Cardiology — MCQs

On this page
A 34-year-old man presents with multiple painful ulcers on his penis. He says that the ulcers all appeared suddenly at the same time 3 days ago. He reports that he is sexually active with multiple partners and uses condoms inconsistently. He is afebrile and his vital signs are within normal limits. Physical examination reveals multiple small shallow ulcers with an erythematous base and without discharge. There is significant inguinal lymphadenopathy present. Which of the following is the most likely etiologic agent of this patient’s ulcers?
A 35-year-old woman presents to the clinic for a several-month history of heat intolerance. She lives in a small apartment with her husband and reports that she always feels hot and sweaty, even when their air conditioning is on high. On further questioning, she's also had a 4.5 kg (10 lb) unintentional weight loss. The vital signs include: heart rate 102/min and blood pressure 150/80 mm Hg. The physical exam is notable for warm and slightly moist skin. She also exhibits a fine tremor in her hands when her arms are outstretched. Which of the following laboratory values is most likely low in this patient?
A 64-year-old man presents with a complaint of prominent stiffness in his legs which is causing a difficulty in ambulation. He is not able to relax his trunk area and has frequent, painful muscle spasms. He denies diplopia, swallowing difficulties, and urinary or bowel problems. He has a medical history of stage IV lung cancer. He has received 4 sessions of chemotherapy. The neurological examination reveals an increased generalized muscle tone. He has a spastic gait with exaggerated lumbar lordosis. The needle electromyography (EMG) studies show continuous motor unit activity that persists at rest. Which paraneoplastic antibody is most likely associated with the symptoms of this patient?
A 55-year-old woman sees her family doctor for a follow-up appointment to discuss her imaging studies. She previously presented with chest pain and shortness of breath for the past 2 months. Her CT scan shows a 3.5 cm mass in the lower lobe of her right lung. The mass has irregular borders. Saddle/hilar lymph nodes are enlarged. No distant metastases are identified with PET imaging. The patient has been a smoker for over 35 years (1.5 packs per day), but she has recently quit. This patient is referred to the Pulmonary Diseases Center. What is the most effective step in appropriately managing her case?
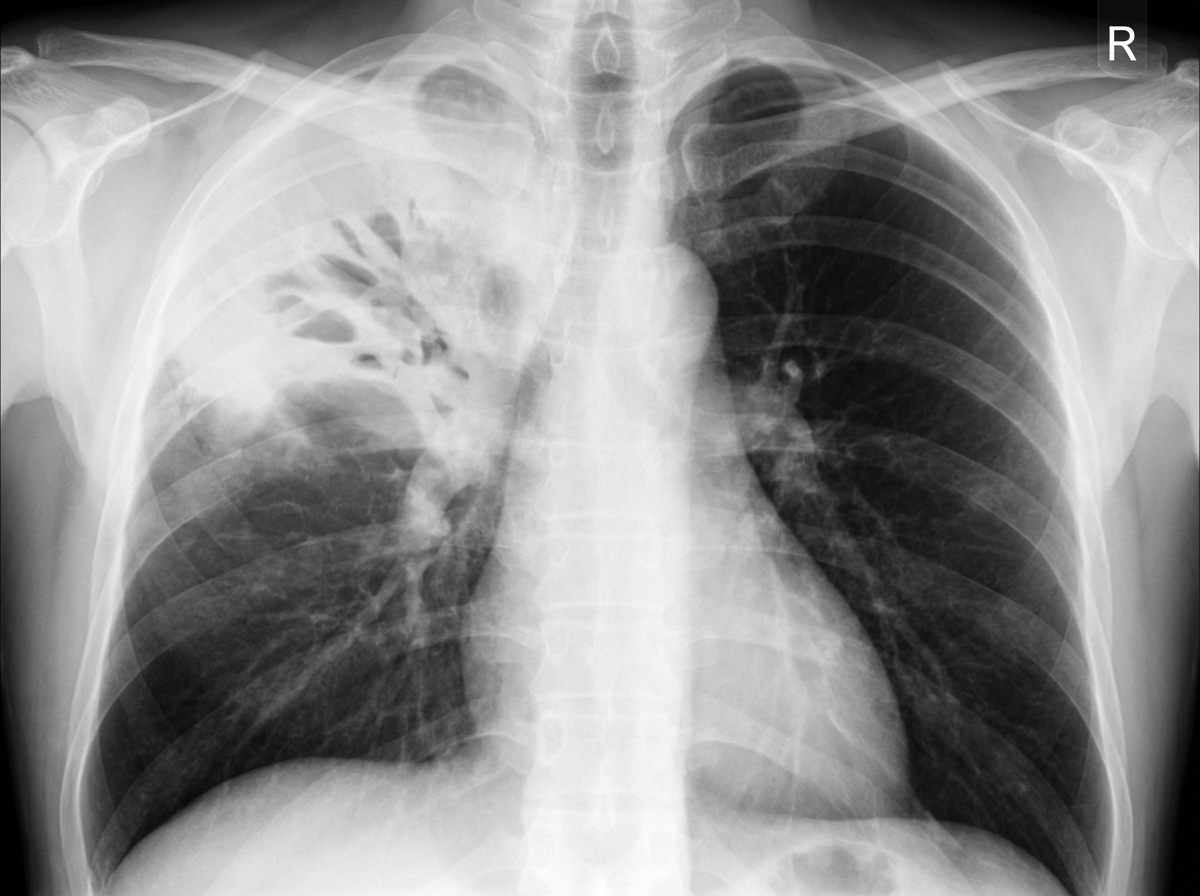
A 67-year-old woman is brought to the emergency department for evaluation of fever, chest pain, and a cough that has produced a moderate amount of greenish-yellow sputum for the past 2 days. During this period, she has had severe malaise, chills, and difficulty breathing. Her past medical history is significant for hypertension, hypercholesterolemia, and type 2 diabetes, for which she takes lisinopril, atorvastatin, and metformin. She has smoked one pack of cigarettes daily for 20 years. Her vital signs show her temperature is 39.0°C (102.2°F), pulse is 110/min, respirations are 33/min, and blood pressure is 143/88 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 94%. Crackles are heard on auscultation of the right upper lobe. Laboratory studies show a leukocyte count of 12,300/mm3, an erythrocyte sedimentation rate of 60 mm/h, and urea nitrogen of 15 mg/dL. A chest X-ray is shown. Which of the following is the most appropriate next step to manage this patient’s symptoms?
A 53-year-old woman presents to her primary care provider complaining of fatigue for the last several months. She reports feeling tired all day, regardless of her quality or quantity of sleep. On further questioning, she has also noted constipation and a 4.5 kg (10 lb) weight gain. She denies shortness of breath, chest pain, lightheadedness, or blood in her stool. At the doctor’s office, the vital signs include: pulse 58/min, blood pressure 104/68 mm Hg, and oxygen saturation 98% on room air. The physical exam shows only slightly dry skin. The complete blood count (CBC) is within normal limits. Which of the following best describes the pathogenesis of this patient's condition?
A 43-year-old man is brought to the emergency department because of severe retrosternal pain radiating to the back and left shoulder for 4 hours. The pain began after attending a farewell party for his coworker at a local bar. He had 3–4 episodes of nonbilious vomiting before the onset of the pain. He has hypertension. His father died of cardiac arrest at the age of 55 years. He has smoked one pack of cigarettes daily for the last 23 years and drinks 2–3 beers daily. His current medications include amlodipine and valsartan. He appears pale. His temperature is 37° C (98.6° F), pulse is 115/min, and blood pressure is 90/60 mm Hg. There are decreased breath sounds over the left base and crepitus is palpable over the thorax. Abdominal examination shows tenderness to palpation in the epigastric region; bowel sounds are normal. Laboratory studies show: Hemoglobin 16.5 g/dL Leukocyte count 11,100/mm3 Serum Na+ 133 mEq/L K+ 3.2 mEq/L Cl- 98 mEq/L HCO3- 30 mEq/L Creatinine 1.4 mg/dL An ECG shows sinus tachycardia with left ventricular hypertrophy. Intravenous fluid resuscitation and antibiotics are begun. Which of the following is the most appropriate test to confirm the diagnosis in this patient?
A 57-year-old man presents to his primary care provider with progressive right foot swelling, redness, and malaise. He reports seeing a blister on his forefoot several months ago after he started using new work boots. He has dressed the affected area daily with bandages; however, healing has not occurred. He has a history of type 2 diabetes mellitus and stage 2 chronic kidney disease. He has smoked 20 to 30 cigarettes daily for the past 25 years. Vital signs are a temperature of 38.1°C (100.58°F), blood pressure of 110/70 mm Hg, and pulse of 102/minute. On physical examination, there is a malodorous right foot ulcer overlying the first metatarsophalangeal joint. Fluctuance and erythema extend 3 cm beyond the ulcer border. Moderate pitting edema is notable over the remaining areas of the foot and ankle. Which of the following is the best initial step for this patient?
A 40-year-old man comes to the physician because of weight gain over the past 3 months. During this period, he has gained 10 kg (22 lb) unintentionally. He also reports decreased sexual desire, oily skin, and sleeping difficulties. There is no personal or family history of serious illness. He has smoked one pack of cigarettes daily for the past 10 years. The patient appears lethargic. His temperature is 37°C (98.6°F), pulse is 80/min, and blood pressure is 150/90 mm Hg. Physical examination shows central obesity, acne, and thin, easily bruisable skin with stretch marks on the abdomen. There is darkening of the mucous membranes and the skin creases. Examination of the muscles shows atrophy and weakness of proximal muscle groups. His serum glucose concentration is 240 mg/dL. Which of the following findings would most likely be present on imaging?
A 26-year-old woman comes to the physician for a pre-employment examination. She has no complaints. She has a history of polycystic ovarian syndrome. She exercises daily and plays soccer recreationally on the weekends. Her mother was diagnosed with hypertension at a young age. She does not smoke and drinks 2 glasses of wine on the weekends. Her current medications include an oral contraceptive pill and a daily multivitamin. Her vital signs are within normal limits. Cardiac examination shows a grade 1/6 decrescendo diastolic murmur heard best at the left sternal border. Her lungs are clear to auscultation bilaterally. Peripheral pulses are normal and there is no lower extremity edema. An electrocardiogram shows sinus rhythm with a normal axis. Which of the following is the most appropriate next step in management?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
