Cardiology — MCQs

On this page
A 68-year-old man presents to the emergency department complaining of difficulty in breathing for the past 2 days. He has had recurrent episodes of bacterial pneumonia in the right lower lobe during the last 6 months. His last episode of pneumonia started 7 days ago for which he is being treated with antibiotics. He has a 35-pack-year smoking history. Past medical history is significant for hypertension for which he takes lisinopril. Physical examination reveals decreased breath sounds and dullness to percussion in the right lung base. Chest X-ray reveals a large right-sided pleural effusion, and chest CT scan shows a large mass near the hilum of the right lung. Cytologic examination of pleural fluid shows evidence of malignancy. Which of the following is the most likely diagnosis of this patient?
An 82-year-old man presents to the emergency department complaining of vision loss in his left eye. He states that it suddenly appeared as if a curtain was coming down over his left eye. It resolved after five minutes, and his vision has returned to normal. He has a history of coronary artery disease and type 2 diabetes. What is the most likely cause of this patient's presentation?
A 30-year-old woman presents to the clinic for a 3-month history of painful hair loss. She was in her usual state of health until about 3 months ago when she started to develop some painfully itchy spots across her scalp. Since that time these spots have lost hair and scarred, with new spots continuing to form. On further questioning, she shares that, for the last couple of years, she has generally felt poorly, specifically noting intermittent fevers, muscle and joint pains, and fatigue. On physical exam, she has several erythematous and scaly plaques across her scalp. These areas have no hair growth, but some do demonstrate hyperpigmentation. Which of the following is the most likely diagnosis?
A 25-year-old woman is being evaluated due to complaint of fatigue and voiding pink urine. The laboratory results are as follows: Hb 6.7 Red blood cell count 3.0 x 1012/L Leukocyte count 5,000/mm3 Platelets 170 x 109/L Reticulocyte count 6% Hematocrit 32% The physician thinks that the patient is suffering from an acquired mutation in hematopoietic stem cells, which is confirmed by flow cytometry analysis that revealed these cells are CD 55 and CD 59 negative. However, the physician is interested in knowing the corrected reticulocyte count before starting the patient on eculizumab. What value does the physician find after calculating the corrected reticulocyte count?
A 70-year-old man with a recent above-the-knee amputation of the left lower extremity, due to wet gangrene secondary to refractory peripheral artery disease, presents with weakness and dizziness. He says that the symptoms began acutely 24 hours after surgery and have not improved. The amputation was complicated by substantial blood loss. He was placed on empiric antibiotic therapy with ciprofloxacin and clindamycin before the procedure, and blood and wound culture results are still pending. The medical history is significant for type 2 diabetes mellitus and hypertension. Current medications are metformin and lisinopril. The family history is significant for type 2 diabetes mellitus in both parents. Review of symptoms is significant for palpitations and a mild headache for the past 24 hours. His temperature is 38.2°C (100.8°F); blood pressure, 120/70 mm Hg (supine); pulse, 102/min; respiratory rate, 16/min; and oxygen saturation, 99% on room air. When standing, the blood pressure is 90/65 mm Hg and the pulse is 115/min. On physical examination, the patient appears pale and listless. The surgical amputation site does not show any signs of ongoing blood loss or infection. Laboratory tests and an ECG are pending. Which of the following is the next best step in management?
A 34-year-old man comes to the physician for a follow-up examination. He has a 3-month history of a nonproductive cough. He has been treated with diphenhydramine since his last visit 2 weeks ago, but his symptoms have persisted. He does not smoke. He drinks 3 beers on the weekends. He is 177 cm (5 ft 10 in) tall and weighs 100 kg (220.46 lbs); BMI is 35.1 kg/m2. His temperature is 37.1°C (98.8°F), pulse is 78/min, respirations are 14/min, and blood pressure is 130/80 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 97%. Physical examination and an x-ray of the chest show no abnormalities. Which of the following is the most appropriate next step in management?
A 32-year-old man is brought to the emergency department because of a 2-day history of confusion and rapidly progressive dyspnea. He has had a fever and chills for the past five days. Five years ago, he was diagnosed with hepatitis C. He has smoked two packs of cigarettes daily for 15 years and drinks one to two beers daily. He has a history of past intravenous heroin use. He appears pale, anxious, and in severe distress. His temperature is 39.3°C (102.7°F), respirations are 30/min, pulse is 59/min, and blood pressure is 80/50 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 75%. Examination shows multiple linear hemorrhages underneath the nails. There are nontender maculae on both palms and soles. Fine rales are heard bilaterally on auscultation of the chest. Cardiac examination shows an S3; a grade 3/6 high-pitched decrescendo early diastolic murmur is heard along the left sternal border and right second intercostal space. An x-ray of the chest shows a normal sized heart and pulmonary edema. An ECG shows P waves and QRS complexes that occur at regular intervals, but independently of each other. A transesophageal echocardiography (TEE) is most likely to show which of the following?
A 55-year-old man presents to the physician with tiredness, lethargy, bone pain, and colicky right abdominal pain for 1 month. He has no comorbidities. He does not have any significant past medical history. His height is 176 cm (5 ft 7 in), weight is 88 kg (194 lb), and his BMI is 28.47 kg/m2. The physical examination is normal, except for mild right lumbar region tenderness. Laboratory studies show: Hemoglobin 13.5 g/dL Serum TSH 2.2 mU/L Serum calcium 12.3 mg/dL Serum phosphorus 1.1 mg/dL Serum sodium 136 mEq/L Serum potassium 3.5 mEq/L Serum creatinine 1.1 mg/dL Urine calcium Elevated An ultrasound of the abdomen reveals a single stone in the right ureter without hydroureteronephrosis. Clinically, no evidence of malignancy was observed. An X-ray of the long bones reveals diffuse osteopenia with subperiosteal bone resorption. The serum parathyroid hormone level is tested and it is grossly elevated. What is the most appropriate next step in his management?
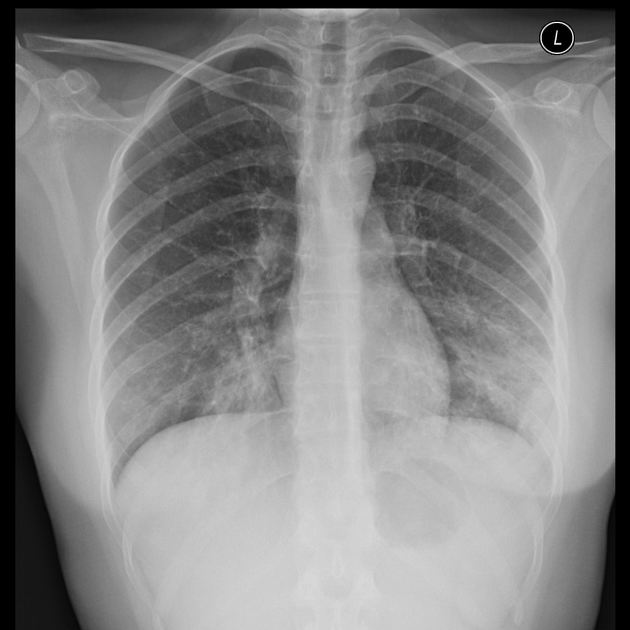
A 24-year-old woman, otherwise healthy, presents with a non-productive cough, sore throat, and myalgia. The patient reports that her symptoms started gradually 2 weeks ago and have not improved. She has no significant past medical history and no current medications. She is a college student and denies any recent overseas travel. The patient received the flu vaccine this year, and her 2-part PPD required for school was negative. She does not smoke, drink, or use recreational drugs. The patient denies being sexually active. The vital signs include: temperature 37.0°C (98.6°F), blood pressure 110/75 mm Hg, pulse 98/min, respirations 20/min, and oxygen saturation 99% on room air. On physical exam, the patient is alert and cooperative. The cardiac exam is normal. There are rales present bilaterally over both lung fields. The skin and conjunctiva are pale. The laboratory tests are pending. The chest X-ray is shown in the image. Which of the following laboratory findings would also commonly be found in this patient?
A 32-year-old man comes to the emergency room because of severe breathlessness for the past few hours. Over the course of a few years, he has been treated for asthma by several physicians, but his symptoms have continued to progress. He has never smoked. Both his father who died at the age of 40 years and his uncle (father's brother), died with chronic obstructive pulmonary disorder. His respiratory rate is 19/min and temperature is 37.0°C (98.6°F). On physical examination, the patient has significantly longer exhalation than inhalation. His expiratory time is longer than 6 seconds. Clubbing is present. Chest auscultation reveals bilateral crackles. Mild hepatomegaly is present. What is the most likely diagnosis?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
