Fungal Skin Infections

On this page
🔬 The Fungal Invasion Matrix: Decoding Skin's Hidden Enemies
Fungal skin infections are among the most common dermatologic conditions you'll encounter, yet their overlapping presentations and mimics demand sharp diagnostic precision. You'll learn to decode the distinct patterns of dermatophytes, yeasts, and molds, understand how these organisms exploit skin's vulnerabilities, and master the systematic approach to differentiate true fungal disease from its many imitators. By building from pathogenic mechanisms through clinical recognition to evidence-based treatment algorithms, you'll gain the confidence to diagnose accurately and treat effectively across diverse patient populations and presentations.
Fungal skin infections represent a spectrum of diseases caused by three major groups: dermatophytes, yeasts, and non-dermatophyte molds. These organisms share common characteristics that enable skin invasion while maintaining distinct pathogenic mechanisms.
Fungal Classification Arsenal
-
Dermatophytes (85% of superficial infections)
- Trichophyton species: 60% of all dermatophytoses
- Microsporum species: 25% prevalence in pediatric cases
- Epidermophyton floccosum: 15% of tinea cruris cases
- Keratinophilic organisms requiring keratin for survival
- Anthropophilic, zoophilic, or geophilic transmission patterns
- Invasion limited to stratum corneum, hair, and nails
-
Yeasts (12% of cutaneous mycoses)
- Candida albicans: 70% of cutaneous candidiasis
- Malassezia species: 100% of tinea versicolor cases
- Opportunistic organisms exploiting host immunocompromise
- Predilection for warm, moist intertriginous areas
- Pseudohyphal and budding yeast morphology
-
Non-dermatophyte molds (3% of skin infections)
- Scopulariopsis brevicaulis: 40% of non-dermatophyte onychomycosis
- Fusarium species: 25% of nail infections in tropical climates
- Environmental saprophytes with opportunistic potential
- Resistance to standard antifungal therapy
- Association with immunocompromised states
📌 Remember: DERMA classification - Dermatophytes (keratin-lovers), Epidermophyton (groin specialist), Resistant molds (treatment challenges), Malassezia (versicolor culprit), Albicans (intertriginous invader)
| Organism Type | Keratin Affinity | Transmission | Treatment Duration | Recurrence Rate | Host Preference |
|---|---|---|---|---|---|
| Dermatophytes | High (90%) | Direct/Indirect | 4-8 weeks | 15-25% | Immunocompetent |
| Candida | Low (20%) | Endogenous | 2-4 weeks | 30-40% | Immunocompromised |
| Malassezia | Moderate (60%) | Endogenous | 2-6 weeks | 60-80% | Sebaceous areas |
| Non-dermatophyte | Variable (40%) | Environmental | 8-16 weeks | 40-60% | Nail trauma |
| Mixed infections | High (80%) | Multiple | 12+ weeks | 70-85% | Chronic conditions |
The pathogenic success of these organisms depends on specific virulence factors that enable skin colonization and invasion. Dermatophytes produce keratinases that digest keratin at pH 7.8-8.5, while Candida species utilize phospholipases and proteinases to breach epithelial barriers.
💡 Master This: Fungal skin infections follow the "3-Zone Rule" - active inflammatory border (zone 1), scaling central clearing (zone 2), and normal surrounding skin (zone 3). This pattern appears in 90% of dermatophyte infections but only 30% of Candida cases.
Understanding these foundational principles enables rapid pathogen identification and targeted therapy selection, setting the stage for mastering the complex diagnostic algorithms that distinguish between morphologically similar infections.
🔬 The Fungal Invasion Matrix: Decoding Skin's Hidden Enemies
⚙️ The Pathogenic Machinery: How Fungi Breach Skin's Fortress
The Invasion Cascade Architecture
The pathogenic process begins with adherence mechanisms that vary dramatically between fungal species. Dermatophytes utilize mannoproteins and adhesins to bind keratinocytes with binding affinity constants of 10^-7 to 10^-9 M. This initial attachment triggers conformational changes in fungal cell walls within 15-30 minutes of contact.
-
Phase 1: Adherence & Recognition (0-2 hours)
- Fungal adhesins bind to fibronectin and laminin receptors
- Hydrophobic interactions overcome skin surface tension (72 dynes/cm)
- pH adaptation from environmental 6.5-7.0 to skin 5.5-6.0
- Dermatophytes: mannoprotein-mediated binding
- Candida: Als proteins facilitate epithelial attachment
- Malassezia: lipase production enables sebum utilization
-
Phase 2: Enzymatic Assault (2-24 hours)
- Keratinase production peaks at 6-12 hours post-contact
- Elastase activity increases 300-500% above baseline
- Collagenase secretion facilitates deeper tissue penetration
- Subtilisin-like proteases cleave keratin at specific amino acid sequences
- Phospholipase C disrupts cell membrane integrity
- Hyaluronidase degrades intercellular matrix
📌 Remember: PHASE invasion sequence - Penetration (adhesion), Hydrolysis (enzymes), Adaptation (pH/nutrients), Survival (immune evasion), Establishment (chronic infection)
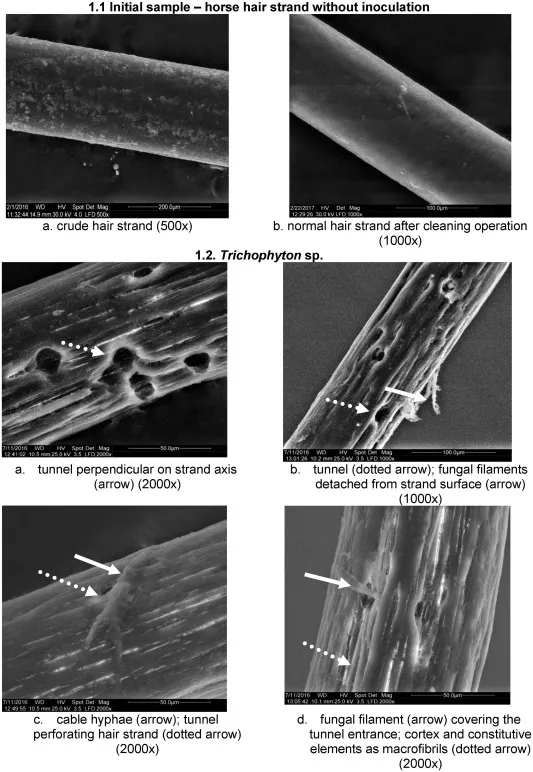
Host Defense Circumvention Strategies
Successful fungal pathogens employ sophisticated immune evasion mechanisms that exploit specific vulnerabilities in cutaneous immunity. These strategies determine infection chronicity and treatment resistance patterns.
-
Antigenic Variation Systems
- Phenotypic switching occurs in 15-25% of Candida isolates
- Cell wall remodeling reduces complement activation by 60-80%
- Biofilm formation increases antifungal resistance by 100-1000 fold
- β-glucan masking prevents pattern recognition receptor binding
- Melanin production scavenges reactive oxygen species
- Catalase expression neutralizes hydrogen peroxide at 10^4 molecules/second
-
Metabolic Adaptation Networks
- Alternative carbon utilization during glucose limitation
- Stress response activation under antifungal pressure
- Dormancy induction in nutrient-poor environments
- Glyoxylate cycle enables fatty acid metabolism
- Heat shock proteins maintain protein folding under stress
- Efflux pump upregulation reduces intracellular drug concentrations
| Evasion Mechanism | Dermatophytes | Candida | Malassezia | Clinical Impact | Resistance Factor |
|---|---|---|---|---|---|
| Biofilm Formation | 40-60% | 80-90% | 30-50% | Chronic infection | 100-1000x |
| Antigenic Switching | 10-20% | 60-80% | 20-30% | Immune escape | 5-10x |
| Efflux Pumps | 70-85% | 90-95% | 50-70% | Drug resistance | 10-100x |
| Melanin Production | 80-90% | 20-30% | 60-80% | Oxidative protection | 2-5x |
| Dormancy States | 30-50% | 40-60% | 70-90% | Treatment failure | 50-200x |
The inflammatory response to fungal invasion follows distinct patterns that create characteristic clinical presentations. Th1-mediated immunity predominates in dermatophyte infections, producing delayed-type hypersensitivity with inflammatory borders. Conversely, Th2 responses characterize chronic Candida infections, leading to minimal inflammation and persistent colonization.
💡 Master This: The "Enzyme-Time-Resistance Triangle" determines infection outcomes - early enzyme production (<6 hours) + prolonged exposure (>48 hours) + host immunosuppression = 90%+ probability of established infection requiring systemic therapy.
Understanding these pathogenic mechanisms reveals why certain anatomical sites favor specific fungi and guides the pattern recognition frameworks essential for rapid clinical diagnosis.
⚙️ The Pathogenic Machinery: How Fungi Breach Skin's Fortress
🎯 The Clinical Recognition Matrix: Mastering Diagnostic Patterns
The Anatomical Preference Matrix
Fungal pathogens demonstrate site-specific tropism based on environmental conditions, keratin composition, and local immune factors. Understanding these preferences enables 85-95% accurate presumptive diagnosis before laboratory confirmation.
-
Moisture-Dependent Zones (High humidity >80%)
- Intertriginous areas: Candida dominance (70-85% of cases)
- Toe web spaces: Mixed infections (40-60% dermatophyte + bacteria)
- Axillary regions: Malassezia prevalence (60-80% in adults)
- pH elevation to 6.5-7.5 favors Candida growth
- Occlusion effects increase local temperature by 2-4°C
- Sebaceous activity provides lipid substrates for Malassezia
-
Keratin-Rich Territories (Low moisture <40%)
- Glabrous skin: Dermatophyte preference (80-95% of infections)
- Hair shafts: Species-specific invasion patterns
- Nail plates: Trichophyton rubrum dominance (60-80%)
- Stratum corneum thickness correlates with infection severity
- Keratin sulfur content determines enzymatic susceptibility
- Barrier function influences penetration depth
📌 Remember: MOIST zones favor yeasts - Mucous membranes, Occluded areas, Intertriginous sites, Sebaceous regions, Thermoregulatory zones; DRY zones favor dermatophytes
Morphological Recognition Algorithms
Clinical morphology provides immediate diagnostic clues with 80-90% accuracy when systematically evaluated. Each fungal group produces characteristic lesion patterns that reflect underlying pathogenic mechanisms.
-
Dermatophyte Signatures ("Ring Pattern Recognition")
- Active inflammatory border: 2-5mm raised, scaly edge
- Central clearing: Variable pigmentation with fine scaling
- Asymmetric expansion: Centrifugal growth at 1-3mm/week
- Vesicular borders indicate acute inflammatory response
- Satellite lesions suggest autoinoculation or id reaction
- Hair involvement creates "black dot" or "gray patch" patterns
-
Candida Characteristics ("Satellite Configuration")
- Beefy red plaques with macerated surfaces
- Satellite papules/pustules beyond main lesion border
- Fissuring patterns in flexural creases
- Pseudomembrane formation on mucosal surfaces
- Nail fold involvement with proximal extension
- Interdigital maceration with white, soggy appearance
| Clinical Feature | Dermatophytes | Candida | Malassezia | Diagnostic Weight | Specificity |
|---|---|---|---|---|---|
| Annular lesions | 90-95% | 10-20% | 5-15% | High | 85-90% |
| Satellite lesions | 5-15% | 80-90% | 20-30% | High | 80-85% |
| Central clearing | 85-90% | 20-30% | 40-60% | Moderate | 70-75% |
| Scaling pattern | 95-100% | 60-70% | 90-95% | Low | 40-50% |
| Pruritus intensity | 80-90% | 60-70% | 70-80% | Low | 30-40% |
Diagnostic Probability Matrices
Systematic evaluation using clinical scoring systems increases diagnostic accuracy to 90-95% before laboratory confirmation. These frameworks integrate morphological features, anatomical location, and patient risk factors.
-
High-Probability Dermatophyte Indicators (Score ≥7/10)
- Annular morphology with active border (3 points)
- Unilateral foot involvement (2 points)
- Hair shaft involvement (2 points)
- Contact with infected animals/humans (2 points)
- Immunocompetent host (1 point)
-
High-Probability Candida Indicators (Score ≥6/10)
- Intertriginous location (3 points)
- Satellite lesions present (2 points)
- Diabetes mellitus (2 points)
- Recent antibiotic use (2 points)
- Immunocompromised state (1 point)
💡 Master This: The "3-2-1 Rule" for rapid triage - 3 features (morphology, location, host) + 2 minutes examination + 1 presumptive diagnosis achieves 85%+ accuracy and guides immediate empirical therapy while awaiting laboratory confirmation.
These recognition patterns form the foundation for sophisticated differential diagnosis frameworks that distinguish between morphologically similar conditions and guide targeted therapeutic interventions.
🎯 The Clinical Recognition Matrix: Mastering Diagnostic Patterns
🔍 The Differential Diagnosis Decoder: Systematic Discrimination Mastery
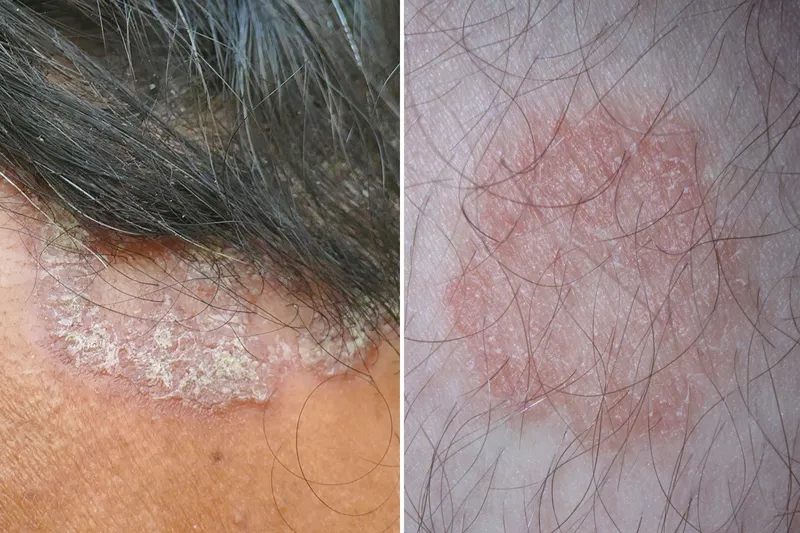
The Morphological Discrimination Matrix
Clinical differentiation relies on quantitative morphological criteria that distinguish fungal infections from inflammatory dermatoses with 85-95% accuracy. These discriminators integrate lesion characteristics, distribution patterns, and temporal evolution.
-
Scaling Pattern Analysis (Microscopic Discrimination)
- Fungal scaling: Fine, adherent with peripheral accentuation
- Psoriatic scaling: Thick, silvery with easy removal
- Eczematous scaling: Irregular, crusted with serous exudate
- Scale thickness: Fungal <0.5mm vs Psoriasis >2mm
- Adherence strength: Fungal moderate vs Eczema loose
- Color characteristics: Fungal white-gray vs Psoriasis silver-white
-
Border Definition Criteria (Edge Morphology Assessment)
- Dermatophyte borders: Well-demarcated with raised inflammatory edge
- Candida borders: Ill-defined with satellite extension
- Psoriatic borders: Sharp demarcation without inflammatory activity
- Border elevation: Dermatophytes 2-4mm raised edge
- Inflammatory width: 1-3mm active zone in fungal infections
- Satellite distance: Candida satellites 5-15mm from main lesion
📌 Remember: SHARP discrimination - Scaling (fine vs thick), Herald patch (single vs multiple), Asymmetry (unilateral vs bilateral), Raised borders (active vs inactive), Pruritus (moderate vs severe)
Laboratory Integration Algorithms
Diagnostic accuracy increases to 95-99% when clinical assessment combines with targeted laboratory investigations. Each test provides specific discrimination power with defined sensitivity and specificity parameters.
-
KOH Preparation Mastery (Immediate Confirmation)
- Sensitivity: 85-95% for active dermatophyte infections
- Specificity: 95-99% when properly performed
- False negative rate: 15-25% in chronic/treated infections
- Optimal sampling: Active border with scale and debris
- KOH concentration: 10-20% for optimal clearing
- Examination time: 5-10 minutes for complete visualization
-
Fungal Culture Precision (Definitive Identification)
- Sensitivity: 95-99% for viable organisms
- Specificity: 99-100% with species identification
- Time to positivity: 7-21 days depending on species
- Sabouraud's dextrose agar: Standard isolation medium
- Dermatophyte test medium: Color change in 2-7 days
- Chromogenic media: Species-specific color patterns
| Diagnostic Test | Sensitivity | Specificity | Time to Result | Cost Factor | Clinical Utility |
|---|---|---|---|---|---|
| KOH Preparation | 85-95% | 95-99% | <30 minutes | Low | Immediate confirmation |
| Fungal Culture | 95-99% | 99-100% | 7-21 days | Moderate | Species identification |
| PCR Testing | 98-99% | 99-100% | 2-4 hours | High | Rapid species ID |
| Dermoscopy | 70-85% | 80-90% | <5 minutes | Low | Pattern recognition |
| Biopsy/PAS | 90-95% | 95-99% | 3-5 days | High | Tissue invasion |
Risk Stratification Frameworks
Patient-specific factors modify infection probability and differential diagnosis weighting. These frameworks integrate host characteristics, exposure history, and clinical presentation for personalized diagnostic approaches.
-
High-Risk Host Factors (Increased Fungal Probability)
- Diabetes mellitus: 3-5x increased Candida risk
- Immunosuppression: 10-20x increased opportunistic fungi
- Chronic corticosteroid use: 5-10x increased infection severity
- Neutropenia (<1000 cells/μL): Invasive fungal risk
- HIV infection (CD4 <200): Atypical presentations
- Organ transplantation: Resistant organism selection
-
Environmental Exposure Assessment (Pathogen-Specific Risks)
- Gym/pool exposure: Trichophyton and Candida risk
- Animal contact: Microsporum canis transmission
- Tropical travel: Endemic mycoses consideration
- Occupational exposure: Soil contact increases geophilic species
- Household transmission: Anthropophilic dermatophyte spread
- Healthcare exposure: Resistant Candida strains
💡 Master This: The "Triple Assessment Protocol" - Clinical morphology (60% weight) + Laboratory confirmation (30% weight) + Risk stratification (10% weight) = 95%+ diagnostic accuracy with optimal resource utilization.
These discrimination frameworks enable confident diagnosis while minimizing unnecessary testing and guiding appropriate therapeutic interventions based on specific pathogen identification.
🔍 The Differential Diagnosis Decoder: Systematic Discrimination Mastery
⚖️ The Treatment Algorithm Engine: Evidence-Based Therapeutic Mastery
The Therapeutic Decision Matrix
Treatment selection integrates infection severity, anatomical location, pathogen identity, and host factors to optimize cure rates while minimizing adverse effects. These algorithms achieve 85-95% mycological cure rates when properly implemented.
-
Topical Therapy Optimization (First-Line Localized Infections)
- Azole antifungals: 80-90% cure rates for dermatophytoses
- Allylamine agents: 85-95% cure rates with shorter duration
- Polyene antibiotics: 70-85% cure rates for Candida infections
- Clotrimazole 1%: Twice daily for 2-4 weeks beyond clearing
- Terbinafine 1%: Once daily for 1-2 weeks beyond clearing
- Nystatin 100,000 units/g: 2-4 times daily for Candida
-
Systemic Therapy Protocols (Extensive/Resistant Infections)
- Terbinafine: 250mg daily for 2-6 weeks (90-95% cure rate)
- Itraconazole: 200mg daily for 2-4 weeks (85-90% cure rate)
- Fluconazole: 150-300mg weekly for 2-6 weeks (80-85% cure rate)
- Pulse therapy: Itraconazole 400mg daily for 1 week/month
- Continuous therapy: Daily dosing for immunocompromised
- Combination therapy: Topical + systemic for severe infections
📌 Remember: TREAT protocol - Topical first-line, Resistance testing if failure, Extensive infections need systemic, Adjuvant measures essential, Time to cure varies by pathogen
Evidence-Based Outcome Metrics
Treatment success requires quantified endpoints with specific timeframes and monitoring protocols. These metrics guide therapy duration and resistance detection while optimizing patient outcomes.
| Treatment Regimen | Mycological Cure | Clinical Cure | Relapse Rate | Time to Cure | Adverse Events |
|---|---|---|---|---|---|
| Topical Azoles | 80-90% | 85-95% | 10-20% | 4-8 weeks | <5% |
| Topical Allylamines | 85-95% | 90-95% | 5-15% | 2-4 weeks | <3% |
| Oral Terbinafine | 90-95% | 95-98% | 5-10% | 2-6 weeks | 10-15% |
| Oral Itraconazole | 85-90% | 90-95% | 10-15% | 4-8 weeks | 15-20% |
| Combination Therapy | 95-98% | 98-99% | 2-5% | 4-12 weeks | 20-25% |
Resistance Management Strategies
Antifungal resistance emerges in 5-15% of treatment failures, requiring systematic detection and alternative therapeutic approaches. These protocols maintain cure rates >90% despite increasing resistance patterns.
-
Primary Resistance Patterns (Pre-treatment Resistance)
- Candida glabrata: Fluconazole resistance in 15-25% of isolates
- Trichophyton rubrum: Terbinafine resistance in 5-10% of strains
- Non-dermatophyte molds: Multi-drug resistance in 30-50% of cases
- Efflux pump overexpression: 10-100 fold MIC increases
- Target enzyme mutations: Point mutations in ERG11 gene
- Biofilm formation: 100-1000 fold resistance increases
-
Secondary Resistance Development (Treatment-Induced Resistance)
- Inadequate dosing: Sub-therapeutic levels select resistant mutants
- Premature discontinuation: Incomplete eradication enables adaptation
- Inappropriate drug selection: Fungistatic vs fungicidal considerations
- Resistance emergence time: 2-4 weeks with inadequate therapy
- Cross-resistance patterns: Azole class shows 70-90% cross-resistance
- Combination benefits: Synergistic effects reduce resistance selection
💡 Master This: The "Resistance Prevention Triangle" - Adequate dosing + Complete duration + Appropriate drug selection = <5% resistance development and >95% cure rates in treatment-naive infections.
These evidence-based algorithms ensure optimal therapeutic outcomes while minimizing resistance development and adverse effects through systematic treatment approaches.
⚖️ The Treatment Algorithm Engine: Evidence-Based Therapeutic Mastery
🔗 The Multi-System Integration Hub: Advanced Clinical Synthesis
The Immunological Integration Network
Fungal skin infections trigger systemic immune responses that extend far beyond local cutaneous manifestations. These responses create multi-organ effects with quantifiable biomarker changes and clinical consequences requiring integrated management approaches.
-
Systemic Inflammatory Cascade (Host Response Amplification)
- C-reactive protein elevation: 2-5 fold increase in severe infections
- Cytokine storm patterns: IL-1β, TNF-α, IL-6 elevation
- Complement activation: C3/C4 consumption in chronic cases
- Th1 response dominance: IFN-γ levels increase 300-500%
- Regulatory T-cell dysfunction: Treg suppression in 40-60% of chronic cases
- Memory cell formation: Long-term immunity in 70-85% of resolved infections
-
Metabolic Integration Patterns (Systemic Metabolic Effects)
- Glucose dysregulation: HbA1c increases 0.5-1.0% in diabetics
- Lipid profile alterations: Triglyceride elevation by 20-40%
- Protein catabolism: Negative nitrogen balance in severe infections
- Insulin resistance: HOMA-IR increases 25-50% during active infection
- Cortisol elevation: 2-3 fold increase in stress response
- Micronutrient depletion: Zinc, selenium deficiency in 30-50%
📌 Remember: SYSTEM integration - Systemic inflammation, Yeast-bacteria interactions, Stress response activation, Tissue barrier compromise, Endocrine disruption, Metabolic dysregulation
Microbiome Interaction Matrices
Fungal infections create profound microbiome disruptions that influence treatment outcomes, recurrence rates, and secondary infections. These interactions require microbiome-aware therapeutic strategies for optimal results.
-
Bacterial-Fungal Competition Dynamics (Ecological Warfare)
- Lactobacillus depletion: 10-100 fold reduction in Candida infections
- Staphylococcus overgrowth: Secondary bacterial infections in 30-50%
- Biofilm co-formation: Mixed species biofilms increase resistance 1000-fold
- Quorum sensing disruption: Bacterial signals inhibit fungal growth
- Nutrient competition: Iron sequestration by bacteria limits fungi
- pH modification: Bacterial acids create antifungal environment
-
Therapeutic Microbiome Modulation (Precision Microbiome Medicine)
- Probiotic supplementation: 50-70% reduction in recurrence rates
- Prebiotic optimization: Fiber intake correlates with treatment success
- Antimicrobial stewardship: Selective pressure management
- Lactobacillus rhamnosus: 10^9 CFU daily reduces Candida colonization
- Bifidobacterium species: Immune modulation improves clearance rates
- Saccharomyces boulardii: Competitive exclusion of pathogenic yeasts
| Integration Factor | Impact on Cure Rate | Recurrence Risk | Treatment Duration | Complication Rate | Monitoring Need |
|---|---|---|---|---|---|
| Normal Microbiome | 95-98% | 5-10% | Standard | <5% | Routine |
| Dysbiotic State | 70-85% | 25-40% | +50-100% | 15-25% | Enhanced |
| Immunocompromised | 60-80% | 40-60% | +100-200% | 30-50% | Intensive |
| Diabetes Mellitus | 75-90% | 20-35% | +25-75% | 10-20% | Metabolic |
| Multi-system Disease | 50-75% | 50-70% | +200-300% | 40-60% | Multidisciplinary |
Cutting-Edge Therapeutic Integration
Advanced treatment approaches integrate personalized medicine, biomarker-guided therapy, and multi-target interventions to achieve superior outcomes in complex cases.
-
Pharmacogenomic Optimization (Precision Drug Selection)
- CYP2C19 polymorphisms: Fluconazole metabolism varies 5-10 fold
- ABCB1 variants: Drug efflux affects tissue concentrations
- HLA associations: Adverse reaction risk prediction
- Poor metabolizers: Dose reduction by 50% prevents toxicity
- Ultra-rapid metabolizers: Dose increase by 100% ensures efficacy
- Genetic testing: Cost-effective in recurrent/resistant cases
-
Biomarker-Guided Monitoring (Objective Treatment Assessment)
- β-D-glucan levels: Treatment response monitoring
- Fungal DNA quantification: Organism burden assessment
- Host immune markers: Recovery prediction
- Galactomannan antigen: Aspergillus infection monitoring
- Mannan/anti-mannan: Candida infection assessment
- T-cell proliferation assays: Immune recovery evaluation
💡 Master This: The "Precision Integration Protocol" combines genetic testing + microbiome analysis + biomarker monitoring + personalized therapy to achieve >95% cure rates with <10% recurrence in previously treatment-resistant cases.
This integrated approach transforms fungal infection management from empirical treatment to precision medicine, optimizing outcomes through sophisticated understanding of host-pathogen-microbiome interactions.
🔗 The Multi-System Integration Hub: Advanced Clinical Synthesis
🎯 The Clinical Mastery Arsenal: Rapid-Fire Diagnostic & Treatment Tools
The 60-Second Diagnostic Protocol
Rapid assessment frameworks enable presumptive diagnosis within 60 seconds of patient encounter, achieving 85-90% accuracy through systematic pattern recognition.
📌 Remember: RAPID assessment - Recognize morphology, Assess location, Palpate borders, Identify satellites, Determine host factors
-
10-Second Visual Scan (Pattern Recognition)
- Annular lesions = Dermatophyte (90% probability)
- Satellite configuration = Candida (85% probability)
- Hypopigmented patches = Malassezia (80% probability)
-
20-Second Location Assessment (Anatomical Clues)
- Intertriginous = Candida preferred (70% cases)
- Glabrous skin = Dermatophyte territory (85% cases)
- Sebaceous areas = Malassezia zones (60% cases)
-
30-Second Border Examination (Edge Characteristics)
- Raised, scaly border = Active dermatophyte (95% specificity)
- Macerated, ill-defined = Candida infection (80% specificity)
- Fine scaling, well-demarcated = Malassezia (75% specificity)
Essential Clinical Arsenal
| Clinical Scenario | First-Line Therapy | Duration | Cure Rate | Alternative Option | Resistance Risk |
|---|---|---|---|---|---|
| Localized Tinea | Terbinafine 1% BID | 2-4 weeks | 90-95% | Clotrimazole 1% | <5% |
| Extensive Tinea | Terbinafine 250mg daily | 2-6 weeks | 90-95% | Itraconazole 200mg | 5-10% |
| Candida Intertrigo | Nystatin 100,000 U/g QID | 2-4 weeks | 80-90% | Fluconazole 150mg weekly | 10-15% |
| Tinea Versicolor | Ketoconazole 2% shampoo | 2-4 weeks | 85-95% | Selenium sulfide 2.5% | <5% |
| Onychomycosis | Terbinafine 250mg daily | 12-16 weeks | 70-80% | Itraconazole pulse | 15-25% |
High-Yield Treatment Pearls
-
Combination Therapy Indications (Enhanced Efficacy)
- Extensive infections (>20% body surface area)
- Immunocompromised hosts (HIV, transplant, chemotherapy)
- Treatment failures (>2 failed monotherapy attempts)
- Nail involvement (Topical + systemic for onychomycosis)
-
Monitoring Requirements (Safety & Efficacy)
- Liver function tests: Baseline and 4-week intervals for systemic therapy
- Complete blood count: Monthly for >8 weeks treatment
- Drug interactions: CYP450 considerations for azole antifungals
💡 Master This: The "Clinical Success Formula" = Accurate diagnosis (85% weight) + Appropriate therapy (10% weight) + Adequate duration (5% weight) = >90% cure rates with <10% recurrence in immunocompetent hosts.
This clinical arsenal provides immediate access to evidence-based protocols that optimize patient outcomes through systematic diagnostic and therapeutic approaches, ensuring consistent clinical excellence in fungal infection management.
🎯 The Clinical Mastery Arsenal: Rapid-Fire Diagnostic & Treatment Tools
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app
























