Cardiology — MCQs

On this page
A 53-year-old woman comes to the physician because of a 3-year history of increasing weakness of her extremities and neck pain that is worse on coughing or sneezing. She first noticed weakness of her right upper extremity 3 years ago, which progressed to her right lower extremity 2 years ago, her left lower extremity 1 year ago, and her left upper extremity 6 months ago. She has had difficulty swallowing and speaking for the past 5 months. Vital signs are within normal limits. Examination shows an ataxic gait. Speech is dysarthritic. Muscular examination shows spasticity and muscle strength is decreased in all extremities. There is bilateral atrophy of the sternocleidomastoid and trapezius muscles. Deep tendon reflexes are 4+ bilaterally. Plantar response shows an extensor response bilaterally. Sensation is decreased below the C5 dermatome bilaterally. Which of the following is the most likely cause of this patient's symptoms?
A 40-year-old woman comes to the emergency department because of difficulty walking for the past 4 hours. She first noticed her symptoms after getting up this morning and her foot dragging while walking. She feels tired. She has a history of chronic sinusitis. Six months ago, she was diagnosed with asthma. Current medications include an albuterol inhaler and inhaled corticosteroids. Her temperature is 38.9°C (102°F), pulse is 80/min, and her blood pressure is 140/90 mm Hg. Auscultation of her lungs shows diffuse wheezing over bilateral lung fields. Physical examination shows tender subcutaneous nodules on the extensor surfaces of the elbows. There are palpable, non-blanching erythematous lesions on both shins. Dorsiflexion of the right foot is impaired. Sensation to pinprick, light touch, and vibration is decreased over the ulnar aspect of the left forearm. Laboratory studies show: Hemoglobin 11.3 g/dL Leukocyte count 24,500 Segmented neutrophils 48% Eosinophils 29% Lymphocytes 19% Monocytes 4% Platelet count 290,000/mm3 Serum Urea nitrogen 32 mg/dL Creatinine 1.85 mg/dL Urine Blood 2+ Protein 3+ Which of the following is the most likely diagnosis in this patient?
A 67-year-old woman presents with her husband because of left leg pain and swelling of 3 days' duration. She has a history of type 2 diabetes mellitus and recent hospitalization for congestive heart failure exacerbation. On physical examination, the left calf is 4 cm greater in circumference than the right. Pitting edema is present on the left leg and there are superficial dilated veins. Venous duplex ultrasound shows an inability to fully compress the lumen of the profunda femoris vein. Which of the following is the most likely diagnosis?
A 16-year-old woman presents to the emergency department for evaluation of acute vomiting and abdominal pain. Onset was roughly 3 hours ago while she was sleeping. She has no known past medical history. Her family history is positive for hypothyroidism and diabetes mellitus in her maternal grandmother. On examination, she is found to have fruity breath and poor skin turgor. She appears fatigued and her consciousness is slightly altered. Laboratory results show a blood glucose level of 691 mg/dL, sodium of 125 mg/dL, and elevated serum ketones. Of the following, which is the next best step in patient management?
A 13-year-old boy is brought to the physician because of bleeding from his lips earlier that day. He has a history of recurrent nosebleeds since childhood. His father has a similar history of recurrent nosebleeds. He is at the 60th percentile for height and weight. Examination shows multiple, small dilated capillaries over the lips, nose, and fingers. The remainder of the examination shows no abnormalities. Which of the following conditions is this patient at increased risk for?
A 29-year-old man presents to the emergency department with chest pain and fatigue for the past week. The patient is homeless and his medical history is not known. His temperature is 103°F (39.4°C), blood pressure is 97/58 mmHg, pulse is 140/min, respirations are 25/min, and oxygen saturation is 95% on room air. Physical exam is notable for scars in the antecubital fossa and a murmur over the left sternal border. The patient is admitted to the intensive care unit and is treated appropriately. On day 3 of his hospital stay, the patient presents with right-sided weakness in his arm and leg and dysarthric speech. Which of the following is the most likely etiology of his current symptoms?
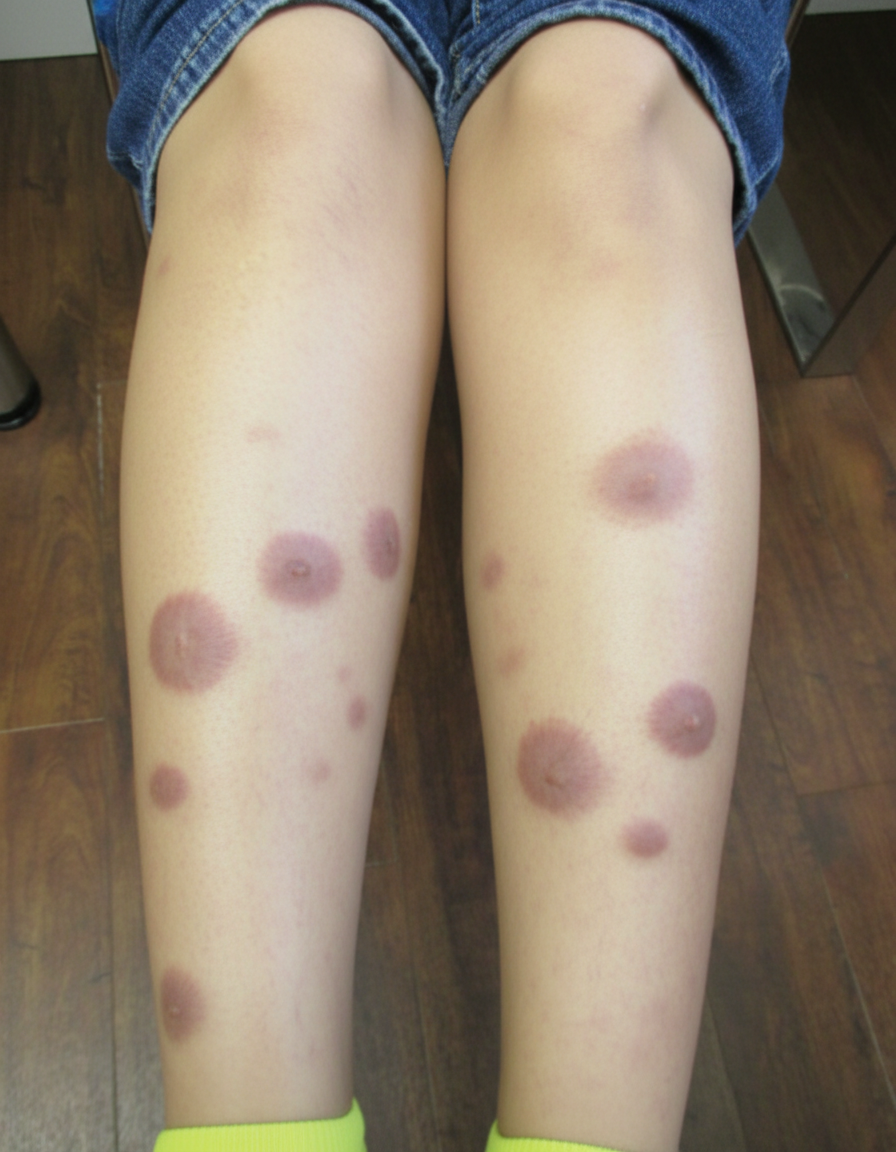
An otherwise healthy 28-year-old woman comes to the physician because of a 14-day history of painful red nodules on her legs associated with malaise and mild joint pains. She reports that the nodules were initially smaller and distinct but some have fused together over the past 3–4 days and now appear like bruises. There is no preceding history of fever, trauma, or insect bites. Her vital signs are within normal limits. A photograph of the tender lesions on her shins is shown. The remainder of the examination shows no abnormalities. Complete blood count and antistreptolysin O (ASO) titers are within the reference range. Erythrocyte sedimentation rate is 30 mm/h. Which of the following is the most appropriate next step in management ?
A 63-year-old man presents to the clinic with fever accompanied by shortness of breath. The symptoms developed a week ago and have been progressively worsening over the last 2 days. He reports his cough is productive of thick, yellow sputum. He was diagnosed with chronic obstructive pulmonary disease 3 years ago and has been on treatment ever since. He quit smoking 10 years ago but occasionally experiences shortness of breath along with chest tightness that improves with the use of an inhaler. However, this time the symptoms seem to be more severe and unrelenting. His temperature is 38.6°C (101.4°F), the respirations are 21/min, the blood pressure is 100/60 mm Hg, and the pulse is 105/min. Auscultation reveals bilateral crackles and expiratory wheezes. His oxygen saturation is 95% on room air. According to this patient’s history, which of the following should be the next step in the management of this patient?
Please refer to the summary above to answer this question Which of the following is the most likely diagnosis? Patient Information Age: 66 years Gender: M, self-identified Ethnicity: African-American Site of Care: office History Reason for Visit/Chief Concern: "I need to go to the bathroom all the time." History of Present Illness: 1-year history of frequent urination urinates every 2–3 hours during the day and wakes up at least 3 times at night to urinate has had 2 episodes of cystitis treated with antibiotics in the past 4 months has a weak urinary stream has not noticed any blood in the urine does not have any pain with urination or ejaculatory dysfunction Past Medical History: type 2 diabetes mellitus nephrolithiasis, treated with percutaneous nephrolithotomy essential tremor Medications: metformin, canagliflozin, propranolol Allergies: sulfa drugs Social History: sexually active with his wife; does not use condoms consistently has smoked one pack of cigarettes daily for 50 years drinks one to two glasses of beer weekly Physical Examination Temp Pulse Resp BP O2 Sat Ht Wt BMI 37°C (98.6°F) 72/min 16/min 134/81 mm Hg – 183 cm (6 ft) 105 kg (231 lb) 31 kg/m2 Appearance: no acute distress Pulmonary: clear to auscultation Cardiac: regular rate and rhythm; normal S1, S2; S4 gallop Abdominal: overweight; no tenderness, guarding, masses, bruits, or hepatosplenomegaly Extremities: no joint erythema, edema, or warmth; dorsalis pedis, radial, and femoral pulses intact Genitourinary: no lesions or discharge Rectal: slightly enlarged, smooth, nontender prostate Neurologic: alert and oriented; cranial nerves grossly intact; no focal neurologic deficits
A 53-year-old woman comes to the physician because of intermittent heaviness and paresthesia of the right arm for the past 2 months. She has also had multiple episodes of lightheadedness while painting a mural for the past 2 weeks. During these episodes, she was nauseated and had blurred vision. Her symptoms resolved after she drank some juice. She has hypertension, type 2 diabetes mellitus, and hypercholesterolemia. Current medications include metformin, glipizide, enalapril, and atorvastatin. She appears anxious. Examination shows decreased radial and brachial pulses on the right upper extremity. The skin over the right upper extremity is cooler than the left. Cardiopulmonary examination shows no abnormalities. Neurologic examination shows no focal findings. Which of the following is the most likely underlying cause of this patient's symptoms?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
