Cardiology — MCQs

On this page
A 48-year-old man comes to the physician because of a 1-month history of a productive cough. He has daily yellowish sputum with occasional streaks of blood in it. Twelve years ago, he was treated for pulmonary tuberculosis for 6 months. He has hypertension and coronary artery disease. He does not smoke or drink alcohol. Current medications include metoprolol, clopidogrel, rosuvastatin, and enalapril. He appears thin. His temperature is 37.2°C (99°F), pulse is 98/min, and blood pressure is 138/92 mm Hg. Pulmonary examination shows inspiratory crackles at the right infraclavicular area. His hemoglobin concentration is 12.2 g/dL, leukocyte count is 11,300/mm3, and erythrocyte sedimentation rate is 38 mm/h. Urinalysis is normal. An x-ray of his chest is shown. Which of the following is most likely to be seen on further evaluation of the patient?
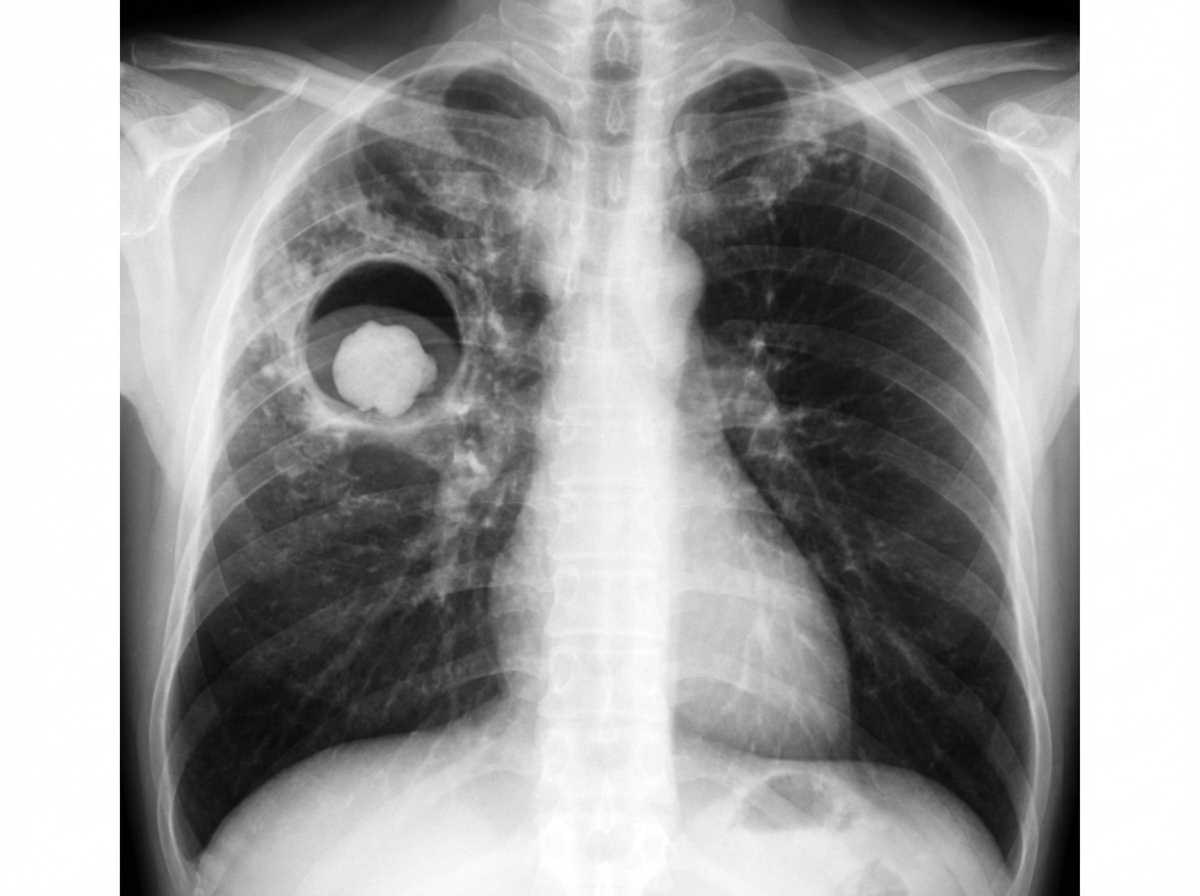
A 33-year-old African American woman presents to the clinic complaining of pain and swelling of her hands and wrists for the past 5 months. The symptoms are worse in the morning and are associated with stiffness that lasts about 15 minutes. She also complains of profound fatigue and decreased appetite. She is sexually active with one partner in a monogamous relationship. Past medical history is unremarkable and she is taking oral contraceptives. She smokes 1–2 cigarettes per day and drinks alcohol socially on the weekends. Temperature is 37.2°C (99.1°F), blood pressure is 130/82 mm Hg, pulse is 76/min, and respirations are 12/min. Physical examination reveals wrists that are tender to palpation, warm, and mildly swollen. Several metacarpophalangeal and proximal interphalangeal joints on both hands are also tender. Hand and wrist strength is 5/5 bilaterally. A non-tender ulcer on the buccal mucosa is also noted. When asked about it, the patient reports that it has been there for several months and does not bother her. Laboratory results are as follows: Complete blood count Hemoglobin 10.3 g/dL Platelets 90,000/mm3 Leukocytes 6,700/mm3 Blood urea nitrogen 16 mg/dL Creatinine 2.1 mg/dL Urinalysis Blood 10–20 red blood cells/hpf Protein 2+ protein B-HCG Negative Which of the following is the most likely diagnosis in this patient?
A 62-year-old man presents to the physician because of difficulty initiating urination, terminal dribbling of urine, and bone pain for 3 months. He has no medical history of serious illness, and he currently takes no medications. His father had prostate cancer at age 58. His vital signs are within normal limits. The physical examination shows tenderness over the lower lumbar vertebrae and the right pelvis. The digital rectal exam (DRE) shows a prostate size equivalent to 2 finger pads with a hard nodule. The laboratory tests show the following results: Serum Prostate-specific antigen (PSA) 15 ng/mL Testosterone 350 ng/mL (N=270–1070 ng/mL) The prostate biopsy confirms the presence of prostate cancer with aggressive histologic features. The MRI shows local extension of the tumor. The radionuclide bone scan shows multiple metastatic sites. Which of the following is the most appropriate next step in management?
A 45-year-old woman comes to the physician because of shortness of breath while lying on her back over the past month. During this period, she has also had several episodes of bloody coughing. The patient reports that she had a heart problem when she was a child that was treated with antibiotics. She emigrated to the US from Russia 5 years ago. There is no family history of serious illness. Pulmonary examination shows crackles at both lung bases. Cardiac examination is shown. An ECG shows tachycardia and no P waves. Which of the following is the most likely diagnosis?
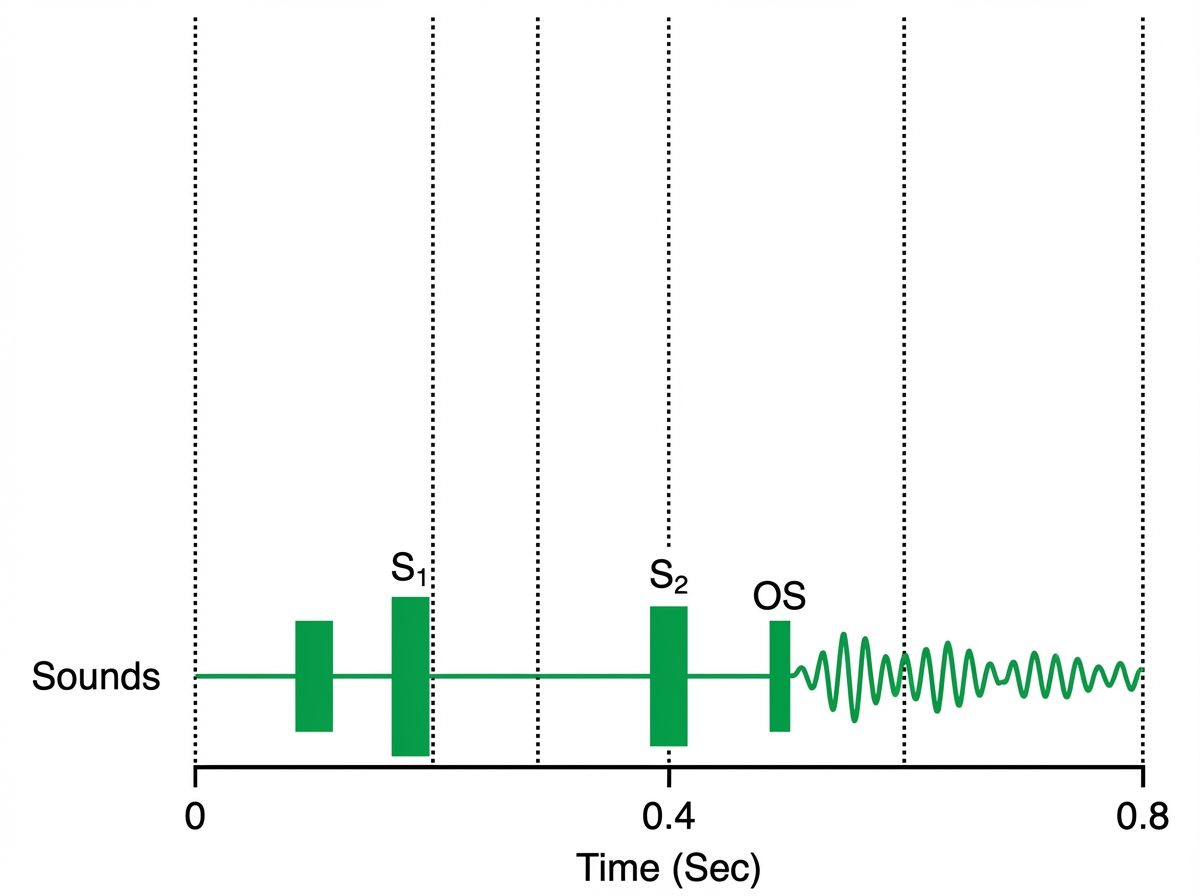
A previously healthy 48-year-old man comes to the physician for a 3-month history of myalgias and recurrent episodes of retrosternal chest pain and dizziness. He has had a 5-kg (11-lb) weight loss during this period. His temperature is 39.1°C (102.3°F), pulse is 90/min, and blood pressure is 160/102 mm Hg. Physical examination shows lacy, purplish discoloration of the skin with multiple erythematous, tender subcutaneous nodules on the lower legs. Some of the nodules have central ulcerations. Serum studies show an erythrocyte sedimentation rate of 76 mg/dL and creatinine level of 1.8 mg/dL. Renal MR angiography shows irregular areas of dilation and constriction in the renal arteries bilaterally. Further evaluation of this patient is most likely to show which of the following?
A previously healthy 35-year-old woman comes to the emergency department because of a sudden onset of difficulty breathing that began when she woke up that morning. She also reports a dry cough and chest pain that is worse with inspiration. She does not smoke, drink alcohol, or use illicit drugs. Her only medication is an oral contraceptive. Her temperature is 38°C (100.4°F), pulse is 90/min, respirations are 22/min, and blood pressure is 120/70 mm Hg. Oxygen saturation is 93% on room air. Physical examination is unremarkable. An ECG shows non-specific ST segment changes. An x-ray of the chest shows no abnormalities. In addition to oxygen supplementation, which of the following is the most appropriate next step in management?
A 12-year-old boy presents with a 3-day history of frothy brown urine. He does not complain of any other symptoms. He notes that 3 weeks ago he had a fever with a sore throat, but he did not receive any treatment at the time. His blood pressure is 152/94 mm Hg, heart rate is 72/min, respiratory rate is 15/min, and temperature is 37.0°C (98.6°F). Review of his medical record shows that his blood pressure was 118/74 mm Hg just 4 weeks ago. Laboratory analysis reveals elevated serum creatinine, hematuria with RBC casts, and elevated urine protein without frank proteinuria. What laboratory test can confirm the most likely diagnosis in this patient?
A 64-year-old woman comes to the physician because of worsening intermittent nausea and burning pain in her upper abdomen for 4 hours. She has not had retrosternal chest pain, shortness of breathing, or vomiting. She has hypertension and type 2 diabetes mellitus. She has smoked one pack of cigarettes daily for 20 years. Her only medications are lisinopril and insulin. Her temperature is 37°C (98.6°F), pulse is 90/min, respirations are 12/min, and blood pressure is 155/75 mm Hg. The lungs are clear to auscultation. The abdomen is soft, with mild tenderness to palpation of the epigastrium but no guarding or rebound. Bowel sounds are normal. An ECG is shown. This patient's current condition is most likely to cause which of the following findings on cardiac examination?
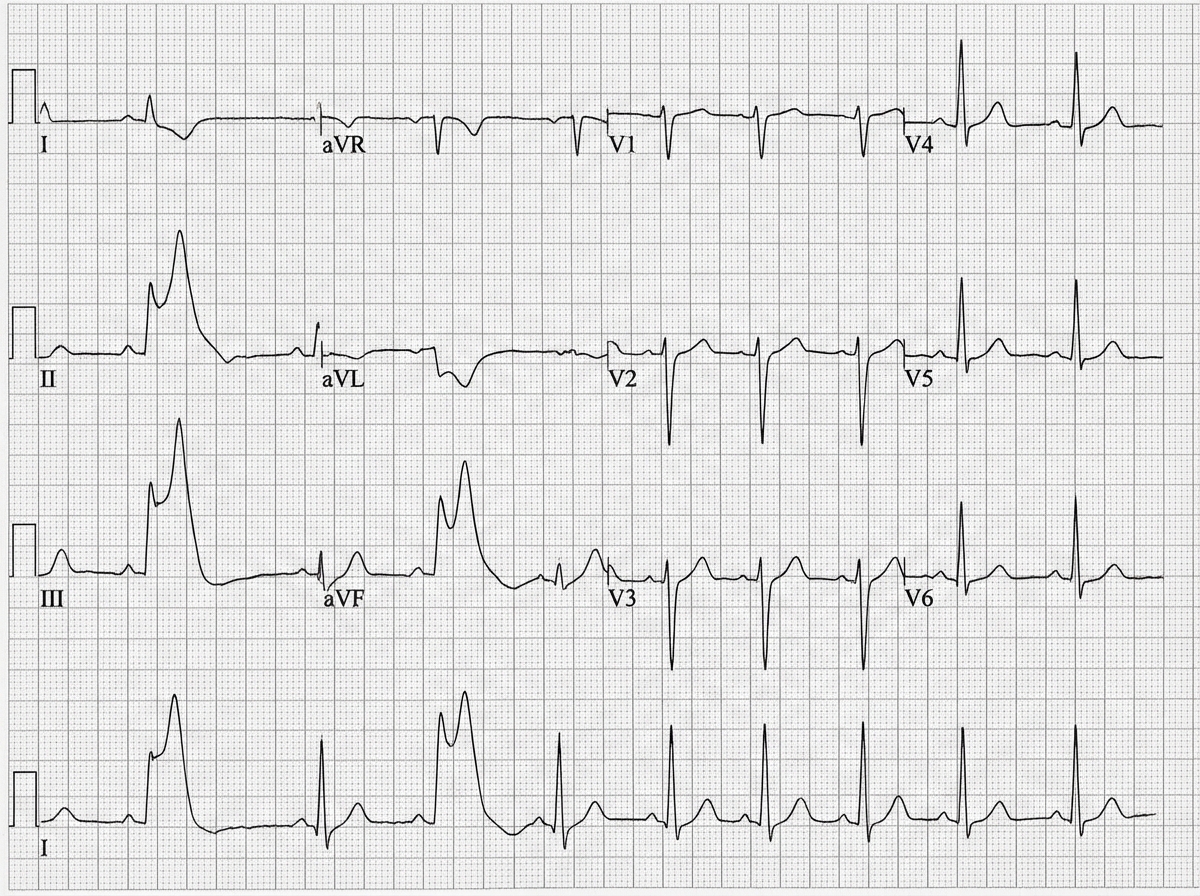
A 78-year-old male has been hospitalized for the past 3 days after undergoing a revision left total hip replacement. Over the past several hours, the nursing staff reports that the patient has exhibited fluctuating periods of intermittent drowsiness and confusion where he has been speaking to nonexistent visitors in his hospital room. The patient's daughter is present at bedside and reports that the patient lives alone and successfully manages his own affairs without assistance. Which of the following is most likely true of this patient's current condition?
Eight hours after undergoing successful cholecystectomy, a 65-year-old man with scoliosis complains of shortness of breath. Respirations are 28/min and pulse oximetry on room air shows an oxygen saturation of 85%. Physical examination shows kyphotic deformation of the thorax. Cardiopulmonary examination shows intercostal retractions and diminished breath sounds on the left side. There is trace pedal edema bilaterally. An x-ray of the chest shows bilateral fluffy infiltrates, and the cardiac silhouette is shifted slightly to the left side. Which of the following is the most likely explanation for this patient's hypoxia?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
