Cardiology — MCQs

On this page
A 65-year-old man presents to the emergency department for a loss of vision. He was outside gardening when he suddenly lost vision in his right eye. He then immediately called emergency medical services, but by the time they arrived, the episode had resolved. Currently, he states that he feels fine. The patient has a past medical history of diabetes and hypertension. His current medications include lisinopril, atorvastatin, metformin, and insulin. His temperature is 99.5°F (37.5°C), blood pressure is 140/95 mmHg, pulse is 90/min, respirations are 12/min, and oxygen saturation is 98% on room air. Cardiac exam is notable for a systolic murmur along the right sternal border that radiates to the carotids. Pulmonary exam reveals mild bibasilar crackles. Neurological exam reveals cranial nerves II-XII as grossly intact with 5/5 strength and normal sensation in the upper and lower extremities. The patient has a negative Romberg's maneuver, and his gait is stable. A CT scan of the head demonstrates mild cerebral atrophy but no other findings. Which of the following is the next best step in management?
A 45-year-old male presents to the hospital complaining of frequent headaches and a decreased libido. During the physical exam, the patient also states that he has recently been experiencing vision problems. The patient is suffering from what type of adenoma?
A 62-year-old man presents for evaluation of an adrenal nodule, which was accidentally discovered while performing a computerized tomography (CT) scan of the abdomen for recurrent abdominal pain. The CT was negative except for a 3 cm low-density, well-circumscribed nodule in the left adrenal gland. He reports weight gain of 12 kg (26.4 lb) over the past 3 years. He has type 2 diabetes mellitus and hypertension, which have been difficult to control with medications. Which of the following is the best initial test for this patient?
A 49-year-old man presents to a physician with the complaint of pain in the thigh after walking. He says that he is an office clerk with a sedentary lifestyle and usually drives to his office. On 2 occasions last month he had to walk to his office, which is less than a quarter of a mile from his home. On both occasions, soon after walking, he experienced pain in the right thigh which subsided spontaneously within a few minutes. His past medical history is negative for hypertension, hypercholesterolemia, or ischemic heart disease. He is a non-smoker and non-alcoholic. His father has ischemic heart disease. His physical examination is within normal limits, and the peripheral pulses are palpable in all extremities. His detailed diagnostic evaluation, including magnetic resonance angiogram (MRA) and exercise treadmill ankle-brachial index (ABI) testing, suggests a diagnosis of peripheral vascular disease due to atherosclerosis of the right iliac artery. Which of the following is the best initial treatment option?
A 50-year-old female is evaluated by her physician for recent weight gain. Physical examination is notable for truncal obesity, wasting of her distal musculature and moon facies. In addition she complains of abnormal stretch marks that surround her abdomen. The physician suspects pituitary adenoma. Which of the following high-dose dexamethasone suppression test findings and baseline ACTH findings would support his view?
A 25-year-old man presents to the emergency department with back pain. He states that it started yesterday and has been gradually getting worse. He states that the pain is worsened with moving and lifting and is relieved with rest and ibuprofen. He has a past medical history of smoking and IV drug abuse and states he last used IV drugs 2 days ago. He thinks his symptoms may be related to lifting a heavy box. His temperature is 99.3°F (37.4°C), blood pressure is 122/88 mmHg, pulse is 77/min, respirations are 14/min, and oxygen saturation is 99% on room air. Physical exam is notable for focal back pain lateral to the patient’s spine on the left. There is no midline tenderness and the rest of the patient’s exam is unremarkable. There are scars in the antecubital fossae bilaterally. Laboratory values including a C-reactive protein are unremarkable. Which of the following is the most likely diagnosis?
A 34-year-old female presents to her primary care physician complaining of fatigue. Over the last three months she has experienced decreased energy and gained 7 pounds. Review of systems is negative for symptoms of depression but is positive for constipation, myalgias, and cold intolerance. Physical exam is notable for delayed deep tendon reflex relaxation. Vital signs are as follows: T 37.1 C, HR 61, BP 132/88, RR 16, and SpO2 100%. Which of the following is the best initial screening test for this patient?
A 63-year-old woman with a previous diagnosis of rheumatoid arthritis and Sjogren syndrome was referred for a second opinion. She has had a known chronic idiopathic pericardial effusion for about a year and has dealt with intermittent chest pain ever since. She underwent 2 diagnostic pericardiocenteses, but the fluid returned each time. She also has used empiric anti-inflammatory therapies with NSAIDs and colchicine without significant changes in the size of the pericardial effusion. The etiological testing was negative. At this visit, she is still complaining of pain in her chest but has no evidence of distended neck veins. An ECG shows sinus rhythm with low QRS voltages. What will be the procedure of choice that would be both therapeutic and diagnostic?
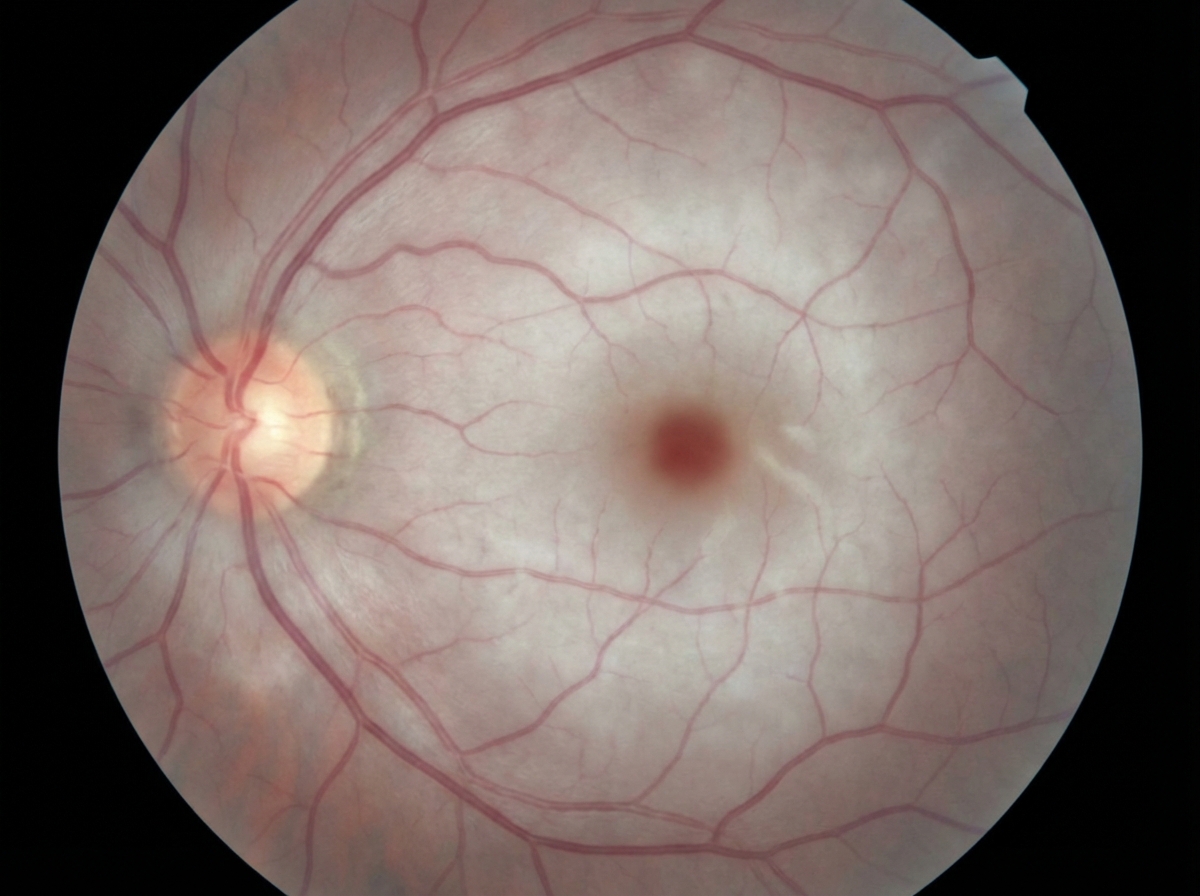
An 81-year-old man comes to the emergency department because of left-sided visual loss that started 1 hour ago. He describes initially seeing jagged edges, which was followed by abrupt, complete loss of central vision in the left eye. He has hypertension and type 2 diabetes mellitus. Blood pressure is 145/89 mm Hg. Neurologic examination shows no abnormalities. A photograph of the fundoscopic findings is shown. Which of the following tests is most likely to confirm this patient's underlying condition?
A 68-year-old woman is brought to the physician by her husband for the evaluation of confusion and memory deficits for the last month. During this period, she has also had mild weakness in her left leg. She has hypertension and hyperlipidemia. Her current medications include enalapril and atorvastatin. She has smoked two packs of cigarettes daily for the last 45 years. She drinks a glass of wine every day. Her temperature is 37°C (98.6°F), pulse is 75/min, and blood pressure is 135/85 mm Hg. She is oriented only to person. She recalls 2 out of 3 objects immediately and none after 5 minutes. The patient is unable to lift her eyebrows or to smile. Muscle strength is decreased in the left lower extremity. A T2-weighted MRI scan of the head shows several hyperintense round lesions in the frontal and temporal lobe at the border of the gray and white matter. Which of the following is the most likely diagnosis?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
