Cardiology — MCQs

On this page
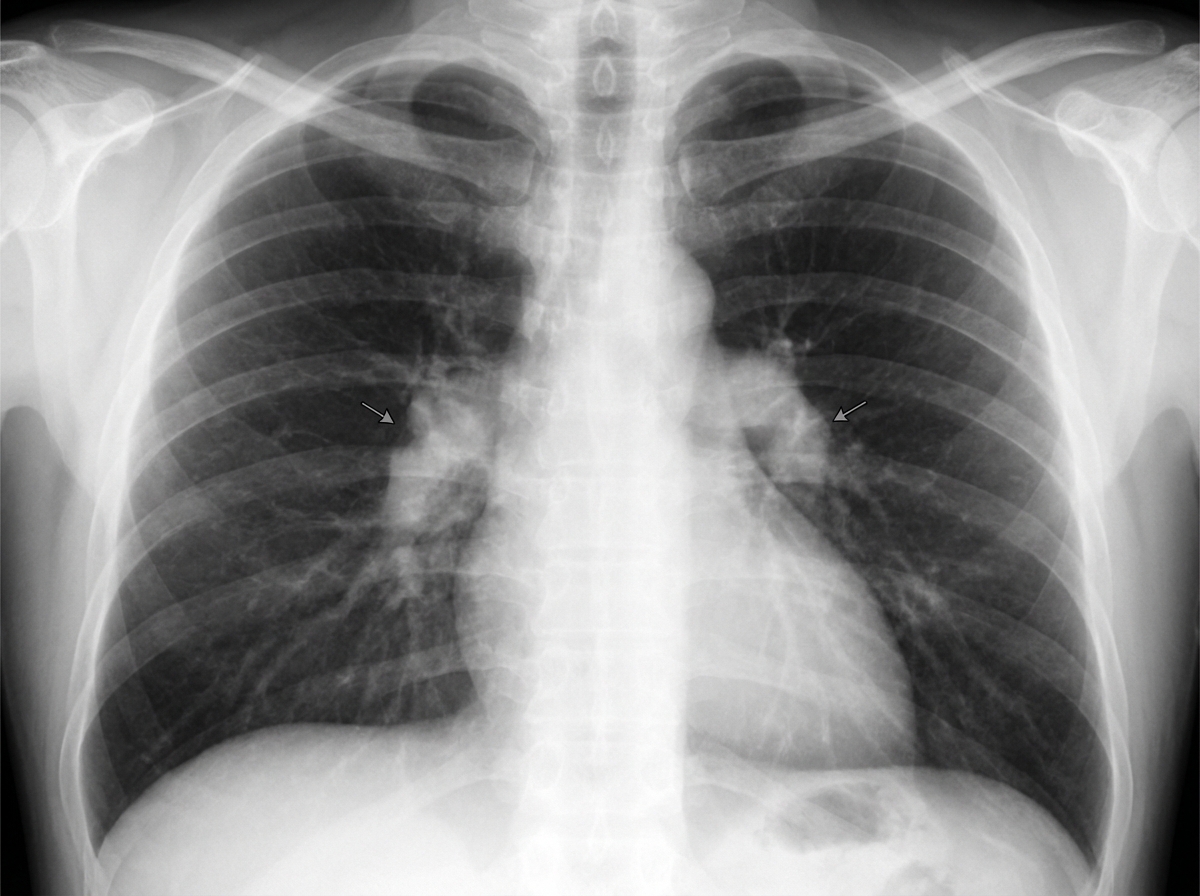
A 30-year-old African-American woman comes to the physician for a routine checkup. She feels well. She has a history of type 2 diabetes mellitus that is well-controlled with metformin. Her mother died of a progressive lung disease at the age of 50 years. The patient is sexually active with her husband, and they use condoms consistently. She has smoked one pack of cigarettes daily for the past 10 years. She drinks one to two glasses of wine per day. She does not use illicit drugs. Vital signs are within normal limits. Examination, including ophthalmologic evaluation, shows no abnormalities. Laboratory studies, including serum creatinine and calcium concentrations, are within normal limits. An ECG shows no abnormalities. A tuberculin skin test is negative. A chest x-ray is shown. Which of the following is the most appropriate next step in management?
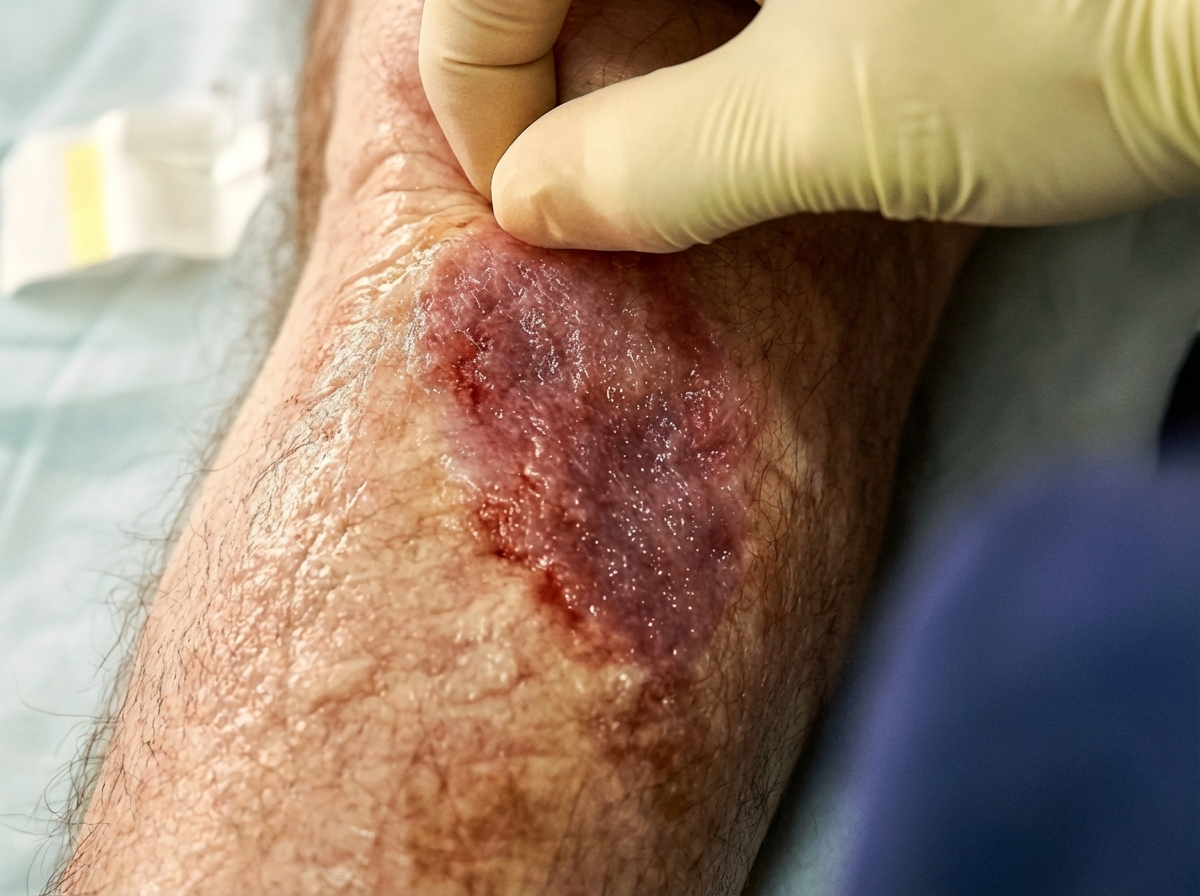
A 67-year-old woman presents with right leg pain and swelling of 5 days’ duration. She has a history of hypertension for 15 years and had a recent hospitalization for pneumonia. She had been recuperating at home but on beginning to mobilize and walk, the right leg became painful and swollen. Her temperature is 37.1°C (98.7°F), the blood pressure is 130/80 mm Hg, and the pulse is 75/min. On physical examination, the right calf is 4 cm greater in circumference than the left when measured 10 cm below the tibial tuberosity. Dilated superficial veins are present on the right foot and the right leg is slightly redder than the left. There is some tenderness on palpation in the popliteal fossa behind the knee. Which of the following is the best initial step in the management of this patient’s condition?
A 67-year-old man presents to his primary care provider because of fatigue and loss of appetite. He is also concerned that his legs are swollen below the knee. He has had type 2 diabetes for 35 years, for which he takes metformin and glyburide. Today his temperature is 36.5°C (97.7°F), the blood pressure is 165/82 mm Hg, and the pulse is 88/min. Presence of which of the following would make diabetic kidney disease less likely in this patient?
A 97-year-old man visits the urology clinic 5 days after experiencing urinary retention at an emergency department visit. The patient has a history of hypertension, type II diabetes mellitus, stroke, dyslipidemia, a past myocardial infarction, and severe osteoarthritis in his right hip. He is not compliant with his medications and his multiple comorbidities are poorly managed. In the hospital, the patient’s urinary retention was treated with Foley catheterization. At clinic, the patient’s serum-specific prostate-specific antigen (PSA) is 6.0 ng/mL (normal is < 4 ng/mL). Digital rectal examination (DRE) demonstrates a nontender prostate with several rock hard nodules. The patient's Foley is removed and he is able to urinate on his own. Which is the most appropriate next step in management?
A 72-year-old man presents to his primary care physician because he feels like his vision has been changing over the last 6 months. In particular, he feels that he cannot see as well out of his right eye as previously. His past medical history is significant for myocardial infarction as well as Lyme disease. On presentation, he is found to have a droopy right eyelid as well as persistent constriction of his right pupil. Additionally, the skin on his right half of his face is found to be cracked and dry. Which of the following is most likely associated with this patient's symptoms?
A 27-year-old woman presents with a history of repeated episodes of discoloration of the fingers over the last 3 years. She mentions that the episodes are usually triggered by exposure to cold, which leads to a sequential white, blue, and red discoloration of her fingers, followed by resolution of the symptoms. During an episode, she experiences pain and numbness in the affected fingers. The episodes are usually of short duration and do not interfere with her life, so she did not seek medical advice till now. Which of the following additional clinical features in this patient would most likely support the most likely diagnosis?
A 80-year-old man is brought to the emergency department with complaints that he "can't control his left leg". His symptoms started a few hours ago. He was outside taking a walk with his wife when suddenly his leg shot out and kicked her. His past medical history is notable for diabetes, hypertension, and a myocardial infarction 5 years ago. He smokes 1-2 cigarettes/day. He does not use alcohol or illicit drugs. On exam, the patient has intermittent wide, flinging movements that affect his proximal left arm and left leg. Which of the following parts of his brain is most likely damaged?
A 61-year-old man comes to the physician because of a 3-month history of worsening exertional dyspnea and a persistent dry cough. For 37 years he has worked in a naval shipyard. He has smoked 1 pack of cigarettes daily for the past 40 years. Pulmonary examination shows fine bibasilar end-expiratory crackles. An x-ray of the chest shows diffuse bilateral infiltrates predominantly in the lower lobes and pleural reticulonodular opacities. A CT scan of the chest shows pleural plaques and subpleural linear opacities. The patient is most likely to develop which of the following conditions?
A 56-year-old woman presents to the emergency department with a 1-hour history of persistent nasal bleeding. The bleeding started spontaneously. The patient experienced a similar episode last year. Currently, she has hypertension and takes hydrochlorothiazide and losartan. She is anxious. Her blood pressure is 175/88 mm Hg. During the examination, the patient holds a blood-stained gauze against her right nostril. Upon removal of the gauze, blood slowly drips down from her right nostril. Examination of the left nostril reveals no abnormalities. Squeezing the nostrils for 20 minutes fails to control bleeding. Which of the following interventions is the most appropriate next step in the management of this patient?
A 57-year-old man presents with a large wound on his right lower leg that has been present for 6 months as shown in the picture. He has had chronically swollen legs for over 10 years. His mother and brother had similar problems with their legs. He had a documented deep vein thrombosis (DVT) in the affected leg 5 years earlier, but has no other past medical history. He has a blood pressure of 126/84 and heart rate of 62/min. Which of the following is the most likely diagnosis?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
