Cardiology — MCQs

On this page
A 44-year-old woman presents to her primary care physician’s office with episodes of pain in her right hand. She says that the pain is most significant at night and awakens her from sleep numerous times. When she experiences this pain, she immediately puts her hand under warm running water or shakes her hand. She has also experienced episodes of numbness in the affected hand. Driving and extending the right arm also provoke her symptoms. She denies any trauma to the hand or associated weakness. Medical history is notable for hypothyroidism treated with levothyroxine. She works as a secretary for a law firm. On physical exam, when the patient hyperflexes her wrist, pain and paresthesia affect the first 3 digits of the right hand. Which of the following is the confirmatory diagnostic test for this patient?
An 81-year-old man comes to the physician because of increased exertional dyspnea and dizziness over the past 8 weeks. He has hypertension for which he takes lisinopril. He has smoked one pack of cigarettes daily for the past 50 years. Physical examination shows weak peripheral pulses. Cardiac examination is shown. Which of the following is the most likely diagnosis?
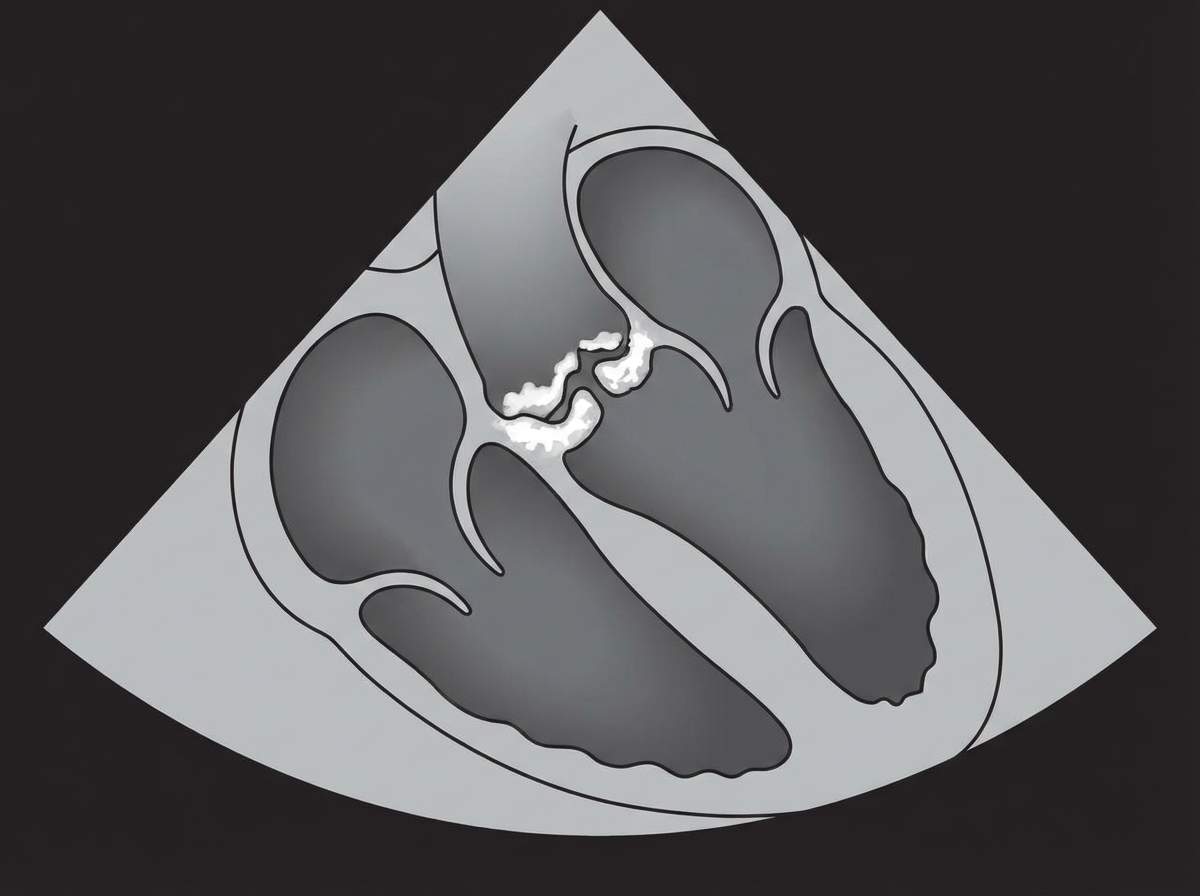
A 31-year-old woman presents to the physician for a routine health maintenance examination. She feels well and has no current complaints. She has no history of serious illness and takes no medications. The vital signs include: blood pressure 185/110 mm Hg, pulse 75/min, and respiration rate 12/min. Her high blood pressure is confirmed during a 2nd visit. Neurologic examination shows no abnormalities. Careful auscultation of the abdomen reveals bruits in both upper quadrants near the midline. The remainder of the physical exam is unremarkable. The results of a complete blood count (CBC), renal function panel, and urinalysis showed no abnormalities. Conventional angiography confirms bilateral disease involvement. To control this patient’s hypertension, it is most appropriate to recommend which of the following?
A 65-year-old woman presents to the clinic for a routine checkup. She has unintentionally lost 4.5 kg (9.9 lb) in the past month but denies any other complaints. Her pulse rate is 90/min, respiratory rate is 18/min, temperature is 37.0°C (98.6°F), and blood pressure is 150/70 mm Hg. An irregularly irregular rhythm is heard on auscultation of the heart. Neck examination shows a markedly enlarged thyroid with no lymphadenopathy or bruit. Laboratory tests show low serum thyroid-stimulating hormone level, high T4 level, absent thyroid-stimulating immunoglobulin, and absent anti-thyroid peroxidase antibody. Nuclear scintigraphy shows patchy uptake with multiple hot and cold areas. Which of the following is the most likely diagnosis?
A 66-year old man comes to the physician because of fatigue for 6 months. He says that he wakes up every morning feeling tired. Most days of the week he feels sleepy during the day and often takes an afternoon nap for an hour. His wife says he snores in the middle of the night. He has a history of heart failure and atrial fibrillation. His medications include aspirin, atorvastatin, lisinopril, metoprolol, and warfarin. He drinks 1–2 glasses of wine daily with dinner; he does not smoke. He is 175 cm (5 ft 9 in) tall and weighs 96 kg (212 lb); BMI is 31.3 kg/m2. His blood pressure is 142/88 mm Hg, pulse is 98/min, and respirations are 22/min. Examination of the oral cavity shows a low-lying palate. Cardiac examination shows an irregularly irregular rhythm and no murmurs. The remainder of the examination shows no abnormalities. Which of the following is the most appropriate next step in management?
A 73-year-old male is brought into the ED unconscious with cold, clammy skin. His blood pressure is 65 over palpable. There are no signs of blood loss. You recognize the patient is in acute shock and blood is drawn for investigation as resuscitation is initiated. Which of the following might you expect in your laboratory investigation for this patient?
A 14-year-old boy is brought to the emergency department from school after falling in gym class. He was unable to stand after the accident and has a painful and swollen knee. On presentation he says that he has never had an incident like this before; however, he does suffer from hard to control nosebleeds and prolonged bleeding after minor cuts. Based on his presentation a panel of bleeding tests is obtained with the following results: Bleeding time: Prolonged Prothrombin time: Normal Partial thromboplastin time: Prolonged Which of the following describes the function of the component that is defective in the most likely cause of this patient's symptoms?
A 66-year-old man is brought to the emergency department because of fever, chills, and altered mental status for 3 days. According to his daughter, he has had a productive cough during this period. He has type 2 diabetes, hypertension, hypercholesterolemia, peripheral neuropathic pain, and a history of deep vein thromboses. Current medications include insulin, lisinopril, atorvastatin, warfarin, and carbamazepine. He is oriented only to self. His temperature is 39.3°C (102.7°F), pulse is 110/min, respirations are 26/min, and blood pressure is 86/50 mm Hg. Physical examination shows ecchymoses on both lower extremities. Crackles are heard at the right lung base. Laboratory studies show: Hemoglobin 11.1 g/dL Leukocyte count 18,000/mm3 Platelet count 45,000/mm3 Prothrombin time 45 sec Partial thromboplastin time 75 sec Serum Na+ 135 mEq/L K+ 5.4 mEq/L Cl- 98 mEq/L Urea nitrogen 46 mg/dL Glucose 222 mg/dL Creatinine 3.3 mg/dL Which of the following is the most likely cause of this patient's ecchymoses?
A 27-year-old man is brought to the emergency department with his family because of abdominal pain, excessive urination and drowsiness since the day before. He has had type 1 diabetes mellitus for 2 years. He ran out of insulin 2 days ago. His vital signs at admission include a temperature of 36.8°C (98.24°F), a blood pressure of 102/69 mmHg, and a pulse of 121/min. On physical examination, he is lethargic and his breathing is rapid and deep. There is a mild generalized abdominal tenderness without rebound tenderness or guarding. His serum glucose is 480 mg/dL. The patient is admitted to the intensive care unit and management is started. Which of the following is considered a resolution criterion for this patient's condition?
A 25-year-old man comes to the physician because of a severe headache for 1 hour. Every day of the past week, he has experienced 3–4 episodes of severe pain over his left forehead. Each episode lasts around 30–45 minutes, and he reports pacing around restlessly during these episodes. He has been using acetaminophen for these episodes, but it has provided only minimal relief. He works as a financial analyst and says his job is very stressful. He had experienced similar symptoms 4 months ago but did not seek treatment at that time. He has no history of serious illness and takes no other medications. He has smoked one pack of cigarettes daily for 7 years. He appears anxious. Vital signs are within normal limits. There is conjunctival injection and tearing of the left eye. The remainder of the physical examination is unremarkable. Which of the following measures is most likely to provide acute relief of this patient's headaches?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
