Cardiology — MCQs

On this page
A 32-year-old man presents to the physician for a check-up as part of his immigration application. On auscultation, there is a mild rumble heard at the cardiac apex preceded by an opening snap. His blood pressure is 132/76 and heart rate is 78/min. The patient suffers from occasional asthma attacks but has noticed that he becomes short of breath on exertion over the past 2 years. He is otherwise healthy. He does not recall if he had any serious infections during childhood, and there is no family history of congenital diseases. Which of the following could have been used to prevent the development of this condition?
A 29-year-old nulliparous woman is found upon transthoracic echocardiography to have a dilated aorta and mitral valve prolapse. The patient has a history of joint pain, and physical examination reveals pectus excavatum and stretch marks on the skin. She does not take any medications and has no history of past drug use. The patient’s findings are most likely associated with which of the following underlying diagnoses?
A 40-year-old man comes to the physician for the evaluation of episodic headaches for 5 months. The headaches involve both temples and are 4/10 in intensity. The patient has been taking acetaminophen, but the headaches did not subside. He has also had visual disturbances, including double vision. He has no nausea, temperature intolerance, or weight changes. The patient does not smoke. He drinks 2–3 beers on weekends. He appears pale. His temperature is 37°C (98.6°F), pulse is 75/min, and blood pressure 125/80 mm Hg. Ophthalmologic examination shows impaired peripheral vision bilaterally. An MRI scan of the head with contrast shows a 16 × 11 × 9 mm intrasellar mass. Further evaluation is most likely to show which of the following findings?
A 24-year-old woman comes to the physician because of progressively worsening joint pain. She has had diffuse, aching pain in her knees, shoulders, and hands bilaterally for the past few months, but the pain has become much more severe in the past few weeks. She also reports night sweats and generalized malaise. On physical examination, radial and pedal pulses are weak. There are erythematous nodules over the legs that measure 3–5 cm. Laboratory studies show: Hematocrit 33.2% Hemoglobin 10.7 g/dL Leukocyte count 11,300/mm3 Platelet count 615,000/mm3 Erythrocyte sedimentation rate 94 mm/h Serum C-reactive protein 40 mg/dL (N=0.08–3.1) Which of the following is the most likely diagnosis?
A 55-year-old man presents to the physician with a cough which he has had for the last 5 years. He also mentions that he has been feeling breathless when playing any active sport for the last 1 year. He is a manager in a corporate company and has been a regular smoker for 10 years. He has visited multiple physicians and undergone multiple diagnostic evaluations, without permanent benefit. On physical examination his temperature is 37.0°C (98.6°F), the heart rate is 88/min, the blood pressure is 122/80 mm Hg, and the respiratory rate is 20/min. Inspection suggests a barrel chest and auscultation reveals the presence of bilateral end-expiratory wheezing and scattered rhonchi. He undergoes a detailed diagnostic evaluation which includes a complete blood count, chest radiogram, arterial blood gas analysis, and pulmonary function tests, all of which confirm a diagnosis of chronic obstructive lung disease. After analyzing all the clinical information and diagnostic workup, the physician differentiates between emphysema and chronic bronchitis based on a single clue. Which of the following is the most likely clue that helped the physician in making the differential diagnosis?
A 60-year-old man comes to the emergency department because of nausea, headache, and generalized fatigue for 2 days. He has not vomited. He was diagnosed with small cell lung cancer and liver metastases around 3 months ago and is currently receiving chemotherapy with cisplatin and etoposide. His last chemotherapy cycle ended one week ago. He has chronic obstructive lung disease and type 2 diabetes mellitus. Current medications include insulin and a salmeterol-fluticasone inhaler. He appears malnourished. He is oriented to time, place, and person. His temperature is 37.1°C (98.8°F), pulse is 87/min, respirations are 13/min, and blood pressure is 132/82 mm Hg. There is no edema. Examination shows decreased breath sounds over the left lung. Cardiac examination shows an S4. The abdomen is soft and nontender. Neurological examination shows no focal findings. Laboratory studies show: Hemoglobin 11.6 g/dL Leukocyte count 4,300/mm3 Platelet count 146,000/mm3 Serum Na+ 125 mEq/L Cl− 105 mEq/L K+ 4.5 mEq/L HCO3− 24 mEq/L Glucose 225 mg/dL Total bilirubin 1.1 mg/dL Alkaline phosphatase 80 U/L Aspartate aminotransferase (AST, GOT) 78 U/L Alanine aminotransferase (ALT, GPT) 90 U/L Further evaluation of this patient is likely to show which of the following sets of laboratory findings? (Serum osmolality / Urine osmolality / Urinary sodium excretion)
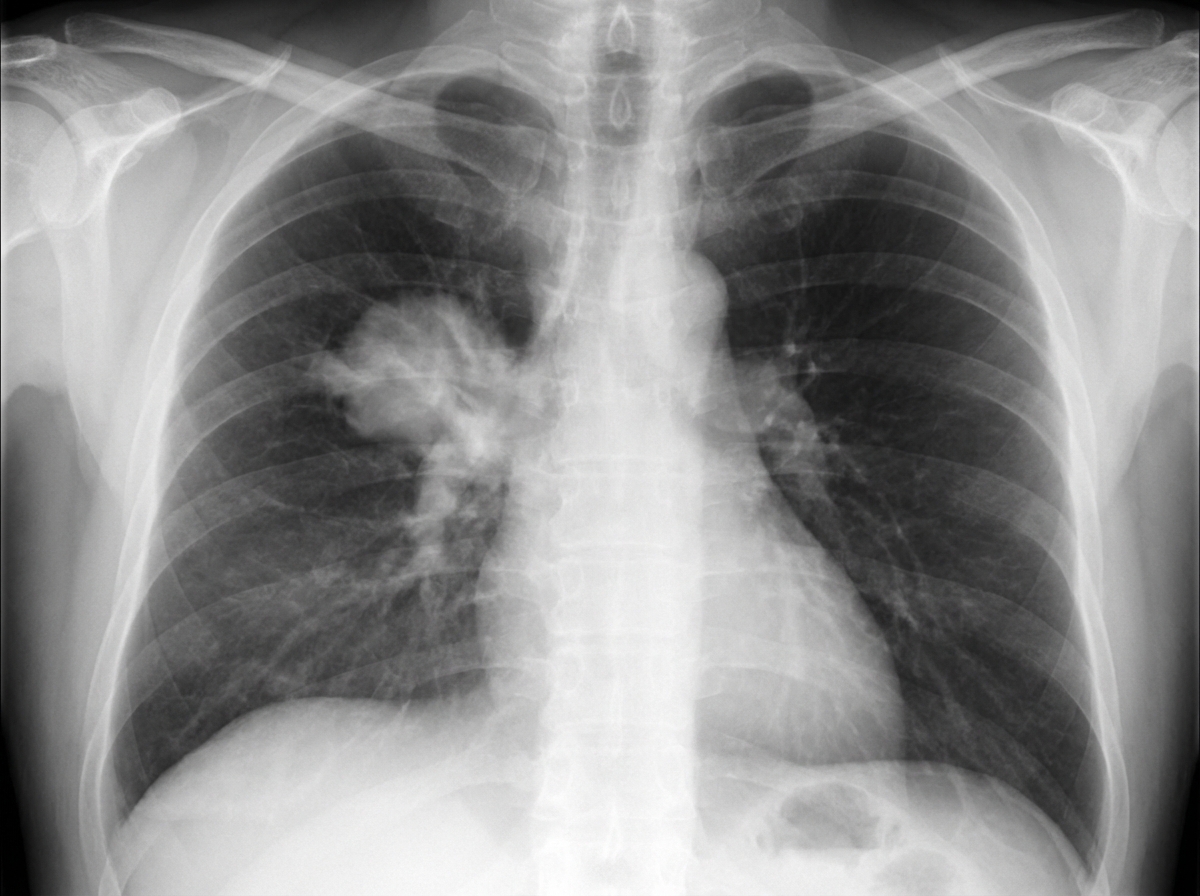
A 71-year-old woman comes to the physician because of a 4-month history of worsening cough and a 4.5-kg (10-lb) weight loss. She has smoked one pack of cigarettes daily for 35 years. Physical examination shows wheezing over the right lung fields. Laboratory studies show a serum calcium concentration of 12.5 mg/dL. X-rays of the chest are shown. Which of the following is the most likely diagnosis?
A 19-year-old Caucasian college student is home for the summer. Her parents note that she has lost quite a bit of weight. The daughter explains that the weight loss was unintentional. She also notes an increase in thirst, hunger, and urine output. Her parents decide to take her to their family physician, who suspects finding which of the following?
A 14-year-old boy is brought to the physician for generalized fatigue and mild shortness of breath on exertion for 3 months. He has a history of recurrent patellar dislocations. He is at the 99th percentile for height and at the 30th percentile for weight. His temperature is 37°C (98.6°F), pulse is 99/min, and blood pressure is 140/50 mm Hg. Examination shows scoliosis, a protruding breast bone, thin extremities, and flat feet. Ocular examination shows upwards displacement of bilateral lenses. A grade 3/6 early diastolic murmur is heard along the left sternal border. Further evaluation of this patient is most likely to show which of the following?
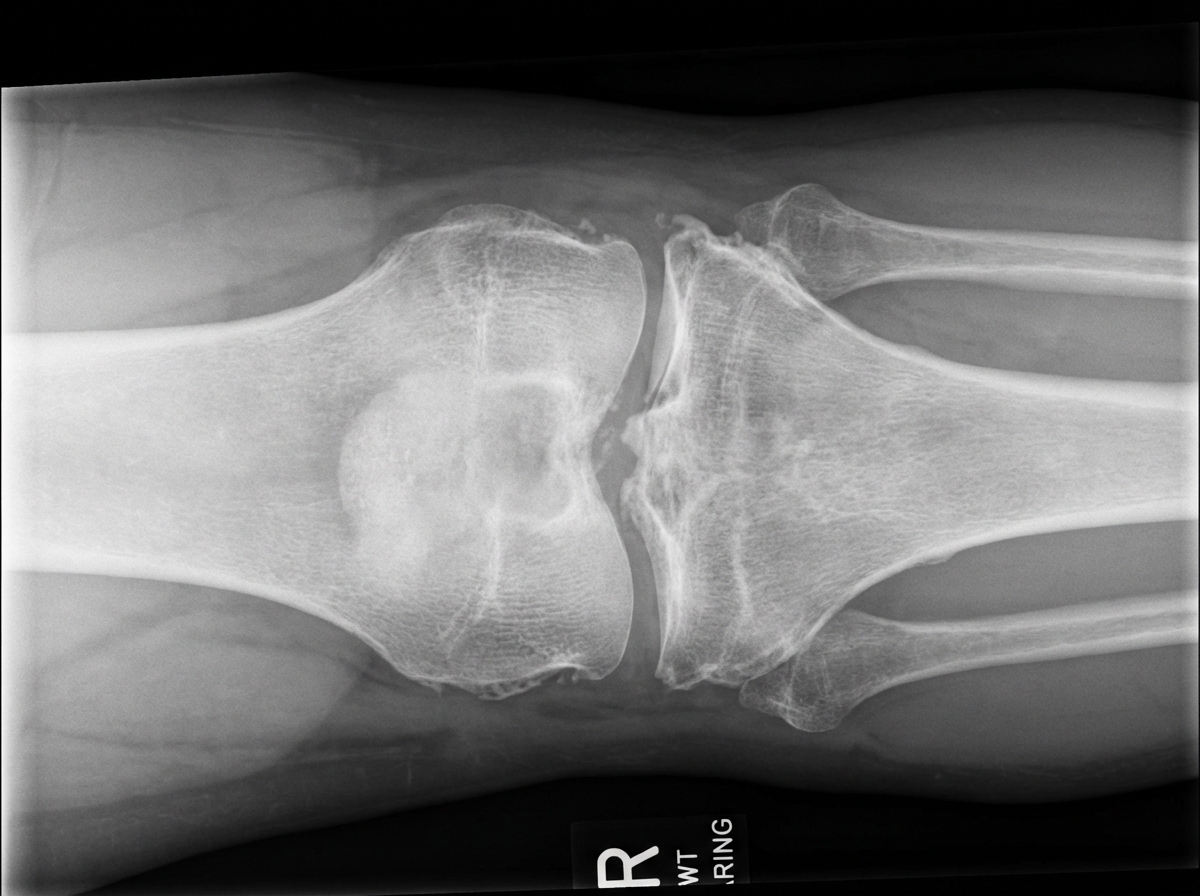
A 52-year-old woman comes to the physician because of a 3-week history of pain in her right knee. The pain is worse at the end of the day and when she walks. She says that it has become difficult for her to walk up the flight of stairs to reach her apartment. She has hypertension and psoriasis. Her sister has rheumatoid arthritis. She drinks 2–3 beers daily. Current medications include hydrochlorothiazide, topical betamethasone, and a multivitamin. She is 160 cm (5 ft 3 in) tall and weighs 92 kg (202 lb); BMI is 36 kg/m2. She appears anxious. Her temperature is 37°C (98.6°F), pulse is 87/min, and blood pressure is 135/83 mm Hg. Cardiopulmonary examinations shows no abnormalities. There are several scaly plaques over the patient's upper and lower extremities. The right knee is not tender nor erythematous; range of motion is limited. Crepitus is heard on flexion and extension of the knee. Her hemoglobin concentration is 12.6 g/dL, leukocyte count is 9,000/mm3, and erythrocyte sedimentation rate is 16 mm/h. An x-ray of the right knee is shown. Which of the following is the most appropriate next step in the management of this patient?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
