Back
How to Study USMLE Step 1 Immunology: High-Yield Topics, Mnemonics & Exam Strategy 2026
Master USMLE Step 1 immunology with this comprehensive study guide. Learn high-yield topics, essential mnemonics, and proven exam strategies for 2026.

How to Study USMLE Step 1 Immunology: High-Yield Topics, Mnemonics & Exam Strategy 2026
You probably already know that immunology is the subject that separates Step 1 survivors from casualties. Its not just another organ system — its the foundation that connects everything from infectious disease to pharmacology to pathology. Miss immunology concepts, and you'll stumble through 47 questions that could have been easy points.
Here's what most students get wrong: they treat immunology like memorization when its actually pattern recognition. The exam doesnt ask you to recite cytokine functions — it shows you a clinical vignette and expects you to spot the immunological mechanism driving the pathology.
USMLE Step 1 allocates roughly 10-15% of questions to immunology, but these questions have tentacles reaching into every other subject. A cardiology question about myocarditis? That's immunology. A dermatology question about drug reactions? Type II hypersensitivity. An infectious disease question about opportunistic infections? Immunodeficiency.
This guide breaks down exactly what gets tested, which topics deserve your limited study time, and how to build the pattern recognition that turns immunology from a weakness into a strength.
Why Most Students Struggle with Step 1 Immunology
Traditional immunology study fails because it focuses on isolated facts instead of integrated understanding. You memorize that IL-2 comes from Th1 cells, but when the exam presents a patient with recurrent infections and asks about the likely cytokine deficiency, you freeze.
The problem is depth without connection. Students drill individual immune components — complement proteins, cytokine functions, T-cell subsets — without understanding how they work together in disease states. When Oncourse AI's Mnemonic engine generates topic-specific recall chains, students can lock in IL-1 through IL-12, TNF-α and IFN-γ in a single structured pass rather than re-reading the same table repeatedly.
Step 1 immunology questions follow predictable patterns:
Clinical vignette → identify the immune mechanism
Lab values/findings → determine the immunodeficiency
Drug mechanism → predict the immunological effect
Disease progression → understand the inflammatory cascade
Master these patterns, and immunology becomes your competitive advantage.
High-Yield Immunology Topics: Priority Tiers
Not all immunology topics carry equal weight on Step 1. Focus your energy where it counts most.
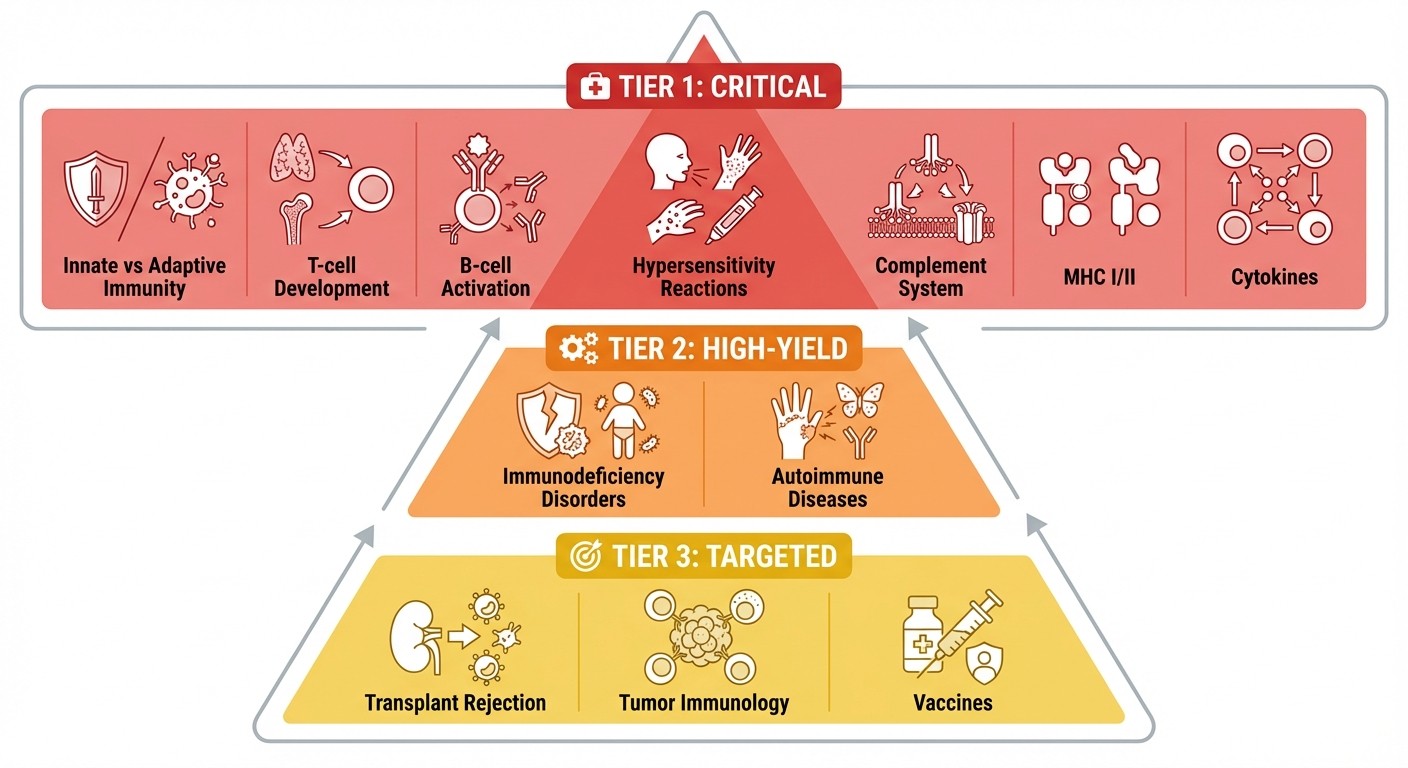
Tier 1: Must-Know Topics (Study These First)
These concepts appear in 60-70% of immunology questions and serve as building blocks for everything else.
Innate vs Adaptive Immunity
The exam loves scenarios that test your understanding of which immune component responds first. Know that innate immunity (neutrophils, macrophages, complement) activates immediately but lacks memory, while adaptive immunity (T-cells, B-cells) takes 3-5 days but creates lasting protection.
Classic exam scenario: Patient with recurrent bacterial infections despite normal T-cell and B-cell counts → think neutrophil defect or complement deficiency.
T-Cell Development and Selection
Positive selection (can the T-cell recognize self-MHC?) occurs in the thymic cortex. Negative selection (does the T-cell react too strongly to self-antigens?) happens in the thymic medulla. This process explains why DiGeorge syndrome (absent thymus) leads to opportunistic infections — no T-cell education center.
When immunology mechanisms like T-cell selection are hard to visualize from text alone, Rezzy (AI tutor in Oncourse) lets students ask follow-up questions directly on any lesson. Students can ask "Why does negative selection happen in the thymus, not periphery?" and get instant, context-aware explanations.
B-Cell Activation and Antibody Class Switching
B-cells need two signals: antigen binding to BCR (signal 1) and T-helper cell cytokines (signal 2). Class switching from IgM to other antibodies requires specific cytokines:
IL-4 → IgE (allergic reactions)
IL-5 → IgA (mucosal immunity)
IFN-γ → IgG (opsonization)
Hypersensitivity Reactions (Types I-IV)
Every Step 1 has multiple hypersensitivity questions. Each type has distinct timing, mechanism, and clinical presentations:
Type | Mechanism | Timing | Classic Example |
|---|---|---|---|
Type I | IgE-mediated | Minutes | Anaphylaxis to penicillin |
Type II | Antibody-mediated | Hours | Hemolytic transfusion reaction |
Type III | Immune complex | Hours to days | SLE nephritis |
Type IV | T-cell mediated | Days | Contact dermatitis |
Complement System
Focus on the three pathways (classical, alternative, lectin) and their clinical relevance. C3 deficiency causes recurrent encapsulated bacterial infections. C5-C9 deficiencies predispose to Neisseria infections. Late complement deficiencies (C6-C9) specifically increase meningococcal susceptibility.
MHC Class I vs Class II
MHC I (found on all nucleated cells) presents intracellular peptides to CD8+ T-cells. MHC II (found on antigen-presenting cells) presents extracellular peptides to CD4+ T-cells. Remember: "MHC I = inside, MHC II = outside."
Key Cytokines and Their Functions
Master these essential cytokines that appear repeatedly on exams:
IL-1: Fever, acute-phase response (from macrophages)
IL-2: T-cell proliferation (from Th1 cells)
IL-4: IgE class switching, Th2 differentiation (from Th2 cells)
IL-5: Eosinophil activation (from Th2 cells)
IL-6: Acute-phase proteins, B-cell maturation (from macrophages)
IL-10: Anti-inflammatory (from Treg cells)
IL-12: Th1 differentiation, NK cell activation (from dendritic cells)
TNF-α: Inflammation, fever, weight loss (from macrophages)
IFN-γ: Macrophage activation, Th1 response (from Th1/NK cells)
Tier 2: High-Yield Topics (Learn After Mastering Tier 1)
Primary Immunodeficiency Disorders
These show up as case-based questions testing your ability to connect clinical presentation with underlying defect.
X-linked agammaglobulinemia (Bruton): No mature B-cells, recurrent bacterial infections after 6 months
SCID: Combined T and B-cell defects, opportunistic infections from birth
DiGeorge syndrome: Absent thymus, recurrent viral/fungal infections plus hypocalcemia
Common variable immunodeficiency (CVID): Late-onset hypogammaglobulinemia
Chronic granulomatous disease (CGD): Defective NADPH oxidase, catalase-positive infections
Chediak-Higashi: Giant lysosomes, recurrent pyogenic infections, partial albinism
Wiskott-Aldrich: Thrombocytopenia, eczema, immunodeficiency
Cards like "DiGeorge syndrome → chromosome 22q11 deletion → absent thymus + parathyroids" stay fresh when you use Oncourse AI's spaced repetition flashcard engine (Synapses), which surfaces weak immunology cards at exactly the right intervals before the exam.
Autoimmune Disease Mechanisms
Understand the immunological basis of major autoimmune conditions:
SLE: Type III hypersensitivity, anti-nuclear antibodies
Rheumatoid arthritis: Rheumatoid factor, anti-CCP antibodies
Multiple sclerosis: T-cell mediated destruction of myelin
Myasthenia gravis: Antibodies against acetylcholine receptors
Graves disease: TSH receptor-stimulating antibodies
Hashimoto thyroiditis: Anti-TPO, anti-thyroglobulin antibodies
Tier 3: Targeted Topics (Study These Last)
Transplant Rejection Types
Hyperacute: Minutes, pre-existing antibodies
Acute cellular: Days to weeks, T-cell mediated
Acute humoral: Weeks, antibody-mediated
Chronic: Months to years, fibrosis and scarring
Tumor Immunology
Focus on immune surveillance mechanisms and how tumors evade detection. Know about tumor-associated antigens and the role of NK cells in tumor surveillance.
Passive vs Active Immunity
Active immunity develops after vaccination or infection. Passive immunity involves transfer of antibodies (maternal antibodies, immunoglobulin therapy).
Essential Immunology Mnemonics for Step 1
Memory devices can make the difference when youre under exam pressure and need instant recall.
Cytokine Sources and Functions: "IL-1 Makes Hot: IL-1 from macrophages causes fever IL-2 T's Please: IL-2 from T-cells stimulates T-cell proliferation IL-4 E's for Allergies: IL-4 causes IgE switching for allergic reactions IL-5 A's for Airways: IL-5 activates eosinophils in asthma IL-6 B's and Bads: IL-6 causes B-cell maturation and bad acute-phase proteins" Hypersensitivity Types: "ACID" for hypersensitivity timing:
Anaphylactic (Type I): Minutes
Cytotoxic (Type II): Hours
Complex-mediated (Type III): Hours-days
Delayed (Type IV): Days
Immunodeficiency Memory Device: "Boys Can't Make (X-linked) B-cells" for X-linked agammaglobulinemia "SCID Kids Can't Survive" for severe combined immunodeficiency "DiGeorge Can't Count (T's)" for T-cell deficiency with thymic aplasia
Proven Study Strategy for Step 1 Immunology
Phase 1: Build the Foundation (Week 1)
Start with cellular mechanisms before jumping into diseases. Understand how normal immune responses work — this makes pathology logical instead of random facts to memorize.
Focus sequence:
1. Innate immunity components and function
2. Adaptive immunity development and activation
3. Antibody structure and class switching
4. Cell-mediated vs humoral immunity
Use immunology lessons to build conceptual understanding before moving to question practice.
Phase 2: Disease Correlation (Week 2)
Now connect immune mechanisms to clinical presentations. This phase transforms immunology from abstract concepts into practical diagnostic tools.
Study approach:
1. Primary immunodeficiencies → learn the classic presentations
2. Hypersensitivity reactions → memorize the prototypical examples
3. Autoimmune diseases → understand the underlying mechanisms
4. Complement deficiencies → know which infections they predispose to
After building the mnemonic foundation, students can immediately test recall using Probe Game — gamified rapid-fire cytokine quizzing that converts passive reading into active retrieval in under 5 minutes.
Phase 3: MCQ Mastery (Week 3-4)
This is where immunology clicks. Practice MCQs reveal the patterns Step 1 uses to test immunological concepts.
High-yield question types to master:
Patient with recurrent infections → identify the immune defect
Drug with immunological side effects → predict the mechanism
Laboratory findings → determine the immunodeficiency type
Clinical scenario → classify the hypersensitivity reaction
Practice with immunology MCQs to build pattern recognition. Focus on questions that integrate immunology with other subjects — these mirror real Step 1 questions.
Phase 4: Weak Spot Elimination (Final Week)
Use spaced repetition to maintain what youve learned while targeting remaining gaps. Review immunology flashcards daily to keep key facts fresh.
Students who combine Synapses for immunodeficiencies with Clinical Rounds case scenarios get both the recall AND the clinical application — covering both presentation recognition and mechanism understanding.
Common Step 1 Immunology Exam Traps
MHC Class Confusion
Trap: Mixing up MHC I and MHC II functions
Reality: MHC I = intracellular peptides → CD8+ cells. MHC II = extracellular peptides → CD4+ cells
Memory aid: "MHC I = I (inside), MHC II = II (outside)"
Hypersensitivity Timing Mistakes
Trap: Confusing Type II and Type III timing
Reality: Type II is antibody-mediated (hours), Type III is immune complex-mediated (hours to days)
Key difference: Type II targets cell surface antigens, Type III involves circulating immune complexes
Cytokine Source Confusion
Trap: Attributing cytokines to wrong cell types
Reality: Know the major sources — IL-1/IL-6/TNF-α from macrophages, IL-2/IFN-γ from Th1 cells, IL-4/IL-5 from Th2 cells
Practice tip: Create source-function cards rather than just function cards
Complement Pathway Mixing
Trap: Confusing classical vs alternative pathway triggers
Reality: Classical = antibody-antigen complexes, Alternative = pathogen surfaces directly, Lectin = mannose-binding lectin
Clinical correlation: Classical defects → SLE-like symptoms, Alternative defects → bacterial infections
Integration with Other Step 1 Subjects
Immunology doesnt exist in isolation on Step 1. High-scoring students connect immunological concepts across subjects:
Immunology + Pharmacology: Understand how immunosuppressive drugs work (cyclosporine blocks IL-2, methotrexate inhibits folate metabolism in rapidly dividing lymphocytes) Immunology + Microbiology: Know which pathogens exploit specific immune defects (Pneumocystis in T-cell deficiencies, encapsulated bacteria in B-cell/complement defects) Immunology + Pathology: Understand inflammatory responses in tissue damage (acute vs chronic inflammation, granulomatous responses)
For comprehensive coverage of related subjects, explore our guides on behavioral science and other Step 1 topics.
Final Week Review Strategy
The week before Step 1, focus on high-yield immunology facts that commonly appear as "gimme" questions:
Daily review checklist:
Cytokine functions and sources (5 minutes)
Immunodeficiency presentations (5 minutes)
Hypersensitivity reaction types (3 minutes)
Complement pathway overview (3 minutes)
MHC class differences (2 minutes)
Red flag topics to review if youve struggled:
DiGeorge syndrome clinical features
X-linked agammaglobulinemia vs CVID differences
Type II vs Type III hypersensitivity mechanisms
Alternative complement pathway initiation
Frequently Asked Questions
How much of Step 1 is immunology?
Immunology comprises approximately 10-15% of USMLE Step 1 questions, but immunological concepts appear throughout other subjects. Expect 20-30 dedicated immunology questions plus another 15-20 questions where immunology knowledge is essential for correct answers.
Should I memorize all cytokine functions?
Focus on the major cytokines (IL-1, IL-2, IL-4, IL-5, IL-6, IL-10, IL-12, TNF-α, IFN-γ) and their primary functions. Know the source cells and main effects rather than exhaustive lists of minor functions.
Which immunodeficiencies are highest yield for Step 1?
X-linked agammaglobulinemia, SCID, DiGeorge syndrome, CVID, and CGD appear most frequently. Know their inheritance patterns, age of onset, types of infections, and key laboratory findings.
How do I remember hypersensitivity reaction types?
Use the "ACID" mnemonic for timing and focus on one classic example for each type. Type I = anaphylaxis, Type II = hemolytic transfusion reaction, Type III = SLE, Type IV = contact dermatitis.
Is complement worth studying in detail?
Yes, but focus on clinical correlations rather than biochemical details. Know which complement deficiencies predispose to specific infections and understand the basic pathway differences.
How should I integrate immunology with other subjects?
Study immunology alongside microbiology and pharmacology. Many Step 1 questions test the intersection of these subjects — like understanding why certain infections occur in specific immunodeficiencies.
Prepare smarter with Oncourse AI — adaptive MCQs, spaced repetition, and AI explanations built for USMLE Step 1. Download free on Android and iOS.