Cardiology — MCQs

On this page
A 40-year-old woman comes to the physician because of a 1-week history of fatigue, dark urine, and a feeling of heaviness in her legs. Two weeks ago, she returned from a vacation to Brazil, where she spent most of her days exploring the city of Rio de Janeiro on foot. She also gained 3 kg (7 lb) during her vacation. She has systemic lupus erythematosus. Her only medication is hydroxychloroquine. Her temperature is 37.5°C (99.5°F), pulse is 78/min, and blood pressure is 162/98 mm Hg. Physical examination shows 2+ pretibial edema bilaterally. Urinalysis shows: Blood 3+ Protein 1+ RBC 6–8/hpf with dysmorphic features RBC casts numerous WBC 8/hpf WBC casts rare Bacteria negative Which of the following is the most likely cause of this patient's leg findings?
A 32-year-old woman presents to her primary care physician for a general wellness appointment. The patient has no complaints currently and just wants to be sure that she is in good health. The patient has a past medical history of asthma, hypertension, and anxiety. Her current medications include albuterol, fluticasone, hydrochlorothiazide, lisinopril, and fexofenadine. Her temperature is 99.5°F (37.5°C), blood pressure is 165/95 mmHg, pulse is 70/min, respirations are 15/min, and oxygen saturation is 98% on room air. On exam, you note a healthy young woman with a lean habitus. Cardiac exam reveals a S1 and S2 heart sound with a normal rate. Pulmonary exam is clear to auscultation bilaterally with good air movement. Abdominal exam reveals a bruit, normoactive bowel sounds, and an audible borborygmus. Neurological exam reveals cranial nerves II-XII as grossly intact with normal strength and reflexes in the upper and lower extremities. Which of the following is the best next step in management?
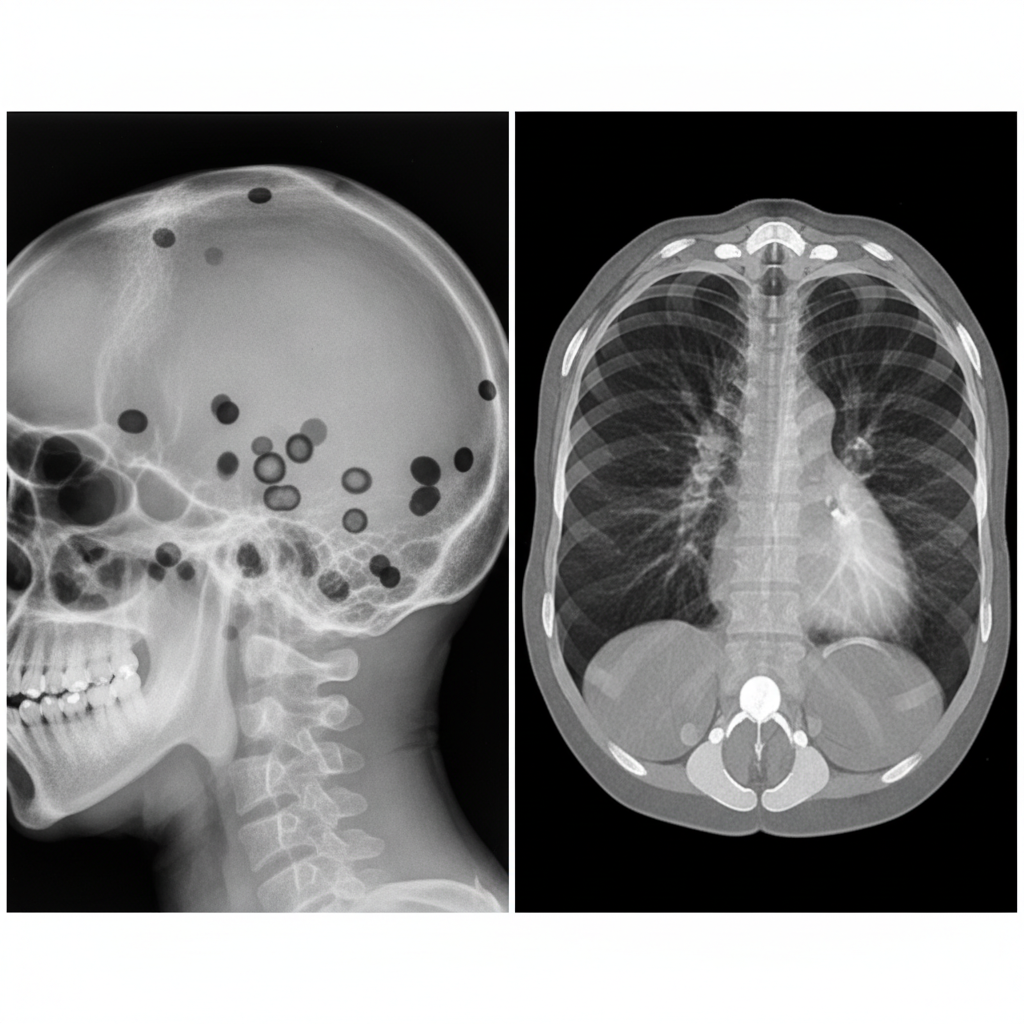
A 68-year-old woman is brought to the emergency department because of fever, productive cough, and dyspnea for 3 days. She has had upper back pain for 3 months, which is worse after activity. She takes ibuprofen for pain relief. She has no history of smoking. The temperature is 39.5°C (103.1°F), the blood pressure is 100/70 mm Hg, the pulse is 95/min, and the respirations are 22/min. Lung auscultation shows rales in the left lower lobe area. Painful lymph nodes (1 × 1 cm) are palpated in the left axillary and cervical regions. There is point tenderness along several thoracic vertebrae. Laboratory studies are pending. A skull X-ray and lung window thoracic computed tomography scan are shown. Which of the following disorders most likely played a role in this patient’s acute condition?
A 37-year-old woman presents to the emergency department complaining of generalized malaise, weakness, headache, nausea, vomiting, and diarrhea; she last felt well roughly two days ago. She is otherwise healthy, and takes no medications. Her vital signs are: T 38.0, HR 96 beats per minute, BP 110/73, and O2 sat 96% on room air. Examination reveals a somewhat ill-appearing woman; she is drowsy but arousable and has no focal neurological deficits. Initial laboratory studies are notable for hematocrit 26%, platelets of 80,000/mL, and serum creatinine of 1.5 mg/dL. Which of the following is the most appropriate treatment at this time?
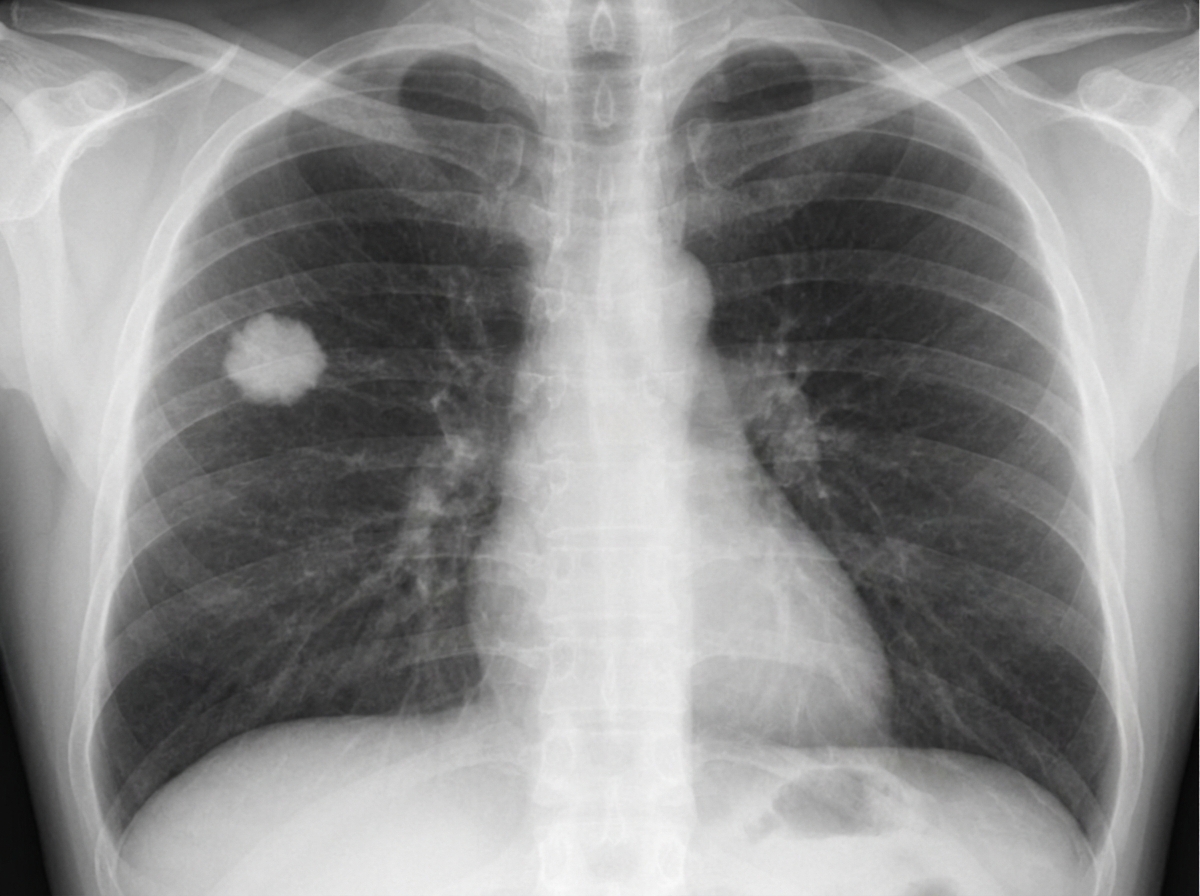
A 60-year-old man comes to the physician for an examination prior to a scheduled cholecystectomy. He has hypertension treated with hydrochlorothiazide. His mother had chronic granulomatous disease of the lung. He works in a glass manufacturing plant. He has smoked two packs of cigarettes daily for 38 years. His vital signs are within normal limits. Examination shows no abnormalities. Laboratory studies are within the reference range. An x-ray of the chest is shown. Which of the following is the most appropriate next step in management?
A 60-year-old man seeks evaluation at a medical office due to leg pain while walking. He says the pain starts in his buttocks and extends to his thighs and down to his calves. Previously, the pain resolved with rest, but the pain now persists in his feet, even during rest. His past medical history is significant for diabetes mellitus, hypertension, and cigarette smoking. The vital signs are within normal limits. The physical examination shows an atrophied leg with bilateral loss of hair. Which of the following is the most likely cause of this patient’s condition?
A 35-year-old woman comes to the physician because of a 1-month history of double vision, difficulty climbing stairs, and weakness when trying to brush her hair. She reports that these symptoms are worse after she exercises and disappear after she rests for a few hours. Physical examination shows drooping of her right upper eyelid that worsens when the patient is asked to gaze at the ceiling for 2 minutes. There is diminished motor strength in the upper extremities. The remainder of the examination shows no abnormalities. Which of the following is the most likely diagnosis?
A 53-year-old man comes to the emergency department because of severe right-sided flank pain for 3 hours. The pain is colicky, radiates towards his right groin, and he describes it as 8/10 in intensity. He has vomited once. He has no history of similar episodes in the past. Last year, he was treated with naproxen for swelling and pain of his right toe. He has a history of hypertension. He drinks one to two beers on the weekends. Current medications include amlodipine. He appears uncomfortable. His temperature is 37.1°C (99.3°F), pulse is 101/min, and blood pressure is 130/90 mm Hg. Examination shows a soft, nontender abdomen and right costovertebral angle tenderness. An upright x-ray of the abdomen shows no abnormalities. A CT scan of the abdomen and pelvis shows a 7-mm stone in the proximal ureter and grade I hydronephrosis on the right. Which of the following is most likely to be seen on urinalysis?
A 69-year-old male presents to the emergency room with back pain. He has a history of personality disorder and metastatic prostate cancer and was not a candidate for surgical resection. He began chemotherapy but discontinued due to unremitting nausea. He denies any bowel or bladder incontinence. He has never had pain like this before and is demanding morphine. The nurse administers IV morphine and he feels more comfortable. Vital signs are stable. On physical examination you note tenderness to palpation along the lower spine, weakness in the bilateral lower extremities, left greater than right. Neurological examination is also notable for hyporeflexia in the knee and ankle jerks bilaterally. You conduct a rectal examination, which reveals saddle anesthesia. Regarding this patient, what is the most likely diagnosis and the appropriate next step in management?
A 68-year-old man comes to the physician because of recurrent episodes of nausea and abdominal discomfort for the past 4 months. The discomfort is located in the upper abdomen and sometimes occurs after eating, especially after a big meal. He has tried to go for a walk after dinner to help with digestion, but his complaints have only increased. For the past 3 weeks he has also had symptoms while climbing the stairs to his apartment. He has type 2 diabetes mellitus, hypertension, and stage 2 peripheral arterial disease. He has smoked one pack of cigarettes daily for the past 45 years. He drinks one to two beers daily and occasionally more on weekends. His current medications include metformin, enalapril, and aspirin. He is 168 cm (5 ft 6 in) tall and weighs 126 kg (278 lb); BMI is 45 kg/m2. His temperature is 36.4°C (97.5°F), pulse is 78/min, and blood pressure is 148/86 mm Hg. On physical examination, the abdomen is soft and nontender with no organomegaly. Foot pulses are absent bilaterally. An ECG shows no abnormalities. Which of the following is the most appropriate next step in diagnosis?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
