Primary osteoarthritis affects all except:
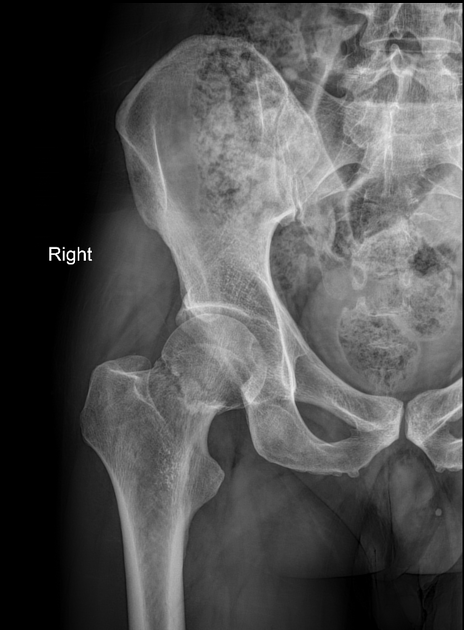
79 yrs old lady had fall, the following X-ray was taken. Which of the following is treatment?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Dorsum of first webspace is supplied by which nerve?
Gastric lavage is contraindicated in?
A patient presented with sudden onset of thunderclap headache & dilated pupils. Findings are consistent with:
Treatment of choice for recurrent thyrotoxicosis after surgery is:-
MC cause of nephrotic syndrome in adults:-
A child presents with night blindness, delayed dark adaptation. Which investigation is to be done further to confirm the diagnosis?
Primary osteoarthritis affects all except:
79 yrs old lady had fall, the following X-ray was taken. Which of the following is treatment?

A newborn loses maximum heat from:
Purpose of adding zinc to insulin in commercial preparations for treatment of diabetes mellitus is:-