Cardiology — MCQs

On this page
A 42-year-old woman comes to the physician because of a 2-week history of joint pain and fatigue. She has a history of multiple unprovoked deep vein thromboses. Physical examination shows small bilateral knee effusions and erythematous raised patches with scaling and follicular plugging over the ears and scalp. Oral examination shows several small ulcers. Laboratory evaluation of this patient is most likely to show which of the following?
A previously healthy 26-year-old man is brought to the emergency department 30 minutes after collapsing during soccer practice. The patient appears well. His pulse is 73/min and blood pressure is 125/78 mm Hg. Cardiac examination is shown. Rapid squatting decreases the intensity of the patient's auscultation finding. Which of the following is the most likely cause of this patient's condition?
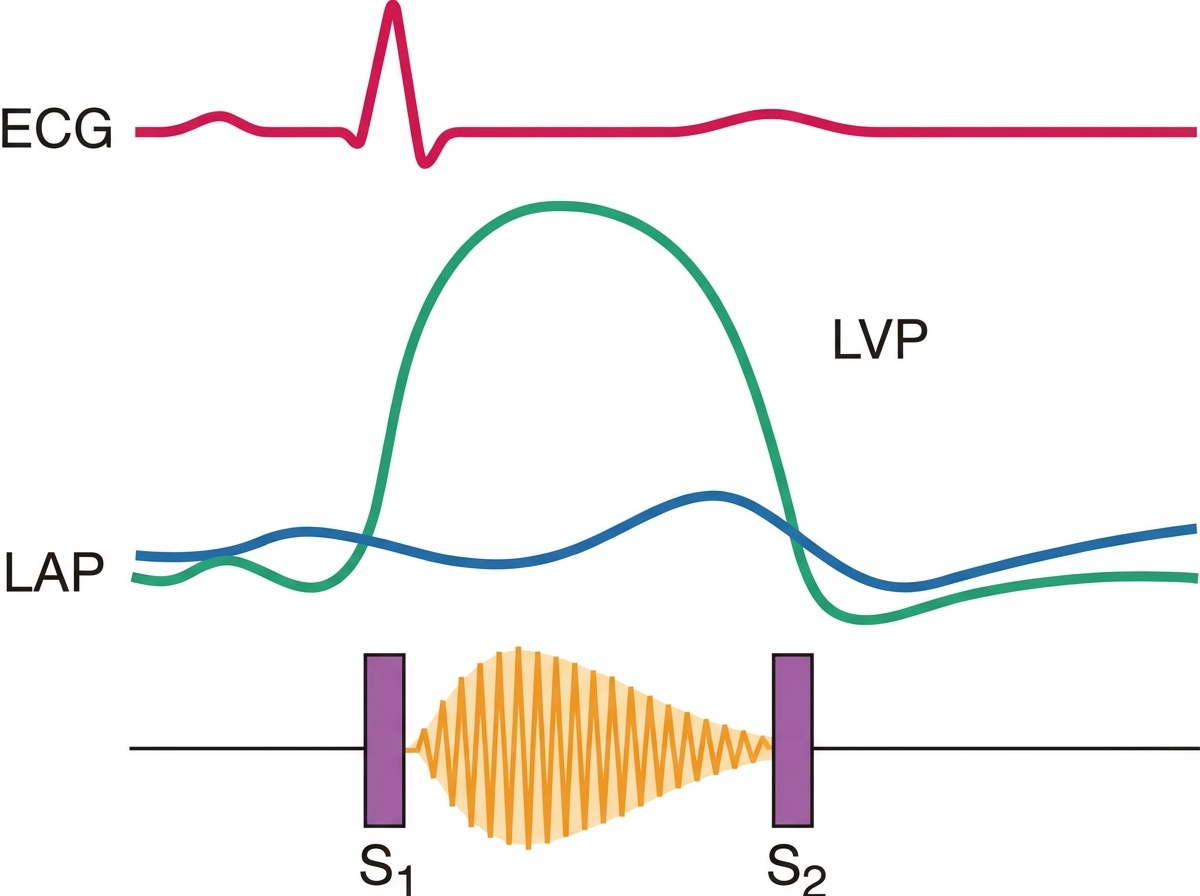
A 74-year-old man comes to the physician for a 6-month history of progressively worsening fatigue and shortness of breath on exertion. He immigrated to the United States 35 years ago from India. His pulse is 89/min and blood pressure is 145/60 mm Hg. Crackles are heard at the lung bases. Cardiac examination shows a grade 3/6 early diastolic murmur loudest at the third left intercostal space. Further evaluation of this patient is most likely to show which of the following?
A 55-year-old woman complains of daytime somnolence. Her BMI is 32 kg/m² and her husband says she snores frequently during the night. Polysomnography test reveals the patient experiences more than 5 obstructive events an hour. The patient is at increased risk of developing which of the following?
A 61-year-old man presents to the emergency department with new-onset dizziness. He reports associated symptoms of confusion, headaches, and loss of coordination. The patient’s wife also mentions he has had recent frequent nosebleeds. Physical examination demonstrates a double vision. Routine blood work is significant for a slightly reduced platelet count. A noncontrast CT of the head is normal. A serum protein electrophoresis is performed and shows an elevated IgM spike. The consulting hematologist strongly suspects Waldenström’s macroglobulinemia. Which of the following is the best course of treatment for this patient?
A previously healthy 20-year-old man is brought to the emergency department 15 minutes after collapsing while playing basketball. He has no history of serious illness. On arrival, there is no palpable pulse or respiratory effort observed. He is declared dead. The family agrees to an autopsy. Cardiac workup prior to this patient's death would most likely have shown which of the following findings?
A 51-year-old man presents to his physician with increased thirst, frequent urination, and fatigue. These symptoms have increased gradually over the past 3 years. He has no past medical history or current medications. Also, he has no family history of endocrinological or cardiovascular diseases. The blood pressure is 140/90 mm Hg, and the heart rate is 71/min. The patient is afebrile. The BMI is 35.4 kg/m2. On physical examination, there is an increased adipose tissue over the back of the neck, and hyperpigmentation of the axilla and inguinal folds. Which of the following laboratory results is diagnostic of this patient’s most likely condition?
A 12-year-old girl is brought to the physician by her mother because she has been waking up multiple times at night to go to the bathroom even though she avoids drinking large amounts of water close to bedtime. She has no significant medical history apart from 3 episodes of lower urinary tract infections treated with nitrofurantoin in the past 2 years. Her family emigrated from Nigeria 10 years ago. Physical examination shows no abnormalities. Laboratory studies show: Hemoglobin 14.2 g/dL MCV 92 fL Reticulocytes 1.5% Serum Osmolality 290 mOsmol/kg H2O Urine Leukocytes negative Nitrite negative Glucose negative Osmolality 130 mOsmol/kg H2O Hemoglobin electrophoresis shows: HbA 56% HbS 43% HbF 1% This patient is at greatest risk for which of the following conditions?
A 55-year-old man presents to the family medicine clinic after noticing a gradually enlarging smooth and symmetrical bump on his left forearm at the site of his PPD placement 2 days ago. The patient takes lisinopril for hypertension and metformin for diabetes mellitus type 2. He was screened for tuberculosis 2 days ago as a requirement for work. He works as a guard at the county prison. He smokes a half-pack of cigarettes per day and has done so for the last 5 years. His heart rate is 88/min, respiratory rate is 16/min, temperature is 37.3°C (99.2°F), and blood pressure is 142/86 mm Hg. The patient appears clean and overweight. The bleb from the screening test is measured at 12 mm. Acid-fast smear of a sputum sample is negative. Which of the following is recommended for the patient at this time?
A 50-year-old man presents to his primary care physician for management of a lung nodule. The nodule was discovered incidentally when a chest radiograph was performed to rule out pneumonia. The nodule is 8.5 mm in size and was confirmed by CT. The patient is otherwise healthy, has never smoked, and exercises regularly. The patient works in a dairy factory. He has had no symptoms during this time. His temperature is 97.6°F (36.4°C), blood pressure is 122/81 mmHg, pulse is 83/min, respirations are 12/min, and oxygen saturation is 98% on room air. Physical exam including auscultation of the lungs is unremarkable. Which of the following is the most appropriate next step in management?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
