - Gastric polyps occur in **approximately 25% of patients** with Peutz-Jeghers syndrome. - While gastric involvement can occur, it is **less common** than small intestinal involvement. - The stomach is a secondary site compared to the small intestine. *Esophagus* - Esophageal involvement with polyps in Peutz-Jeghers syndrome is **very rare**. - The typical distribution of hamartomatous polyps extends from stomach to rectum, with minimal esophageal involvement. - Esophagus is the least commonly affected GI organ in this syndrome.
Psychiatry
1 questionsManagement of a violent patient in psychiatry includes all except:
FMGE 2018 - Psychiatry FMGE Practice Questions and MCQs
Question 211: Management of a violent patient in psychiatry includes all except:
- A. CBT (Correct Answer)
- B. Haloperidol
- C. ECT
- D. BZD
Explanation: ***CBT*** - **Cognitive Behavioral Therapy (CBT)** is a long-term psychological intervention aimed at changing maladaptive thought patterns and behaviors. It is **not suitable for immediate management** of an acutely violent patient. - While CBT can be beneficial for aggression management in a stable patient, it requires patient cooperation, cognitive engagement, and time, which are not available during a **violent psychiatric emergency**. *Haloperidol* - **Haloperidol** is a potent typical antipsychotic frequently used in acute settings for rapid tranquilization of violent or severely agitated patients. - It is effective in reducing **psychosis-related agitation** and can be administered **intramuscularly** for quick onset of action. - Often used in combination with benzodiazepines for optimal control of acute violence. *ECT* - **Electroconvulsive Therapy (ECT)** may be considered in **severe, treatment-resistant cases** of violence associated with conditions like uncontrolled mania, catatonic excitement, or psychotic depression when pharmacological interventions have failed. - While not used for immediate acute management due to logistical requirements (consent, anesthesia, specialized setup), it can be an effective option for severe psychiatric conditions with persistent violence. - It works by inducing a brief controlled seizure, which can rapidly alleviate severe symptoms. *BZD* - **Benzodiazepines (BZDs)** like lorazepam or diazepam are **first-line agents** in the acute management of violent or agitated patients due to their rapid anxiolytic, sedative, and muscle relaxant properties. - They are particularly useful for **calming acute agitation** and are often combined with antipsychotics for rapid tranquilization. - Can be administered intramuscularly or intravenously for quick action in psychiatric emergencies.