Cardiology — MCQs

On this page
Five days after admission into the ICU for drug-induced acute kidney injury, a 27-year-old woman develops fever. She is currently on a ventilator and sedatives. Hemodialysis is performed via a catheter placed in the right internal jugular vein. Feeding is via a nasogastric tube. An indwelling urinary catheter shows minimum output. Her blood pressure is 85/45 mm Hg, the pulse is 112/min, the respirations are 32/min, and the temperature is 39.6°C (103.3°F). The examination of the central catheter shows erythema around the insertion site with no discharge. Lung auscultation shows rhonchi. Cardiac examination shows no new findings. A chest CT scan shows bilateral pleural effusions with no lung infiltration. Empirical antibiotic therapy is initiated. Blood cultures obtained from peripheral blood and the catheter tip show S. aureus with a similar antibiogram. Urinary culture obtained from the indwelling catheter shows polymicrobial growth. Which of the following best explains this patient’s recent findings?
Six days after undergoing a left hemicolectomy for colorectal carcinoma, a 59-year-old man collapses in the hospital hallway and is unconscious for 30 seconds. Afterwards, he complains of shortness of breath and chest pain with deep inhalation. He has hypertension and hyperlipidemia. He smoked one pack of cigarettes daily for 35 years but quit prior to admission to the hospital. He does not drink alcohol. He is in distress and appears ill. His temperature is 36.5°C (97.7°F), blood pressure is 80/50 mm Hg, and pulse is 135/min and weak. Oxygen saturation is 88% on room air. Physical examination shows elevated jugular venous distention. Cardiac examination shows a regular, rapid heart rate and a holosystolic murmur that increases during inspiration. His abdomen is soft and mildly tender to palpation around the surgical site. Examination of his extremities shows pitting edema of the left leg. His skin is cold and clammy. Further examination is most likely to reveal which of the following findings?
A 63-year-old man presents to his primary care physician complaining of excessive daytime sleepiness. He explains that this problem has worsened slowly over the past few years but is now interfering with his ability to play with his grandchildren. He worked previously as an overnight train conductor, but he has been retired for the past 3 years. He sleeps approximately 8-9 hours per night and believes his sleep quality is good; however, his wife notes that he often snores loudly during sleep. He has never experienced muscle weakness or hallucinations. He has also been experiencing headaches in the morning and endorses a depressed mood. His physical exam is most notable for his large body habitus, with a BMI of 34. What is the best description of the underlying mechanism for this patient's excessive daytime sleepiness?
A 48-year-old woman presents to her primary care physician with complaints of persistent fatigue, dizziness, and weight loss for the past 3 months. She has a history of hypothyroidism and takes thyroxine replacement. Her blood pressure is 90/60 mm Hg in a supine position and 65/40 mm Hg while sitting, temperature is 36.8°C (98.2°F), and pulse is 75/min. On physical examination, there is a mild increase in thyroid size, with a rubbery consistency. Her skin shows diffuse hyperpigmentation, more pronounced in the oral mucosa and palmar creases. Which of the following best represent the etiology of this patient’s condition?
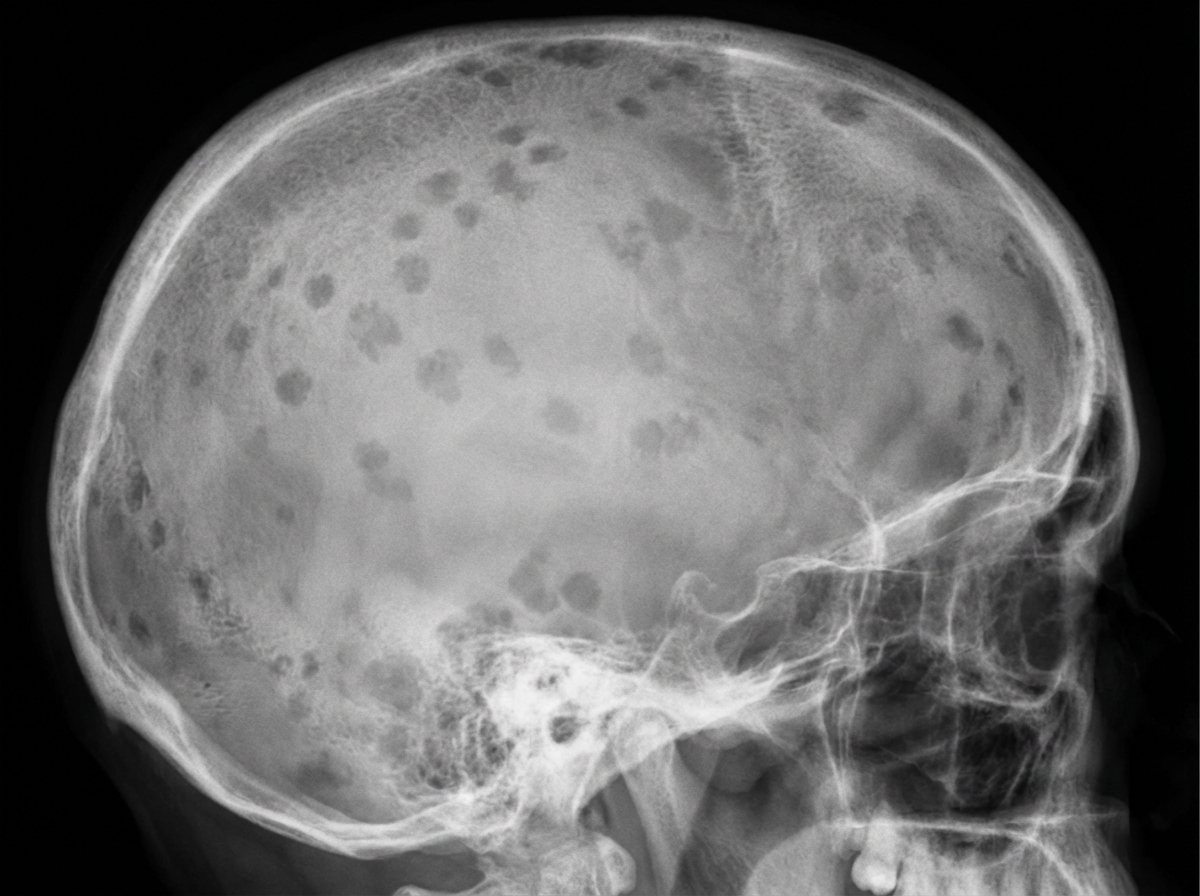
A 71-year-old African American man is brought to the emergency department with a worsening productive cough and dyspnea for 2 days. He has had generalized bone pain for 2 months. He was admitted for pyelonephritis last month. He also received outpatient treatment for pneumonia almost 2 months ago. Over the past 2 months, he has been taking over-the-counter ibuprofen for pain as needed. He appears anxious. The vital signs include: temperature 38.8°C (101.8°F), pulse 95/min, respiratory rate 20/min, and blood pressure 155/90 mm Hg. The conjunctivae are pale. Crackles are heard in the right lower lobe. The cardiac examination shows no abnormalities. The laboratory studies show the following: Hemoglobin 9 g/dL Mean corpuscular volume 95 μm3 Leukocyte count 13,500/mm3 Segmented neutrophils 75% Lymphocytes 25% Platelet count 240,000/mm3 ESR 85 mm/hr Serum Na+ 135 mEq/L K+ 4.2 mEq/L Cl− 113 mEq/L HCO3− 20 mEq/L Ca+ 12.4 mg/dL Albumin 4 g/dL Urea nitrogen 38 mg/dL Creatinine 2.2 mg/dL A chest X-ray shows a right lower lobe opacity and blurring of the ipsilateral diaphragmatic dome. Skull and pelvic X-rays are performed (see image). Which of the following is the most likely underlying cause of this patient’s recent infections?
A 23-year-old woman presents with ongoing diplopia for 1 week. She has noticed that her diplopia is more prominent when she looks at objects in her periphery. It does not present when looking straight ahead. She does not have a fever, headache, ocular pain, lacrimation, blurring of vision, or changes in her color vision. She is a college student and is otherwise healthy. The neurological examination reveals that when she looks to the left, her right eye does not adduct while her left eye abducts with nystagmus. Furthermore, when she looks to the right, her left eye does not adduct while her right eye abducts with prominent nystagmus. Her pupils are bilateral, equal and reactive to light and accommodation. The convergence is normal. The rest of the cranial nerve examination is unremarkable. What is the next best step in the management of this patient?
A 65-year-old man with hypertension and type 2 diabetes mellitus is brought to the emergency department 20 minutes after the onset of severe anterior chest pain and shortness of breath. He has smoked one pack of cigarettes daily for 30 years. He appears distressed. His pulse is 116/min, respirations are 22/min, and blood pressure is 156/88 mm Hg. Pulse oximetry on room air shows an oxygen saturation of 98%. A grade 3/6, high-pitched, blowing, diastolic murmur is heard over the right upper sternal border. Which of the following is the most likely cause of this patient's symptoms?
A 39-year-old woman presents with progressive weakness, exercise intolerance, and occasional dizziness for the past 3 months. Past medical history is unremarkable. She reports an 18-pack-year smoking history and drinks alcohol rarely. Her vital signs include: temperature 36.6°C (97.8°F), blood pressure 139/82 mm Hg, pulse 98/min. Physical examination is unremarkable. Her laboratory results are significant for the following: Hemoglobin 9.2 g/dL Erythrocyte count 2.1 million/mm3 Mean corpuscular volume (MCV) 88 μm3 Mean corpuscular hemoglobin (MCH) 32 pg/cell Leukocyte count 7,500/mm3 Which of the following is the best next step in the management of this patient’s condition?
A 45-year-old woman comes to the physician because of fatigue, irregular menses, and recurrent respiratory infections for the past 6 months. Her blood pressure is 151/82 mm Hg. Physical examination shows a round face, thinning of the skin, and multiple bruises on her arms. Further studies confirm the diagnosis of an ACTH-secreting pituitary adenoma. This patient is at greatest risk for which of the following?
A 54-year-old man comes to the emergency department because of a 3-week history of intermittent swelling of his left arm and feeling of fullness in his head that is exacerbated by lying down and bending over to tie his shoes. Physical examination shows left-sided facial edema and distention of superficial veins in the neck and left chest wall. Which of the following is the most likely cause of this patient's symptoms?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
