Cardiology — MCQs

On this page
A 27-year-old man presents to the emergency department with weakness and a fever for the past week. The patient is homeless and has a past medical history of alcohol and IV drug abuse. His temperature is 102°F (38.9°C), blood pressure is 107/68 mmHg, pulse is 120/min, respirations are 17/min, and oxygen saturation is 98% on room air. Physical exam is notable for a tremulous patient with antecubital scars and a murmur over the left lower sternal border. Blood cultures are drawn and the patient is started on vancomycin and ceftriaxone and is admitted to the ICU. The patient's fever and symptoms do not improve despite antibiotic therapy for which the initial identified organism is susceptible. Cultures currently reveal MRSA as one of the infective organisms. Which of the following is the best next step in management?
A 61-year-old white man presents to the emergency department because of progressive fatigue and shortness of breath on exertion and while lying down. He has had type 2 diabetes mellitus for 25 years and hypertension for 15 years. He is taking metformin and captopril for his diabetes and hypertension. He has smoked 10 cigarettes per day for the past 12 years and drinks alcohol occasionally. His temperature is 36.7°C (98.0°F) and blood pressure is 130/60 mm Hg. On physical examination, his arterial pulse shows a rapid rise and a quick collapse. An early diastolic murmur is audible over the left upper sternal border. Echocardiography shows severe chronic aortic regurgitation with a left ventricular ejection fraction of 55%–60% and mild left ventricular hypertrophy. Which of the following is an indication for aortic valve replacement in this patient?
A 38-year-old man is brought to the emergency department after losing consciousness upon rising from his chair at work. The patient has had progressive cough, shortness of breath, fever, and chills for 6 days but did not seek medical attention for these symptoms. He appears distressed, flushed, and diaphoretic. He is 170 cm (5 ft 7 in) tall and weighs 120 kg (265 lbs); BMI is 41.5 kg/m2. His temperature is 39.4°C (102.9°F), pulse is 129/min, respirations are 22/min, and blood pressure is 91/50 mm Hg when supine. Crackles and bronchial breath sounds are heard over the right posterior hemithorax. A 2/6 midsystolic blowing murmur is heard along the left upper sternal border. Examination shows diffuse diaphoresis, flushed extremities, and dullness to percussion over the right posterior hemithorax. The abdomen is soft and nontender. Multiple nurses and physicians have been unable to attain intravenous access. A large-bore central venous catheter is inserted into the right internal jugular vein by standard sterile procedure. Which of the following is the most appropriate next step in the management of this patient?
A 62-year-old man comes to the physician because of increased frequency of urination. He also says that he needs to urinate 4 to 5 times nightly and has difficulty initiating a urinary stream. He has had several episodes of acute cystitis treated with ciprofloxacin during the past year. Digital rectal examination shows a firm, symmetrically enlarged, non-tender prostate. This patient is most likely to develop which of the following complications?
A 42-year-old woman comes to the physician because of stiffness and pain in multiple joints. She says that the fingers on both of her hands have become increasingly stiff and difficult to move over the past 8 months. She also complains of nails that break easily and look spotty as well as chronic back pain. She had a urinary tract infection a year ago that was treated with antibiotics. She is sexually active with 2 male partners and uses condoms inconsistently. Her vitals are within normal limits. A photograph of her right hand is shown. There are multiple, well-demarcated red plaques with silvery-white scales over the shins and back. Serum studies show a negative rheumatoid factor and ANA. Which of the following is the most likely diagnosis?
A 37-year-old woman is being evaluated for difficulty with swallowing for the past few months. She explains that she experiences difficulty swallowing solid foods only. Her medical history is relevant for hypothyroidism and migraines. Her current medications include daily levothyroxine and acetaminophen as needed for pain. The vital signs include blood pressure 110/90 mm Hg, pulse rate 55/min, and respiratory rate 12/min. On physical examination, her abdomen is non-tender. Her voice is hoarse, but there is no pharyngeal hyperemia on oral examination. On cardiac auscultation, an opening snap followed by an early to mid-diastolic rumble is heard over the apex. A barium swallow X-ray is performed and is unremarkable. Echocardiography shows an enlarged left atrium and abnormal blood flow through 1 of the atrioventricular valves. What is the most likely valve abnormality seen in this patient?
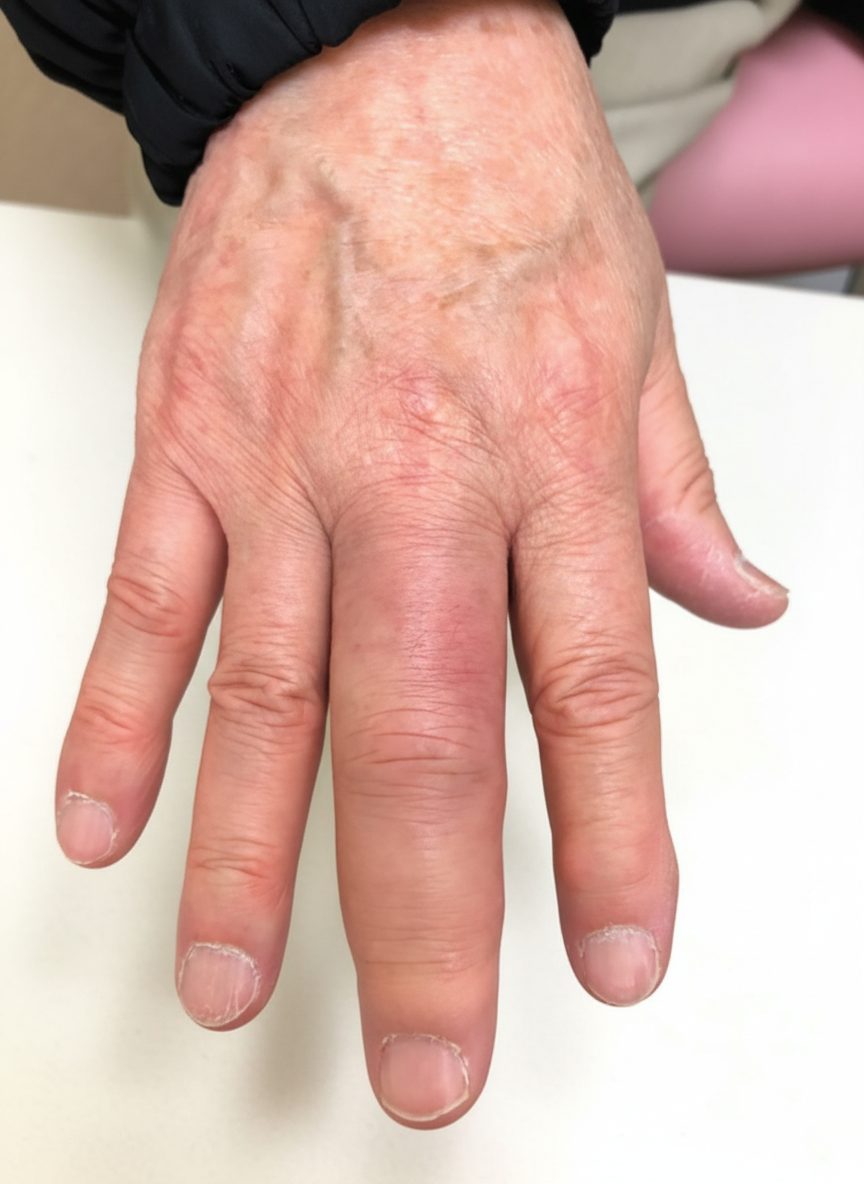
A 42-year-old man comes to the physician for a routine health maintenance examination. He feels well but has had several episodes of “finger pallor” over the past 4 months. During these episodes, the 4th finger of his left hand turns white. The color usually returns within 20 minutes, followed by redness and warmth of the finger. The episodes are not painful. The complaints most commonly occur on his way to work, when it is very cold outside. One time, it happened when he was rushing to the daycare center because he was late for picking up his daughter. The patient has gastroesophageal reflux disease treated with lansoprazole. His vital signs are within normal limits. The blood flow to the hand is intact on compression of the ulnar artery at the wrist, as well as on compression of the radial artery. When the patient is asked to immerse his hands in cold water, a change in the color of the 4th digit of his left hand is seen. A photograph of the affected hand is shown. His hemoglobin concentration is 14.2 g/dL, serum creatinine is 0.9 mg/dL, and ESR is 35 mm/h. Which of the following is the most appropriate next step in management?

A 60-year-old man comes to the physician because of a 6-month history of progressively worsening urinary frequency. He feels the urge to urinate every hour or two, which restricts his daily activities and interferes with his sleep. He has no fever, hematuria, or burning pain on micturition. He has hypertension and type 2 diabetes mellitus. Current medications include metformin and amlodipine. He does not smoke and drinks 1 to 2 beers daily. His vital signs are within normal limits. Abdominal examination shows no abnormalities. Digital rectal examination shows a nontender, firm, symmetrically enlarged prostate with no nodules. Which of the following is the most appropriate next step in management?
A 64-year-old man presents to his primary care physician's office for a routine check-up. His past medical history is significant for type 2 diabetes mellitus, hypertension, chronic atrial fibrillation, and ischemic cardiomyopathy. On his last visit three months ago, he was found to have hyperkalemia, at which time lisinopril and spironolactone were removed from his medication regimen. Currently, his medications include coumadin, aspirin, metformin, glyburide, metoprolol, furosemide, and amlodipine. His T is 37 C (98.6 F), BP 154/92 mm Hg, HR 80/min, and RR 16/min. His physical exam is notable for elevated jugular venous pressure, an S3 heart sound, and 1+ pitting pedal edema. His repeat lab work at the current visit is as follows: Sodium: 138 mEq/L, potassium: 5.7 mEq/L, chloride 112 mEq/L, bicarbonate 18 mEq/L, BUN 29 mg/dL, and creatinine 2.1 mg/dL. Which of the following is the most likely cause of this patient's acid-base and electrolyte abnormalities?
A 40-year-old man comes to the physician for a follow-up examination. He feels well. He has no urinary urgency, increased frequency, dysuria, or gross hematuria. He has a history of recurrent urinary tract infections. His last urinary tract infection was 3 months ago and was treated with ciprofloxacin. Current medications include a multivitamin. He has smoked one pack of cigarettes daily for 18 years. Vital signs are within normal limits. The abdomen is soft and nontender. There is no costovertebral angle tenderness. Laboratory studies show: Hemoglobin 11.2 g/dL Leukocyte count 9,500/mm3 Platelet count 170,000/mm3 Serum Na+ 135 mEq/L K+ 4.9 mEq/L Cl- 101 mEq/L Urea nitrogen 18 mg/dL Creatinine 0.6 mg/dL Urine Blood 2+ Protein negative RBC 5–7/hpf, normal shape and size RBC casts negative WBC 0–2/hpf Bacteria negative Urine cultures are negative. Urine analysis is repeated and shows similar results. A cystoscopy shows no abnormalities. Which of the following is the most appropriate next step in management?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
