Cardiology — MCQs

On this page
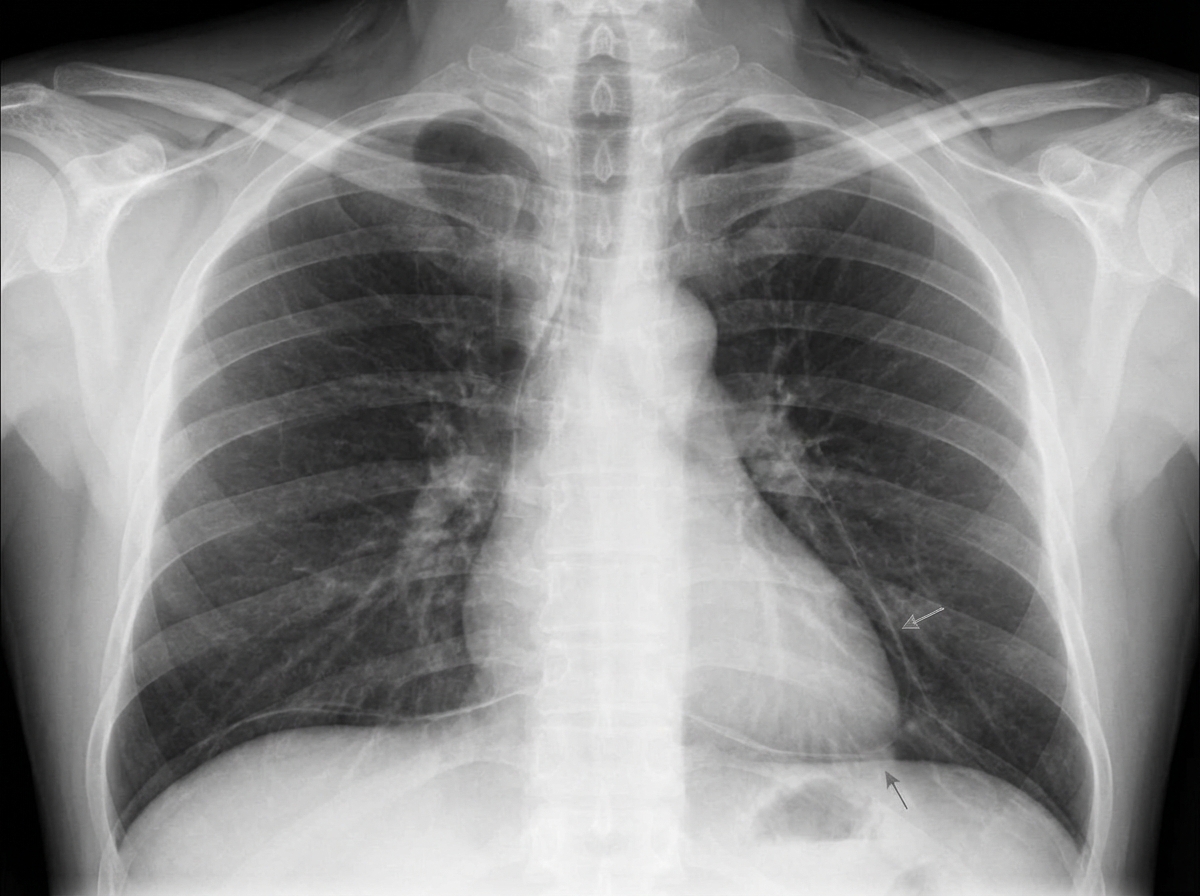
A 17-year-old boy presents to the emergency department for the evaluation of severe chest pain that started one hour ago. The pain suddenly began after he lifted a heavy object and the pain is constant. He has no history of a serious illness and takes no medications. His blood pressure is 125/85 mm Hg, the pulse is 89/min, the respiratory rate is 15/min, and the temperature is 36.7°C (98.1°F). Examination of the supraclavicular notch shows mild swelling of the skin with crepitation on palpation. Auscultation of the precordium in the left lateral decubitus position reveals a clicking sound with every heartbeat. The remainder of the physical examination shows no abnormalities. A chest X-ray is shown. Which of the following is the most appropriate next step in management?
A 52-year-old man with a history of Type 1 diabetes mellitus presents to the emergency room with increasing fatigue. Two days ago, he ran out of insulin and has not had time to obtain a new prescription. He denies fevers or chills. His temperature is 37.2 degrees Celsius, blood pressure 84/56 mmHg, heart rate 100/min, respiratory rate 20/min, and SpO2 97% on room air. His physical exam is otherwise within normal limits. An arterial blood gas analysis shows the following: pH 7.25, PCO2 29, PO2 95, HCO3- 15. Which of the following acid-base disorders is present?
A 71-year-old woman comes to the physician because of sudden loss of vision in her right eye for 15 minutes that morning, which subsided spontaneously. Over the past 4 months, she has had fatigue, a 4-kg (8.8-lb) weight loss, and has woken up on several occasions at night covered in sweat. She has had frequent headaches and pain in her jaw while chewing for the past 2 months. She does not smoke or drink alcohol. Her temperature is 37.5°C (99.5°F), pulse is 88/min, and blood pressure is 118/78 mm Hg. Examination shows a visual acuity of 20/25 in the left eye and 20/30 in the right eye. The pupils are equal and reactive. There is no swelling of the optic discs. Her hemoglobin concentration is 10.5 g/dL, platelet count is 420,000/mm3, and erythrocyte sedimentation rate is 69 mm/h. The patient's condition puts her at the greatest risk of developing which of the following complications?
A 39-year-old female presents with confusion. Her husband reports that she doesn't know where she is and cannot remember the date. She was recently diagnosed with small cell lung cancer. Vital signs are T 37C, HR 80, BP 120/80 mmHg, RR 14, and O2 sat 99% on room air. She is not orthostatic. Physical examination reveals moist mucous membranes and normal capillary refill. A basic metabolic profile reveals that serum sodium is 129. Regarding this patient's illness, which of the following is true?
A 70-year-old caucasian woman presents to her primary care provider complaining of a heavy cough with blood-tinged sputum. Her cough has bothered her for the last 2 weeks. Over the counter medications are no longer alleviating her symptoms. She also reports that she has unintentionally lost 6.8 kg (15 lb) in the last 5 months. Her past medical history is significant for peptic ulcer disease that was positive for H. pylori on biopsy and was treated with triple-drug therapy. She is a lifetime non-smoker and worked as a teacher before retiring at the age of 60. Today, her temperature is 36.9°C (98.4°F), blood pressure is 128/82 mm Hg, pulse is 87/min, and pulse oximetry is 90% on room air. On physical exam, her heart has a regular rate and rhythm. Auscultation of the lungs revealed scattered crackles and wheezes. A CT scan of the lungs shows an irregular mass in the peripheral region of the inferior lobe of the right lung and a CT guided biopsy is positive for malignant tissue architecture and gland formation with a significant amount of mucus. Which of the following risk factors most likely predisposed this patient to her condition?
A 23-year-old man comes to the physician because of lightening of his skin on both hands, under his eyes, and on his neck for 2 years. During this period the lesions slowly grew in size. There is no itchiness or pain. He regularly visits his family in India. Vital signs are within normal limits. Examination shows sharply demarcated, depigmented skin patches on the dorsum of both hands, in the periocular region, and on the neck. Sensation of the skin is intact. The lesions fluorescence blue-white under Wood's lamp. Which of the following findings is most likely to be associated with this patient's diagnosis?
A 50-year-old man comes to the physician because of diffuse weakness for the past several months. There is an anterior mediastinal mass on a lateral x-ray of the chest that was performed as part of a pre-employment medical evaluation. He has gastroesophageal reflux disease. His only medication is rabeprazole. He is 178 cm (5 ft 10 in) tall and weighs 77 kg (170 lb); BMI is 24.3 kg/m2. Vital signs are within normal limits. There is no cervical or axillary lymphadenopathy. Cardiopulmonary examination shows no abnormalities. The abdomen is soft and nontender; there is no splenomegaly. Further evaluation of this patient is most likely to show which of the following?
A 52-year-old Caucasian man with hypertension comes to the physician because of frequent urination and increased thirst. He drinks 4 oz of alcohol daily and has smoked 1 pack of cigarettes daily for the past 30 years. He is 180 cm (5 ft 10 in) tall and weighs 106 kg (233 lb); BMI is 33 kg/m2. His blood pressure is 130/80 mm Hg. Laboratory studies show a hemoglobin A1c of 8.5%. Which of the following is the most likely predisposing factor for this patient's condition?
An 80-year-old man presents to the emergency department because of gnawing substernal chest pain that started an hour ago and radiates to his neck and left jaw. A 12-lead ECG is obtained and shows ST-segment elevation with newly developing Q waves. He is admitted for treatment. 4 days after hospitalization he suddenly develops altered mental status, and his blood pressure falls from 115/75 mm Hg to 80/40 mm Hg. Physical examination shows jugular venous distention, pulsus paradoxus, and distant heart sounds. What is the most likely cause of this patient's condition?
A 61-year-old woman comes to the physician because of a 1-week history of dizziness, nausea, vomiting, and repeated falls. Neurologic examination shows past-pointing on a finger-nose test. She has a broad-based gait. Ophthalmologic exam shows rhythmic leftward movement of the globes. A serum antibody assay is positive for anti-Yo antibodies directed at proteins expressed by Purkinje cells. This patient's condition is most likely associated with which of the following tumors?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
