Cardiology — MCQs

On this page
A 65-year-old man comes to the physician because of fatigue and nausea for 1 week. Over the past six months, he has had to get up twice every night to urinate. Occasionally, he has had discomfort during urination. He has arterial hypertension. His father died of renal cell carcinoma. Current medications include ramipril. His temperature is 37.3°C (99.1°F), pulse is 88/min, and blood pressure is 124/78 mm Hg. The abdomen is soft and nontender. Cardiac and pulmonary examinations show no abnormalities. Rectal examination shows a symmetrically enlarged and smooth prostate. Serum studies show: Hemoglobin 14.9 g/dL Leukocyte count 7500/mm3 Platelet count 215,000/mm3 Serum Na+ 136 mEq/L Cl- 101 mEq/L K+ 4.9 mEq/L HCO3- 23 mEq/L Glucose 95 mg/dL Urea nitrogen 25 mg/dL Creatinine 1.9 mg/dL PSA 2.1 ng/mL (normal <4 ng/mL) Urine Blood negative Protein 1+ Glucose negative RBC casts negative Which of the following is the most appropriate next step in management?
A 33-year-old woman presents to the clinic complaining of a 9-month history of weight loss, fatigue, and a general sense of malaise. She additionally complains of an unusual sensation in her chest upon rapidly rising from a supine to a standing position. Current vitals include a temperature of 36.8°C (98.2°F), pulse of 72/min, blood pressure of 118/63 mm Hg, and a respiratory rate of 15/min. Her BMI is 21 kg/m2. Auscultation demonstrates an early-mid diastole low-pitched sound at the apex of the heart. A chest X-ray reveals a poorly demarcated abnormality in the heart and requires CT imaging for further analysis. What would most likely be seen on CT imaging?
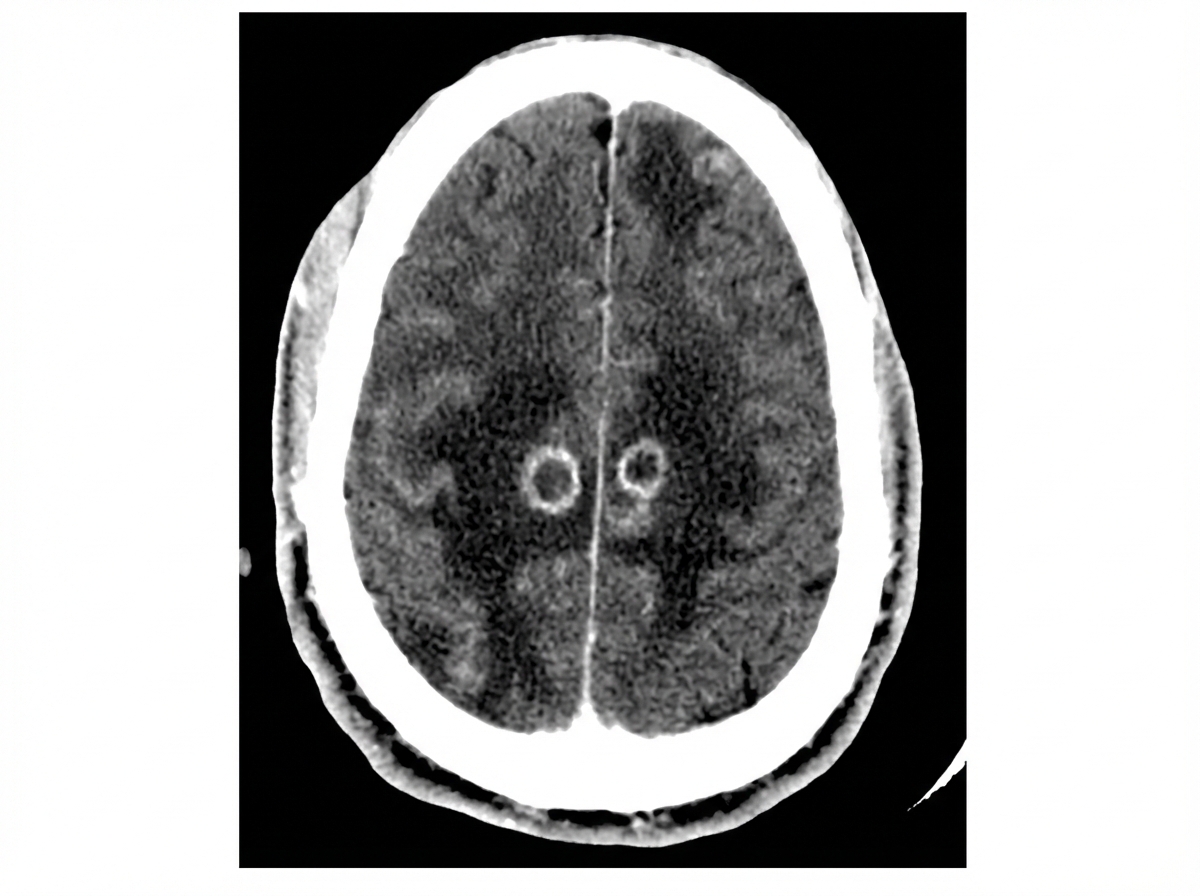
A 32-year-old HIV positive female known to be non-adherent to her treatment regimen, presents to the hospital with the complaint of new-onset headaches. Her vital signs are only significant for a low-grade fever. Neurological examination reveals right-sided upper motor neuron signs, as well as inattention and difficulty with concentration. The patient currently does not have a primary medical provider. A CT of the patients head is shown in the image below. What is the next best step in management for this patient?
A 23-year-old woman presents to the emergency department with pain and frequent urination. She states she has felt uncomfortable with frequent small-volume urinary voids for the past 3 days, which have progressively worsened. The patient has no past medical history. She currently smokes 1 pack of cigarettes per day and engages in unprotected sex with 2 male partners. Her temperature is 103°F (39.4°C), blood pressure is 127/68 mmHg, pulse is 97/min, respirations are 17/min, and oxygen saturation is 98% on room air. Cardiac, pulmonary, and abdominal exams are within normal limits. There is tenderness upon palpation of the left costovertebral angle and the left flank. Urine is collected and a pregnancy test is negative. Which of the following is the best next step in management?
A 47-year-old man with a history of diabetes mellitus presents for a primary care visit. His diabetes is well controlled on metformin, with fasting glucose concentrations between 110–150 mg/dl. His blood pressure on multiple office visits are between 115-130/75-85 mmHg. Today his temperature is 98°F (36.7 °C), blood pressure is 125/80 mmHg, pulse is 86/min, and respirations are 15/min. Labs are obtained with the following results: Hemoglobin A1c: 6.7% Glucose: 120 mg/dl Cholesterol (plasma): 190 mg/dL Urine albumin: 60mg/24hr Which of the following treatments is effective in slowing the progression of the most likely cause of this patient's abnormal albumin result?
A 45-year-old chronic smoker presents to the physician with a complaint of worsening left shoulder pain for several months which has become acutely worse the past 2 weeks and now radiates down his left arm. Physical examination reveals a palpable 2 x 1.5 cm supraclavicular lymph node along with decreased grip strength in his left hand. Examination of the face reveals partial ptosis of the left eyelid and miosis of the left eye. Laboratory testing shows the following values: Sodium (Na+) 135 mEq/L Potassium (K+) 3.6 mEq/L Chloride (Cl-) 100 mEq/L BUN 12 mg/dL Creatinine (Cr) 0.6 mg/dL Magnesium (Mg2+) 1.5 mg/dL Phosphate 3 mg/dL Calcium (Ca2+) 8.5 mg/dL An X-ray of the chest reveals a soft tissue mass at the apex of the left lung with possible involvement of the first rib. What is the most likely diagnosis?
A 33-year-old Honduran woman presents to your clinic with shortness of breath. She reports that her symptoms have progressed over the past several months and are now impacting her quality of life because she cannot complete her usual exercise routine. She recalls "normal" childhood illnesses, including sore throats and fevers, but never required hospitalization. Vital signs are temperature 37 degrees Celsius, blood pressure 110/70 mm Hg, heart rate 109/min, respiratory rate 22/min, and oxygen saturation 98% on room air. Physical exam reveals a holosystolic, high-pitched, blowing murmur at the cardiac apex. One would expect that this murmur would also:
A 32-year-old man comes to the emergency department because of worsening shortness of breath and a productive cough for 3 days. He sustained trauma to the right hemithorax during a fight 3 weeks ago. He had significant pain and mild shortness of breath following the incident but did not seek medical care. He does not smoke or drink alcohol. He is a construction worker. His temperature is 38.4°C (101.1°F), pulse is 95/min, respirations are 18/min, and blood pressure is 120/75 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 96%. Pulmonary examination shows decreased breath sounds over the right lower lung fields. CT scan of the chest shows fractures of the right 7th and 8th ribs, right pleural splitting and thickening, and a dense fluid collection in the pleural space. Which of the following is the most likely diagnosis?
A 23-year-old man comes to the emergency department for 2 days of severe headaches. The pain is most intense on his left forehead and eye. He had similar symptoms last summer. He has been taking indomethacin every 6 hours for the last 24 hours but has not had any relief. He has smoked 1 pack of cigarettes daily for the past 5 years. He works as an accountant and describes his work as very stressful. Physical examination shows drooping of the left eyelid, tearing of the left eye, and rhinorrhea. The left pupil is 2 mm and the right pupil is 4 mm. There is localized tenderness along the right supraspinatus muscle. The remainder of the examination shows no abnormalities. Which of the following is the most likely diagnosis?
A 22-year-old patient presents to the rural medicine clinic for a physical examination. She has a past medical history of major depressive disorder. The patient has a history of smoking 1 pack of cigarettes daily for 5 years. She states that she is not currently sexually active, but had sexual intercourse in the past. Her paternal grandfather died of a heart attack at the age of 60. She takes citalopram by mouth once every morning. The blood pressure is 110/70 mm Hg, the heart rate is 76/min, and the respiratory rate is 12/min. Her physical examination reveals a well-nourished, alert, and oriented female. While auscultating the heart, a 2/6 holosystolic murmur at the left upper sternal border is present. Which of the following would be the most appropriate next step for this patient?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
