Cardiology — MCQs

On this page
A 48-year-old man presents to the ER with a sudden-onset, severe headache. He is vomiting and appears confused. His wife, who accompanied him, says that he has not had any trauma, and that the patient has no relevant family history. He undergoes a non-contrast head CT that shows blood between the arachnoid and pia mater. What is the most likely complication from this condition?
A 57-year-old construction worker presents with gradually worsening shortness of breath for the past several months and left pleuritic chest pain for 2 weeks. He denies fever, cough, night sweats, wheezing, or smoking. He is recently diagnosed with hypertension and started amlodipine 10 days ago. He has been working in construction for the last 25 years and before that, he worked at a ship dry-dock for 15 years. Physical exam reveals bilateral crackles at the lung bases. Chest X-ray reveals bilateral infiltrates at the lung bases. Pulmonary function tests show a slightly increased FEV1/FVC ratio, but total lung volume is decreased. CT scan shows pleural scarring. What of the following conditions is the most likely explanation in this case?
A 17-year-old boy comes to the physician for a follow-up visit. Two days ago, he had a routine health maintenance examination that showed 3+ proteinuria on urine dipstick testing. During the initial routine examination, the patient reported feeling well, apart from being exhausted from his day at work. He had an upper respiratory infection 1 month ago, which resolved spontaneously within 5 days of onset. He has no history of serious illness. He works as an intern at a shooting range, where he does not usually use appropriate hearing protection. Today, he appears tired and complains about the early morning doctor's appointment. He is 170 cm (5 ft 7 in) tall and weighs 81.5 kg (180 lb); BMI is 28 kg/m2. His temperature is 37°C (98.6°F), pulse is 72/min, and blood pressure is 118/70 mm Hg. Examination shows facial acne. There is mild sensorineural hearing loss bilaterally. The remainder of the examination shows no abnormalities. Laboratory studies show: Serum Urea 8 mg/dL Creatinine 1.0 mg/dL Urine Glucose negative Protein 1+ Blood negative Nitrite negative Leukocytes negative pH 6.0 Specific gravity 1.005 Which of the following is the most likely explanation for this patient's findings?
A 71-year-old woman presents with a transient episode of right arm and hand weakness that resolved in approximately one hour. Her symptoms started while she was gardening. Her past medical history is notable for hypertension, diabetes, anxiety, and dyslipidemia. Her current medications include insulin, metformin, and fluoxetine. Examination reveals a left carotid bruit. Ultrasound duplex of her carotid arteries demonstrates right and left carotid stenosis of 35% and 50%, respectively. Which of the following is the best next step in management?
A 65-year-old woman comes to the emergency department because of blurry vision for 10 hours. She has also had urinary urgency and discomfort while urinating for the past 4 days. She has been feeling increasingly weak and nauseous since yesterday. She has a history of type 2 diabetes mellitus and arterial hypertension. One year ago she was treated for an infection of her eyes. She drinks 2–3 glasses of wine weekly. Current medications include captopril, metoprolol, metformin, and insulin. Her temperature is 37.5°C (99.5°F), pulse is 107/min, and blood pressure is 95/70 mm Hg. Visual acuity is decreased in both eyes. The pupils are equal and reactive to light. The corneal reflexes are brisk. The mucous membranes of the mouth are dry. The abdomen is soft and not distended. Cardiopulmonary examination shows no abnormalities. Which of the following is the most likely diagnosis?
A 56-year-old woman comes to the physician for follow-up after a measurement of elevated blood pressure at her last visit three months ago. She works as a high school teacher at a local school. She says that she mostly eats cafeteria food and take-out. She denies any regular physical activity. She does not smoke or use any recreational drugs. She drinks 2 to 3 glasses of wine per day. She has hypercholesterolemia for which she takes atorvastatin. Her height is 165 cm (5 ft 5 in), weight is 82 kg (181 lb), and BMI is 30.1 kg/m2. Her pulse is 67/min, respirations are 18/min, and blood pressure is 152/87 mm Hg on the right arm and 155/92 mm Hg on the left arm. She would like to try lifestyle modifications to improve her blood pressure before considering pharmacologic therapy. Which of the following lifestyle modifications is most likely to result in the greatest reduction of this patient's systolic blood pressure?
A 7-year-old boy is brought to the physician for a follow-up examination after the removal of a tooth. During the procedure, he had prolonged bleeding that did not resolve with pressure and gauze packing and eventually required suture placement. His older brother had a similar episode a year ago, but his parents and two sisters have never had problems with prolonged bleeding. Physical examination shows no abnormalities. Genetic analysis confirms an X-linked recessive disorder. Which of the following is most likely deficient in this patient?
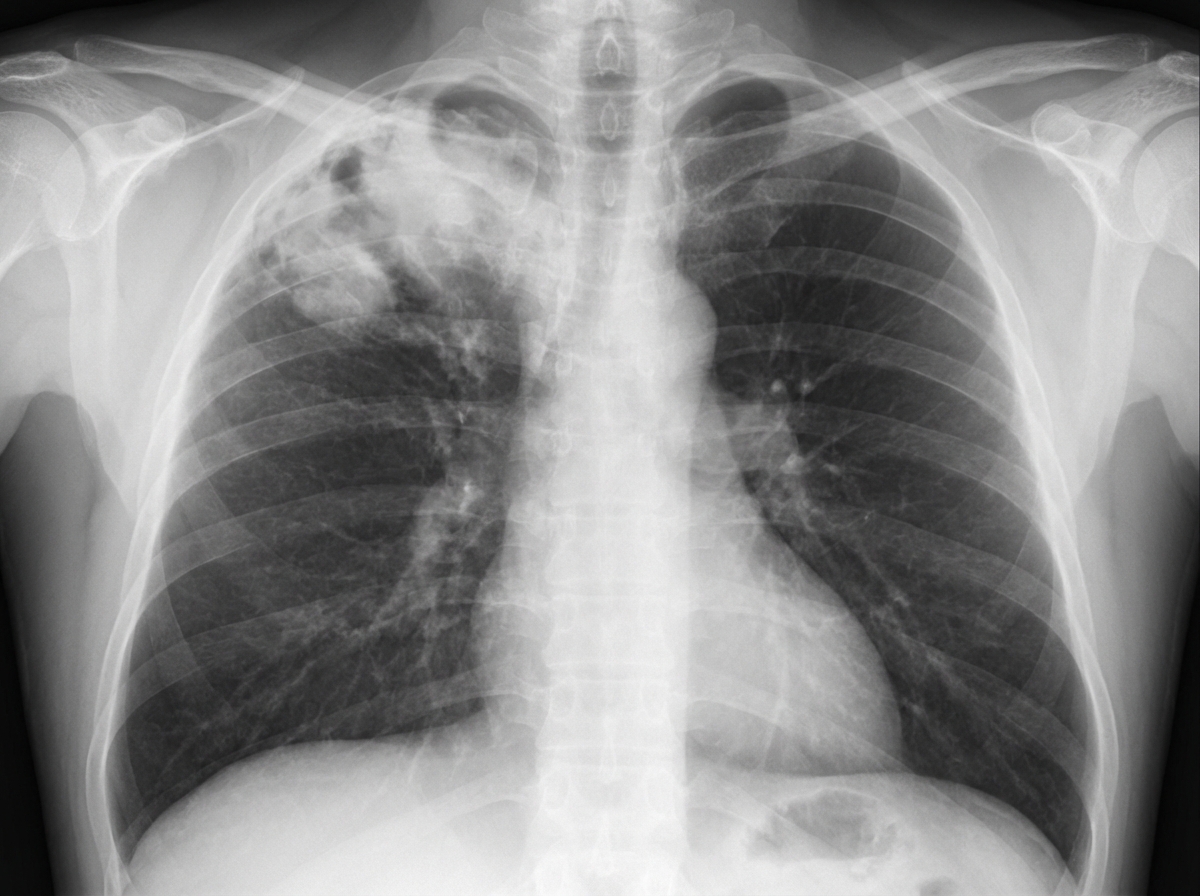
A 68-year-old male is diagnosed with squamous cell carcinoma in the upper lobe of his right lung. A chest radiograph can be seen in image A. Which of the following would you most expect to find in this patient?
A 48-year-old female suffers a traumatic brain injury while skiing in a remote area. Upon her arrival to the ER, she is severely hypoxemic and not responsive to O2 therapy. She is started on a mechanical ventilator and 2 days later upon auscultation, you note late inspiratory crackles. Which of the following is most likely normal in this patient?
A 60-year-old man comes to the physician because of recurrent nose bleeds that occur with light trauma or at random times during the day. Over the past 6 months, the patient has felt weak and fatigued and has had a 10-kg (22-lb) weight loss. He has poor appetite and describes abdominal discomfort. He does not have night sweats. His pulse is 72/min, blood pressure is 130/70 mm Hg, and his temperature is 37.5°C (99.5°F). The spleen is palpated 10 cm below the left costal margin. Multiple bruises are noted on both upper extremities. Laboratory studies show. Hemoglobin 9.8 g/dL Hematocrit 29.9% Leukocyte count 4,500/mm3 Neutrophils 30% Platelet count 74,000/mm3 Serum Lactate dehydrogenase 410 IU/L A peripheral blood smear detects tartrate-resistant acid phosphatase activity. Which of the following is the most appropriate initial treatment for this patient?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
