Cardiology — MCQs

On this page
A 37-year-old woman presents to her primary care physician for bilateral nipple discharge. The patient states that she has observed a milky discharge coming from her nipples for the past month. On review of systems, the patient states that she has felt fatigued lately and has experienced decreased libido. She also endorses headaches that typically resolve by the middle of the day and a 5 pound weight gain this past month. The patient has a past medical history of obesity, schizophrenia, and constipation. Her temperature is 99.5°F (37.5°C), blood pressure is 145/95 mmHg, pulse is 60/min, respirations are 15/min, and oxygen saturation is 98% on room air. On physical exam, you note an obese, fatigued-appearing woman. Dermatologic exam reveals fine, thin hair over her body. Cardiopulmonary exam is within normal limits. Neurological exam reveals cranial nerves II-XII as grossly intact. The patient exhibits 1+ sluggish reflexes. Which of the following is the most likely diagnosis?
A 41-year-old woman presents to the emergency room with chest pain. She has had progressive substernal chest pain accompanied by weakness and mild shortness of breath for the past 2 hours. Her past medical history is notable for poorly controlled systemic lupus erythematosus (SLE), Sjogren syndrome, and interstitial lung disease. She was hospitalized last year with pericarditis presumed to be from SLE. Her temperature is 98.6°F (37°C), blood pressure is 106/56 mmHg, pulse is 132/min, and respirations are 26/min. On exam, the skin overlying the internal jugular vein fills at 9 cm above the sternal angle and distant heart sounds are appreciated. There is no friction rub. She is given 1000cc of intravenous fluids with no appreciable change in her blood pressure. An electrocardiogram in this patient would most likely reveal which of the following findings?
A 57-year-old immigrant from Nigeria presents to the emergency department for sudden, severe pain and swelling in her lower extremity. She was at a rehabilitation hospital when her symptoms became apparent. The patient has a past medical history of obesity, diabetes, bipolar disorder, and tonic-clonic seizures. Her current medications include metformin, insulin, lisinopril, and valproic acid. The patient is a prominent IV drug and alcohol user who has presented to the ED many times for intoxication. On physical exam you note anasarca and asymmetric lower extremity swelling. Based on the results of a doppler ultrasound of her swollen lower extremity, heparin is started. The patient is then transferred to the general medicine floor for continued management. Laboratory studies are shown below. Serum: Na+: 137 mEq/L K+: 5.5 mEq/L Cl-: 100 mEq/L HCO3-: 24 mEq/L Urea nitrogen: 22 mg/dL Ca2+: 5.7 mg/dL Creatinine: 1.7 mg/dL Glucose: 70 mg/dL The patient's presentation includes generalized edema (anasarca) along with laboratory abnormalities. What is the most likely underlying diagnosis that explains her overall clinical presentation?
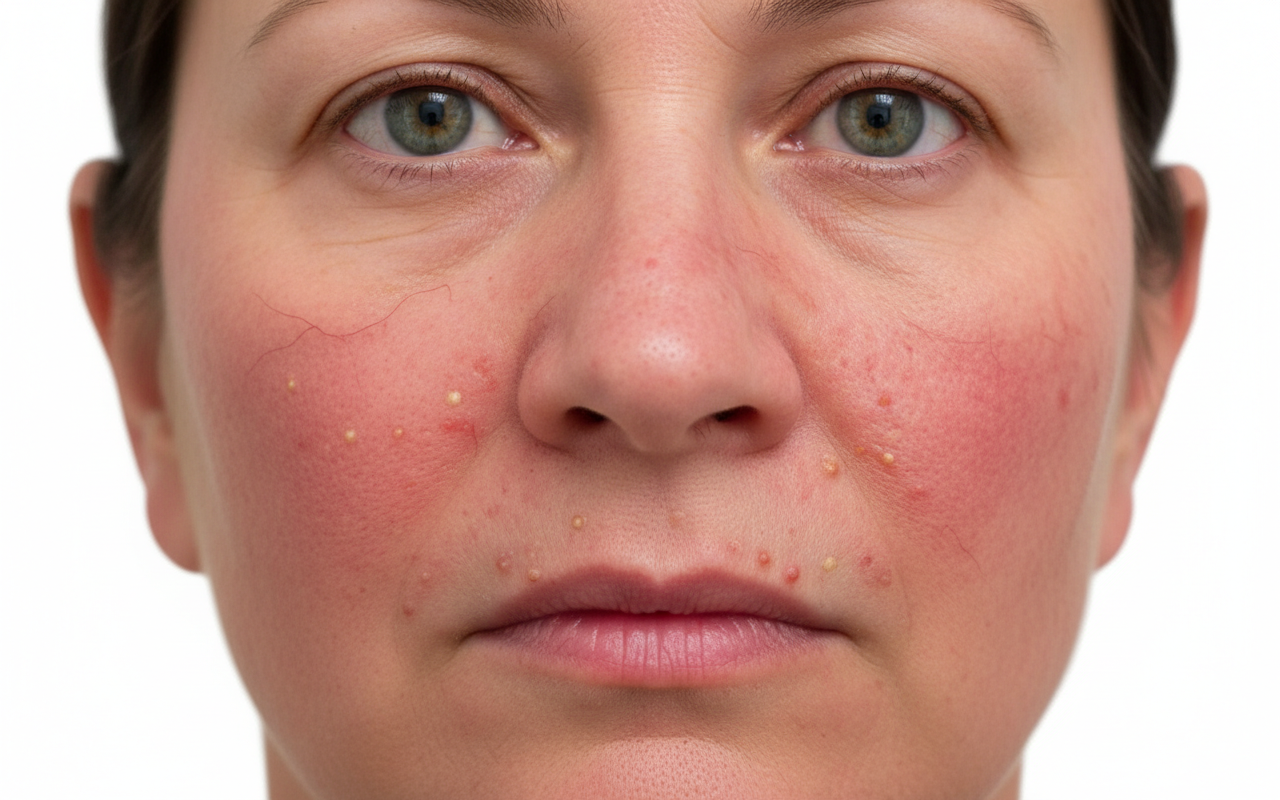
A 67-year-old man with hypertension comes to the physician because of a 5-month history of a facial rash. He occasionally feels burning or stinging over the affected area. His only medication is lisinopril. Physical examination shows the findings in the photograph. Which of the following is the most common trigger for exacerbation of this patient's skin condition?
A 62-year-old man comes to the physician because of increasing pain in his right leg for 2 months. The pain persists throughout the day and is not relieved by rest. He tried taking acetaminophen, but it provided no relief from his symptoms. There is no family history of serious illness. He does not smoke. He occasionally drinks a beer. Vital signs are within normal limits. On examination, the right tibia is bowing anteriorly; range of motion is limited by pain. An x-ray of the right leg shows a deformed tibia with multiple lesions of increased and decreased density and a thickened cortical bone. Laboratory studies show markedly elevated serum alkaline phosphatase and normal calcium and phosphate levels. This patient is most likely to develop which of the following complications?
A 67-year-old man with type 2 diabetes mellitus comes to the emergency department because of lightheadedness over the past 2 hours. He reports that he has had similar episodes of lightheadedness and palpitations over the past 3 days. His only medication is metformin. His pulse is 110/min and irregularly irregular. An ECG shows a variable R-R interval and absence of P waves. The patient undergoes transesophageal echocardiography. During the procedure, the tip of the ultrasound probe is angled posteriorly within the esophagus. This view is most helpful for evaluating which of the following conditions?
A 44-year-old woman comes to the physician for the evaluation of a 1-month history of fatigue and difficulty swallowing. During this period, she has also had dry skin, thinning hair, and rounding of her face. She has type 1 diabetes mellitus and rheumatoid arthritis. Her father had a thyroidectomy for papillary thyroid cancer. The patient had smoked one pack of cigarettes daily for 20 years but quit 3 years ago. She drinks 2–3 glasses of wine daily. Her current medications include insulin, omeprazole, and daily ibuprofen. She appears well. Her temperature is 36.3°C (97.3°F), pulse is 62/min, and blood pressure is 102/76 mm Hg. Examination of the neck shows a painless, diffusely enlarged thyroid gland. Cardiopulmonary examination shows no abnormalities. Further evaluation is most likely to show which of the following?
A 47-year-old woman complains of weight gain and irregular menses for the past 2 years. She has gained 13 kg (28.6 lb) and feels that most of the weight gain is in her abdomen and face. She has type 2 diabetes and hypertension for 1 year, and they are difficult to control with medications. Vital signs include a temperature of 36.9°C (98.4°F), blood pressure of 160/100 mm Hg, and pulse of 95/min. The patient's late-night salivary cortisol is elevated. Morning plasma ACTH is high. Brain magnetic resonance imaging shows a 2 cm pituitary adenoma. Which of the following is the optimal therapy for this patient?
A 62-year-old man with a past medical history notable for hemochromatosis now presents for urgent care with complaints of increased thirst and urinary frequency. Physical examination is grossly unremarkable, although there is a bronze discoloration of his skin. His vital signs include: temperature 36.7°C (98.0°F), blood pressure 126/74 mm Hg, heart rate 74/min, and respiratory rate 14/min. Laboratory analysis reveals fasting blood glucose of 192 mg/dL and subsequently, HbA1c of 8.7. Given the following options, what is the definitive treatment for the patient's underlying disease?
A 50-year-old man presents with a complaint of pain and swelling of his right leg for the past 2 days. He remembers hitting his leg against a table 3 days earlier. Since then, the pain and swelling of the leg have gradually increased. His past medical history is significant for atopy and pulmonary tuberculosis. The patient reports a 20-pack-year smoking history and currently smokes 2 packs of cigarettes per day. His pulse is 98/min, respiratory rate is 15/min, temperature is 38.4°C (101.2°F), and blood pressure is 100/60 mm Hg. On physical examination, his right leg is visibly swollen up to the groin with moderate erythema and 2+ pitting edema. The peripheral pulses are 2+ in the right leg and there is no discomfort. There is no increased resistance or pain in the right calf in response to forced dorsiflexion of the right foot. Which of the following is the best next step in the management of this patient?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
