Cardiology — MCQs

On this page
A 33-year-old woman presents to the emergency department with weakness. She states that at the end of the day she feels so fatigued and weak that she can hardly care for herself. She currently feels this way. The patient has had multiple illnesses recently and has been traveling, hiking, and camping. Her temperature is 98.0°F (36.7°C), blood pressure is 124/84 mmHg, pulse is 82/min, respirations are 12/min, and oxygen saturation is 98% on room air. Physical exam is notable for 2/5 strength of the upper extremities and 4/5 strength of the lower extremities. Visual exam is notable for mild diplopia. Which of the following is the most likely diagnosis?
A 32-year-old male presents for a new patient visit. He states that he is in good health but has had decreasing exercise tolerance and increased levels of shortness of breath over the past 5 years. He believed that it was due to aging; he has not seen a doctor in 10 years. On auscultation, you note an early diastolic decrescendo blowing murmur that radiates along the left sternal border. In the United States, what is the most likely cause of this patient's condition?
A 45 year-old gentleman presents to his primary care physician complaining of wrist pain and is diagnosed with carpal tunnel syndrome. Upon further questioning, the patient admits that he has recently been outgrowing his gloves and shoes and has had to purchase a new hat as well due to increased head size. Upon exam, he is found to have new mild hypertension and on basic labs he is found to be hyperglycemic. Which of the following is the best blood test to diagnose his suspected disorder?
A 59-year-old male with a history of hypertension presents with chest pain and hoarseness. Patient reports that his hoarseness onset gradually approximately 2 weeks ago and has steadily worsened. He states that approximately 2 hours ago he had sudden onset chest pain which has not improved. The patient describes the chest pain as severe, sharp in character, localized to the midline and radiating to the back. Past medical history is significant for hypertension diagnosed 10 years previously, which was being managed medically, although patient admits he stopped taking his medication and has not been to his doctor in the last couple of years. No current medications. Patient admits to a 20-pack-year smoking history. Vital signs are temperature 37 °C (98.6 °F), blood pressure 169/100 mm Hg, pulse 85/min, respiration rate 19/min, and oxygen saturation 98% on room air. On physical exam, patient is diaphoretic and in distress. Cardiac exam is significant for an early diastolic murmur. Lungs are clear to auscultation. Remainder of physical exam is normal. While performing the exam, the patient suddenly grips his chest and has a syncopal episode. He cannot be roused. Repeat vital signs show blood pressure 85/50 mm Hg, pulse 145/min, respiration rate 25/min, and oxygen saturation 92% on room air. Extremities are pale and cool. Patient is intubated. High flow supplemental oxygen and aggressive fluid resuscitation are initiated. Type and crossmatch are ordered. Which of the following is the next best step in management?
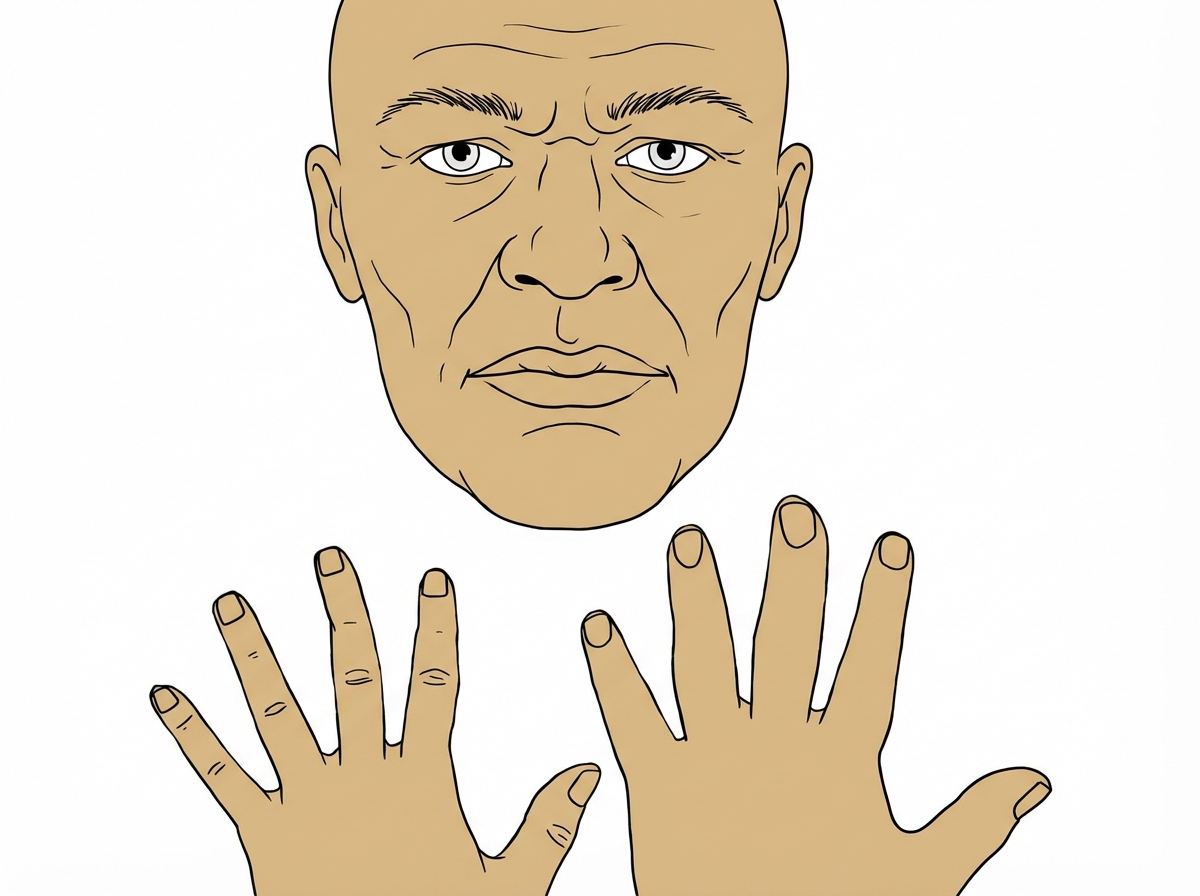
A 43-year-old man visits his physician’s office for a routine check-up. He tells his physician that he is otherwise healthy, except for persistent headaches that he gets every morning. Upon further questioning, he reveals that he has been changing glove sizes quite frequently over the past couple of years. His wedding ring doesn’t fit him anymore. He thought this was probably due to some extra weight that he has put on. Vital signs include: blood pressure 160/90 mm Hg, heart rate 82/min, and respiratory rate 21/min. His current physical appearance is cataloged in the image. His past medical history is significant for diabetes for which he has been receiving treatment for the past 2 years. Which of the following organs most likely has a structural abnormality that has resulted in this patient’s current presentation?
A 41-year-old man presents to a New Mexico emergency department with a 12 hour history of shortness of breath and a nonproductive cough. He says that last week he experienced fevers, chills, fatigue, and myalgias but assumed that he simply had a cold. The symptoms went away after 3 days and he felt fine for several days afterward until he started experiencing shortness of breath even at rest. He works as an exterminator and recently had a job in a rodent infested home. Physical exam reveals a thin, tachypneic man with diffuse rales bilaterally. The most likely cause of this patient's symptoms is associated with which of the following?
A 51-year-old woman is brought to the emergency department because of an aggressive cough with copious amounts of thick, foamy, yellow-green sputum. She says she has had this cough for about 11 years with exacerbations similar to her presentation today. She also reports that her cough is worse in the morning. She was evaluated multiple times in the past because of recurrent bouts of bronchitis that have required treatment with antibiotics. She is a non-smoker. On physical examination, the blood pressure is 125/78 mm Hg, pulse rate is 80/min, respiratory rate is 16/min, and temperature is 36.7°C (98.0°F). Chest auscultation reveals crackles and wheezing over the right middle lobe and the rest of her physical examinations are normal. The chest X-ray shows irregular opacities in the right middle lobe and diffuse airway thickening. Based on this history and physical examination, which of the following is the most likely diagnosis?
A 44-year-old woman with recurrent urinary tract infections is brought to the emergency department by ambulance after sudden onset of severe headache 30 minutes ago. She has a history of occasional, mild headaches in the morning. There is no other history of serious illness. Both her father and her paternal grandmother died of chronic kidney disease. Her temperature is 37.2°C (99.1°F) and blood pressure is 145/90 mm Hg. Physical examination shows neck stiffness. When her hip is flexed, she is unable to fully extend her knee because of pain. Lumbar puncture performed 12 hours after headache onset yields 10 mL of yellow-colored fluid with no leukocytes. Which of the following is the most likely predisposing factor for this patient's current condition?
A 72-year-old man presents to the emergency department because of difficulty breathing and sharp chest pain. The chest pain increases in intensity with lying down, and it radiates to the scapular ridge. Approximately 3 weeks ago, he had an anterior ST-elevation myocardial infarction, which was treated with intravenous alteplase. He was discharged home in a stable condition. Current vital signs include a temperature of 38.1 (100.5°F), blood pressure of 131/91 mm Hg, and pulse of 99/min. On examination, heart sounds are distant and a scratching sound is heard on the left sternal border. ECG reveals widespread concave ST elevations in the precordial leads and PR depressions in leads V2-V6. Which of the following is the most likely cause of this patient condition?
A 20-year-old man comes to the emergency room because of palpitations and mild dyspnea for the last 2 hours. He has had similar episodes in the past that resolved within 20 minutes, but they have been worsening since he started training for his first marathon 1 month ago. Ten years ago, he was treated for streptococcal pharyngitis with a 10-day course of penicillin. His maternal uncle passed away unexpectedly from a heart condition at age 40. He is 180 cm (5 ft 11 in) tall and weighs 85 kg (187 lb); BMI is 26.2 kg/m2. His temperature is 36.5°C (97.7°F), pulse is 70/min, respirations are 18/min, and blood pressure is 132/60 mm Hg. On examination, there is a decrescendo early diastolic murmur heard best along the left sternal border. His head slightly bobs about every second. The remainder of the examination shows no abnormalities. Which of the following is most likely to be present?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
