Cardiology — MCQs

On this page
What does the following ECG show?
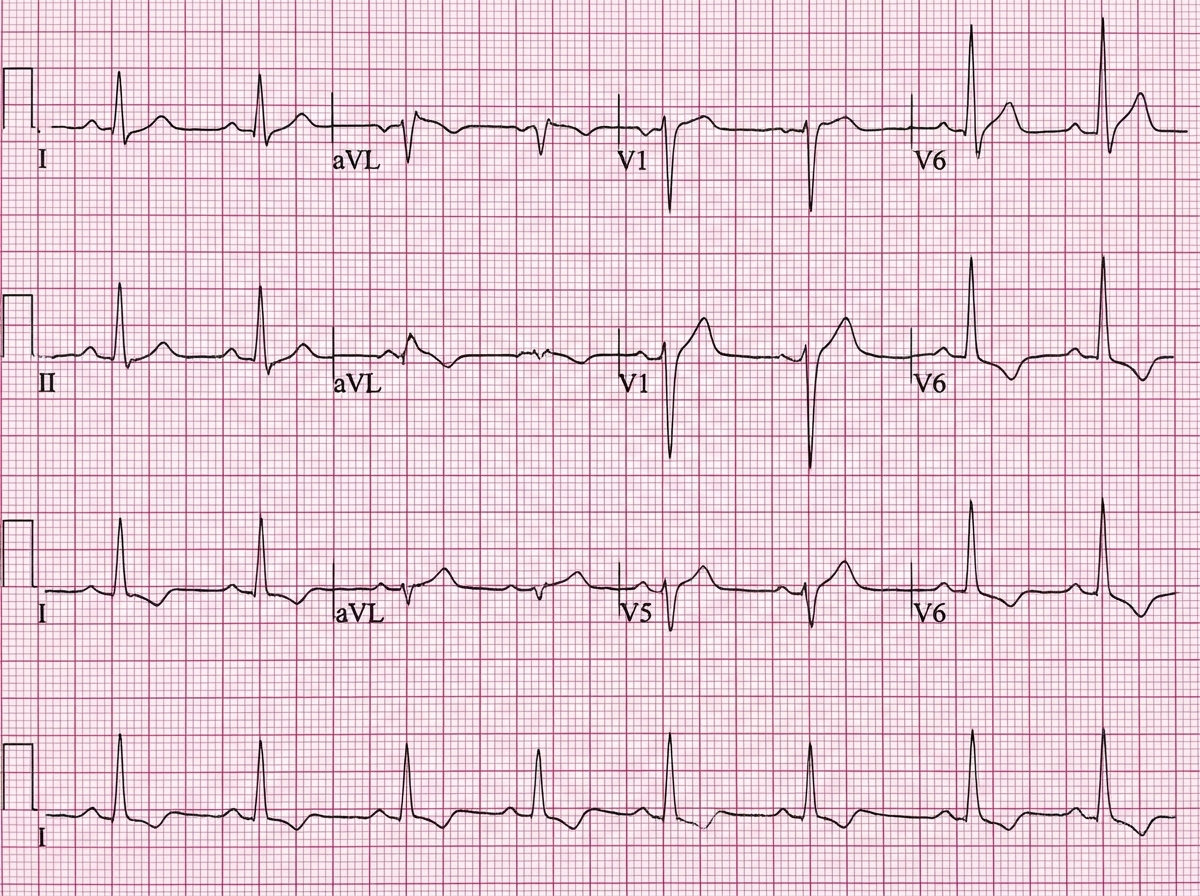
A 55-year-old woman with non-ischemic cardiomyopathy presents with palpitations. ECG shows:
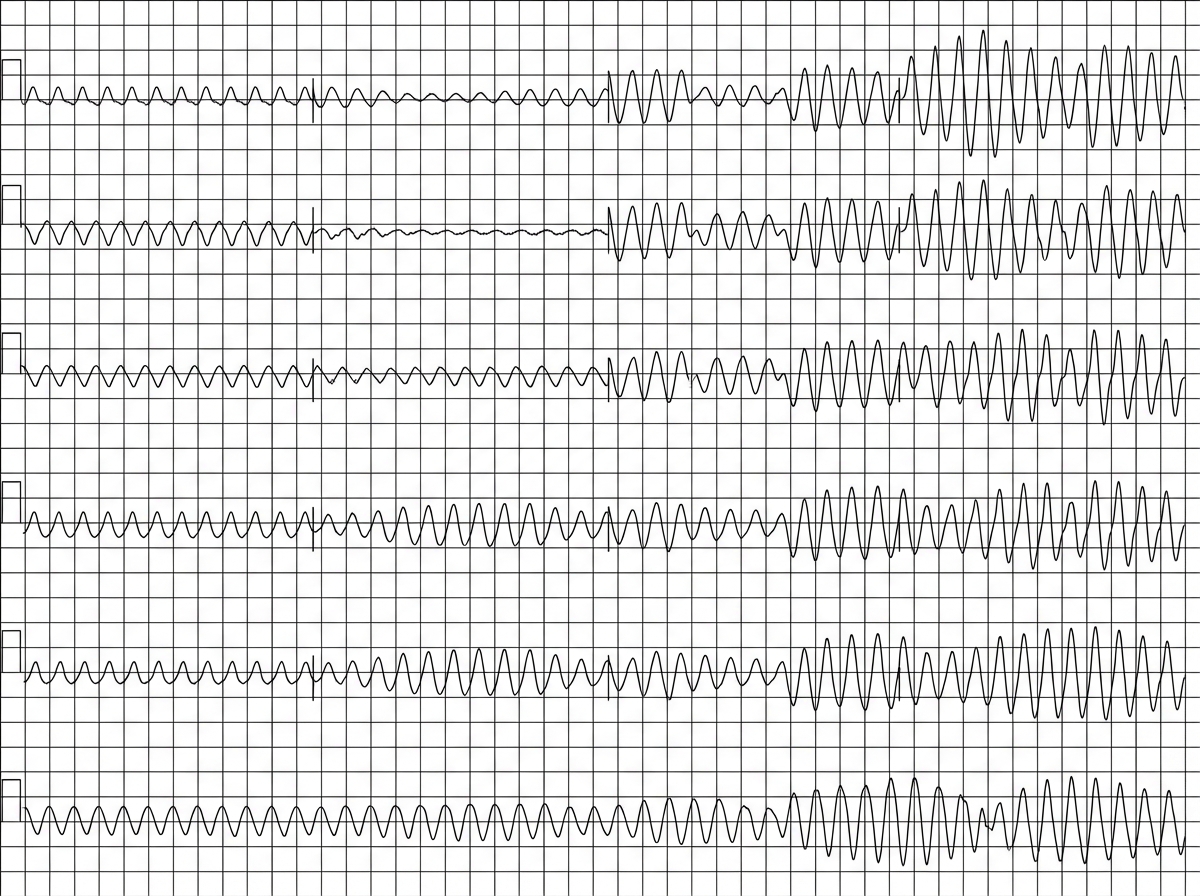
A patient becomes pulseless and his BP crashes after myocardial infarction. Diagnosis is:
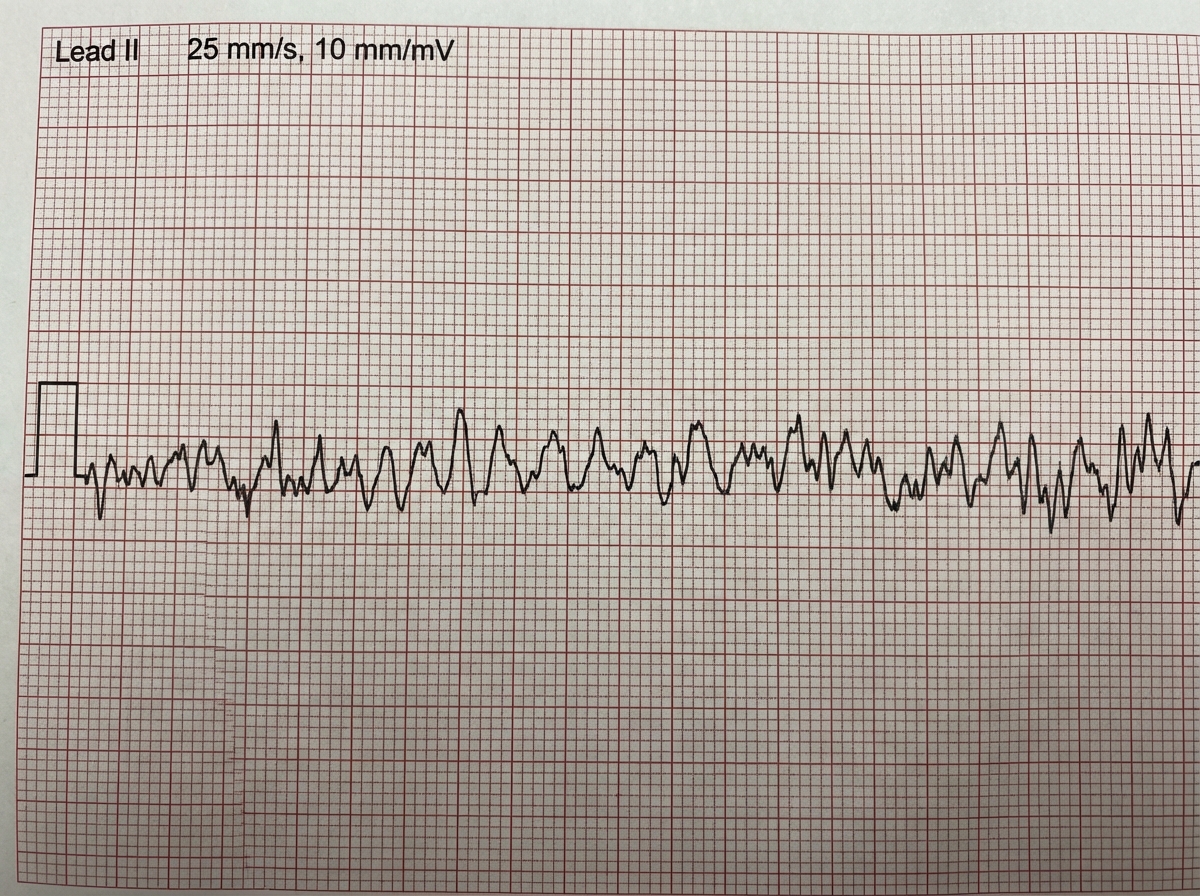
A 68 -year-old man presents with symptoms of alcohol withdrawal. ECG shows:
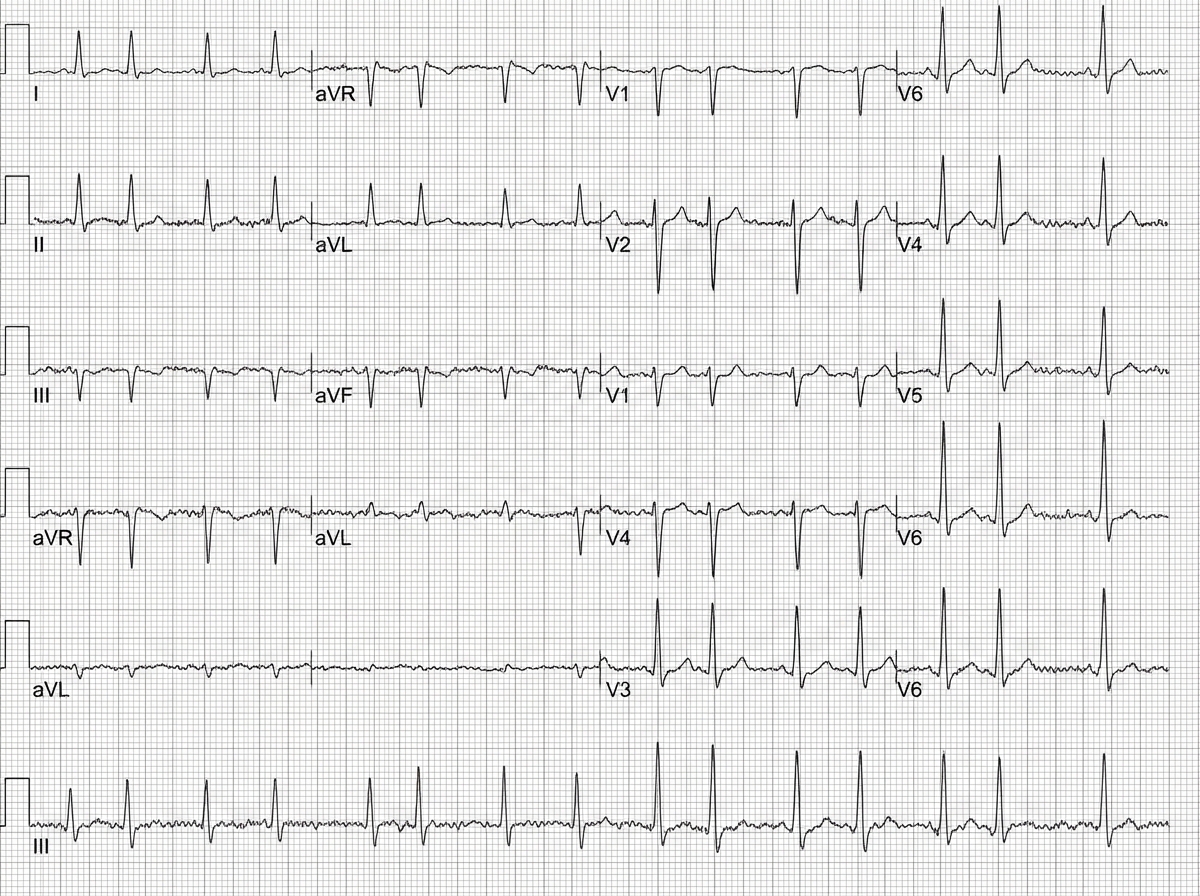
Comment on the diagnosis from the ECG shown below:
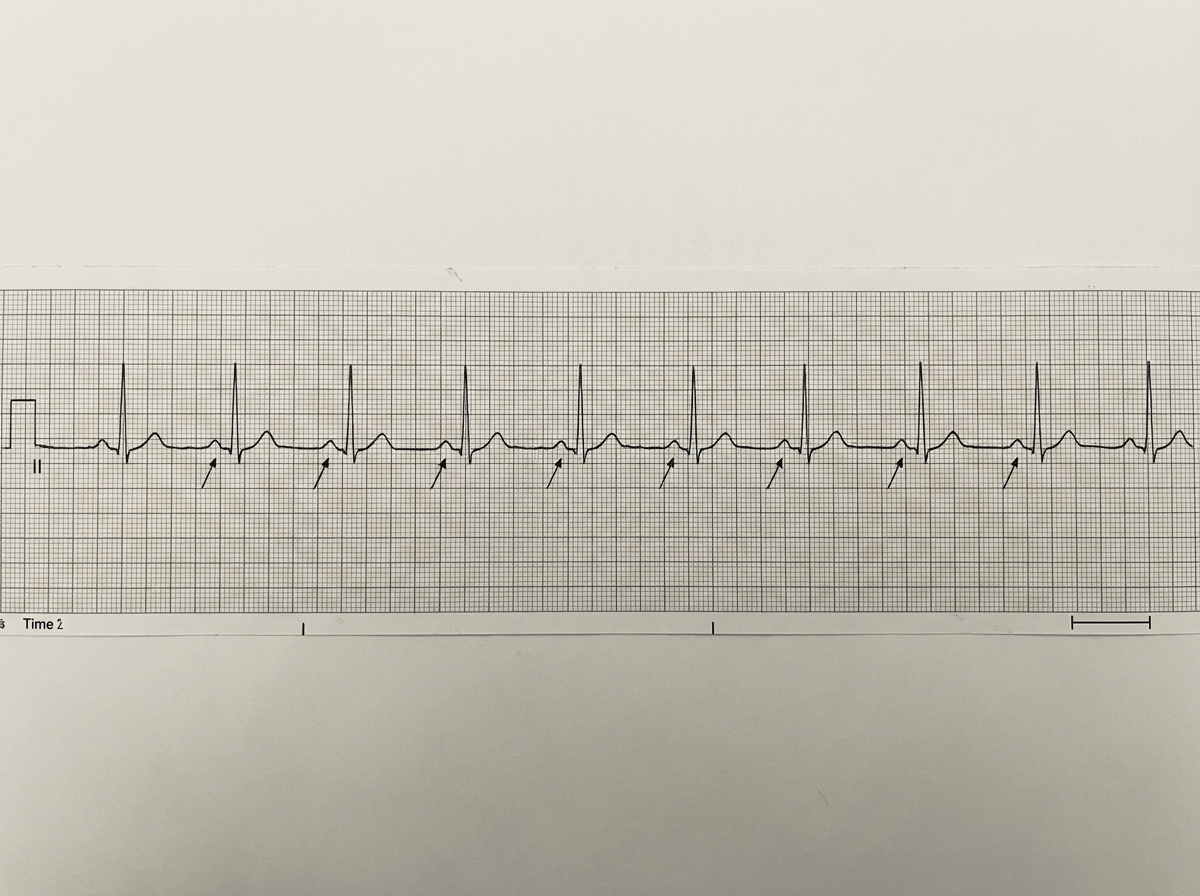
In the ECG shown below, which drug will not be given?
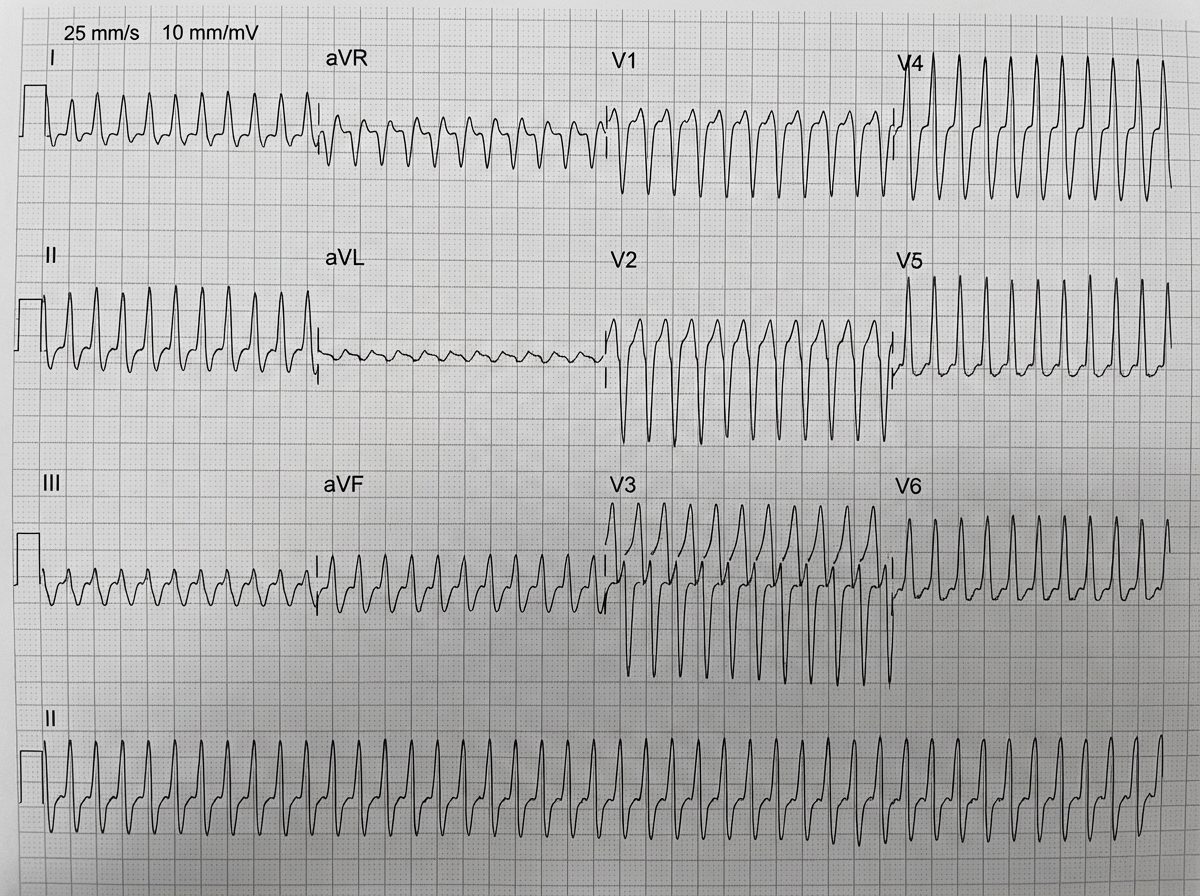
What does the following ECG show?
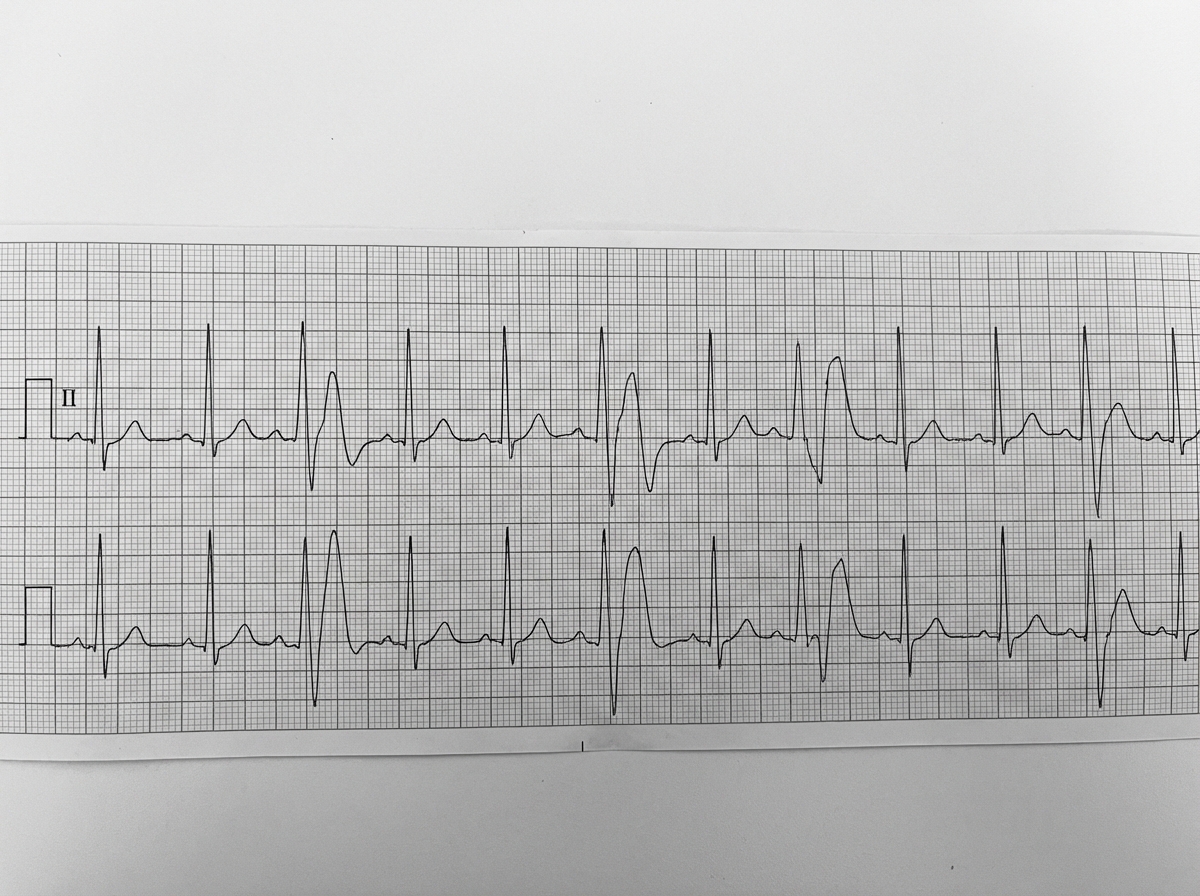
A 35-year-old lady has been diagnosed with anxiety neurosis by her psychiatrist. She came to you for second opinion. Comment on the diagnosis based on ECG.
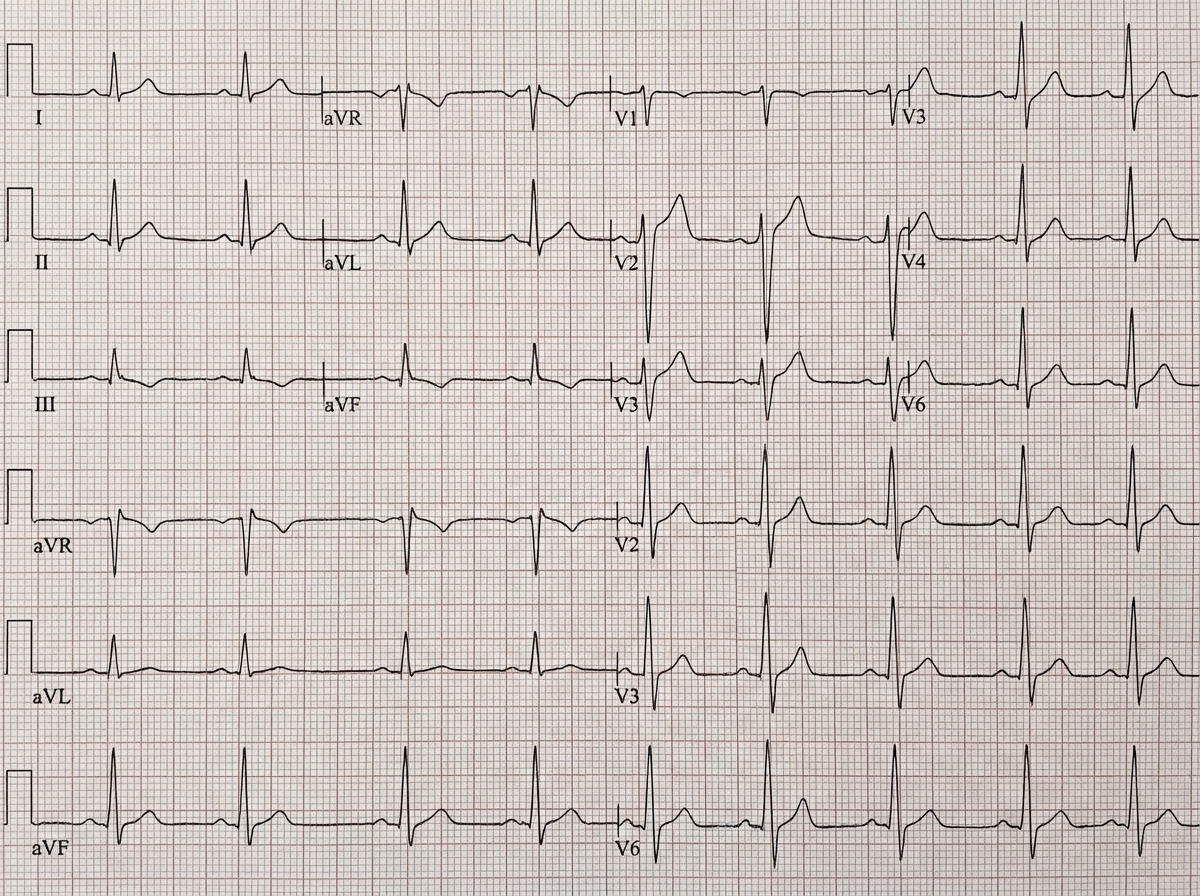
A 46-year-old man presents with diffuse chest pain at rest and recent history of cough, fever and rhinorrhea lasting for 3 days. ECG shows diffuse ST-segment elevation with PR-segment depression. What is the most likely diagnosis?
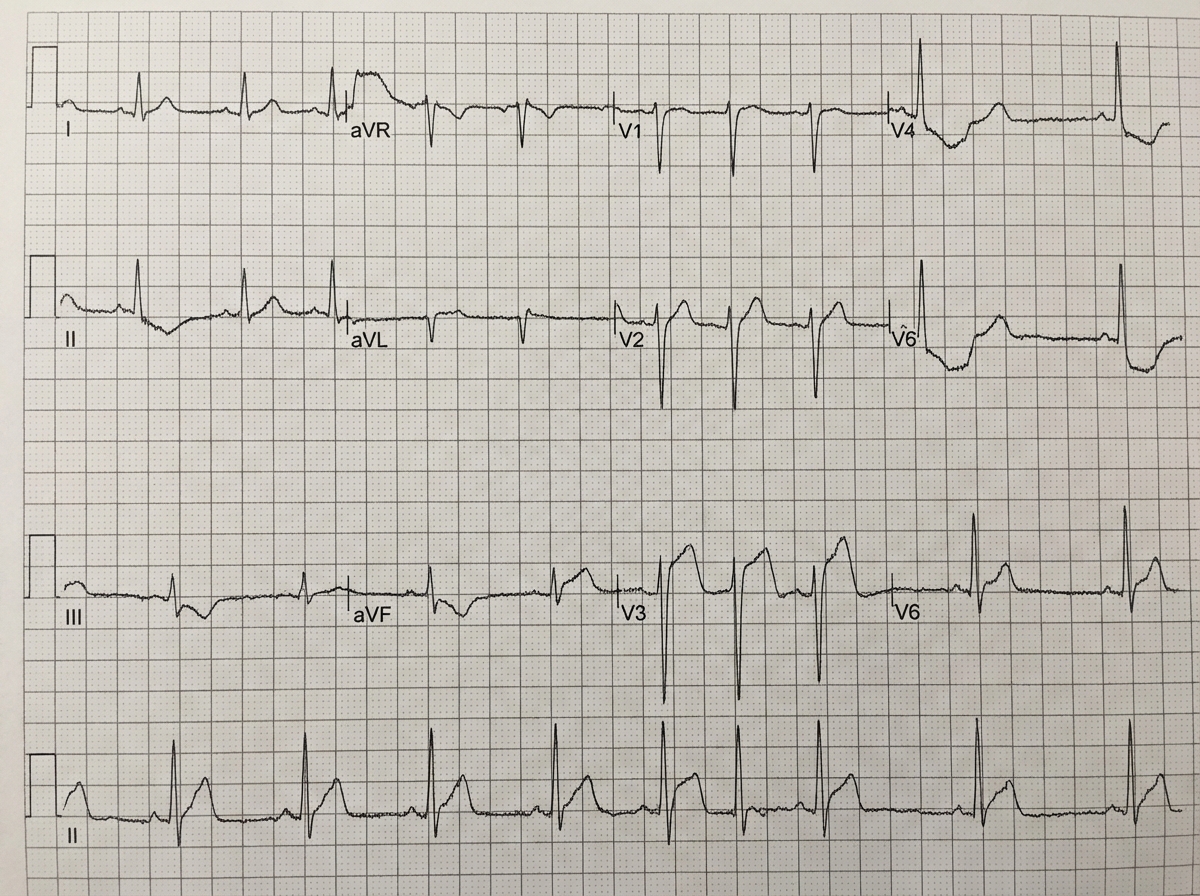
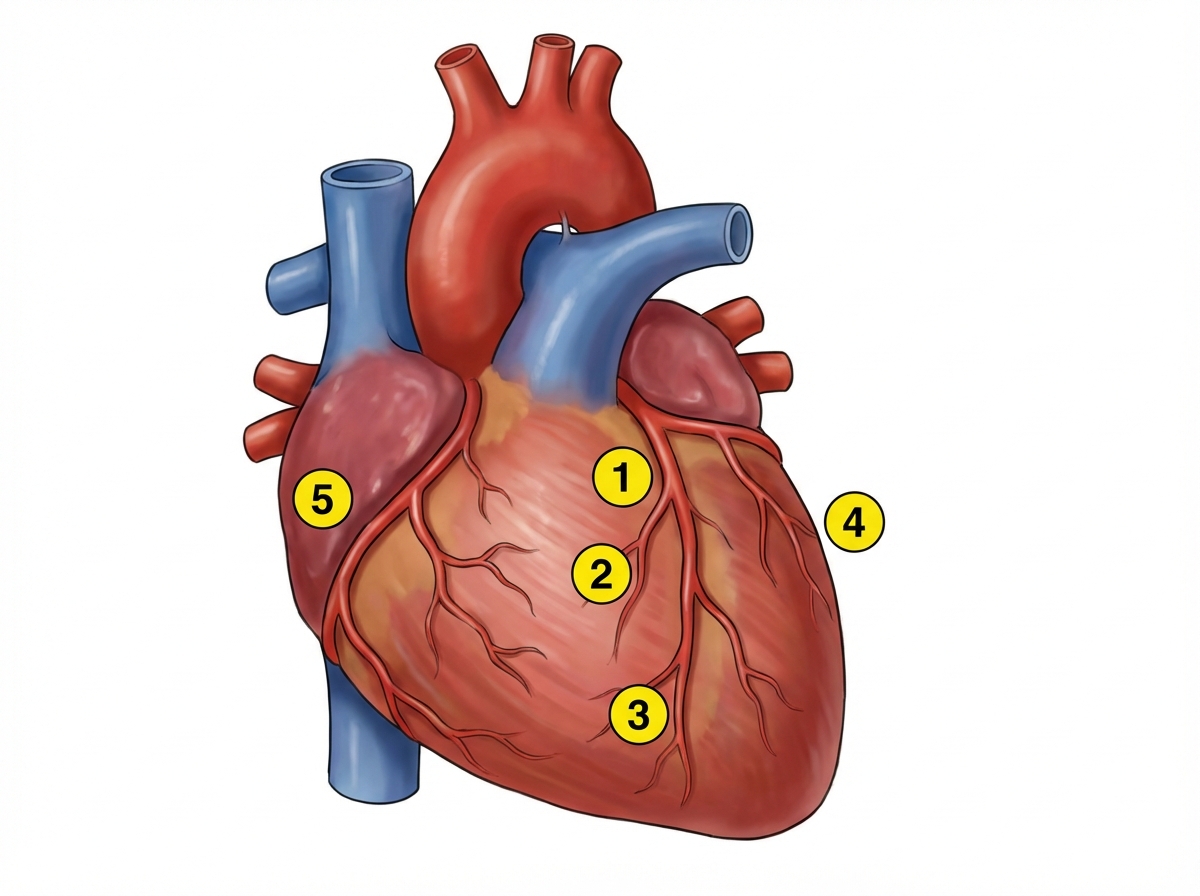
ECG of a patient had ST segment elevation in V1-V6, lead I and AVL. Which of the following branches is involved?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
