Cardiology — MCQs

On this page
A 74-year-old gentleman presents to his family practitioner with the complaint of an inability to open his left eye since this morning. He also complains of intermittent pain and numbness in his left arm that has been present for the last few days. He denies ocular pain, difficulty swallowing, fatigability, or diplopia. His symptoms remain constant without fluctuation. He has a history of diabetes mellitus type 2, hypertension, and hypercholesterolemia. Further history reveals that he has lost 5.4 kg (12 lb) of weight in the past 4 months. He is a chronic smoker with a 72 pack-year smoking history. His blood pressure is 142/76 mm Hg, the heart rate is 76/min, the respiratory rate is 12/min, the temperature is 36.8°C (98.4°F), and BMI is the 18.2 kg/m2. The patient is awake, alert, and oriented to person, place, and time. He has partial drooping of the left eyelid while the right eyelid appears normal. The left pupil is 1 mm and the right pupil is 3 mm in diameter. Extraocular muscle movements are normal. What additional clinical feature would most likely be present in this patient?
A 68-year-old male is brought to the emergency department by his wife. An hour earlier, he dropped to the floor and began to violently shake his extremities. He urinated on the carpet and seemed confused for several minutes after. He is now feeling better. He has never experienced an episode like this before, nor does he think anyone in his family has. He and his wife are concerned that he has unintentionally lost 22.6 kg (50 lb) in the past 6 months. He has also been experiencing chest pain and has coughed up blood on a few occasions. He has a 50-pack-year smoking history and quit 2 years ago. His temperature is 36.8°C (98.2°F), heart rate is 98/min, respiratory rate is 15/min, blood pressure is 100/75 mm Hg, and his O2 saturation is 100% on room air. The physical exam, including a full neurologic and cardiac assessment, demonstrates no abnormal findings. Edema, ascites, and skin tenting are notably absent. A brain MRI does not indicate areas of infarction or metastatic lesions. ECG is normal. Urine toxicology screen is negative. EEG is pending. Laboratory findings are shown below: BUN 15 mg/dL N: 7 to 20 mg/dL pCO2 40 mm Hg N: 35-45 mm Hg Creatinine 0.8 mg/dL N: 0.8 to 1.4 mg/dL Glucose 95 mg/dL N: 64 to 128 mg/dL Serum chloride 103 mmol/L N: 101 to 111 mmol/L Serum potassium 3.9 mEq/L N: 3.7 to 5.2 mEq/L Serum sodium 115 mEq/L N: 136 to 144 mEq/L Total calcium 2.3 mmol/L N: 2-2.6 mmol/L Magnesium 1.7 mEq/L N: 1.5-2 mEq/L Phosphate 0.9 mmol/L N: 0.8-1.5 mmol/L Hemoglobin 14 g/dL N: 13-17 g/dL (men), 12-15 g/dL (women) Glycosylated hemoglobin 5.5% N: 4%-6% Total cholesterol 4 mmol/L N: 3-5.5 mmol/L Bicarbonate (HCO3) 19 mmol/L N: 18-22 mmol/L What is indicated first?
A 31-year-old man is referred to a neurologist due to his gradually increasing eccentric behavior and involuntary movements, especially the movements of his arms and hands. He also has difficulty with his short-term memory. Past medical history is otherwise noncontributory. His father had similar symptoms before he died but those symptoms started at the age of 33. His blood pressure is 125/92 mm Hg, pulse is 90/min, respiratory rate 12/min, and temperature is 36.6°C (97.9°F). Physical exam reveals involuntary writhing movements of hands, slow eye movements, and sporadic rigidity. The physician explains that this is an inherited disorder where the symptoms occur progressively at an earlier age than the parent and often with increased severity in the future generations. Which of the following is the most likely diagnosis of this patient?
A 75-year-old woman with late-onset autoimmune diabetes mellitus, rheumatoid arthritis, coronary artery disease, and idiopathic pulmonary fibrosis presents to the ship medic with altered mental status. While on her current cruise to the Caribbean islands, she experienced nausea, vomiting, and diarrhea. She takes aspirin, simvastatin, low-dose prednisone, glargine, and aspart. She is allergic to amoxicillin and shellfish. She works as a greeter at a warehouse and smokes 5 packs/day. Her temperature is 100.5°F (38.1°C), blood pressure is 90/55 mmHg, pulse is 130/min, and respirations are 30/min. Her pupils are equal and reactive to light bilaterally. Her lungs are clear to auscultation bilaterally, but her breath has a fruity odor. She has an early systolic murmur best appreciated at the left upper sternal border. She has reproducible peri-umbilical tenderness. Which of the following will most likely be present in this patient?
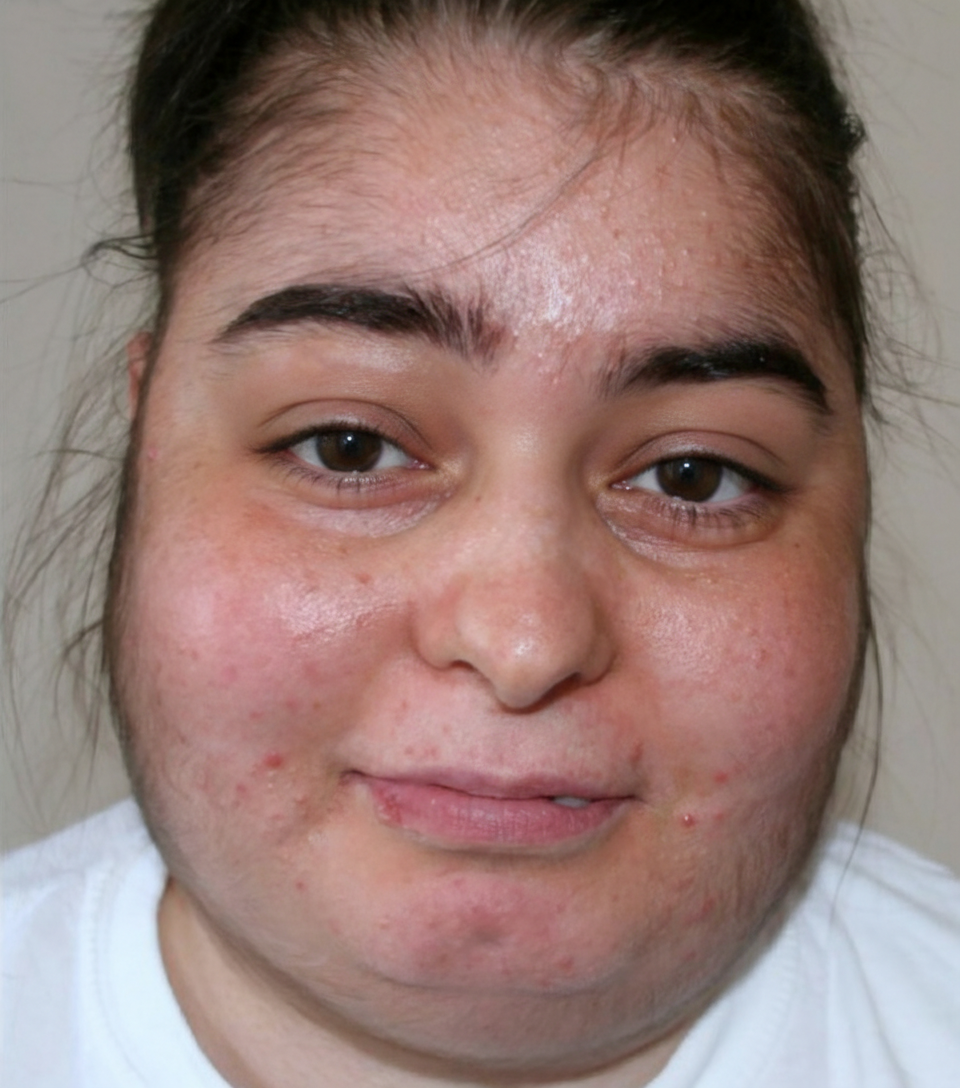
A 69-year-old man presents with granulomatosis with polyangiitis diagnosed about 8 months ago. He was treated appropriately and states that his symptoms are well controlled. He is presenting today for a general follow up visit. His temperature is 99.0°F (37.2°C), blood pressure is 184/104 mmHg, pulse is 88/min, respirations are 12/min, and oxygen saturation is 98% on room air. His physical examination is notable for the findings in Figures A and B. Which of the following would be found in this patient on serum laboratory studies?
A 15-year-old boy is brought to the office by his mother with complaints of facial puffiness and smoky urine. The mother noticed puffiness on her son’s face a week ago, and it has been progressively worsening since then. She also states that her son had a sore throat 3 weeks ago. The patient does not have fever/chills, changes in urinary frequency, or abdominal discomfort. On physical examination, facial edema is noted. The vital signs include: blood pressure 145/85 mm Hg, pulse 96/min, temperature 36.7°C (98.1°F), and respiratory rate 20/min. A complete blood count report shows: Hemoglobin 10.1 g/dL RBC 4.9 million cells/µL Hematocrit 46% Total leukocyte count 6,800 cells/µL Neutrophils 70% Lymphocytes 26% Monocytes 3% Eosinophil 1% Basophils 0% Platelets 210,000 cells/µL ESR 18 mm (1st hour) Urinalysis shows: pH 6.4 Color dark brown RBC plenty WBC 3–4/HPF Protein absent Cast RBC and granular casts Glucose absent Crystal none Ketone absent Nitrite absent Which of the following laboratory findings can be expected in this patient?
A 37-year-old man presents to the emergency department for a persistent fever. The patient states he has felt unwell for the past week and has felt subjectively febrile. The patient has a past medical history of a suicide attempt and alcohol abuse. He is not currently taking any medications. The patient admits to using heroin and cocaine and drinking 5-8 alcoholic drinks per day. His temperature is 103°F (39.4°C), blood pressure is 92/59 mmHg, pulse is 110/min, respirations are 20/min, and oxygen saturation is 96% on room air. Cardiopulmonary exam is notable for a systolic murmur heard best along the left sternal border. Dermatologic exam reveals scarring in the antecubital fossa. Which of the following is the next best step in management?
A 55-year-old male bodybuilder presents to the emergency department with weakness of his right arm. The patient states he has experienced these symptoms for a few weeks; however, today his hand felt so weak he dropped his cup of tea. The patient has a past medical history of diabetes. He drinks 2-7 alcoholic drinks per day and has smoked 2 packs of cigarettes per day since he was 25. The patient admits to using anabolic steroids. He has lost 17 pounds since he last came to the emergency department 1 month ago. His temperature is 99.5°F (37.5°C), blood pressure is 177/108 mmHg, pulse is 90/min, respirations are 17/min, and oxygen saturation is 98% on room air. Physical exam reveals decreased sensation in the right arm and 2/5 strength in the right arm and 5/5 strength in the left arm. The patient states that he is experiencing a dull aching and burning pain in his right arm during the exam. Which of the following is the most likely diagnosis?
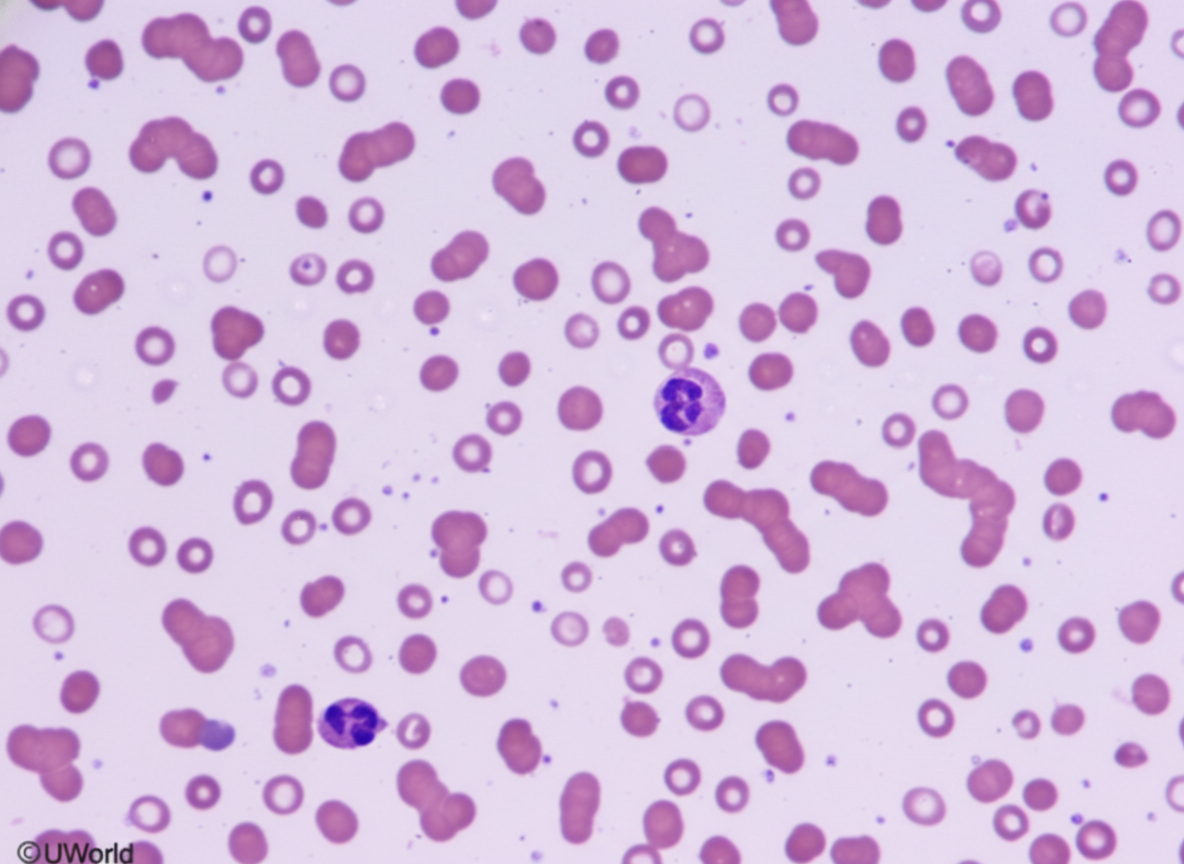
A 69-year-old woman comes to the physician because of a 3-week history of headache and worsening vision. Ophthalmologic examination shows a visual acuity of 20/120 in the right eye and 20/80 in the left eye. Physical examination shows no other abnormalities. Laboratory studies show a hemoglobin of 14.2 g/dL and total serum calcium of 9.9 mg/dL. A photomicrograph of a peripheral blood smear is shown. Serum electrophoresis shows increased concentration of a pentameric immunoglobulin. Which of the following is the most likely diagnosis?
A 70-year-old man is accompanied by his wife to the primary care clinic for hand tremors. He states that he first noticed the tremor of his left hand 1 year ago. Since then, the tremor has been worsening and now he can hardly relax when trying to read. His wife says that she is also worried about his memory. She had to take over the finances several weeks ago after learning that he had forgotten to pay the bills for the past few months. The patient’s medical history is significant for hypertension. He takes aspirin and amlodipine. His mother had schizophrenia. The patient drinks 1-2 beers a night and is a former cigar smoker. On physical examination, he speaks softly and has reduced facial expressions. He has a resting tremor that is worse on the left, and he resists manipulation of his bilateral upper extremities. Which of the following is the most likely diagnosis?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
