Cardiology — MCQs

On this page
A 19-year-old basketball player unexpectedly collapses on the court. Several minutes later he returns to consciousness and is able to continue playing. This has happened several times before with similar outcomes. He had no significant past medical history. Which of the following is most likely to be found in this patient?
A 67-year-old man with a past medical history of poorly-controlled type 2 diabetes mellitus (T2DM) is brought to the emergency department for acute onset nausea and vomiting. According to the patient, he suddenly experienced vertigo and began vomiting 3 hours ago while watching TV. He reports hiking in New Hampshire with his wife 2 days ago. Past medical history is significant for a myocardial infarction (MI) that was treated with cardiac stenting, T2DM, and hypertension. Medications include lisinopril, aspirin, atorvastatin, warfarin, and insulin. Physical examination demonstrates left-sided facial droop and decreased pinprick sensation at the right arm and leg. What is the most likely etiology of this patient’s symptoms?
A 19-year-old woman presents to her gynecologist’s office stating that she has never had a period. She is slightly alarmed because most of her friends in college have been menstruating for years. She is also concerned about her short stature. When she previously visited her family physician during early puberty, she was told that she will gain the appropriate height during her final teenage years. However, over the past few years, she has gained only a couple of inches. On examination, she has a wide chest and short neck. Her breast development is at Tanner stage 1. Her external genitalia is normal with sparse hair distribution over the mons pubis. Her gynecologist suspects a genetic condition and sends her for genetic counseling. Based on her clinical findings, which of the following diseases is she most likely to develop?
A 29-year-old woman presents to the emergency department with joint pain and a notable rash. She has had joint pain for the past 12 months but noticed the rash recently as well as generalized malaise. She states her joint pain is symmetric, in her upper extremities, and is worse in the morning. Her temperature is 97.6°F (36.4°C), blood pressure is 111/74 mmHg, pulse is 83/min, respirations are 14/min, and oxygen saturation is 98% on room air. Laboratory studies are ordered as seen below. Hemoglobin: 10 g/dL Hematocrit: 30% Leukocyte count: 6,800/mm^3 with normal differential Platelet count: 207,000/mm^3 Serum: Na+: 140 mEq/L Cl-: 101 mEq/L K+: 4.9 mEq/L HCO3-: 21 mEq/L BUN: 30 mg/dL Glucose: 120 mg/dL Creatinine: 1.8 mg/dL The patient is ultimately admitted to the hospital. Which of the following is the most appropriate test to monitor her disease progression?
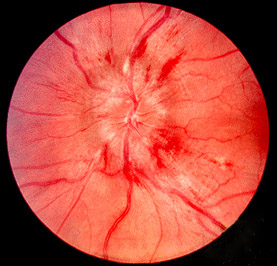
A 72-year-old woman comes to the emergency department 1 hour after the sudden onset of a diffuse, dull, throbbing headache. She also reports blurred vision, nausea, and one episode of vomiting. She has a history of poorly controlled hypertension. A photograph of her fundoscopic examination is shown. Which of the following is the most likely underlying cause of this patient's symptoms?
A 63-year-old man undergoes workup for nocturnal dyspnea and what he describes as a "choking" sensation while sleeping. He also endorses fatigue and dyspnea on exertion. Physical exam reveals a normal S1, loud P2, and a neck circumference of 17 inches (43 cm) (normal < 14 inches (< 35 cm)). His temperature is 98.8°F (37°C), blood pressure is 128/82 mmHg, pulse is 86/min, and respirations are 19/min. He undergoes spirometry, which is unrevealing, and polysomnography, which shows 16 hypopneic and apneic events per hour. Mean pulmonary arterial pressure is 30 mmHg. Which of the following complications is this patient most at risk for?
A 22-year-old man comes to the emergency department because of several episodes of blood in his urine and decreased urine output for 5 days. His blood pressure is 158/94 mm Hg. Examination shows bilateral lower extremity edema. Urinalysis shows 3+ protein and red blood cell casts. Mass spectrometry analysis of the urinary protein detects albumin, transferrin, and IgG. Which of the following best describes this type of proteinuria?
A 28-year-old woman comes to the emergency department for a rash that began 3 days ago. She has low-grade fever and muscle aches. She has no history of serious illness and takes no medications. She has had 5 male sexual partners over the past year and uses condoms inconsistently. Her temperature is 38.1°C (100.6° F), pulse is 85/min, and blood pressure is 126/89 mm Hg. Examination shows a diffuse maculopapular rash that includes the palms and soles. The remainder of the examination shows no abnormalities. A venereal disease research laboratory (VDRL) test is positive. Which of the following is the next appropriate step in management?
A 34-year-old man with a 2-year history of rheumatoid arthritis is being evaluated on a follow-up visit. He is currently on methotrexate and celecoxib for pain management and has shown a good response until now. However, on this visit, he mentions that the morning stiffness has been getting progressively worse. On physical examination, both his wrists are erythematous and swollen, nodules on his elbows are also noted. Rheumatoid factor is 30 (normal reference values: < 15 IU/mL), ESR is 50 mm/h, anti-citrullinated protein antibodies is 55 (normal reference values: < 20). What is the next best step in the management of this patient?
A 62-year-old man comes to the physician in May for a routine health maintenance examination. He feels well. He underwent a right inguinal hernia repair 6 months ago. He has hypertension and type 2 diabetes mellitus. There is no family history of serious illness. Current medications include metformin, sitagliptin, enalapril, and metoprolol. He received the zoster vaccine 1 year ago. He received the PPSV23 vaccine 4 years ago. His last colonoscopy was 7 years ago and was normal. He smoked a pack of cigarettes a day for 20 years but quit 17 years ago. He drinks two to three alcoholic beverages on weekends. He is allergic to amoxicillin. He is scheduled to visit Australia and New Zealand in 2 weeks to celebrate his 25th wedding anniversary. He appears healthy. Vital signs are within normal limits. An S4 is heard at the apex. The remainder of the examination shows no abnormalities. Which of the following is the most appropriate recommendation at this time?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
