Cardiology — MCQs

On this page
A 34-year-old woman presents to her primary care provider after intermittently passing bright pink urine over several days. She is concerned this discoloration is due to blood. Her medical history is unremarkable, she denies being sick in the past weeks and has only taken a couple of diclofenac capsules for pelvic pain associated to her menstrual period. She does not drink alcohol or smoke cigarettes. At the doctor’s office, her blood pressure is 150/90 mm Hg, pulse is 80/min, respiratory rate is 18/min, and temperature is 36.5°C (97.7°F). On physical exam, she has 2+ pitting edema up to her knees. A urinalysis is taken which shows red blood cells, red blood cell casts, and acanthocytes. No proteinuria was detected. Her serum creatinine is 2.4 mg/dL, blood urea nitrogen 42 mg/dL, serum potassium 4.8 mEq/L, serum sodium 140 mEq/L, serum chloride 102 mEq/L. Which of the following is the most appropriate next step in the management of this case?
A 28-year-old man comes to the physician for a follow-up examination after a previous visit showed an elevated serum calcium level. He has a history of bipolar disorder. His mother had a parathyroidectomy in her 30s. The patient does not drink alcohol or smoke. Current medications include lithium and a daily multivitamin. His vital signs are within normal limits. Physical examination shows no abnormalities. Laboratory studies show: Serum Sodium 146 mEq/L Potassium 3.7 mEq/L Calcium 11.2 mg/dL Magnesium 2.3 mEq/L PTH 610 pg/mL Albumin 4.2 g/dL 24-hour urine Calcium 23 mg Which of the following is the most likely cause of this patient’s findings?
A 53-year-old woman presents to her primary care physician with complaints of pain and swelling in her hands and fingers. She states that she has had these symptoms since she was in her 20s, but they have recently become more severe. She states that her wedding ring no longer fits, due to increased swelling of her fingers. She is a 30-pack-year smoker with a body mass index (BMI) of 31 kg/m2. The vital signs include: blood pressure 122/78 mm Hg, heart rate 72/min, and respiratory rate 15/min. On physical exam, a mild systolic murmur is heard over the apex, and her lungs are clear bilaterally. There is swelling of all the digits bilaterally, and a yellow-white plaque is noted beneath 3 of her nail beds. When asked about the plaques, she states that she was given itraconazole for them about 3 weeks ago; however, the plaques did not resolve. When asked further about joint pain, she notes that she has had shoulder and knee pain for the last several years, although she has not sought medical care for this. Which of the following is the best initial step in this patient’s therapeutic management?
A 19-year-old male arrives to student health for an annual check up. He is up to date on his infant and childhood vaccinations up to age 10. At age 12, he received a single dose of the tetanus, diphtheria, and acellular pertussis vaccine, and a quadrivalent meningococcal conjugate vaccine. A month ago, he received the influenza vaccine. The patient has no significant medical history. He takes over the counter ibuprofen for occasional headaches. He has a father with hypertension and hyperlipidemia, and his brother has asthma. He is sexually active with his current girlfriend. He denies tobacco use, illicit drug use, and recent or future travel. The patient’s temperature is 98°F (36.7°C), blood pressure is 118/78 mmHg, pulse is 70/min, and respirations are 14/min with an oxygen saturation of 99% O2 on room air. A physical examination is normal. What of the following is the best recommendation for vaccination?
A 57-year-old man with a history of coronary artery disease has been brought to the emergency department due to the sudden onset of chest pain. He was diagnosed with hypertension 12 years ago and takes enalapril regularly. The patient is hypotensive to 70/42 mm Hg, and on further examination his skin is cold and clammy. He is diagnosed with a life-threatening condition that resulted from inadequate circulation of blood, with decreased cardiac output and high pulmonary capillary wedge pressure. Which of the conditions below can cause the same disorder? I. Acute myocardial infarction II. Atrial fibrillation III. Hemorrhage IV. Valvular stenosis V. Pulmonary embolism VI. Sepsis
A 55-year-old man presents to the physician for the evaluation of excessive daytime sleepiness over the past six months. Despite sleeping 8–9 hours a night and taking a nap during the day, he feels drowsy and is afraid to drive. His wife complains of loud snoring and gasping during the night. His blood pressure is 155/95 mm Hg. BMI is 37 kg/m2. Oropharyngeal examination shows a small orifice and an enlarged tongue and uvula. The soft palate is low-lying. The examination of the nasal cavity shows no septal deviation or polyps. Examination of the lungs and heart shows no abnormalities. Polysomnography shows an apnea-hypopnea index of 20 episodes/h. The patient is educated about weight loss, exercise, and regular sleep hours and duration. Which of the following is the most appropriate next step in management?
A 60-year-old man comes to the emergency department because of a 3-day history of fever and shortness of breath. He has a history of COPD treated with inhaled albuterol. His temperature is 39.0°C (102.2°F), pulse is 95/min, respirations are 20/min, and blood pressure is 130/80 mm Hg. Cardiopulmonary examination shows decreased breath sounds and poor air movement over the left lung. A lateral decubitus x-ray of the chest shows a pleural effusion height of 2 cm. Thoracentesis is performed and pleural fluid analysis shows a protein concentration of 4.0 g/dL and LDH of 280 U/L. Which of the following is the most likely underlying cause of this patient's effusion?
A 59-year-old man is brought to the emergency department by a coworker for right arm weakness and numbness. The symptoms started suddenly 2 hours ago. His coworker also noticed his face appears to droop on the right side and his speech is slurred. He has a history of hypertension, hyperlipidemia, type 2 diabetes, and peripheral arterial disease. He works as a partner at a law firm and has been under more stress than usual lately. His father died of a stroke at age 70. The patient has smoked a pack of cigarettes daily for the last 40 years. He drinks two pints (750 mL) of whiskey each week. He takes aspirin, atorvastatin, lisinopril, and metformin daily. He is 167.6 cm (5 ft 6 in) tall and weighs 104.3 kg (230 lb); BMI is 37 kg/m2. His temperature is 37.1°C (98.8°F), pulse is 92/min, respirations are 15/min, and blood pressure is 143/92 mm Hg. He is fully alert and oriented. Neurological examination shows asymmetry of the face with droop of the lips on the right. There is 3/5 strength in right wrist flexion and extension, and right finger abduction. Sensation to light touch and pinprick is reduced throughout the right arm. Which of the following is the strongest predisposing factor for this patient's condition?
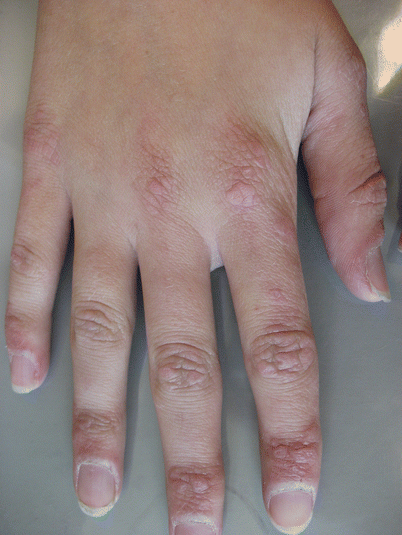
A 56-year-old woman comes to the physician because of increasing muscle weakness in her shoulders and legs for 1 month. She has difficulties standing up and combing her hair. She also has had a skin rash on her face and hands for the past week. She has hypercholesterolemia treated with simvastatin. She has chronic eczema of her feet that is well-controlled with skin moisturizer and corticosteroid cream. Her mother and sister have thyroid disease. Vital signs are within normal limits. Examination shows facial erythema. A photograph of her hands is shown. Muscle strength is 3/5 in the iliopsoas, hamstring, deltoid, and biceps muscles. Sensation to pinprick, temperature, and vibration is intact. Further evaluation of this patient is most likely to show which of the following?
A previously healthy 61-year-old man comes to the physician because of a 6-month history of morning headaches. He also has fatigue and trouble concentrating on his daily tasks at work. He sleeps for 8 hours every night; his wife reports that he sometimes stops breathing for a few seconds while sleeping. His pulse is 71/min and blood pressure is 158/96 mm Hg. He is 178 cm (5 ft 10 in) tall and weighs 100 kg (220 lb); BMI is 31.6 kg/m2 . Which of the following is the most likely cause of this patient's hypertension?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
