Cardiology — MCQs

On this page
A 58-year-old man comes to the physician because of intermittent throbbing headaches over the past year. The headaches are worse when he wakes up and are not accompanied by other symptoms. The patient also reports trouble concentrating on daily tasks at work. His wife has been complaining lately about his snoring during sleep, which he attributes to his chronic sinusitis. He has a history of hypertension and an allergy to dust mites. He has smoked a pack of cigarettes daily for 14 years. His pulse is 72/min and blood pressure is 150/95 mm Hg. He is 178 cm (5 ft 10 in) tall and weighs 120 kg (265 lb); BMI is 37.9 kg/m2. Neurological and cutaneous examination shows no abnormalities. Which of the following is the most likely cause of this patient's hypertension?
A 27-year-old man with a past medical history of type I diabetes mellitus presents to the emergency department with altered mental status. The patient was noted as becoming more lethargic and confused over the past day, prompting his roommates to bring him in. His temperature is 99.0°F (37.2°C), blood pressure is 107/68 mmHg, pulse is 120/min, respirations are 17/min, and oxygen saturation is 98% on room air. Laboratory values are ordered as seen below. Serum: Na+: 144 mEq/L Cl-: 100 mEq/L K+: 6.3 mEq/L HCO3-: 16 mEq/L BUN: 20 mg/dL Glucose: 599 mg/dL Creatinine: 1.4 mg/dL Ca2+: 10.2 mg/dL Which of the following is the appropriate endpoint of treatment for this patient?
A 70-year-old man with a 2 year history of Alzheimer disease is brought in from his nursing facility with altered mental status and recurrent falls during the past few days. Current medications include donepezil and galantamine. His vital signs are as follows: temperature 36.0°C (96.8°F), blood pressure 90/60 mm Hg, heart rate 102/min, respiratory rate 22/min. Physical examination reveals several lacerations on his head and extremities. He is oriented only to the person. Urine and blood cultures are positive for E. coli. The patient is admitted and initial treatment with IV fluids, antibiotics, and subcutaneous prophylactic heparin. On the second day of hospitalization, diffuse bleeding from venipuncture sites and wounds is observed. His blood test results show thrombocytopenia, prolonged PT and PTT, and a positive D-dimer. Which of the following is the most appropriate next step in the management of this patient's condition?
A 69-year-old male presents to the emergency department for slurred speech and an inability to use his right arm which occurred while he was eating dinner. The patient arrived at the emergency department within one hour. A CT scan was performed of the head and did not reveal any signs of hemorrhage. The patient is given thrombolytics and is then managed on the neurology floor. Three days later, the patient is recovering and is stable. He seems depressed but is doing well with his symptoms gradually improving as compared to his initial presentation. The patient complains of neck pain that has worsened slowly over the past few days for which he is being given ibuprofen. Laboratory values are ordered and return as indicated below: Serum: Na+: 130 mEq/L K+: 3.7 mEq/L Cl-: 100 mEq/L HCO3-: 24 mEq/L Urea nitrogen: 7 mg/dL Glucose: 70 mg/dL Creatinine: 0.9 mg/dL Ca2+: 9.7 mg/dL Urine: Appearance: dark Glucose: negative WBC: 0/hpf Bacterial: none Na+: 320 mEq/L/24 hours His temperature is 99.5°F (37.5°C), pulse is 95/min, blood pressure is 129/70 mmHg, respirations are 10/min, and oxygen saturation is 98% on room air. Which of the following is the best next step in management?
A 57-year-old man presents for his yearly wellness visit. He says he has been feeling well and has no complaints. No significant past medical history or current medications. The patient reports a 35-pack-year smoking history but says he quit 5 years ago. His family history is significant for lung cancer in his father who died at age 67. His vital signs include: temperature 36.8°C (98.2°F), pulse 95/min, respiratory rate 16/min, blood pressure 100/75 mm Hg. Physical examination is unremarkable. Laboratory findings are significant for the following: Serum potassium 3.9 mEq/L Serum sodium 140 mEq/L Serum chloride 103 mEq/L Serum calcium 2.5 mmol/L BUN 15 mg/dL Creatinine 0.8 mg/dL Glucose 95 mg/dL Magnesium 1.7 mEq/L Phosphate 1.1 mmol/L Hemoglobin 14 g/dL Bicarbonate (HCO3-) 25 mEq/L Bilirubin, total 0.9 mg/dL Bilirubin, indirect 0.4 mg/dL AST 10 U/L ALT 19 U/L Alkaline phosphatase 40 U/L Albumin 3.6 g/dL Which of the following preventative screening tests is recommended for this patient at this time?
A 37-year-old male presents to your clinic with shortness of breath and lower extremity edema. He was born in Southeast Asia and emigrated to America ten years prior. Examination demonstrates 2+ pitting edema to the level of his knees, ascites, and bibasilar crackles, as well as an opening snap followed by a mid-to-late diastolic murmur. The patient undergoes a right heart catheterization that demonstrates a pulmonary capillary wedge pressure (PCWP) of 24 mmHg. The patient is most likely to have which of the following?
A 75-year-old woman presents to the emergency department because of a brief loss of consciousness, slurred speech, and facial numbness. Family members report that she complained about feeling chest pain and shortness of breath while on her morning walk. Medical history is noncontributory. Physical examination shows decreased pupil reactivity to light and hemiplegic gait. Her pulse is 120/min, respirations are 26/min, temperature is 36.7°C (98.0°F), and blood pressure is 160/80 mm Hg. On heart auscultation, S1 is loud, widely split, and there is a diastolic murmur. Transthoracic echocardiography in a 4-chamber apical view revealed a large oval-shaped and sessile left atrial mass. Which of the following is the most likely complication of this patient's condition?
A 51-year-old woman comes to the physician because of numbness of her legs and toes for 3 months. She has also had fatigue and occasional shortness of breath for the past 5 months. She is a painter. Examination shows pale conjunctivae. Sensation to vibration and position is absent over the lower extremities. She has a broad-based gait. The patient sways when she stands with her feet together and closes her eyes. Which of the following laboratory findings is most likely to be seen in this patient?
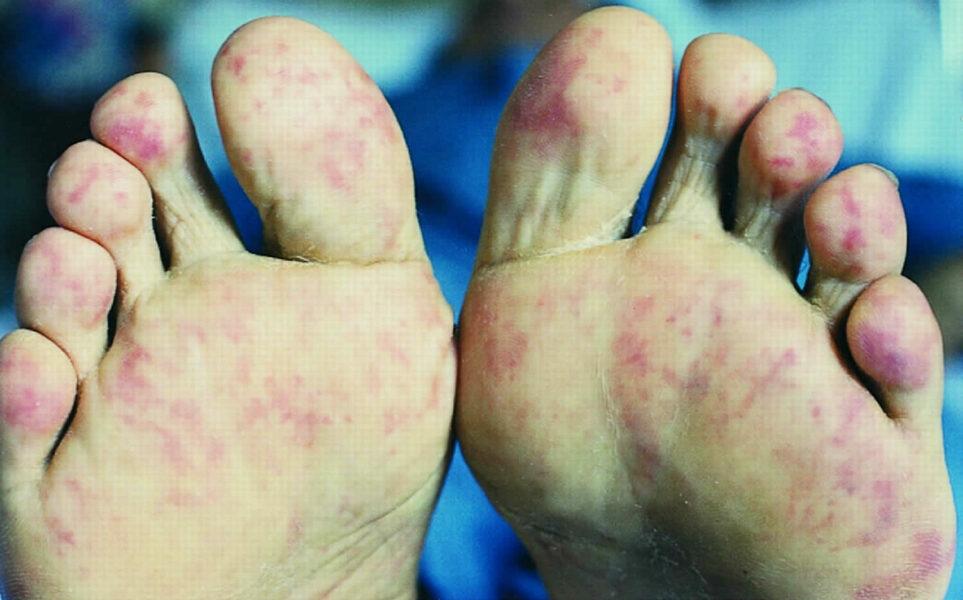
Two days after undergoing emergency cardiac catherization for myocardial infarction, a 68-year-old woman has pain in her toes. During the intervention, she was found to have an occluded left anterior descending artery and 3 stents were placed. She has hypertension, hypercholesterolemia, and coronary artery disease. Prior to admission, her medications were metoprolol, enalapril, atorvastatin, and aspirin. Her temperature is 37.3°C (99.1°F), pulse is 93/min, and blood pressure is 115/78 mm Hg. Examination shows discoloration of the toes of both feet. A photograph of the right foot is shown. The lesions are cool and tender to palpation. The rest of the skin on the feet is warm; femoral and pedal pulses are palpable bilaterally. This patient is at increased risk for which of the following conditions?
A 60-year-old woman presents to the clinic with a 3-month history of shortness of breath that worsens on exertion. She also complains of chronic cough that has lasted for 10 years. Her symptoms are worsened even with light activities like climbing up a flight of stairs. She denies any weight loss, lightheadedness, or fever. Her medical history is significant for hypertension, for which she takes amlodipine daily. She has a 70-pack-year history of cigarette smoking and drinks 3–4 alcoholic beverages per week. Her blood pressure today is 128/84 mm Hg. A chest X-ray shows flattening of the diaphragm bilaterally. Physical examination is notable for coarse wheezing bilaterally. Which of the following is likely to be seen with pulmonary function testing?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
