Cardiology — MCQs

On this page
A 15-year-old boy is brought to the physician by his father because he has been waking up frequently during the night to urinate. Apart from occasional headaches, he has no other complaints. His family recently emigrated from Tanzania and his medical history is unknown. His father was diagnosed with sickle cell disease at the age of 5. Physical examination shows no abnormalities. Laboratory studies show: Hemoglobin 14.5 g/dL Hematocrit 44% MCV 90 fL Reticulocytes 1.5% A hemoglobin electrophoresis shows: HbA 55% HbS 43% HbF 1% This patient is at greatest risk for which of the following conditions?
A 59-year-old woman comes to the physician because of a 1-month history of episodic cough and shortness of breath. The cough is nonproductive and worsens when she climbs stairs and during the night. She has not had chest pain or palpitations. Eight weeks ago, she had fever, sore throat, and nasal congestion. She has a 10-year history of hypertension. She has smoked half a pack of cigarettes daily for 16 years. Her only medication is enalapril. Her pulse is 78/min, respirations are 18/min, and blood pressure is 145/95 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 96%. Diffuse end-expiratory wheezes are heard on pulmonary auscultation. An x-ray of the chest shows no abnormalities. Spirometry shows an FEV1:FVC ratio of 65% and an FEV1 of 60%. Which of the following is the most likely diagnosis?
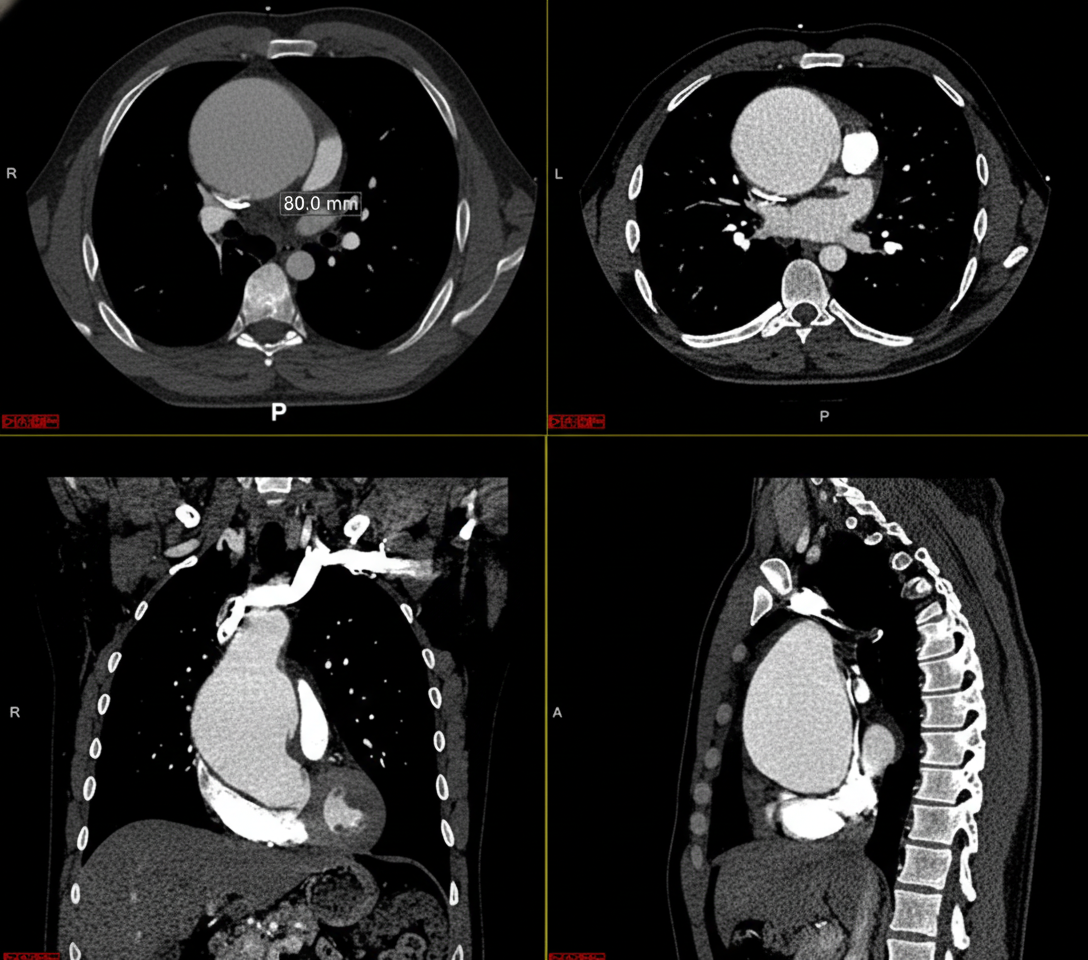
A previously healthy 32-year-old man comes to the physician because of a 1-week history of upper back pain, dyspnea, and a sensation of pressure in his chest. He has had no shortness of breath, palpitations, fevers, or chills. He emigrated from Ecuador when he was 5 years old. He does not smoke or drink alcohol. He takes no medications. He is 194 cm (6 ft 4 in) tall and weighs 70.3 kg (155 lb); BMI is 19 kg/m2. His temperature is 37.2°C (99.0°F), pulse is 73/min, respirations are 15/min, and blood pressure is 152/86 mm Hg in the right arm and 130/72 mm Hg in the left arm. Pulmonary examination shows faint inspiratory wheezing bilaterally. A CT scan of the chest with contrast is shown. Which of the following is the most likely underlying cause of this patient's condition?
A previously healthy 13-year-old girl is brought to the physician for evaluation of a 2-month history of fatigue. She reports recurrent episodes of pain in her right wrist and left knee. During this period, she has had a 4-kg (8.8-lb) weight loss. Her mother has rheumatoid arthritis. Her temperature is 38°C (100.4°F). Examination shows diffuse lymphadenopathy. Oral examination shows several painless oral ulcers. The right wrist and the left knee are swollen and tender. Laboratory studies show a hemoglobin concentration of 9.8 g/dL, a leukocyte count of 2,000/mm3, and a platelet count of 75,000/mm3. Urinalysis shows excessive protein. This patient's condition is associated with which of the following laboratory findings?
A 27-year-old Asian woman presents to her primary care physician with joint pain and a headache. She has had intermittent joint and muscle pain for the past several months in the setting of a chronic headache. She states that the pain seems to migrate from joint to joint, and her muscles typically ache making it hard for her to sleep. The patient's past medical history is non-contributory, and she is currently taking ibuprofen for joint pain. Physical exam is notable for an asymmetrical pulse in the upper extremities. The patient has lost 10 pounds since her previous visit 2 months ago. Laboratory values are notable for an elevated C-reactive protein and erythrocyte sedimentation rate. Which of the following is the best next step in management?
A 49-year-old woman presents to her primary care physician for a routine health maintenance examination. She says that she is currently feeling well and has not noticed any acute changes in her health. She exercises 3 times a week and has tried to increase the amount of fruits and vegetables in her diet. She has smoked approximately 1 pack of cigarettes every 2 days for the last 20 years. Her last pap smear was performed 2 years ago, which was unremarkable. Her past medical history includes hypertension and type II diabetes. Her mother was diagnosed with breast cancer at 62 years of age. The patient is 5 ft 5 in (165.1 cm), weighs 185 lbs (84 kg), and has a BMI of 30.8 kg/m^2. Her blood pressure is 155/98 mmHg, pulse is 90/min, and respirations are 18/min. Physical examination is unremarkable. Lipid studies demonstrate an LDL cholesterol of 130 mg/dL and an HDL cholesterol of 42 mg/dL. Which of the following is the best next step in management?
A 28-year-old woman presents with severe vertigo. She also reports multiple episodes of vomiting and difficulty walking. The vertigo is continuous, not related to the position, and not associated with tinnitus or hearing disturbances. She has a past history of acute vision loss in her right eye that resolved spontaneously several years ago. She also experienced left-sided body numbness 3 years ago that also resolved rapidly. She only recently purchased health insurance and could not fully evaluate the cause of her previous symptoms at the time they presented. The patient is afebrile and her vital signs are within normal limits. On physical examination, she is alert and oriented. An ophthalmic exam reveals horizontal strabismus. There is no facial asymmetry and her tongue is central on the protrusion. Gag and cough reflexes are intact. Muscle strength is 5/5 bilaterally. She has difficulty maintaining her balance while walking and is unable to perform repetitive alternating movements with her hands. Which of the following is the best course of treatment for this patient’s condition?
A 50-year-old woman comes to the physician because of worsening pain and swelling of her left knee. For the past year, she has had pain in her knees and hands bilaterally, but never this severe. During this period, she has also had difficulties moving around for about an hour in the mornings and has been sweating more than usual, especially at night. She has been sexually active with a new partner for the past 4 weeks, and they use condoms inconsistently. She occasionally drinks alcohol. The day before she drank 6 beers because she was celebrating a friend's birthday. Her temperature is 38.5°C (101.3°F), blood pressure is 110/70 mm Hg, and pulse is 92/min. The left knee is erythematous, swollen, and tender; movement is restricted due to pain. There is swelling of the metacarpophalangeal joints and proximal interphalangeal joints bilaterally. Arthrocentesis of the knee with synovial fluid analysis shows a greenish, turbid fluid, a cell count of 68,000 WBC/μL and Gram-negative diplococci. An x-ray of the affected knee is most likely to show which of the following findings?
A 74-year-old man presents to the emergency room with abdominal pain. He reports acute onset of left lower quadrant abdominal pain and nausea three hours prior to presentation. The pain is severe, constant, and non-radiating. He has had two maroon-colored bowel movements since the pain started. His past medical history is notable for hypertension, hyperlipidemia, atrial fibrillation, insulin-dependent diabetes mellitus, and rheumatoid arthritis. He takes lisinopril, hydrochlorothiazide, atorvastatin, dabigatran, methotrexate. He has a 60 pack-year smoking history and drinks 1-2 beers per day. He admits to missing some of his medications recently because he was on vacation in Hawaii. His last colonoscopy was 4 years ago which showed diverticular disease in the descending colon and multiple sessile polyps in the sigmoid colon which were removed. His temperature is 100.1°F (37.8°C), blood pressure is 145/85 mmHg, pulse is 100/min, and respirations are 20/min. On exam, he has notable abdominal distention and is exquisitely tender to palpation in all four abdominal quadrants. Bowel sounds are absent. Which of the following is the most likely cause of this patient’s condition?
A 66-year-old man undergoes a coronary artery bypass grafting. Upon regaining consciousness, he reports that he cannot see from either eye and cannot move his arms. Physical examination shows bilaterally equal, reactive pupils. A fundoscopy shows no abnormalities. An MRI of the brain shows wedge-shaped cortical infarcts in both occipital lobes. Which of the following is the most likely cause of this patient's current symptoms?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
