Cardiology — MCQs

On this page
A 58-year-old female presents to her primary care physician with complaints of chest pain and palpitations. A thorough past medical history reveals a diagnosis of rheumatic fever during childhood. Echocardiography is conducted and shows enlargement of the left atrium and narrowing of the mitral valve opening. Which of the following should the physician expect to hear on cardiac auscultation?
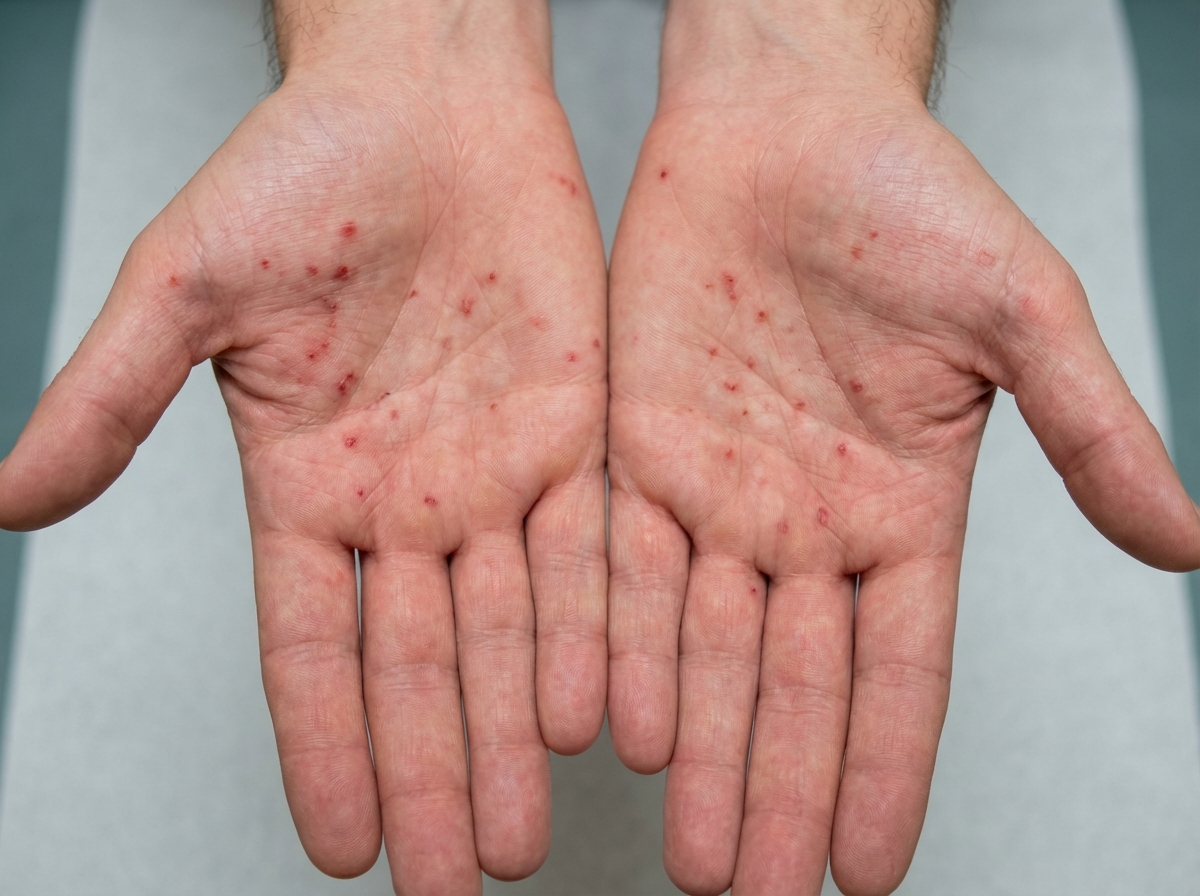
A 34-year-old male is brought to the emergency department. He has prior hospitalizations for opiate overdoses, but today presents with fever, chills, rigors and malaise. On physical exam vitals are temperature: 100.5 deg F (38.1 deg C), pulse is 105/min, blood pressure is 135/60 mmHg, and respirations are 22/min. You note the following findings on the patient's hands (Figures A and B). You note that as the patient is seated, his head bobs with each successive heart beat. Which of the following findings is most likely present in this patient?
A 47-year-old man presents for a routine physical examination as part of an insurance medical assessment. He has no complaints and has no family history of cardiac disease or sudden cardiac death. His blood pressure is 120/80 mm Hg, temperature is 36.7°C (98.1°F), and pulse is 75/min and is regular. On physical examination, he appears slim and his cardiac apex beat is of normal character and non-displaced. On auscultation, he has a midsystolic click followed by a late-systolic high-pitched murmur over the cardiac apex. On standing, the click and murmur occur earlier in systole, and the murmur is of increased intensity. While squatting, the click and murmur occur later in systole, and the murmur is softer in intensity. Echocardiography of this patient will most likely show which of the following findings?
A 44-year-old male immigrant presents to his primary care physician for a new patient visit. The patient reports chronic fatigue but states that he otherwise feels well. His past medical history is not known, and he is not currently taking any medications. The patient admits to drinking 7 alcoholic beverages per day and smoking 1 pack of cigarettes per day. His temperature is 99.4°F (37.4°C), blood pressure is 157/98 mmHg, pulse is 99/min, respirations are 18/min, and oxygen saturation is 100% on room air. Physical exam demonstrates mild pallor but is otherwise not remarkable. Laboratory studies are ordered as seen below. Hemoglobin: 9 g/dL Hematocrit: 33% Leukocyte count: 6,500/mm^3 with normal differential Platelet count: 190,000/mm^3 Mean corpuscular volume (MCV): 60 femtoliters Free iron: 272 mcg/dL Total iron binding capacity (TIBC): 175 mcg/dL Ferritin: 526 ng/mL Reticulocyte count: 2.8% Which of the following is the most likely diagnosis?
A 46-year-old male was found unconscious in the field and brought to the emergency department by EMS. The patient was intubated in transit and given a 2 liter bolus of normal saline. On arrival, the patient's blood pressure is 80/60 mmHg and temperature is 37.5°C. Jugular veins are flat and capillary refill time is 4 seconds. Vascular parameters are measured and are as follows: Cardiac index - Low Pulmonary capillary wedge pressure (PCWP) - Low Systemic vascular resistance - High Which of the following is the most likely diagnosis?
A 59-year-old man presents with the persistent right-sided facial droop and slurred speech for the past 2 hours. He says he had similar symptoms 6 months ago which resolved within 1 hour. His past medical history is significant for long-standing hypertension, managed with hydrochlorothiazide. He reports a 10-pack-year smoking history but denies any alcohol or recreational drug use. The vital signs include: blood pressure 145/95 mm Hg, pulse 95/min, and respiratory rate 18/min. On physical examination, the patient has an asymmetric smile and right-sided weakness of his lower facial muscles. There is a deviation of his tongue towards the right. Dysarthria is noted. His muscle strength in the upper extremities is 4/5 on the right and 5/5 on the left. The remainder of the physical exam is unremarkable. Which of the following is the next most appropriate step in the management of this patient?
A 62-year-old female presents with complaint of chronic productive cough for the last 4 months. She states that she has had 4-5 month periods of similar symptoms over the past several years. She has never smoked, but she reports significant exposure to second-hand smoke in her home. She denies any fevers, reporting only occasional shortness of breath and a persistent cough where she frequently expectorates thick, white sputum. Vital signs are as follows: T 37.1 C, HR 88, BP 136/88, RR 18, O2 sat 94% on room air. Physical exam is significant for bilateral end-expiratory wheezes, a blue tint to the patient's lips and mucous membranes of the mouth, and a barrel chest. Which of the following sets of results would be expected on pulmonary function testing in this patient?
A 32-year-old man is brought into the emergency department by his friends. The patient was playing soccer when he suddenly became short of breath. The patient used his albuterol inhaler with minimal improvement in his symptoms. He is currently struggling to breathe. The patient has a past medical history of asthma and a 25 pack-year smoking history. His current medications include albuterol, fluticasone, and oral prednisone. His temperature is 99.5°F (37.5°C), blood pressure is 137/78 mmHg, pulse is 120/min, respirations are 27/min, and oxygen saturation is 88% on room air. On pulmonary exam, the patient exhibits no wheezing with bilateral minimal air movement. The patient’s laboratory values are ordered as seen below. Hemoglobin: 15 g/dL Hematocrit: 43% Leukocyte count: 5,500/mm^3 with normal differential Platelet count: 194,000/mm^3 Serum: Na+: 138 mEq/L Cl-: 102 mEq/L K+: 4.4 mEq/L HCO3-: 24 mEq/L BUN: 20 mg/dL Glucose: 120 mg/dL Creatinine: 1.0 mg/dL Ca2+: 10.2 mg/dL pH: 7.44 PaCO2: 10 mmHg PaO2: 60 mmHg AST: 12 U/L ALT: 10 U/L The patient is started on an albuterol nebulizer, magnesium sulfate, and tiotropium bromide. Repeat vitals reveal an oxygen saturation of 90% with a pulse of 115/min. Laboratory values are repeated as seen below. pH: 7.40 PaCO2: 44 mmHg PaO2: 64 mmHg Which of the following is the next best step in management of this patient?
A 71-year-old man comes to the physician for routine health maintenance examination. He feels well. He has hypertension and gastroesophageal reflux disease. Current medications include metoprolol and pantoprazole. He does not smoke or drink alcohol. Temperature is 37.3°C (99.1°F), pulse is 75/min, and blood pressure 135/87 mm Hg. Examination shows no abnormalities. Laboratory studies show: Hematocrit 43% Leukocyte count 32,000/mm3 Segmented neutrophils 22% Basophils 1% Eosinophils 2% Lymphocytes 74% Monocytes 1% Platelet count 190,000/mm3 Blood smear shows small, mature lymphocytes and several smudge cells. Immunophenotypic analysis with flow cytometry shows B-cells that express CD19, CD20 and CD23. Which of the following is the most appropriate next step in management?
A 24-year-old man comes to the physician for a 1-week history of a painless swelling on the right side of his neck that he noticed while showering. He is 203 cm (6 ft 8 in) tall and weighs 85 kg (187 lb); BMI is 21 kg/m2. Physical examination shows long, thin fingers and an increased arm-length to body-height ratio. Examination of the neck shows a single 2-cm firm nodule. Ultrasonography of the neck shows a hypoechoic thyroid lesion with irregular margins. A core needle biopsy of the thyroid lesion shows sheets of polygonal cells surrounded by Congo red-stained amorphous tissue. Which of the following additional findings is most likely in this patient?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
