FMGE 2018 — Orthopaedics
12 Previous Year Questions with Answers & Explanations
Adamantinoma affects
Most common site of osteomyelitis in children
Tennis player can spontaneously reduce a shoulder dislocation. He can do it again and again himself. He is suffering from?
Patient had an injury to thumb causing thumb abduction. Which of the following can happen?
Which of the following statements about tubercular osteomyelitis is NOT true?
In fracture of upper 1/3 of forearm, it is immobilized in:
Blount Disease is involvement of
Primary osteoarthritis affects all except:
79 yrs old lady had fall, the following X-ray was taken. Which of the following is treatment?
Blow out fracture can be due to:
FMGE 2018 - Orthopaedics FMGE Practice Questions and MCQs
Question 1: Adamantinoma affects
- A. Humerus
- B. Tibia (Correct Answer)
- C. Femur
- D. Radius
Explanation: ***Tibia*** - **Adamantinoma** is a rare, malignant bone tumor that almost exclusively affects the **tibia**, accounting for over 90% of cases. - It often presents as a **slow-growing mass** associated with pain and swelling in the shin. *Humerus* - While other primary bone tumors can affect the humerus, adamantinoma is **extremely rare** in this location. - The humerus is more commonly affected by tumors like **osteosarcoma** or **Ewing sarcoma**. *Femur* - The femur is a common site for various bone tumors, but **adamantinoma is not typically found** here. - Tumors like **osteosarcoma** and **chondrosarcoma** are much more prevalent in the femur. *Radius* - Similar to the humerus and femur, the radius is **not a characteristic location** for adamantinoma. - Tumors of the radius are generally less common than in the major long bones.
Question 2: Most common site of osteomyelitis in children
- A. Epiphysis
- B. Metaphysis (Correct Answer)
- C. Growth plate
- D. Diaphysis
Explanation: ***Metaphysis*** - The **metaphysis** is the most common site for osteomyelitis in children due to its rich, **slow-flowing sinusoidal blood supply**, which facilitates bacterial seeding. - The **nutrient arteries** in the metaphysis make sharp loops, creating a turbulent flow that slows circulation and allows bacteria to lodge more easily. *Epiphysis* - The **epiphysis** is less commonly affected in children because its separate blood supply is not as prone to bacterial seeding as the metaphysis. - In infants, however, infection can spread from the metaphysis to the epiphysis and joint space due to **transphyseal vessels**. *Growth plate* - The **growth plate** itself is generally resistant to infection due to its avascular nature. - However, infection in the adjacent metaphysis or epiphysis can potentially disrupt its function. *Diaphysis* - While the **diaphysis** has a blood supply, it is less common for osteomyelitis to originate here compared to the metaphysis. - It usually occurs as a secondary spread from a metaphyseal infection or in specific scenarios like in **sickle cell disease**.
Question 3: Tennis player can spontaneously reduce a shoulder dislocation. He can do it again and again himself. He is suffering from?
- A. Inferior shoulder dislocation
- B. Fracture upper end humerus
- C. Acute shoulder dislocation
- D. Recurrent shoulder dislocation (Correct Answer)
Explanation: ***Recurrent shoulder dislocation*** - The ability to **spontaneously reduce** a shoulder dislocation, and the history of it happening "again and again" strongly indicate **recurrent shoulder dislocation**. - This condition often results from **ligamentous laxity** or damage to the **labrum** (Bankart lesion) that fails to stabilize the shoulder joint after an initial dislocation. *Inferior shoulder dislocation* - This is a **specific type of shoulder dislocation** (luxatio erecta) where the humeral head is displaced inferiorly, but "inferior" alone does not explain the recurrent nature. - While possible in an individual, the key element here is the **recurrence** and self-reduction, not just the direction of a single dislocation. *Fracture upper end humerus* - A fracture of the upper end of the humerus is a **bony injury** and would typically present with severe pain, swelling, and inability to move the arm, not spontaneous reduction. - This injury would usually **prevent** the patient from repeatedly dislocating and reducing their shoulder. *Acute shoulder dislocation* - An acute shoulder dislocation refers to a **single, recent episode** of dislocation. - The patient's repeated ability to self-reduce the shoulder indicates a chronic problem rather than an initial, isolated event.
Question 4: Patient had an injury to thumb causing thumb abduction. Which of the following can happen?
- A. Kaplan lesion
- B. Game keepers thumb (Correct Answer)
- C. Mallet finger
- D. Bennett fracture
Explanation: ***Gamekeeper's thumb*** - A **Gamekeeper's thumb**, or **skier's thumb**, is an injury to the **ulnar collateral ligament (UCL)** of the thumb's metacarpophalangeal (MCP) joint. - This injury commonly occurs due to a **forceful abduction** and hyperextension of the thumb. *Kaplan lesion* - A **Kaplan lesion** refers to an avulsion fracture of the radial styloid process, usually associated with scaphoid fractures. - This lesion is typically related to wrist injuries, not primarily thumb abduction. *Bennett fracture* - A **Bennett fracture** is an intra-articular fracture at the base of the first metacarpal bone. - It usually results from an axial load applied to a partially flexed thumb, rather than pure abduction. *Mallet finger* - A **mallet finger** is an injury to the **extensor tendon** of the finger, causing the fingertip to remain in a flexed position. - This injury typically affects the distal interphalangeal (DIP) joint of any finger and is not directly related to thumb abduction.
Question 5: Which of the following statements about tubercular osteomyelitis is NOT true?
- A. Sequestrum is uncommon
- B. It is a type of secondary osteomyelitis
- C. Periosteal reaction is characteristic (Correct Answer)
- D. Inflammation is minimal
Explanation: ***Periosteal reaction is characteristic*** - This statement is **NOT true** for tubercular osteomyelitis; periosteal reaction is generally **minimal or absent** due to the insidious and less florid inflammatory response. - Unlike pyogenic osteomyelitis, which causes significant periosteal new bone formation, tuberculosis typically results in **slow bone destruction** without marked reactive bone changes. *Sequestrum is uncommon* - This statement is **true** because **sequestrum** (a piece of dead bone separated from healthy bone) is less frequently observed in tubercular osteomyelitis compared to pyogenic osteomyelitis. - The **granulomatous inflammation** of tuberculosis tends to cause slow bone necrosis rather than the rapid, liquefactive necrosis that leads to large sequestra. *It is a type of secondary osteomyelitis* - This statement is **true** as tubercular osteomyelitis is almost always secondary to a **primary focus of tuberculosis** elsewhere in the body, typically the lungs [1]. - The infection spreads **hematogenously** to the bone, making it a manifestation of disseminated tuberculosis rather than a primary bone infection [1]. *Inflammation is minimal* - This statement is **true** in the sense that the **acute inflammatory response** in tubercular osteomyelitis is often less pronounced than in pyogenic infections. - While it is a chronic infectious process, the characteristic **granulomatous inflammation** develops over time, and the initial or acute inflammatory signs might be subtle or "minimal" compared to bacterial osteomyelitis [1].
Question 6: In fracture of upper 1/3 of forearm, it is immobilized in:
- A. Supination (Correct Answer)
- B. Pronation
- C. Any position
- D. Mid prone
Explanation: ***Supination*** - In a fracture of the **proximal third of the forearm**, the **biceps brachii** and **supinator muscles**, which are still attached to the proximal fragment, will cause it to **supinate**. - To align the distal fragment with the proximal fragment and ensure proper healing, the forearm must be immobilized in **full supination**. *Pronation* - **Pronation** would cause malalignment of the fracture fragments, as the proximal fragment would remain supinated while the distal fragment is pronated. - This position is only used for fractures of the **distal third of the forearm** where the **pronator quadratus** and **pronator teres** dominate. *Any position* - Immobilizing in **any position** would risk **malunion** or nonunion due to the unopposed muscle forces acting on the proximal and distal fragments. - Correct anatomical alignment is crucial for restoring function and preventing long-term complications. *Mid prone* - The **mid-prone** position is typically used for fractures of the **middle third of the forearm**, where the pronator and supinator muscle forces are more balanced. - In a proximal third fracture, the stronger supinator muscles would still pull the proximal fragment into supination, causing misalignment in the mid-prone position.
Question 7: Blount Disease is involvement of
- A. Distal femur
- B. Distal tibia
- C. Proximal tibia (Correct Answer)
- D. Proximal femur
Explanation: ***Proximal tibia*** - Blount disease, also known as **tibia vara**, is a growth disorder affecting the **tibia** (shin bone) in children. - It specifically involves the **medial physis of the proximal tibia**, leading to abnormal growth in this area and resulting in a **bow-legged** deformity. *Distal femur* - Malformations or growth disturbances of the **distal femur** are typically associated with conditions like genu valgum (**knock-knees**) or other angular deformities originating higher up in the leg. - Blount disease's primary pathology does not originate from the distal femur. *Distal tibia* - Conditions affecting the **distal tibia** can lead to ankle deformities or foot problems. - Blount disease is distinctly a problem of the knee region, not the ankle. *Proximal femur* - Problems in the **proximal femur** are commonly associated with conditions like Legg-Calvé-Perthes disease or developmental dysplasia of the hip. - While these can also cause gait abnormalities, Blount disease's characteristic bowing deformity originates from the tibia.
Question 8: Primary osteoarthritis affects all except:
- A. Metacarpophalangeal joint (Correct Answer)
- B. Hip Joint
- C. Distal interphalangeal joint
- D. Knee joint
Explanation: ***Metacarpophalangeal joint*** - The **metacarpophalangeal (MCP) joints** are typically spared in primary osteoarthritis, making their involvement a less common presentation. - Involvement of the MCP joints, particularly with significant inflammation, might suggest other conditions like **rheumatoid arthritis**. *Hip Joint* - The hip joint is a common site for primary osteoarthritis due to its **weight-bearing function** and susceptibility to mechanical stress. - Patients often experience **groin pain** and reduced range of motion, particularly internal rotation. *Distal interphalangeal joint* - The **distal interphalangeal (DIP) joints** are very commonly affected in primary osteoarthritis, leading to the formation of **Heberden's nodes**. - These nodes are bony enlargements that indicate osteophyte formation and cartilage loss. *Knee joint* - The knee joint is another frequently affected large joint in primary osteoarthritis, often presenting with **pain**, **stiffness**, and **crepitus**. - Its **weight-bearing role** contributes significantly to its vulnerability to degenerative changes.
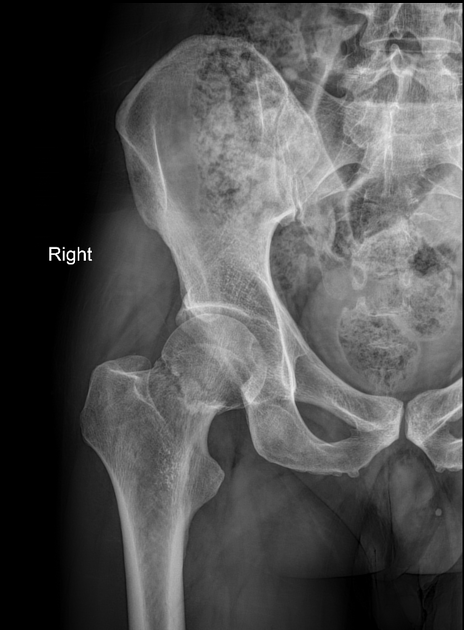
Question 9: 79 yrs old lady had fall, the following X-ray was taken. Which of the following is treatment?
- A. Hip spica
- B. Nailing
- C. Hemiahroplasty (Correct Answer)
- D. Total Hip Replacement
Explanation: ***Hemiarthroplasty*** - The X-ray shows a **displaced femoral neck fracture** in an elderly patient, which typically has a high risk of **avascular necrosis** of the femoral head due to disruption of blood supply. - Hemiarthroplasty involves replacing only the **femoral head and neck** with a prosthetic component, leaving the acetabulum intact, which is suitable for elderly patients with good acetabular cartilage and less active lifestyles. *Hip spica* - A hip spica cast is primarily used for **pediatric femur fractures** or certain types of hip dislocations in children, not for displaced femoral neck fractures in elderly adults. - This method would not provide stable fixation or address the high risk of **avascular necrosis** associated with these fractures in older patients. *Nailing* - Nailing (intramedullary nailing) is typically used for **intertrochanteric fractures** or subtrochanteric fractures, where the fracture line is distal to the femoral neck. - For displaced femoral neck fractures, nailing alone may not provide adequate stability and carries a higher risk of **non-union** or **avascular necrosis** compared to arthroplasty in elderly patients. *Total Hip Replacement* - Total hip replacement involves replacing both the **femoral head and the acetabulum** with prosthetic components. - While an option for femoral neck fractures, it is generally reserved for younger, more active patients or those with pre-existing **acetabular pathology** like arthritis, as it is a more extensive and complex procedure than hemiarthroplasty.
Question 10: Blow out fracture can be due to:
- A. Tennis ball injury (Correct Answer)
- B. Punch at the chin from below
- C. Sudden fall
- D. Chisel and hammer injury
Explanation: ***Tennis ball injury*** - A tennis ball injury to the orbit can cause a **blowout fracture** due to either direct impact compressing the globe or hydraulic pressure from the ball transmission of force, leading to a fracture of the orbital floor or medial wall. - The impact forces the orbital contents posteriorly, increasing intraorbital pressure which in turn causes the weakest bony walls (usually the floor or medial wall) to fracture outwards into the maxillary or ethmoid sinuses, respectively. *Punch at the chin from below* - A punch to the chin from below typically results in fractures of the **mandible**, particularly the condyles or angle. - This mechanism does not directly transmit force to the orbital rim or globe in a way that would cause a classic blowout fracture. *Sudden fall* - A sudden fall can cause various types of fractures depending on the impact site, but it is not a specific or common mechanism for a **blowout fracture**. - Falls usually lead to fractures of the extremities, hips, or skull other than the orbit, depending on how the body impacts the ground. *Chisel and hammer injury* - A chisel and hammer injury would more likely cause a **localized, penetrating injury** or a focal fracture at the point of impact on the face or skull. - This type of injury does not typically generate the diffuse hydraulic pressure within the orbit needed to cause a **blowout fracture** of the orbital floor or medial wall.