Cardiology — MCQs

On this page
A 72-year-old man comes to the physician because of a 2-month history of intermittent retrosternal chest pain and tightness on exertion. He has type 2 diabetes mellitus, osteoarthritis of the right hip, and hypertension. Current medications include insulin, ibuprofen, enalapril, and hydrochlorothiazide. Vital signs are within normal limits. His troponin level is within the reference range. An ECG at rest shows a right bundle branch block and infrequent premature ventricular contractions. The patient's symptoms are reproduced during adenosine stress testing. Repeat ECG during stress testing shows new ST depression of > 1 mm in leads V2, V3, and V4. Which of the following is the most important underlying mechanism of this patient's ECG changes?
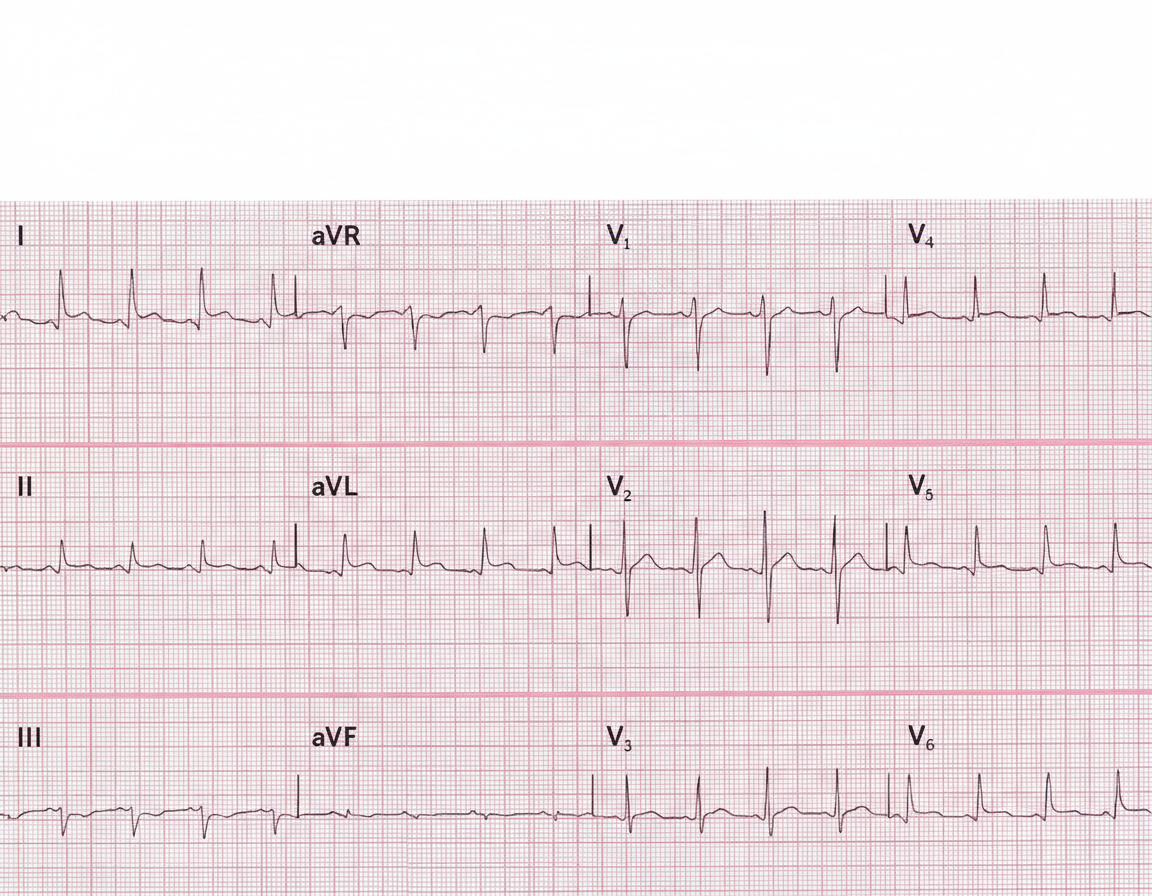
A 29-year-old man presents to the emergency department with a sharp pain in the center of his chest. The pain is knife-like and constant. Sitting alleviates the pain and lying supine aggravates it. He denies the use of nicotine, alcohol or illicit drugs. Vital signs include: temperature 37.0°C (98.6°F), blood pressure 135/92 mm Hg, and pulse 97/min. On examination, a friction rub is heard at the left sternal border while the patient is leaning forward. His ECG is shown in the image. Which of the following can prevent recurrence of this patient’s condition?
A 47-year-old woman with a long history of poorly controlled type 2 diabetes and recurrent urinary tract infections presents with complaints of fever, chills, and severe flank pain. On physical exam, she has left-sided costovertebral tenderness. Vitals include a temperature of 39.4°C (103.0°F), blood pressure of 125/84 mm Hg, and pulse of 84/min. She is currently taking metformin daily. Urine dipstick analysis is positive for leukocytes, nitrites, and blood. Laboratory studies show an elevated creatinine of 2.8 mg/dL (baseline 1.0 mg/dL). Urinalysis reveals fragments of tissue. What is the most likely diagnosis?
A 17-year-old girl comes to the physician because of a sore throat, fevers, and fatigue for the past 3 weeks. Her temperature is 37.8°C (100°F), pulse is 97/min, and blood pressure is 90/60 mm Hg. Examination of the head and neck shows cervical lymphadenopathy, pharyngeal erythema, enlarged tonsils with exudates, and palatal petechiae. The spleen is palpated 2 cm below the left costal margin. Her leukocyte count is 14,100/mm3 with 54% lymphocytes (12% atypical lymphocytes). Results of a heterophile agglutination test are positive. This patient is at increased risk for which of the following conditions?
A 50-year-old man presents to the emergency department with pain and swelling of his right leg for the past 2 days. Three days ago he collapsed on his leg after tripping on a rug. It was a hard fall and left him with bruising of his leg. Since then the pain and swelling of his leg have been gradually increasing. Past medical history is noncontributory. He lives a rather sedentary life and smokes two packs of cigarettes per day. The vital signs include heart rate 98/min, respiratory rate 15/min, temperature 37.8°C (100.1°F), and blood pressure 100/60 mm Hg. On physical examination, his right leg is visibly swollen up to the mid-calf with pitting edema and moderate erythema. Peripheral pulses in the right leg are weak and the leg is tender. Manipulation of the right leg is negative for Homan’s sign. What is the next best step in the management of this patient?
A 78-year-old man is brought to the emergency department because of difficulty speaking. The symptoms began abruptly one hour ago while he was having breakfast with his wife. He has hypertension, type 2 diabetes mellitus, and coronary artery disease. Current medications include pravastatin, lisinopril, metformin, and aspirin. His temperature is 37°C (98.6°F), pulse is 76/min, and blood pressure is 165/90 mm Hg. He is right-handed. The patient speaks in short, simple sentences, and has difficulty repeating sequences of words. He can follow simple instructions. Right facial droop is present. Muscle strength is 4/5 on the right side and 5/5 on the left, and there is a mild right-sided pronator drift. Which of the following is the most likely cause of the patient's symptoms?
A 44-year-old male presents to his primary care physician with complaints of fatigue, muscle weakness, cramps, and increased urination over the past several weeks. His past medical history is significant only for hypertension, for which he was started on hydrochlorothiazide (HCTZ) 4 weeks ago. Vital signs at today's visit are as follows: T 37.2, HR 88, BP 129/80, RR 14, and SpO2 99%. Physical examination does not reveal any abnormal findings. Serologic studies are significant for a serum potassium level of 2.1 mEq/L (normal range 3.5-5.0 mEq/L). Lab-work from his last visit showed a basic metabolic panel and complete blood count results to all be within normal limits. Which of the following underlying diseases most likely contributed to the development of this patient's presenting condition?
A 48-year-old male accountant presents to the family practice clinic for his first health check-up in years. He has no complaints, and as far as he is concerned, he is well. He does not have any known medical conditions. His blood pressure is 140/89 mm Hg and his heart rate is 89/min. Physical examination is otherwise unremarkable. What is the single best initial management for this patient?
A 73-year-old male presents to the ED with several days of fevers, cough productive of mucopurulent sputum, and pleuritic chest pain. He has not been to a doctor in 30 years because he “has never been sick”. His vital signs are: T 101F, HR 98, BP 100/55, RR 31. On physical exam he is confused and has decreased breath sounds and crackles on the lower left lobe. Gram positive diplococci are seen in the sputum. Which of the following is the most appropriate management for his pneumonia?
A 65-year-old man presents to the emergency department for shortness of breath. He was at home working on his car when he suddenly felt very short of breath, which failed to improve with rest. He states he was working with various chemicals and inhalants while trying to replace a broken piece in the engine. The patient was brought in by paramedics and is currently on 100% O2 via nasal cannula. The patient has a 52 pack-year smoking history and drinks 2 to 3 alcoholic drinks every night. He has a past medical history of asthma but admits to not having seen a physician since high school. His temperature is 98.2°F (36.8°C), blood pressure is 157/108 mmHg, pulse is 120/min, respirations are 29/min, and oxygen saturation is 77%. Physical exam demonstrates tachycardia with a systolic murmur heard best along the right upper sternal border. Breath sounds are diminished over the right upper lobe. Bilateral lower extremity pitting edema is noted. Which of the following best describes the most likely diagnosis?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
