Cardiology — MCQs

On this page
A 65-year-old man comes to the physician because of a 10-day history of episodic retrosternal pain, shortness of breath, and palpitations. The episodes occur when he climbs stairs or tries to walk briskly on his treadmill. The symptoms resolve when he stops walking. The previous evening he felt dizzy and weak during such an episode. He also reports that he had a cold 2 weeks ago. He was diagnosed with type 2 diabetes mellitus four years ago but is otherwise healthy. His only medication is glyburide. He appears well. His pulse is 62/min and is weak, respirations are 20/min, and blood pressure is 134/90 mmHg. Cardiovascular examination shows a late systolic ejection murmur that is best heard in the second right intercostal space. The lungs are clear to auscultation. Which of the following mechanisms is the most likely cause of this patient's current condition?
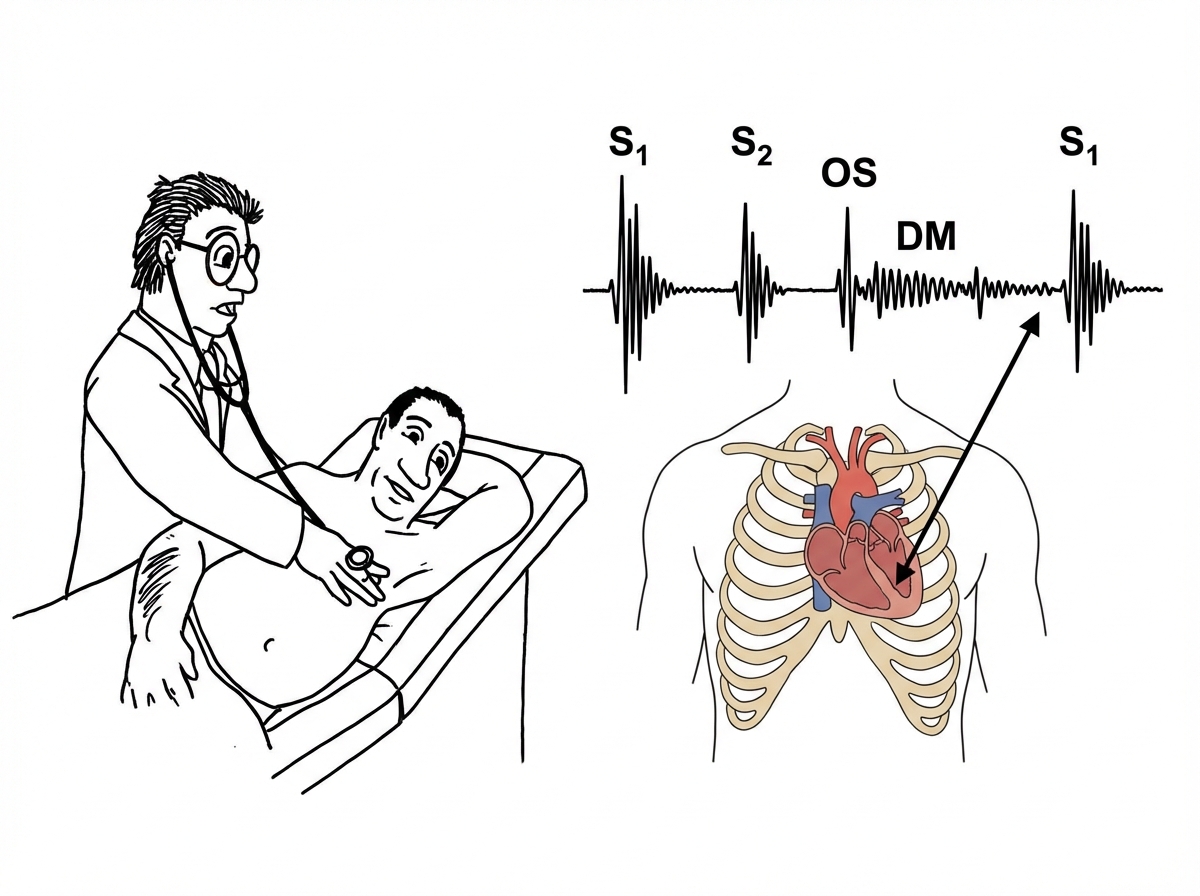
A 48-year-old man comes to the physician because of worsening shortness of breath and nocturnal cough for the past 2 weeks. On two occasions, his cough was bloody. He had a heart condition as a child that was treated with antibiotics. He emigrated to the US from Kazakhstan 15 years ago. Pulmonary examination shows crackles at both lung bases. Cardiac examination is shown. Which of the following is the most likely diagnosis?
A 68-year-old man is brought to the emergency department because of progressive weakness of his lower extremities and urinary incontinence for the past 2 weeks. Over the past 2 months, he has had increasing back pain. His temperature is 37.1°C (98.8°F), pulse is 88/min, and blood pressure is 106/60 mm Hg. Examination shows an ataxic gait. Muscle strength is decreased in bilateral lower extremities. Sensation to pain, temperature, and position sense is absent in the buttocks, perineum, and lower extremities. Ankle clonus is present. Digital rectal examination is unremarkable. An x-ray of the spine shows multiple sclerotic lesions in the thoracic and lumbar vertebrae. Further evaluation of this patient is most likely to show which of the following?
A 47-year-old woman presents to her primary care physician for a wellness checkup. The patient states that she currently feels well and has no complaints. She has failed multiple times at attempting to quit smoking and has a 40 pack-year smoking history. She drinks 4 alcoholic beverages every night. The patient is currently taking a multivitamin and vitamin D supplements. She has also attempted to eat more salmon given that she has heard of its health benefits. Physical exam is notable for back stiffness on mobility testing. The patient states that she frequently has back pain when sitting. Laboratory values are obtained as seen below. Serum: Na+: 139 mEq/L Cl-: 100 mEq/L K+: 4.3 mEq/L HCO3-: 25 mEq/L BUN: 20 mg/dL Glucose: 99 mg/dL Creatinine: 1.1 mg/dL Ca2+: 12.2 mg/dL PTH: 75 pg/mL (normal 10 - 65 pg/mL) Urine: Color: Yellow pH: 7.0 Blood: 1+ Protein: Negative Nitrite: Positive Bacteria: Positive Ca2+: Low Benzodiazepines: Positive Which of the following is the best explanation for this patient’s electrolyte abnormalities?
An 82-year-old man—a retired physics professor—presents with progressive difficulty walking. He has bilateral knee osteoarthritis and has used a walker for the past several years. For the past 6 months, he has experienced problems walking and maintaining balance and has been wheelchair-bound. He has fallen several times, hitting his head a few times but never losing consciousness. He complains of occasional difficulty remembering names and phone numbers, but his memory is otherwise fine. He also complains of occasional incontinence. Physical examination reveals a slow wide-based gait with small steps and intermittent hesitation. He scores 22 out of 30 on the Mini-Mental State Examination (MMSE). A brain MRI demonstrates dilated ventricles with high periventricular fluid-attenuated inversion recovery (FLAIR) signal. A large-volume lumbar puncture improves his gait. Which of the following is the most likely risk factor for the development of this condition?
A 15-year-old girl presents with four days of malaise, painful joints, nodular swelling over her elbows, low-grade fever, and a rash on her chest and left shoulder. Two weeks ago, she complained of a sore throat that gradually improved but was not worked up. She was seen for a follow-up approximately one week later. At this visit her cardiac exam was notable for a late diastolic murmur heard best at the apex in the left lateral decubitus position with no radiation. Which of the following is the best step in the management of this patient?
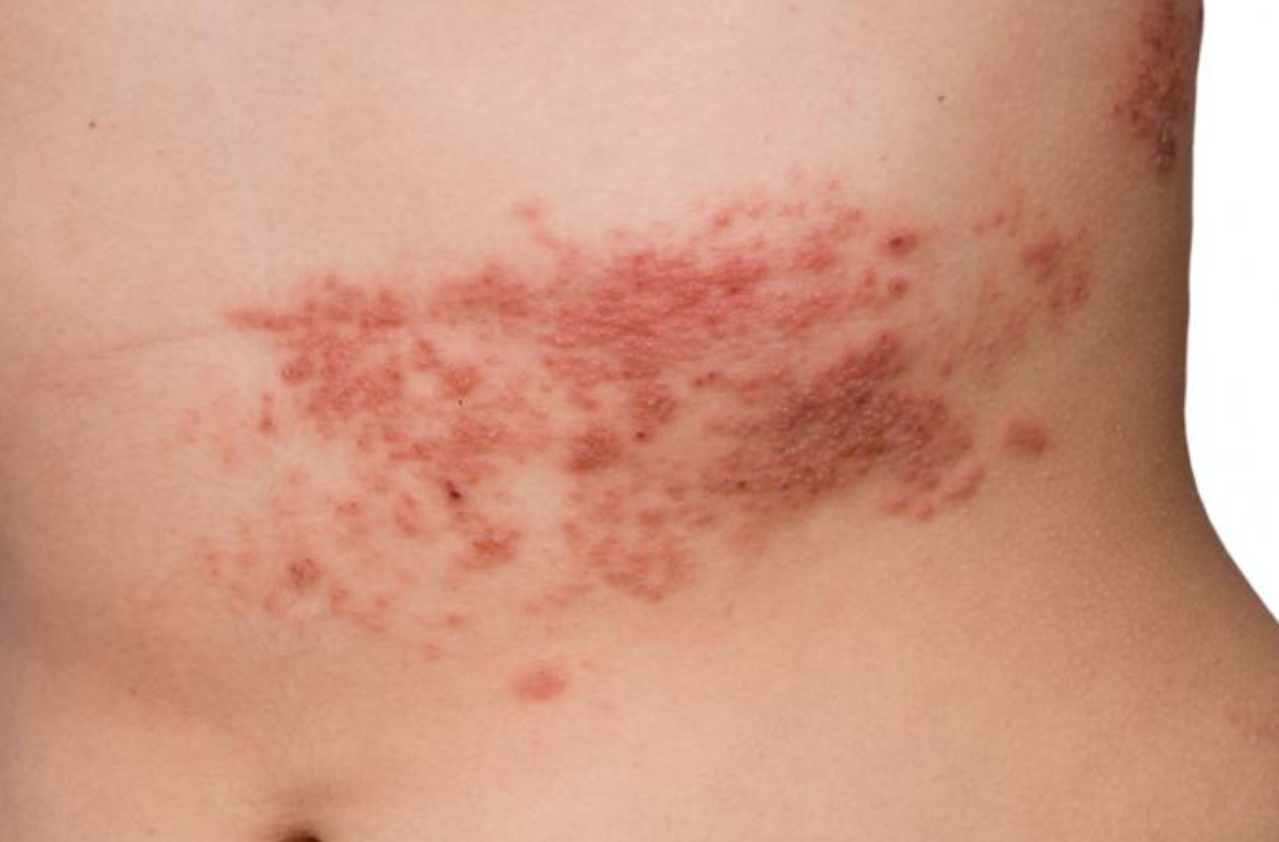
A 30-year-old man comes to the emergency department because of a painful rash for 2 days. The rash initially appeared on his left lower abdomen and has spread to the rest of the abdomen and left upper thigh over the last 24 hours. Pain is exacerbated with movement. He initially thought the skin rash was an allergic reaction to a new laundry detergent, but it did not respond to over-the-counter antihistamines. Six weeks ago, the patient was diagnosed with Hodgkin's lymphoma and was started on doxorubicin, bleomycin, vinblastine, and dacarbazine. He is sexually active with one female partner and uses condoms for contraception. His temperature is 37.9°C (100.2°F), pulse is 80/min, and blood pressure is 117/72 mm Hg. Examination shows two markedly enlarged cervical lymph nodes. A photograph of the rash is shown. Which of the following is the most appropriate next step in management?
A 16-year-old boy comes to the physician with a 4-day history of sore throat and mild fever. He is on the varsity soccer team at his high school, but has been unable to go to practice for the last few days because he has been very tired and is easily exhausted. He has no history of serious illness and takes no medications. His mother has type 2 diabetes mellitus. He appears weak and lethargic. His temperature is 38.7°C (101.7°F), pulse is 84/min, and blood pressure is 116/78 mm Hg. Examination shows enlarged, erythematous, and exudative tonsils; posterior cervical lymphadenopathy is present. Abdominal examination shows no abnormalities. His hemoglobin concentration is 14.5 g/dL and leukocyte count is 11,200/mm3 with 48% lymphocytes. A heterophile antibody test is positive. In addition to supportive therapy, which of the following is the most appropriate next step in management?
A 36-year-old man presents to his physician with the complaint of bilateral lower back pain. The pain is 5/10, constant, aching, aggravated by bending forward and lying supine, and is alleviated by resting in a neutral position. The pain appeared 3 days ago after the patient overstrained at the gym. He does not report changes in sensation or limb weakness. The patient works as a business analyst. The patient’s weight is 88 kg (194 lb), and the height is 186 cm (6 ft 1 in). The vital signs are within normal limits. The neurological examination shows equally normal lower limb reflexes, and preserved muscle tone and power. The paravertebral palpation of the lumbar region increases the pain. Which of the following non-pharmacological interventions is the most appropriate in the presented case?
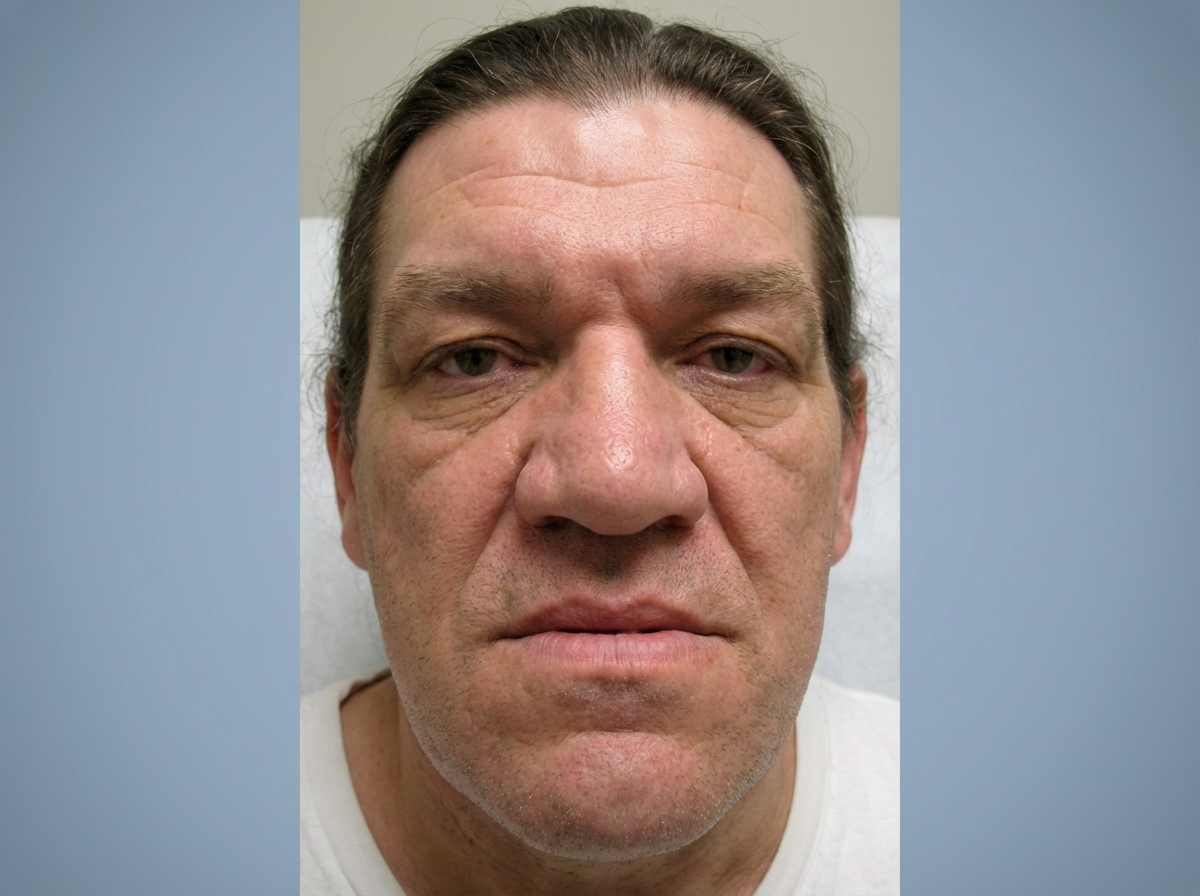
A 46-year-old woman comes to the physician for a routine health maintenance examination. She feels well. She has a history of seizures controlled with levetiracetam. She has needed glasses for the past 13 years. Her father died of pancreatic cancer. She is 175 cm (5 ft 9 in) tall and weighs 79 kg (174 lbs); BMI is 25.8 kg/m2. Vital signs are within normal limits. A photograph of the face is shown. This patient is most likely to be at increased risk for which of the following conditions?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
