Cardiology — MCQs

On this page
A 54-year-old man comes to the physician for an annual health maintenance examination. He reports that he feels well. He has smoked one pack of cigarettes daily for 22 years and drinks three 12-oz bottles of beer each night. He works as an accountant and says he does not have time to exercise regularly. He is 178 cm (5 ft 10 in) tall and weighs 98 kg (216 lb); BMI is 31 kg/m2. His blood pressure is 146/90 mm Hg. Physical examination shows no abnormalities. His serum cholesterol concentration is 232 mg/dL and hemoglobin A1C is 6.9%. Which of the following preventative measures is likely to have the greatest impact on this patient's all-cause mortality risk?
A 76-year-old woman comes to the physician because of increasing muscle pain and stiffness, weakness of her shoulders and legs, and generalized fatigue for the past 4 months. She has been having great difficulty getting out of bed in the morning. On two occasions her son had to come over and help her stand up. She has had a 4-kg (9-lb) weight loss and has not been sleeping well during this period. She has had multiple episodes of left-sided headaches and pain in her jaw while chewing over the past 2 months. She had a fall and hit her head on the staircase banister 3 months ago. Her temperature is 38°C (100.4°F), pulse is 101/min, and blood pressure is 128/88 mm Hg. Examination shows conjunctival pallor. Range of motion of the shoulder and hip is mildly limited by pain. Muscle strength in bilateral upper and lower extremities is normal. Deep tendon reflexes are 2+ bilaterally. On mental status examination, she admits her mood 'is not that great'. Her erythrocyte sedimentation rate is 59 mm/h and serum creatine kinase is 38 mg/dL. Which of the following is the most likely cause of this patient's headache?
A 14-year-old boy is brought to the physician because of fever, malaise, and severe right knee joint pain and swelling for 3 days. He had also had episodes of abdominal pain and epistaxis during this period. Five days ago, he had swelling and pain in his left ankle joint which has since resolved. He reports having a sore throat 3 weeks ago while he was camping in the woods, for which he received symptomatic treatment. His immunizations are up-to-date. His temperature is 38.7°C (101.6°F), pulse is 119/min, and blood pressure is 90/60 mm Hg. Examination shows a swollen, tender right knee; range of motion is limited. There are painless 3- to 4-mm nodules over the elbow. Cardiopulmonary examination is normal. His hemoglobin concentration is 12.3 g/dL, leukocyte count is 11,800/mm3, and erythrocyte sedimentation rate is 58 mm/h. Arthrocentesis of the right knee joint yields clear, straw-colored fluid; no organisms are identified on Gram stain. Analysis of the synovial fluid shows a leukocyte count of 1,350/mm3 with 17% neutrophils. Which of the following is the most likely diagnosis?
A 62-year-old woman comes to the physician in June for a routine check-up. She has chronic back pain and underwent an appendectomy at the age of 27. She is married and has two kids. The patient recently got back from a cruise to Mexico where she celebrated her 40th wedding anniversary. Her last mammogram was 6 months ago and showed no abnormalities. Her last Pap smear was 2 years ago and unremarkable. A colonoscopy 5 years ago was normal. Her mother died of breast cancer last year and her father has arterial hypertension. Her immunization records show that she has never received a pneumococcal or a shingles vaccine, her last tetanus booster was 6 years ago, and her last influenza vaccine was 2 years ago. She drinks 1– 2 alcoholic beverages every weekend. She takes a multivitamin daily and uses topical steroids. She regularly attends water aerobic classes and physical therapy for her back pain. She is 168 cm (5 ft 6 in) tall and weighs 72 kg (160 lb); BMI is 26 kg/m2. Her temperature is 36.7°C (98°F), pulse is 84/min, and blood pressure is 124/70 mm Hg. Which of the following is the most appropriate recommendation at this time?
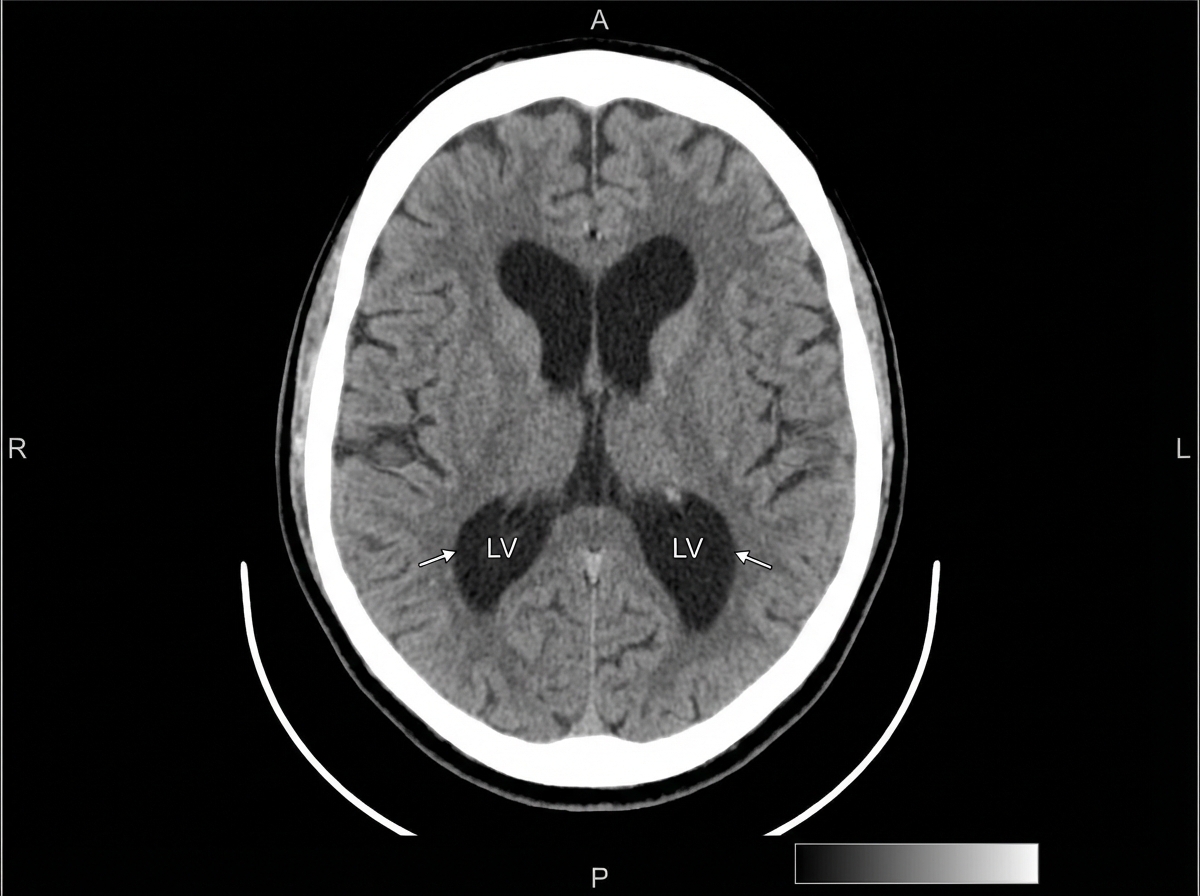
A 68-year-old woman in a wheelchair presents with her husband. She has a 12-month history of progressive difficulty in walking and maintaining balance. Her husband reports that she walks slowly, has difficulty turning, and her feet seem ‘glued to the ground’. She also has problems recalling names and details of recent events. She has no tremors, delusions, hallucinations, sleep disturbances, or head trauma. Past medical history is significant for essential hypertension treated with losartan and urinary incontinence, for which she takes oxybutynin. On physical examination, her vital signs include: temperature 37.0°C (98.6°F), blood pressure 130/70 mm Hg, and pulse 80/min. On neurologic examination, her gait is slow, with short steps and poor foot clearance. A head CT is shown. The patient undergoes a lumbar puncture to remove 50 ml of cerebrospinal fluid, which transiently improves her gait for the next 3 days. What is the next step in the management of this patient?
An 83-year-old woman with a past medical history of poorly controlled diabetes, hyperlipidemia, hypertension, obesity, and recurrent urinary tract infections is brought to the emergency room by her husband due to confusion, generalized malaise and weakness, nausea, and mild lower abdominal pain. Her medications include metformin and glyburide, atorvastatin, lisinopril, and hydrochlorothiazide. At presentation, her oral temperature is 38.9°C (102.2°F), the pulse is 122/min, blood pressure is 93/40 mm Hg, and oxygen saturation is 96% on room air. On physical examination, she is breathing rapid shallow breaths but does not have any rales or crackles on pulmonary auscultation. No murmurs are heard on cardiac auscultation and femoral pulses are bounding. Her skin is warm, flushed, and dry to touch. There is trace bilateral pedal edema present. Her abdomen is soft and non-distended, but she has some involuntary guarding on palpation of the suprapubic region. ECG shows normal amplitude sinus tachycardia without evidence of ST-segment changes or T-wave inversions. Which of the following would most likely be the relative pulmonary artery catheterization measurements of pulmonary capillary wedge pressure (PCWP), mixed venous oxygen saturation (SvO2), calculated cardiac output (CO), and systemic vascular resistance (SVR) in this patient?
A 59-year-old patient with COPD is admitted with difficulty breathing and increased sputum production. Approx. a week ago, he developed an upper respiratory tract infection. On admission, his blood pressure is 130/80 mm Hg, the heart rate 92/min, the respiratory rate 24/min, the temperature 37.6°C (99.7°F), and SaO2 on room air 87%. Chest radiograph shows consolidation in the lower lobe of the right lung. Arterial blood gases (ABG) are taken and antibiotics are started. A nasal cannula provides 2L of oxygen to the patient. When the ABG results arrive, the patient’s SaO2 is 93%. The results are as follows: pH 7.32 PaO2 63 mm Hg PaCO2 57 mm Hg HCO3- 24 mEq/L What is the most appropriate next step in the management of this patient?
A 72-year-old man comes to the physician for a routine physical examination. He says that he has felt well except for occasional headaches. He has no history of major medical illness. His temperature is 37°C (98.6°F), pulse is 80/min, and blood pressure is 155/90 mm Hg. An ultrasound of the kidneys shows a normal right kidney and a left kidney that is 2 cm smaller in length. Further evaluation is most likely to show which of the following?
A 61-year-old man presents to the office with a past medical history of hypertension, diabetes mellitus type II, hypercholesterolemia, and asthma. Recently, he describes increasing difficulty with breathing, particularly when performing manual labor. He also endorses a new cough, which occurs both indoors and out. He denies any recent tobacco use, despite a 40-pack-year history. He mentions that his symptoms are particularly stressful for him since he has been working in the construction industry for the past 30 years. The vital signs include: temperature 36.7°C (98.0°F), blood pressure 126/74 mm Hg, heart rate 74/min, and respiratory rate 14/min. On physical examination you notice clubbing of his digits, wheezing on auscultation, and normal heart sounds. A chest radiograph demonstrates linear opacities at the bilateral lung bases and multiple calcified pleural plaques. What is his most likely diagnosis?
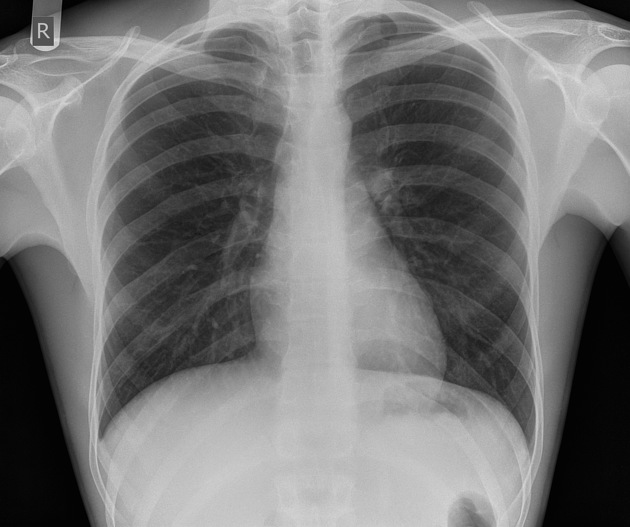
A 56-year-old man presents to his family physician for a routine check-up but also states he has been feeling less energetic than usual. He mentions that he has recently been promoted to a nurse manager position at a regional medical center. His medical history is significant for hypertension and hyperlipidemia, for which he takes enalapril and atorvastatin. The patient has smoked 1 pack of cigarettes daily for the last 30 years. His vital signs include the following: the heart rate is 80/min, the respiratory rate is 18/min, the temperature is 37.1°C (98.8°F), and the blood pressure is 140/84 mm Hg. He appears well-nourished, alert, and interactive. Coarse breath sounds are auscultated in the lung bases bilaterally. A low-dose computerized tomography (CT) scan is scheduled. A tuberculin skin injection is administered and read 2 days later; the induration has a diameter of 12 mm. A Ziehl-Neelsen stain of the sputum sample is negative. The chest radiograph is pictured. Which of the following is recommended at this time?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
