Cardiology — MCQs

On this page
An x-ray of the chest shows an extensive consolidation within the right lower lobe consistent with lobar pneumonia. Sputum and blood cultures are sent to the laboratory for analysis, and empiric antibiotic treatment with intravenous cefotaxime is begun. Which of the following is most likely to have prevented this patient's pneumonia?
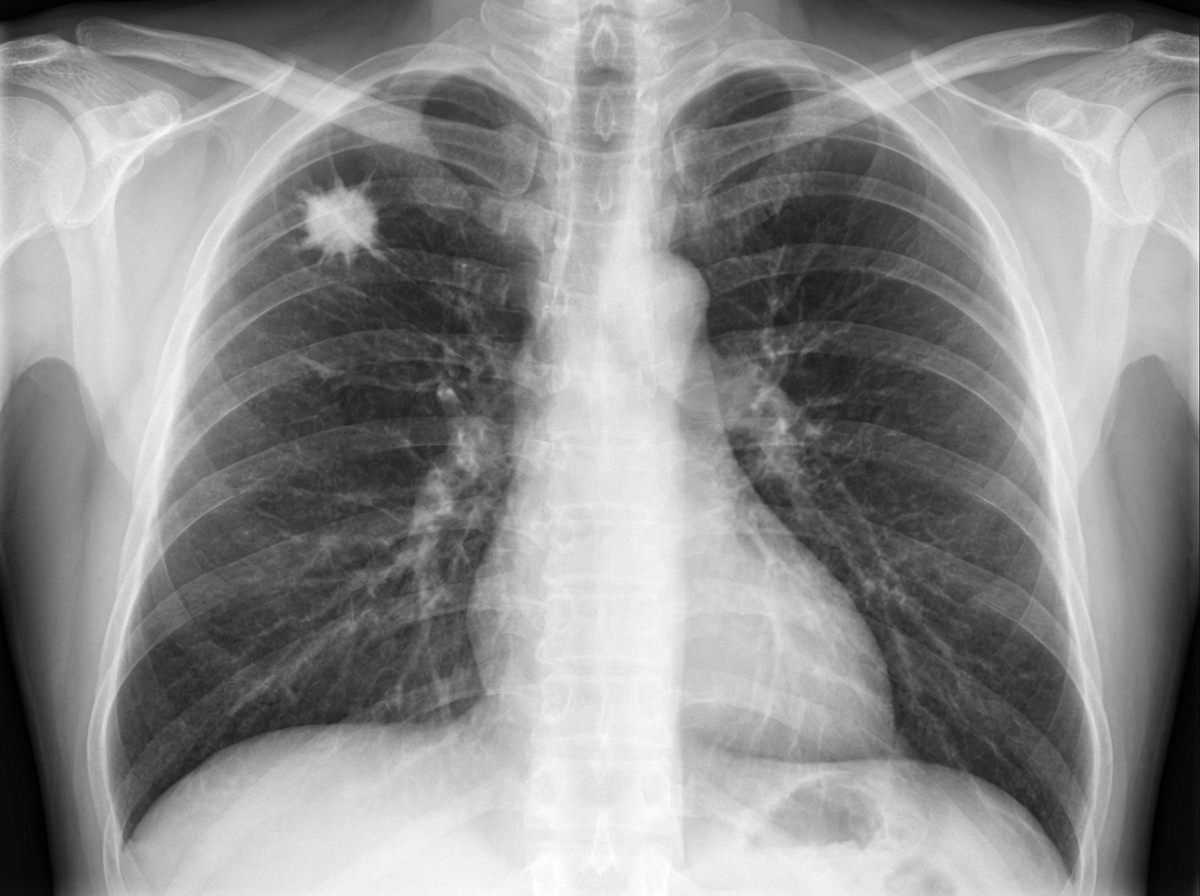
A 62-year-old man comes to the physician because of a persistent cough for the past 2 weeks. During this time, he has also had occasional discomfort in his chest. Three weeks ago, he had a sore throat, headache, and a low-grade fever, which were treated with acetaminophen and rest. He has a history of hypertension and hyperlipidemia. His father died of myocardial infarction at the age of 57 years. He has smoked a pack of cigarettes daily for the past 40 years. Current medications include enalapril and atorvastatin. His temperature is 37°C (98.6°F), pulse is 70/min, and blood pressure is 145/90 mm Hg. Physical examination shows no abnormalities. An x-ray of the chest is shown. Which of the following is the most appropriate next step in management?
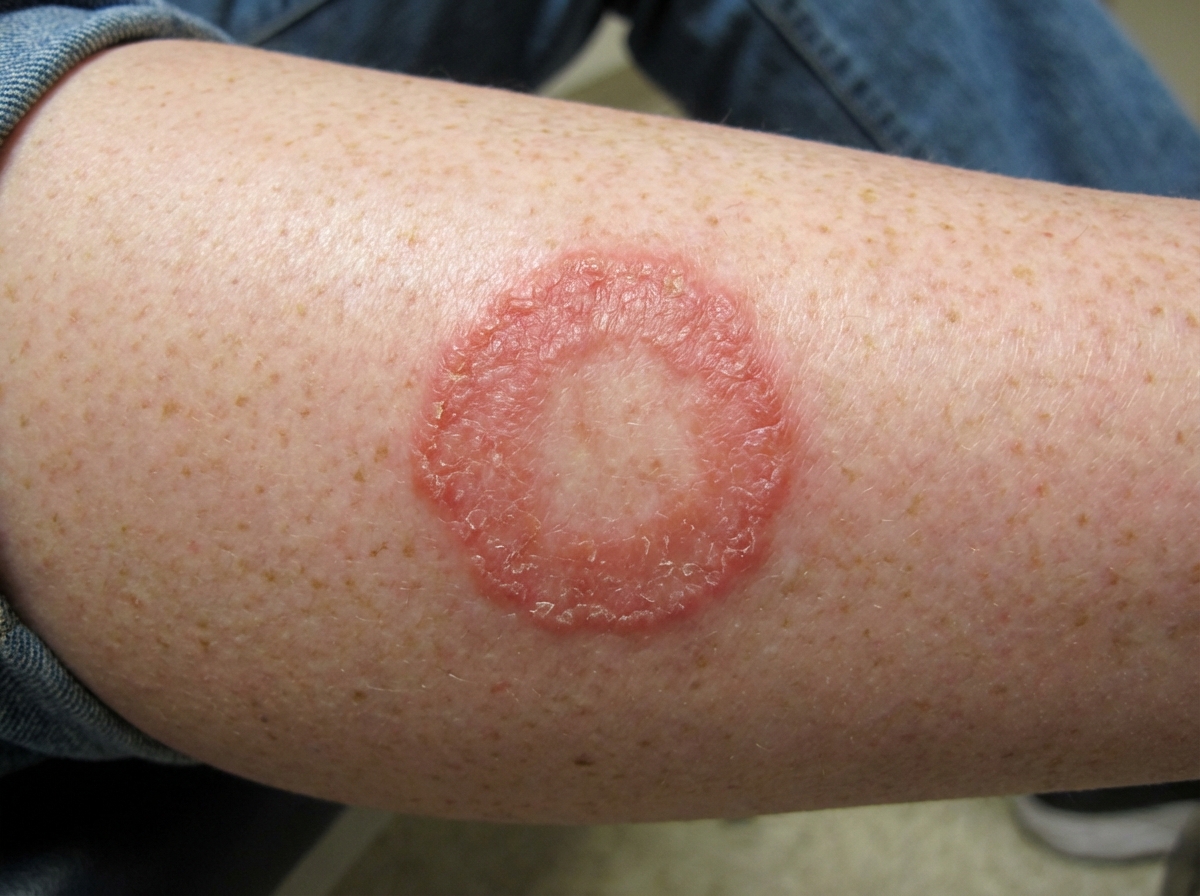
A 35-year-old man comes to the physician because of a rash on the thigh for 10 days. He reports that the rash has been enlarging and is intensely itchy. Two weeks ago, he adopted a stray dog from an animal shelter. Vital signs are within normal limits. A photograph of the examination findings is shown. Which of the following is the most likely cause of this patient's symptoms?
A 74-year-old African-American woman is brought to the emergency department by her home health aid. The patient was eating breakfast this morning when she suddenly was unable to lift her spoon with her right hand. She attempted to get up from the table, but her right leg felt weak. One hour later in the emergency department, her strength is 0/5 in the right upper and right lower extremities. Strength is normal in her left upper and lower extremities. Sensation is normal bilaterally. An emergency CT of the head does not show signs of hemorrhage. Subsequent brain MRI shows an infarct involving the internal capsule. Which of the following is true about her disease process?
A 68-year-old man is admitted to the intensive care unit after open abdominal aortic aneurysm repair. The patient has received 4 units of packed red blood cells during the surgery. During the first 24 hours following the procedure, he has only passed 200 mL of urine. He has congestive heart failure and hypertension. Current medications include atenolol, enalapril, and spironolactone. He appears ill. His temperature is 37.1°C (98.8°F), pulse is 110/min, respirations are 18/min, and blood pressure is 110/78 mm Hg. Examination shows dry mucous membranes and flat neck veins. The remainder of the examination shows no abnormalities. Laboratory studies show a serum creatinine level of 2.0 mg/dL and a BUN of 48 mg/dL. His serum creatinine and BUN on admission were 1.2 mg/dL and 18 mg/dL, respectively. Further evaluation of this patient is most likely to reveal which of the following findings?
A 15-year-old girl is hospitalized because of increased fatigue and weight loss over the past 2 months. The patient has no personal or family history of a serious illness. She takes no medications, currently. Her blood pressure is 175/74 mm Hg on the left arm and 90/45 on the right. The radial pulse is 84/min but weaker on the right side. The femoral blood pressure and pulses show no abnormalities. Temperature is 38.1℃ (100.6℉). The muscles over the right upper arm are slightly atrophic. The remainder of the examination reveals no abnormalities. Laboratory studies show the following results: Hemoglobin 10.4 g/dL Leukocyte count 5,000/mm3 Erythrocyte sedimentation rate 58 mm/h Magnetic resonance arteriography reveals irregularity, stenosis, and poststenotic dilation involving the proximal right subclavian artery. Prednisone is initiated with improvement of her symptoms. Which of the following is the most appropriate next step in the patient management?
A 37-year-old woman accompanied by her husband presents to the emergency department after loss of consciousness 30 minutes ago. The husband reports that she was sitting in a chair at home and began having sustained rhythmic contractions of all 4 extremities for approximately 1 minute. During transport via ambulance she appeared confused but arousable. Her husband reports she has no medical conditions, but for the past 2 months she has occasionally complained of episodes of sweating, palpitations, and anxiety. Her brother has epilepsy and her mother has type 1 diabetes mellitus. Laboratory studies obtained in the emergency department demonstrate the following: Serum: Na+: 136 mEq/L K+: 3.8 mEq/L Cl-: 100 mEq/L HCO3-: 19 mEq/L BUN: 16 mg/dL Creatinine: 0.9 mg/dL Glucose: 54 mg/dL C-peptide: Low Which of the following is the most likely diagnosis?
A 26-year-old man presents to his primary care physician complaining of impotence. He reports that he has a healthy, long-term relationship with a woman whom he hopes to marry, but he is embarrassed that he is unable to have an erection. Which of the following is the next best step?
A 75-year-old man comes to the physician because of a 4-month history of progressive shortness of breath and chest pressure with exertion. Cardiac examination shows a crescendo-decrescendo systolic murmur that is heard best in the second right intercostal space. Radial pulses are decreased and delayed bilaterally. Transesophageal echocardiography shows hypertrophy of the left ventricle and a thick, calcified aortic valve. The area of the left ventricular outflow tract is 30.6 mm2. Using continuous-wave Doppler measurements, the left ventricular outflow tract velocity is 1.0 m/s, and the peak aortic valve velocity is 3.0 m/s. Which of the following values most closely represents the area of the stenotic aortic valve?
A 53-year-old woman comes to the physician because of progressive headache and fatigue for the past 2 months. One year ago, she was diagnosed with Cushing disease, which was ultimately treated with bilateral adrenalectomy. Current medications are hydrocortisone and fludrocortisone. Examination shows generalized hyperpigmentation of the skin and bitemporal visual field defects. Serum studies show an ACTH concentration of 1250 pg/mL (N = 20–100). Which of the following is the most appropriate next step in management?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
