Cardiology — MCQs

On this page
A plain CT scan of the patient's head is performed immediately and shows no evidence of hemorrhage. His temperature is 37.1°C (98.8°F), pulse is 101/min and blood pressure is 174/102 mm Hg. Which of the following is the most appropriate next step in management?
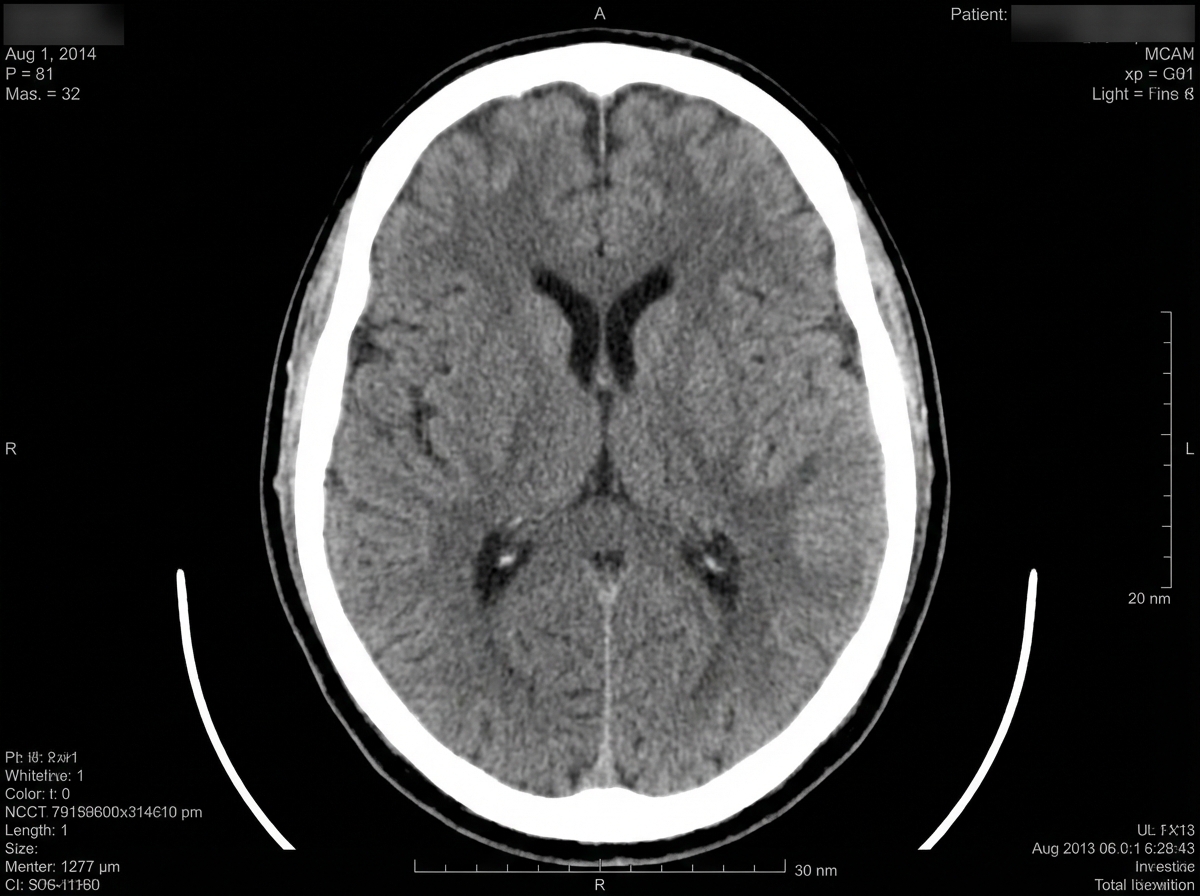
A 74-year-old right-handed woman was referred to the hospital due to concerns of a stroke. In the emergency department, the initial vital signs included blood pressure of 159/98 mm Hg, heart rate of 88/min, and respiratory rate of 20/min. She exhibited paucity of speech and apathy to her condition, although she complied with her physical examination. The initial neurologic evaluation included the following results: Awake, alert, and oriented to person, place, and time No visual field deficits Right-sided gaze deviation with full range of motion with doll’s head maneuver No facial asymmetry Grossly intact hearing No tongue deviation, equal palatal elevation, and good guttural sound production Absent pronator or lower extremity drift Decreased sensation to light touch on the right leg Normal appreciation of light touch, pressure, and pain Normal proprioception and kinesthesia Manual muscle testing: 5+ right and left upper extremities 5+ right hip, thigh, leg, and foot 3+ left hip and thigh 2+ left leg and foot A head computed tomography (CT) scan and a head magnetic resonance imaging (MRI) confirmed areas of ischemia. Which artery is the most likely site of occlusion?
A 34-year-old woman presents with fatigue, depressed mood, weight gain, and constipation. She gradually developed these symptoms over the past 6 months. She is G2P2 with the last pregnancy 9 months ago. She had a complicated delivery with significant blood loss requiring blood transfusions. She used to have a regular 28-day cycle but notes that recently it became irregular with duration lasting up to 40 days, more pain, and greater blood loss. She does not report any chronic conditions, and she is not on any medications. She is a current smoker with a 10-pack-year history. Her blood pressure is 130/80 mm Hg, heart rate is 54/min, respiratory rate is 11/min, and temperature is 35.8°C (96.4°F). Her skin is dry and pale with a fine scaling over the forearms and shins. There is a mild, non-pitting edema of the lower legs. Her lungs are clear to auscultation. Cardiac auscultation does not reveal any pathological sounds or murmurs although S1 and S2 are dulled at all points of auscultation. The abdomen is mildly distended and nontender on palpation. Neurological examination is significant for decreased deep tendon reflexes. Her blood tests show the following results: Erythrocytes count 3.4 million/mm3 Hb 12.2 mg/dL MCV 90 μm3 Reticulocyte count 0.3% Leukocyte count 5,600/mm3 Serum vitamin B12 210 ng/mL T4 total 1.01 μg/dL T4 free 0.6 ng/dL TSH 0.2 μIU/mL Which of the following lab values should be used to monitor treatment in this patient?
A 38-year-old woman presents with worsening fatigue and difficulty talking for the last few hours. Past medical history is significant for type 2 diabetes mellitus, managed with metformin and insulin. Additional current medications are a pill to ''calm her nerves'' that she takes when she has to perform live on stage for work. On physical examination, the patient is lethargic, easily confused, and has difficulty responding to questions or commands. There is also significant diaphoresis of the face and trunk present. Which of the following is the most likely etiology of this patient’s current symptoms?
A 67-year-old woman comes to the clinic complaining of progressive fatigue over the past 4 months. She noticed that she is feeling increasingly short of breath after walking the same distance from the bus stop to her home. She denies chest pain, syncope, lower extremity edema, or a cough. She denies difficulty breathing while sitting comfortably, but she has increased dyspnea upon walking or other mildly strenuous activity. Her past medical history includes mild osteoporosis and occasional gastric reflux disease. She takes oral omeprazole as needed and a daily baby aspirin. The patient is a retired accountant and denies smoking history, but she does admit to 1 small glass of red wine daily for the past 5 years. Her diet consists of a Mediterranean diet that includes fruits, vegetables, and fish. She states that she has been very healthy previously, and managed her own health without a physician for the past 20 years. On physical examination, she has a blood pressure of 128/72 mm Hg, a pulse of 87/min, and an oxygen saturation of 94% on room air. HEENT examination demonstrates mild conjunctival pallor. Lung and abdominal examinations are within normal limits. Heart examination reveals a 2/6 systolic murmur at the right upper sternal border. The following laboratory values are obtained: Hematocrit 29% Hemoglobin 9.8 g/dL Mean red blood cell volume 78 fL Platelets 240,000/mm3 White blood cells 6,000/mm3 What is the most likely reticulocyte range for this patient?
A 20-year-old female with type I diabetes mellitus presents to the emergency department with altered mental status. Her friend said that she has been out late either studying for upcoming tests or attending prayer group meetings. As far as the friend can recollect, the patient appeared to be in her usual state of health until only two days ago, when she was prescribed trimethoprim-sulfamethoxazole for a urinary tract infection. The patient complained that the medication was making her feel nauseous and bloated. The patient also relies on glargine and lispro for glycemic control. Her temperature is 100.5°F (38.1°C), blood pressure is 95/55 mmHg, pulse is 130/min, and respirations are 30/min. Her pupils are equal and reactive to light bilaterally. The remainder of the physical exam is unremarkable. Her basic metabolic panel is displayed below: Serum: Na+: 116 mEq/L Cl-: 90 mEq/L K+: 5.0 mEq/L HCO3-: 2 mEq/L BUN: 50 mg/dL Glucose: 1,200 mg/dL Creatinine: 1.5 mg/dL Which of the following is true regarding this patient's presentation?
A 36-year-old man presents to his physician with an acute burning retrosternal sensation with radiation to his jaw. This sensation began 20 minutes ago when the patient was exercising at the gym. It does not change with position or with a cough. The patient’s vital signs include: blood pressure is 140/90 mm Hg, heart rate is 84/min, respiratory rate is 14/min, and temperature is 36.6℃ (97.9℉). Physical examination is only remarkable for paleness and perspiration. The patient is given sublingual nitroglycerin, the blood is drawn for an express troponin test, and an ECG is going to be performed. At the moment of performing ECG, the patient’s symptoms are gone. ECG shows increased R amplitude in I, II V3-V6, and ST depression measuring for 0.5 mm in the same leads. The express test for troponin is negative. Which of the following tests would be reasonable to perform next to confirm a diagnosis in this patient?
A 46-year-old woman complains of chronic cough for the past 3 weeks. She was recently diagnosed with hypertension and placed on an angiotensin receptor blocker therapy (ARBs). Chest X-ray shows large nodular densities bilaterally. Bronchial biopsy showed granulomatous inflammation of the pulmonary artery. Lab investigations showed a positive cANCA with a serum creatinine of 3.6 mg/dL. Urine analysis shows RBC casts and hematuria. Which is the most likely cause of this presentation?
A 67-year-old man presents to your office with a chief complaint of constipation and many other perturbing minor medical concerns. He reports tiring easily, which he attributes to old age and years of persistent pain in his back and ribs. A complete blood count shows low hemoglobin and elevated serum creatinine. A peripheral blood smear shows stacks of red blood cells among other findings, and serum electropheresis reveals an abnormal concentration of protein resulting in a spike. Which of the following additional findings would you expect to see in this patient?
A 55-year-old woman presents to a primary care clinic for a physical evaluation. She works as a software engineer, travels frequently, is married with 2 kids, and drinks alcohol occasionally. She does not exercise regularly. She currently does not take any medications except for occasional ibuprofen or acetaminophen. She is currently undergoing menopause. Her initial vital signs reveal that her blood pressure is 140/95 mmHg and heart rate is 75/min. She weighs 65 kg (143 lb) and is 160 cm (63 in) tall. Her physical exam is unremarkable. A repeat measurement of her blood pressure is the same as before. Among various laboratory tests for hypertension evaluation, the physician requests fasting glucose and hemoglobin A1c levels. Which of the following is the greatest risk factor for type 2 diabetes mellitus?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
