Cardiology — MCQs

On this page
A 58-year-old man presents to the emergency department with severe chest pain and uneasiness. He says that symptoms onset acutely half an hour ago while he was watching television. He describes the pain as being 8/10 in intensity, sharp in character, localized to the center of the chest and retrosternal, and radiating to the back and shoulders. The patient denies any associated change in the pain with breathing or body position. He says he has associated nausea but denies any vomiting. He denies any recent history of fever, chills, or chronic cough. His past medical history is significant for hypertension, hyperlipidemia, and diabetes mellitus for which he takes lisinopril, hydrochlorothiazide, simvastatin, and metformin. He reports a 30-pack-year smoking history and has 1–2 alcoholic drinks during the weekend. Family history is significant for hypertension, hyperlipidemia, and an ST elevation myocardial infarction in his father and paternal uncle. His blood pressure is 220/110 mm Hg in the right arm and 180/100 mm Hg in the left arm. On physical examination, the patient is diaphoretic. Cardiac exam reveals a grade 2/6 diastolic decrescendo murmur loudest over the left sternal border. Remainder of the physical examination is normal. The chest radiograph shows a widened mediastinum. The electrocardiogram (ECG) reveals non-specific ST segment and T wave changes. Intravenous morphine and beta-blockers are started. Which of the following is the most likely diagnosis in this patient?
A 21-year-old man comes to the physician's office due to a 3-week history of fatigue and a rash, along with the recent development of joint pain that has moved from his knee to his elbows. The patient reports going camping last month but denies having been bitten by a tick. His past medical history is significant for asthma treated with an albuterol inhaler. His pulse is 54/min and blood pressure is 110/72. Physical examination reveals multiple circular red rings with central clearings on the right arm and chest. There is a normal range of motion in all joints and 5/5 strength bilaterally in the upper and lower extremities. Without proper treatment, the patient is at highest risk for which of the following complications?
A 28-year-old man presents to his primary care provider because of shortness of breath, cough, and wheezing. He reports that in high school, he occasionally had shortness of breath and would wheeze after running. His symptoms have progressively worsened over the past 6 months and are now occurring daily. He also finds himself being woken up from sleep by his wheeze approximately 3 times a week. His medical history is unremarkable. He denies tobacco use or excessive alcohol consumption. His temperature is 37.1°C (98.8°F), blood pressure is 121/82 mm Hg, and heart rate is 82/min. Physical examination is remarkable for expiratory wheezing bilaterally. Spirometry shows an FEV1 of 73% of predicted, which improves by 19% with albuterol. In addition to a short-acting beta-agonist as needed, which of the following is the most appropriate therapy for this patient?
A 37-year-old man is presented to the emergency department by paramedics after being involved in a serious 3-car collision on an interstate highway while he was driving his motorcycle. On physical examination, he is responsive only to painful stimuli and his pupils are not reactive to light. His upper extremities are involuntarily flexed with hands clenched into fists. The vital signs include temperature 36.1°C (97.0°F), blood pressure 80/60 mm Hg, and pulse 102/min. A non-contrast computed tomography (CT) scan of the head shows a massive intracerebral hemorrhage with a midline shift. Arterial blood gas (ABG) analysis shows partial pressure of carbon dioxide in arterial blood (PaCO2) of 68 mm Hg, and the patient is put on mechanical ventilation. His condition continues to decline while in the emergency department and it is suspected that this patient is brain dead. Which of the following results can be used to confirm brain death and legally remove this patient from the ventilator?
A 65-year-old man comes to the physician because of a 10-month history of crampy left lower extremity pain that is exacerbated by walking and relieved by rest. The pain is especially severe when he walks on an incline. He has a 20-year history of type 2 diabetes mellitus, for which he takes metformin. He has smoked 1 pack of cigarettes daily for 40 years. His blood pressure is 140/92 mm Hg. Physical examination shows dry and hairless skin over the left foot. Which of the following is the most likely underlying cause of this patient's symptoms?
A 51-year-old woman with a history of palpitations is being evaluated by a surgeon for epigastric pain. It is discovered that she has an epigastric hernia that needs repair. During her preoperative evaluation, she is ordered to receive lab testing, an electrocardiogram (ECG), and a chest X-ray. These screening studies are unremarkable except for her chest X-ray, which shows a 2 cm isolated pulmonary nodule in the middle lobe of the right lung. The nodule has poorly defined margins, and it shows a dense, irregular pattern of calcification. The patient is immediately referred to a pulmonologist for evaluation of the lesion. The patient denies any recent illnesses and states that she has not traveled outside of the country since she was a child. She has had no sick contacts or respiratory symptoms, and she does not currently take any medications. She does, however, admit to a 20-pack-year history of smoking. Which of the following is the most appropriate next step in evaluating this patient’s diagnosis with regard to the pulmonary nodule?
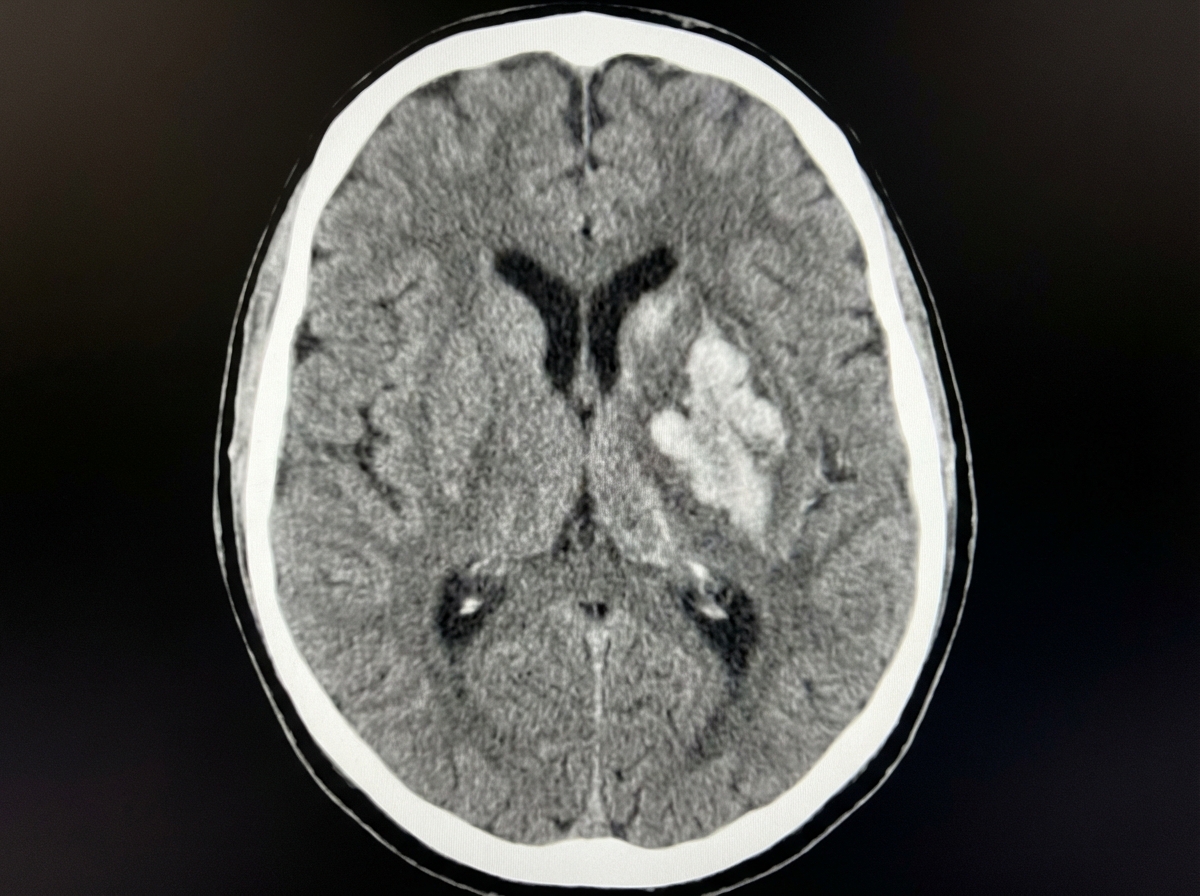
A 68-year-old woman is brought to the emergency department after being found unresponsive in her bedroom in a nursing home facility. Her past medical history is relevant for hypertension, diagnosed 5 years ago, for which she has been prescribed a calcium channel blocker and a thiazide diuretic. Upon admission, she is found with a blood pressure of 200/116 mm Hg, a heart rate of 70/min, a respiratory rate of 15 /min, and a temperature of 36.5°C (97.7°F). Her cardiopulmonary auscultation is unremarkable, except for the identification of a 4th heart sound. Neurological examination reveals the patient is stuporous, with eye-opening response reacting only to pain, no verbal response, and flexion withdrawal to pain. Both pupils are symmetric, with the sluggish pupillary response to light. A noncontrast CT of the head is performed and is shown in the image. Which of the following is the most likely etiology of this patient’s condition?
A 51-year-old woman comes to the physician because of a 3-day history of worsening shortness of breath, nonproductive cough, and sharp substernal chest pain. The chest pain worsens on inspiration and on lying down. The patient was diagnosed with breast cancer 2 months ago and was treated with mastectomy followed by adjuvant radiation therapy. She has hypertension and hyperlipidemia. Current medications include tamoxifen, valsartan, and pitavastatin. She has smoked a pack of cigarettes daily for 15 years but quit after being diagnosed with breast cancer. Her pulse is 95/min, respirations are 20/min, and blood pressure is 110/60 mm Hg. Cardiac examination shows a scratching sound best heard at the left lower sternal border. An ECG shows sinus tachycardia and ST segment elevations in leads I, II, avF, and V1–6. Which of the following is the most likely underlying cause of this patient's symptoms?
A 35-year-old African-American female presents to the emergency room complaining of chest pain. She also complains of recent onset arthritis and increased photosensitivity. Physical examination reveals bilateral facial rash. Which of the following is most likely to be observed in this patient?
A 67-year-old man with a 55-pack-year smoking history, diabetes type II, and hyperlipidemia presents to his primary care clinic for an annual exam. He has no complaints. He reports that his blood glucose has been under tight control and that he has not smoked a cigarette for the past 5 months. His temperature is 97.5°F (36.4°C), blood pressure is 182/112 mmHg, pulse is 85/min, respirations are 15/min, and oxygen saturation is 95% on room air. Physical examination is notable for bruits bilaterally just lateral of midline near his umbilicus. The patient is started on anti-hypertensive medications including a beta-blocker, a thiazide diuretic, and a calcium channel blocker. He returns 1 month later with no change in his blood pressure. Which of the following is the best next step in management?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
