Cardiology — MCQs

On this page
A 47-year-old woman comes to the physician because of a 1-month history of progressive weakness. She has had increased difficulty climbing stairs and standing from a seated position. She takes no medications. Neurologic examination shows weakness of the proximal muscles. Skin examination shows diffuse erythema of the upper back, posterior neck, and shoulders. A photograph of the patient's eye is shown. Antibodies against which of the following are most likely to be present in this patient?
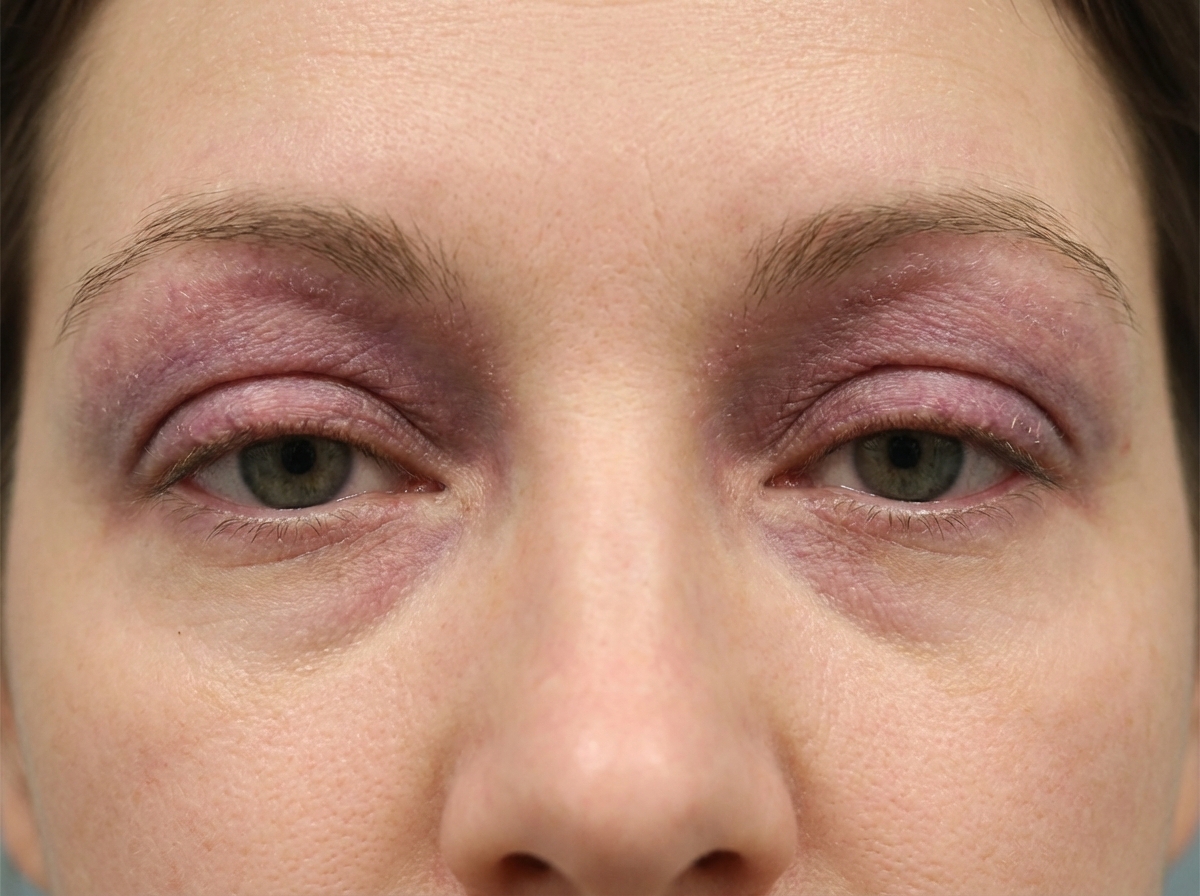
A 12-year-old boy is brought by his mother to the emergency room because of a swollen, hot, and tender knee that he sustained after falling on his way home. He has never had a swollen joint before; however, he has had frequent nosebleeds throughout his life. His mother is worried because they live with her parents who are currently on blood thinners. Every morning she puts the blood thinner pill in the boy's grandfather's milk and was concerned that she may have switched it this morning. Family history reveals a number of uncles who have had bleeding disorders; however, the mother does not know the exact disorder suffered by these relatives. A hematologic panel reveals the following findings: Bleeding time: Increased Prothrombin time: 12 seconds Partial thromboplastin time (PTT): 55 seconds PTT after factor mixing study: 37 seconds Which of the following most likely explains the abnormal partial thromboplastin time in this patient?
A 42-year-old man comes to the physician for a health maintenance examination. He has had generalized fatigue and muscle aches since his previous visit 6 months ago. He has hypertension and gastroesophageal reflux disease. Current medications include amlodipine and omeprazole. His temperature is 37.1°C (98.1°F), pulse is 88/min and blood pressure is 156/102 mm Hg. Physical examination shows no abnormalities. Serum studies show: Na+ 143 mEq/L K+ 2.3 mEq/L Cl- 100 mEq/L HCO3- 31 mEq/L Urea nitrogen 14 mg/dL Creatinine 1 mg/dL His blood pressure medication is discontinued. One week later his plasma aldosterone concentration is 35 ng/dL (N=3.6 - 24.0 ng/dL) and plasma renin activity is 0.4 ng/mL/h (N=0.3 to 4.2 ng/mL/h). An oral sodium loading test over 3 days fails to reduce aldosterone. A contrast-enhanced CT scan of the abdomen and pelvis shows a 3-cm, homogenous, right-sided adrenal mass with rapid contrast washout. He is counseled about his treatment options and chooses to pursue surgery. Which of the following is the most appropriate next step in management?
A 68-year-old female presents to the emergency room with acute onset of dyspnea and hemoptysis. Her past medical history is unremarkable and she has had no prior surgeries. A ventilation-perfusion scan demonstrates a large perfusion defect that is not matched by a ventilation defect in the left lower lobe. Which of the following would you also expect to find in this patient:
A 45-year-old African American woman presents to her family physician for a routine examination. Past medical history is positive for amyloidosis and non-rhythm-based cardiac abnormalities secondary to the amyloidosis. Which of the following cardiac parameters would be expected in this patient?
A 34-year-old man comes to the physician for a routine health maintenance examination. He was diagnosed with HIV 8 years ago. He is currently receiving triple antiretroviral therapy. He is sexually active and uses condoms consistently. He is planning a trip to Thailand with his partner to celebrate his 35th birthday in 6 weeks. His last tetanus and diphtheria booster was given 4 years ago. He received three vaccinations against hepatitis B 5 years ago. He had chickenpox as a child. Other immunization records are unknown. Vital signs are within normal limits. Cardiopulmonary examination shows no abnormalities. Leukocyte count shows 8,700/mm3, and CD4+ T-lymphocyte count is 480 cells/mm3 (Normal ≥ 500); anti-HBs is 150 mIU/mL. Which of the following recommendations is most appropriate at this time?
Two days after admission to the hospital, a 74-year-old man develops confusion and headache. He has also been vomiting over the past hour. His temperature is 36.7°C (98°F), pulse is 98/min, respirations are 22/min, and blood pressure is 140/80 mm Hg. He is lethargic and oriented only to person. Examination shows flushed skin. Fundoscopic examination shows bright red retinal veins. Serum studies show: Na+ 138 mEq/L K+ 3.5 mEq/L Cl- 100 mEq/L HCO3- 17 mEq/L Creatinine 1.2 mg/dL Urea nitrogen 19 mg/dL Lactate 8.0 mEq/L (N = 0.5 - 2.2 mEq/L) Glucose 75 mg/dL Arterial blood gas analysis on room air shows a pH of 7.13. This patient's current presentation is most likely due to complications from treatment of which of the following conditions?
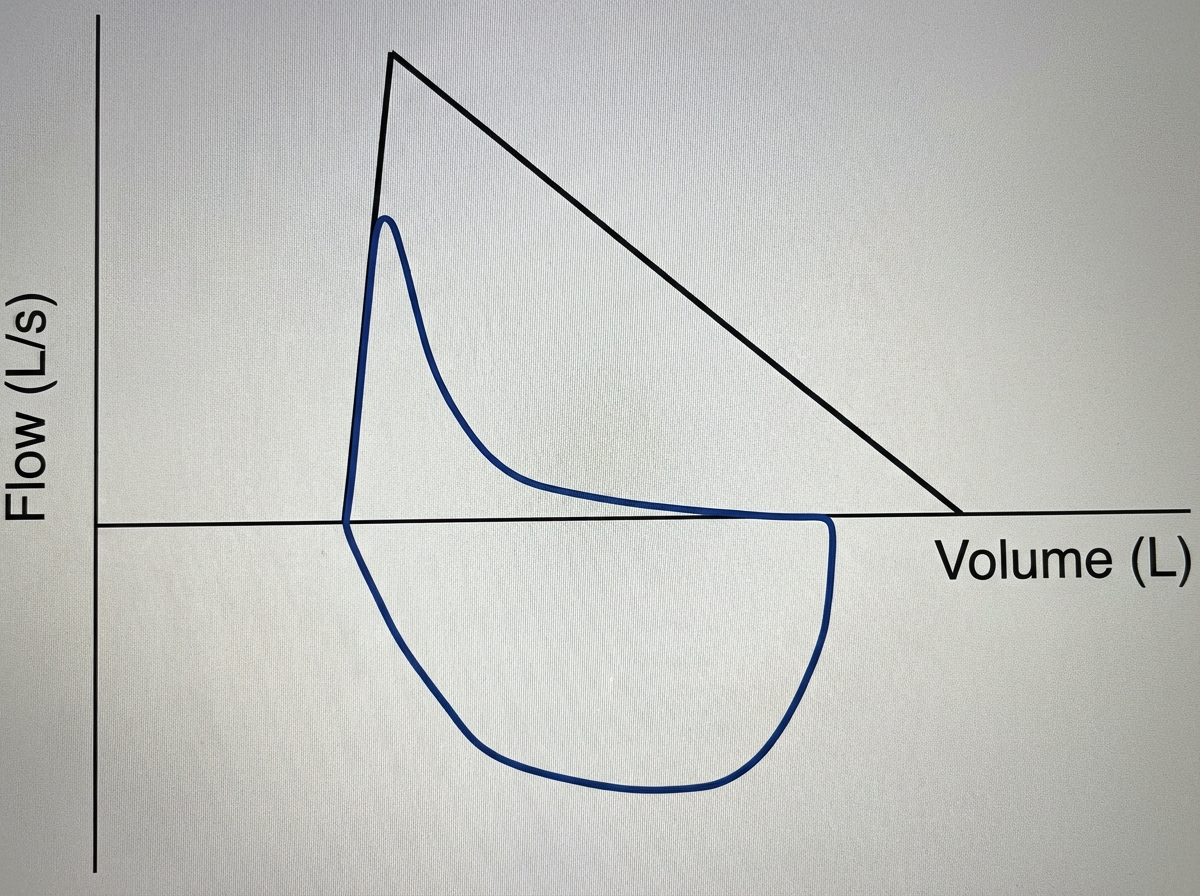
A 63-year-old woman comes to the physician because of worsening shortness of breath, cough, and a 4-kg (8.8-lb) weight loss over the last year. She has no history of serious illness and takes no medications. She has smoked one pack of cigarettes daily for 35 years. Her temperature is 37°C (98.6°F), pulse is 92/min, respirations are 20/min, blood pressure is 124/78 mm Hg, and pulse oximetry on room air shows an oxygen saturation of 93%. Physical examination shows decreased breath sounds. A flow-volume loop obtained via pulmonary function testing is shown. Which of the following is the most likely cause of this patient's respiratory symptoms?
A 30-year-old African American woman comes to the physician because of a 3-month history of increasing shortness of breath, cough, and intermittent fever. She works in a local factory that manufactures components for airplanes. She drinks 2–3 glasses of wine daily and has smoked half a pack of cigarettes daily for the past 5 years. Physical examination shows a purple rash on her cheeks and nose. An x-ray of the chest shows bilateral hilar adenopathy and a calcified nodule in the left lower lobe. A bronchoalveolar lavage shows a CD4:CD8 T-lymphocyte ratio of 10:1 (N=2:1). A biopsy of the nodule shows a noncaseating granuloma. Which of the following is the strongest predisposing factor for the development of this patient's condition?
A 25-year-old man is in the middle of an ascent up a mountain, at an elevation of about 4,500 meters. This is the 4th day of his expedition. His friend notices that in the last few hours, he has been coughing frequently and appears to be short of breath. He has used his albuterol inhaler twice in the past 4 hours, but it does not seem to help. Within the past hour, he has coughed up some frothy, slightly pink sputum and is now complaining of nausea and headache. Other than his asthma, which has been well-controlled on a steroid inhaler, he is healthy. Which of the following is the most likely cause of this man’s symptoms?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
