Cardiology — MCQs

On this page
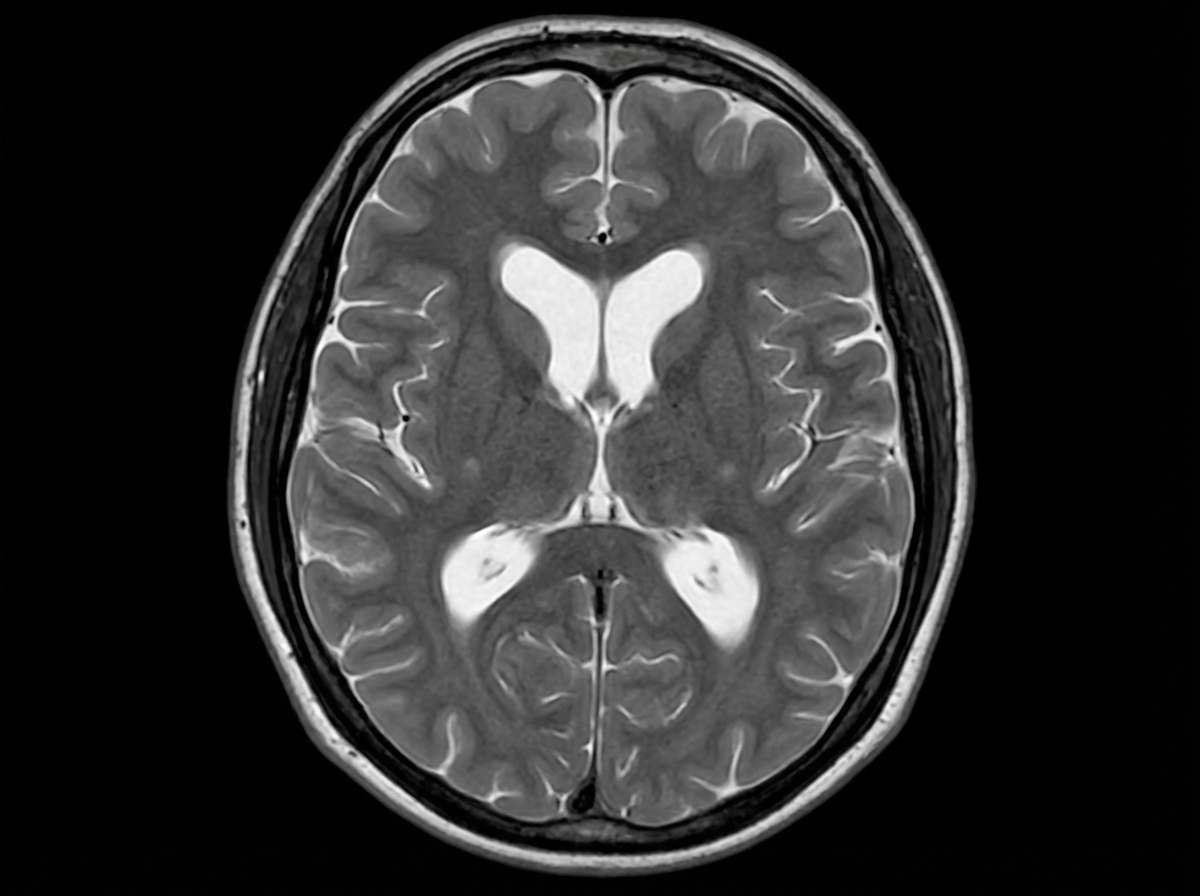
A 74-year-old man is brought to the physician by his wife for progressively worsening confusion and forgetfulness. Vital signs are within normal limits. Physical examination shows a flat affect and impaired short-term memory. An MRI of the brain is shown. Further evaluation of this patient is most likely to show which of the following findings?
A 20-year-old woman visits the clinic for her annual physical examination. She does not have any complaints during this visit. The past medical history is insignificant. She follows a healthy lifestyle with a balanced diet and moderate exercise schedule. She does not smoke or drink alcohol. She does not take any medications currently. The family history is significant for her grandfather and uncle who had their parathyroid glands removed. The vital signs include: blood pressure:122/88 mm Hg, pulse 88/min, respirations 17/min, and temperature 36.7°C (98.0°F). The physical exam is within normal limits. The lab test results are as follows: Blood Urea Nitrogen 12 mg/dL Serum Creatinine 1.1 mg/dL Serum Glucose (Random) 88 mg/dL Serum chloride 107 mmol/L Serum potassium 4.5 mEq/L Serum sodium 140 mEq/L Serum calcium 14.5 mg/dL Serum albumin 4.4 gm/dL Parathyroid Hormone (PTH) 70 pg/mL (Normal: 10-65 pg/mL) 24-Hr urinary calcium 85 mg/day (Normal: 100–300 mg/day) Which of the following is the next best step in the management of this patient?
A 74-year-old woman is brought to the physician by her daughter for worsening memory for the past 1 month. She can no longer manage her bills and frequently forgets the names of her children. Her daughter is also concerned that her mother has a urinary tract infection because she has had increased urinary urgency and several episodes of urinary incontinence. Vital signs are within normal limits. Physical examination shows poor short-term memory recall and a slow gait with wide, short steps. Which of the following is most likely to improve this patient's condition?
A 48-year-old woman comes to the physician because of an increasingly painful swelling behind her right knee for the past 2 months. During this time, she has also had intermittent low-grade fever and she has been more fatigued than usual. She has not had any trauma to the knee. Over the past year, she has had occasional pain in her hands and wrists bilaterally. She has hypertension and type 2 diabetes mellitus. She drinks 1–2 glasses of wine daily and occasionally more on weekends. Current medications include enalapril, metformin, and glimepiride. Her mother and older brother have osteoarthritis. She is 165 cm (5 ft 5 in) tall and weighs 68 kg (150 lb); BMI is 25 kg/m2. Vital signs are within normal limits. Examination shows a 3-cm nontender mass in the right popliteal fossa that becomes prominent when the knee is extended. There is mild swelling and redness of her right knee joint. Which of the following is the most likely diagnosis?
A 24-year-old woman presents with episodic shortness of breath, chest tightness, and wheezing. She has noticed an increased frequency of such episodes in the spring season. She also has a history of urticaria. She has smoked a half pack of cigarettes per day over the last 5 years. Her mother also has similar symptoms. The physical exam is within normal limits. Which of the following findings is characteristic of her condition?
A 55-year-old man with a BMI of 34 kg/m² presents to his primary care physician for knee pain. The patient has had left knee pain, which has been steadily worsening for the past year. He states that ice and rest has led to minor improvement in his symptoms. He recently bumped his knee; however, he says that it has not altered his baseline pain when ambulating. The patient is a butcher and lives with his wife. His current medications include insulin, metformin, hydrochlorothiazide, and lisinopril. He is attending Alcoholics Anonymous with little success. Physical exam reveals a left knee that is mildly erythematous with some bruising. There is no pain upon palpation of the joint or with passive range of motion. The patient exhibits a mildly antalgic gait. Which of the following is the best initial step in management?
A 25-year-old woman presents to her primary care clinic for a general checkup. She states she's been a bit more fatigued lately during finals season but is otherwise well. Her mother and sister have hypothyroidism. She denies weight gain, cold intolerance, constipation, heavy or irregular menses, or changes in the quality of her hair, skin, or nails. Physical exam is unremarkable. Laboratory studies are ordered as seen below. Hemoglobin: 14 g/dL Hematocrit: 40% Leukocyte count: 5,500/mm^3 with normal differential Platelet count: 188,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 102 mEq/L K+: 4.4 mEq/L HCO3-: 24 mEq/L BUN: 20 mg/dL Glucose: 99 mg/dL Creatinine: 0.8 mg/dL Ca2+: 10.2 mg/dL Antithyroid peroxidase Ab: Positive AST: 12 U/L ALT: 10 U/L Which of the following laboratory values is most likely in this patient?
A 43-year-old woman presents to her primary care physician with complaints of mild shortness of breath and right-sided chest pain for three days. She reports that lately she has had a nagging nonproductive cough and low-grade fevers. On examination, her vital signs are: temperature 99.1 deg F (37.3 deg C), blood pressure is 115/70 mmHg, pulse is 91/min, respirations are 17/min, and oxygen saturation 97% on room air. She is well-appearing, with normal work of breathing, and no leg swelling. She is otherwise healthy, with no prior medical or surgical history, currently taking no medications. The attending has a low suspicion for the most concerning diagnosis and would like to exclude it with a very sensitive though non-specific test. Which of the following should this physician order?
A 75-year-old woman presents with sudden loss of vision. She says that she was reading when suddenly she was not able to see the print on half of the page. Her symptoms started 4 hours ago and are accompanied by a severe posterior headache. Vital signs reveal the following: blood pressure 119/76 mm Hg, pulse 89/min, SpO2 98% on room air. The patient was unable to recognize her niece when she arrived to see her. A noncontrast CT of the head shows no evidence of hemorrhagic stroke. What is the most likely diagnosis in this patient?
A 49-year-old man is referred to a cardiologist by his primary care provider (PCP) for a new heart murmur. He otherwise feels well and has no complaints. He had not seen a doctor in the last 15 years but finally went to his PCP for a check-up at the urging of his girlfriend. His past medical history is notable for gastroesophageal reflux disease, hypertension, and hepatitis B. He takes omeprazole and lisinopril. He has a prior history of intravenous drug abuse and a 50-pack-year smoking history. He has had many prior sexual partners and uses protection intermittently. He reports that he may have had a sore on his penis many years ago, but it went away without treatment. His temperature is 99°F (37.2°C), blood pressure is 141/91 mmHg, pulse is 89/min, and respirations are 18/min. On exam, S1 is normal and S2 has a tambour-like quality. There is a visible and palpable pulsation in the suprasternal notch and a diastolic decrescendo murmur over the right upper sternal border. A chest radiograph demonstrates calcification of the aortic root. Which of the following is the most likely cause of this patient's condition?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
