Cardiology — MCQs

On this page
A 19-year-old man with a history of type 1 diabetes presents to the emergency department for the evaluation of a blood glucose level of 492 mg/dL. Laboratory examination revealed a serum bicarbonate level of 13 mEq/L, serum sodium level of 122 mEq/L, and ketonuria. Arterial blood gas demonstrated a pH of 6.9. He is admitted to the hospital and given bicarbonate and then started on an insulin drip and intravenous fluid. Seven hours later when his nurse is making rounds, he is confused and complaining of a severe headache. Repeat sodium levels are unchanged, although his glucose level has improved. His vital signs include a temperature of 36.6°C (98.0°F), pulse 50/min, respiratory rate 13/min and irregular, and blood pressure 177/95 mm Hg. What other examination findings would be expected in this patient?
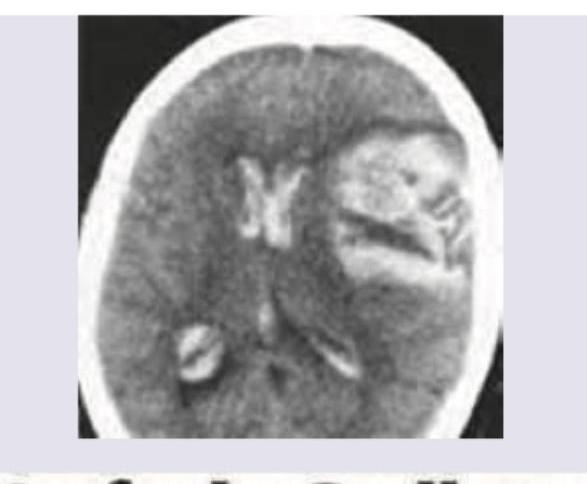
One day after undergoing a left carotid endarterectomy, a 63-year-old man has a severe headache. He describes it as 9 out of 10 in intensity. He has nausea. He had 80% stenosis in the left carotid artery and received heparin prior to the surgery. He has a history of 2 transient ischemic attacks, 2 and 4 months ago. He has hypertension, type 2 diabetes mellitus, and hypercholesterolemia. He has smoked one pack of cigarettes daily for 40 years. He drinks 1–2 beers on weekends. Current medications include lisinopril, metformin, sitagliptin, and aspirin. His temperature is 37.3°C (99.1°F), pulse is 111/min, and blood pressure is 180/110 mm Hg. He is confused and oriented only to person. Examination shows pupils that react sluggishly to light. There is a right facial droop. Muscle strength is decreased in the right upper and lower extremities. Deep tendon reflexes are 3+ on the right. There is a left cervical surgical incision that shows no erythema or discharge. Cardiac examination shows no abnormalities. A complete blood count and serum concentrations of creatinine, electrolytes, and glucose are within the reference range. A CT scan of the head is shown. Which of the following is the strongest predisposing factor for this patient's condition?
A 25-year-old mother presents to her primary care physician for wrist pain. The patient recently gave birth to a healthy newborn at 40 weeks gestation. Beginning one week ago, she started having pain over her wrist that has steadily worsened. The patient notes that she also recently fell while walking and broke the fall with her outstretched arm. The patient is an accountant who works from home and spends roughly eight hours a day typing or preparing financial statements. Recreationally, the patient is a competitive cyclist who began a rigorous training routine since the birth of her child. The patient's past medical history is notable for hypothyroidism that is treated with levothyroxine. On physical exam, inspection of the wrist reveals no visible or palpable abnormalities. Pain is reproduced when the thumb is held in flexion, and the wrist is deviated toward the ulna. The rest of the patient's physical exam is within normal limits. Which of the following is the best next step in management?
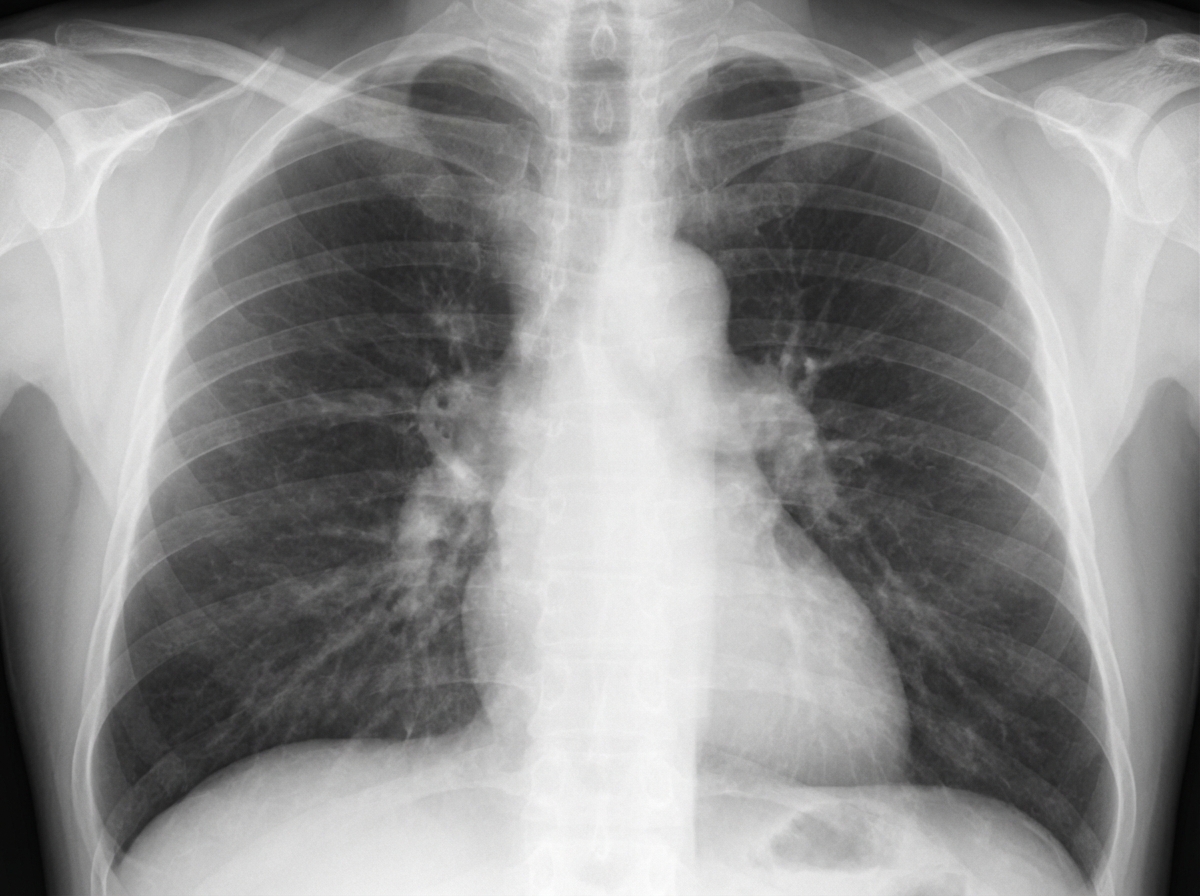
A 61-year-old man presents to the urgent care clinic complaining of cough and unintentional weight loss over the past 3 months. He works as a computer engineer, and he informs you that he has been having to meet several deadlines recently and has been under significant stress. His medical history is significant for gout, hypertension, hypercholesterolemia, diabetes mellitus type 2, and pulmonary histoplasmosis 10 years ago. He currently smokes 2 packs of cigarettes/day, drinks a 6-pack of beer/day, and he endorses a past history of cocaine use back in the early 2000s but currently denies any drug use. The vital signs include: temperature 36.7°C (98.0°F), blood pressure 126/74 mm Hg, heart rate 87/min, and respiratory rate 18/min. His physical examination shows minimal bibasilar rales, but otherwise clear lungs on auscultation, grade 2/6 holosystolic murmur, and a benign abdominal physical examination. However, on routine lab testing, you notice that his sodium is 127 mEq/L. His chest X-ray is shown in the picture. Which of the following is the most likely underlying diagnosis?
A 78-year-old man presents to the hospital because of shortness of breath and chest pain that started a few hours ago. 3 weeks ago he had surgery for a total hip replacement with a prosthesis. The patient was treated with prophylactic doses of low-molecular-weight heparin until he was discharged. He did not have a fever, expectoration, or any accompanying symptoms. He has a history of right leg deep vein thrombosis that occurred 5 years ago. His vital signs include: heart rate 110/min, respiratory rate 22/min, and blood pressure 150/90 mm Hg. There were no significant findings on the physical exam. Chest radiography was within normal limits. What is the most likely diagnosis?
A 74-year-old man is rushed to the emergency department with left-sided weakness, facial deviation, and slurred speech. His wife first noticed these changes about an hour ago. The patient is having difficulty communicating. He can answer questions by nodding his head, and his wife is providing detailed information. He denies fever, loss of consciousness, head injury, bleeding, or seizures. Past medical history is significant for diabetes mellitus, hypertension, hyperlipidemia, ischemic heart disease, chronic kidney disease, and osteoarthritis. He had a heart attack 6 weeks ago. Baseline creatinine is 2.5 mg/dL, and he is not on hemodialysis. Medications include aspirin, clopidogrel, metoprolol, ramipril, rosuvastatin, and insulin detemir. Blood pressure is 175/95 mm Hg and the heart rate is 121/min. Muscle strength is decreased in both the upper and lower extremities on the left-side. A forehead sparing left sided facial weakness is also appreciated. An ECG reveals atrial fibrillation. An urgent head CT shows a hypodense area in the right parietal cortex with no indication of hemorrhage. Treatment with tissue plasminogen activator (tPA) is deferred due to which condition?
A 45-year-old woman presents to her primary care provider complaining of daytime drowsiness and fatigue. She reports that she can manage at most a couple of hours of work before needing a nap. She has also noted impaired memory and a 6.8 kg (15 lb) weight gain. She denies shortness of breath, chest pain, lightheadedness, or blood in her stool. At the doctor’s office, the vital signs include: pulse 58/min, blood pressure 104/68 mm Hg, and oxygen saturation 99% on room air. The physical exam is notable only for slightly dry skin. The complete blood count (CBC) is within normal limits. Which of the following is a likely additional finding in this patient?
A 48-year-old woman is transferred from her primary care physician's office to the emergency department for further evaluation of hypokalemia to 2.5 mEq/L. She was recently diagnosed with hypertension 2 weeks ago and started on medical therapy. The patient said that she enjoys all kinds of food and exercises regularly, but has not been able to complete her workouts as she usually does. Her temperature is 97.7°F (36.5°C), blood pressure is 107/74 mmHg, pulse is 80/min, respirations are 15/min, and SpO2 is 94% on room air. Her physical exam is unremarkable. Peripheral intravenous (IV) access is obtained. Her basic metabolic panel is obtained below. Serum: Na+: 135 mEq/L Cl-: 89 mEq/L K+: 2.2 mEq/L HCO3-: 33 mEq/L BUN: 44 mg/dL Glucose: 147 mg/dL Creatinine: 2.3 mg/dL Magnesium: 2.0 mEq/L What is the next best step in management?
A 22-year-old woman presents to the emergency department with a chief concern of shortness of breath. She was hiking when she suddenly felt unable to breathe and had to take slow deep breaths to improve her symptoms. The patient is a Swedish foreign exchange student and does not speak any English. Her past medical history and current medications are unknown. Her temperature is 99.5°F (37.5°C), blood pressure is 127/68 mmHg, pulse is 120/min, respirations are 22/min, and oxygen saturation is 90% on room air. Physical exam is notable for poor air movement bilaterally and tachycardia. The patient is started on treatment. Which of the following best describes this patient's underlying pathology? FEV1 = Forced expiratory volume in 1 second FVC = Forced vital capacity DLCO = Diffusing capacity of carbon monoxide
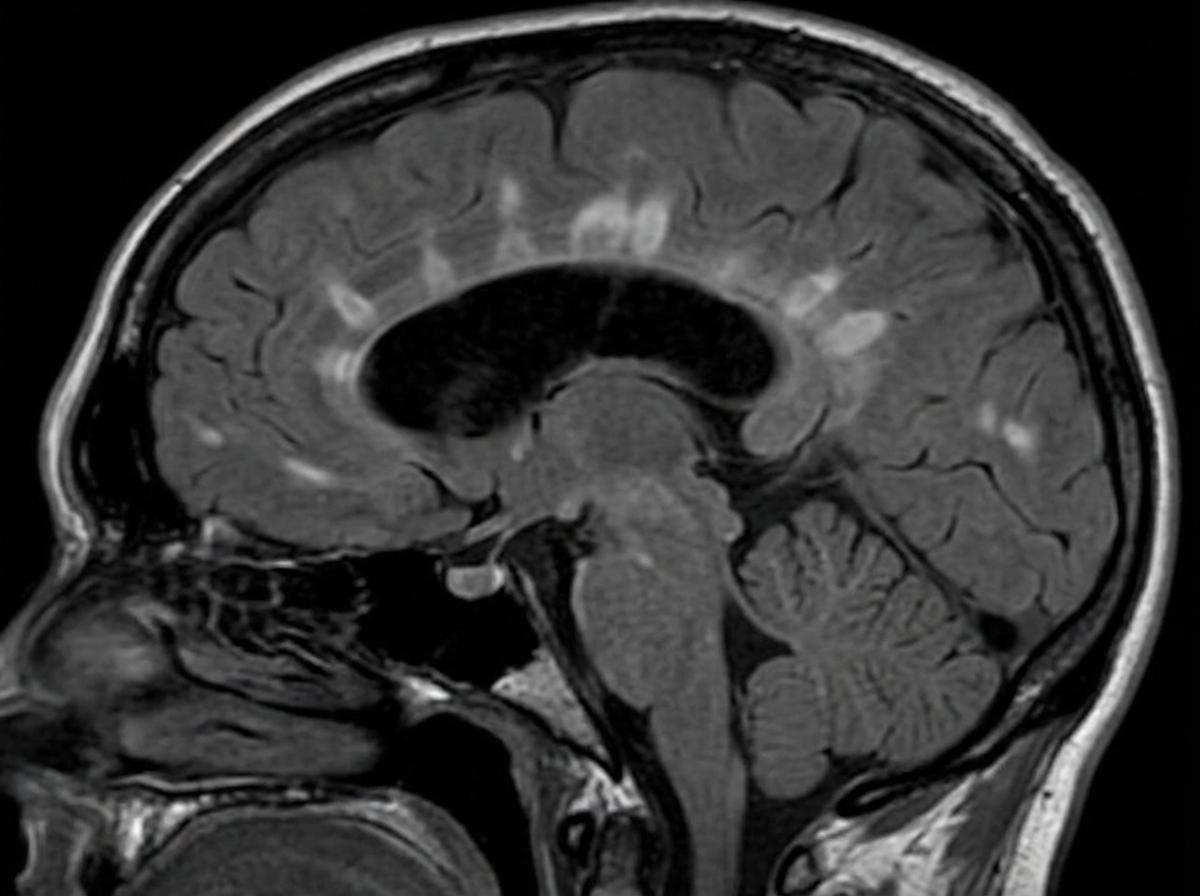
A 29-year-old woman presents with progressive vision loss in her right eye and periorbital pain for 5 days. She says that she has also noticed weakness, numbness, and tingling in her left leg. Her vital signs are within normal limits. Neurological examination shows gait imbalance, positive Babinski reflexes, bilateral spasticity, and exaggerated deep tendon reflexes in the lower extremities bilaterally. FLAIR MRI is obtained and is shown in the image. Which of the following is the most likely cause of this patient’s condition?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
