Cardiology — MCQs

On this page
A 27-year-old woman presents to her primary care physician with a chief complaint of pain in her hands, shoulders, and knees. She states that the pain has lasted for several months but seems to have worsened recently. Any activity such as opening jars, walking, or brushing her teeth is painful. The patient has a past medical history of a suicide attempt in college, constipation, anxiety, depression, and a sunburn associated with surfing which was treated with aloe vera gel. Her temperature is 99.5°F (37.5°C), blood pressure is 137/78 mmHg, pulse is 92/min, respirations are 14/min, and oxygen saturation is 98% on room air. Laboratory values are obtained and shown below. Hemoglobin: 9 g/dL Hematocrit: 33% Leukocyte count: 2,500/mm^3 with normal differential Platelet count: 107,000/mm^3 Serum: Na+: 139 mEq/L Cl-: 102 mEq/L K+: 4.4 mEq/L HCO3-: 24 mEq/L BUN: 21 mg/dL Glucose: 90 mg/dL Creatinine: 1.0 mg/dL Ca2+: 10.2 mg/dL AST: 12 U/L ALT: 10 U/L Which of the following is the most likely to be found in this patient?
A previously healthy 46-year-old man comes to the physician for an 8-month history of headache that is more severe in the mornings. His blood pressure is 151/92 mm Hg. Examination shows enlargement of the nose, forehead, and jaw as well as the hands, fingers, and feet. Ophthalmologic examination shows impaired vision in the outer peripheral fields of both eyes. Laboratory studies show a serum glucose concentration of 225 mg/dL. Which of the following findings is most likely to confirm the diagnosis?
A 51-year-old woman comes to the physician because of swelling of her legs for 4 months. She first noticed the changes on the left leg, followed by the right leg. Sometimes her legs are itchy. She has a 1-month history of hoarseness. She returned from a trip to Mexico 8 months ago. She has a history of hypertension, constipation, and coronary artery disease. She works as a teacher at a primary school. Her mother had type-2 diabetes mellitus. She smoked one-half pack of cigarettes daily for 6 years but stopped smoking 11 years ago. She drinks one glass of wine daily and occasionally more on the weekend. Current medications include aspirin, bisoprolol, and atorvastatin. She is 165 cm (5 ft 5 in) tall and weighs 82 kg (181 lb); BMI is 30.1 kg/m2. Vital signs are within normal limits. Examination shows bilateral pretibial non-pitting edema. The skin is indurated, cool, and dry. Peripheral pulses are palpated bilaterally. The remainder of the examination shows no abnormalities. The patient is at increased risk for which of the following conditions?
A 35-year-old African American woman comes to the physician because of intermittent palpitations over the past 2 weeks. During this period she has also had constipation and has felt more tired than usual. She was diagnosed with hypertension 4 weeks ago and treatment with chlorthalidone was begun. Her temperature is 36.5°C (97.7°F), pulse is 75/min, and blood pressure is 158/97 mm Hg. Physical examination shows a soft and nontender abdomen. There is mild weakness of the upper and lower extremities. Deep tendon reflexes are 1+ bilaterally. Laboratory studies show: Hemoglobin 13.5 g/dL Leukocyte count 5,000/mm3 Serum Na+ 146 mEq/L Cl− 100 mEq/L K+ 2.8 mEq/L HCO3− 30 mEq/L Glucose 97 mg/dL Urea nitrogen 10 mg/dL Creatinine 0.8 mg/dL Test of the stool for occult blood is negative. An ECG shows premature atrial complexes. Chlorthalidone is discontinued and oral potassium chloride therapy is begun. One week later, the patient's plasma aldosterone concentration is 26 ng/dL (N=3.6 to 24.0 ng/dL) and plasma renin activity is 0.8 ng/mL/h (N=0.3 to 4.2 ng/mL/h). Which of the following is the most appropriate next step in management?
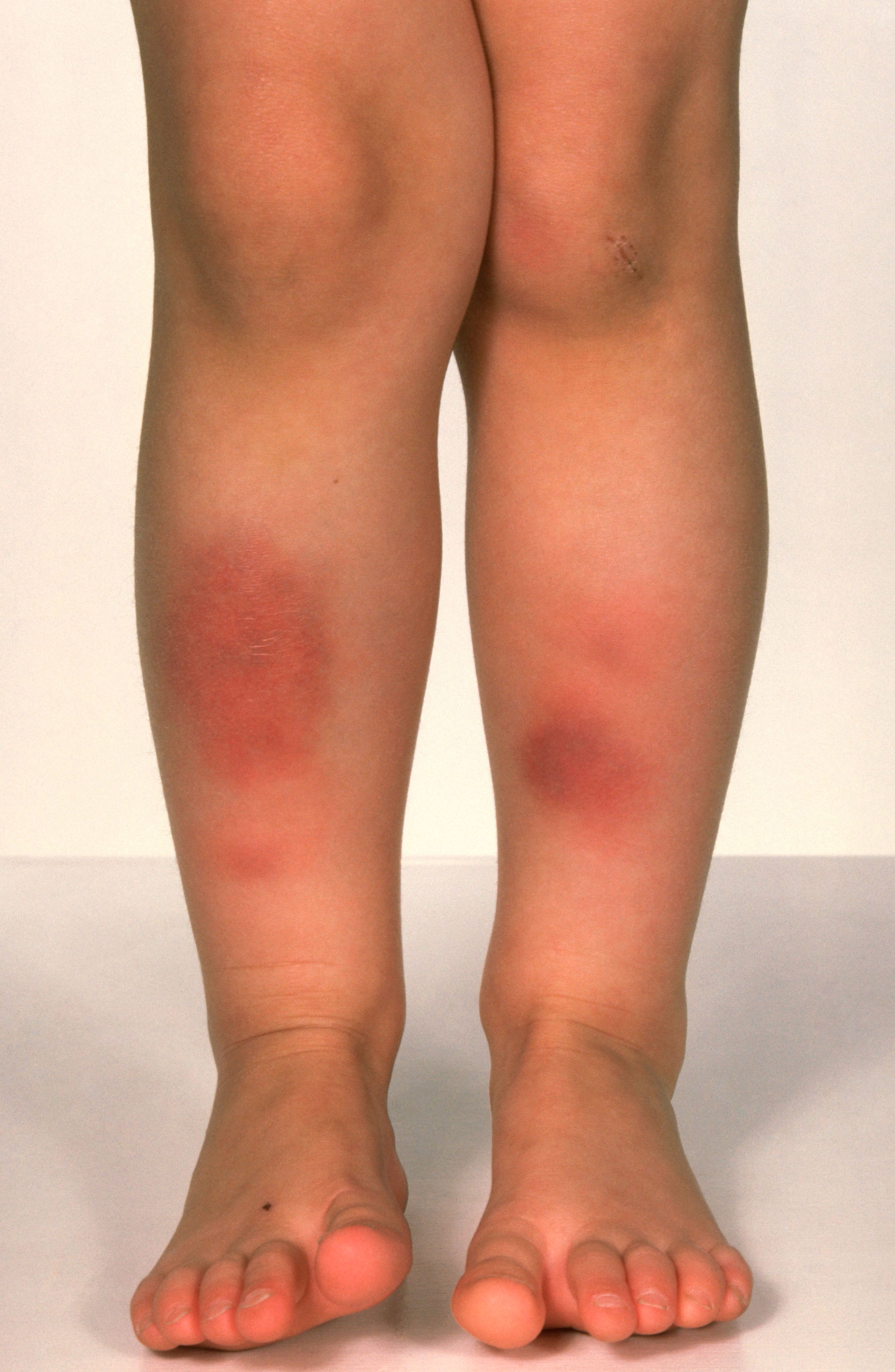
A 33-year-old African-American female presents to her physician with complaints of a persistent, dry cough. She states that the cough has gone on for some time now. Three weeks ago, during her last general checkup, she was started on lisinopril and metformin for concerns regarding an elevated blood pressure and fasting blood glucose. Past medical history is notable for eczema, asthma, and seasonal allergies. At this visit the patient has other non-specific complaints such as fatigue and joint pain as well as a burning sensation in her sternum when she eats large meals. Her physical exam is only notable for painful bumps on her lower extremities (figure A) which the patient attributes to "bumping her shins," during exercise, and an obese habitus. Which of the following is most likely true for this patient's chief concern?
A 50-year-old woman comes to the physician for a follow-up examination. Two weeks ago she was seen for adjustment of her antihypertensive regimen and prescribed lisinopril because of persistently high blood pressure readings. A complete blood count and renal function checked at her last visit were within the normal limits. On questioning, she has had fatigue and frequent headaches over the last month. She has hypertension, type 2 diabetes mellitus, polycystic ovarian disease, and hyperlipidemia. Her mother has hyperthyroidism and hypertension. Current medications include amlodipine and hydrochlorothiazide at maximum doses, lisinopril, metformin, glimepiride, and atorvastatin. She has never smoked and drinks 1–2 glasses of wine with dinner every night. She is 167 cm (5 ft 5 inches) and weighs 81.6 kg (180 lbs); BMI is 30 kg/m2. Her blood pressure is 170/110 mm Hg in both arms, heart rate is 90/min, and respirations are 12/min. Examination shows an obese patient and no other abnormalities. Laboratory studies show: Hemoglobin 14 g/dL Leukocyte count 7,800/mm3 Serum Na+ 139 mEq/L K+ 3.4 mEq/L Cl- 100 mEq/L Creatinine 2.1 mg/dL Urea nitrogen 29 mg/dL TSH 3 μU/mL Urine Blood negative Protein negative Glucose 1+ Which of the following is the most likely diagnosis?
A 35-year-old woman comes to the physician because of a 2-month history of progressive fatigue and intermittent abdominal pain. During this time, she has noticed that her urine is darker when she wakes up in the morning. Her stool is of normal color. Five months ago, she was diagnosed with type 2 diabetes mellitus, for which she takes metformin. Physical examination shows pallor and jaundice. There is no splenomegaly. Laboratory studies show: Hemoglobin 7.5 g/dL WBC count 3,500/mm3 Platelet count 100,000/mm3 Serum Creatinine 1.0 mg/dL Total bilirubin 6.0 mg/dL Direct bilirubin 0.2 mg/dl Lactate dehydrogenase 660 U/L Haptoglobin 18 mg/dL (N=41–165 mg/dL) Her urine is red, but urinalysis shows no RBCs. A Coombs test is negative. Peripheral blood smear shows no abnormalities. This patient is at greatest risk for which of the following complications?
A 50-year-old female presents with a holosystolic murmur heard best over the apex, radiating to the axilla. She has no signs of pulmonary hypertension or edema. What best explains her lack of symptoms?
A 68-year-old man presents to his primary care provider after noticing that his urine has been pink for the last week. He does not have any pain with urination, nor has he had any associated fevers or infections. On his review of systems, the patient notes that he thinks he has lost some weight since his belt is looser, and he has also had occasional dull pressure in his back for the past two months. His temperature is 98.8°F (37.1°C), blood pressure is 132/90 mmHg, pulse is 64/min, and respirations are 12/min. The patient weighs 210 lbs (95.3 kg, BMI 31.9 kg/m²), compared to his weight of 228 lbs (103.4 kg, BMI 34.7 kg/m²) at his last visit 2 years prior. On exam, the patient does not have any back or costovertebral angle tenderness. On abdominal palpation, a firm mass can be appreciated deep in the left abdomen. Given the suspected diagnosis, the clinical workup should also assess for which of the following paraneoplastic syndromes?
A 52-year-old male presents to clinic with complaints of anxiety and fatigue for 4 months. He has also been experiencing palpitations, muscle weakness, increased sweating, and an increase in the frequency of defecation. Past medical history is insignificant. He neither consumes alcohol nor smokes cigarettes. His pulse is 104/min and irregular, blood pressure is 140/80 mm Hg. On examination, you notice that he has bilateral exophthalmos. There are fine tremors in both hands. Which of the following results would you expect to see on a thyroid panel?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
