Cardiology — MCQs

On this page
A 32-year-old woman presents with a severe headache and neck pain for the past 60 minutes. She says the headache was severe and onset suddenly like a ‘thunderclap’. She reports associated nausea, vomiting, neck pain, and stiffness. She denies any recent head trauma, loss of consciousness, visual disturbances, or focal neurologic deficits. Her past medical history is significant for hypertension, managed with hydrochlorothiazide. She denies any history of smoking, alcohol use, or recreational drug use. The vital signs include: temperature 37.0°C (98.6°F), blood pressure 165/95 mm Hg, pulse 92/min, and respiratory rate 15/min. On physical examination, there is mild nuchal rigidity noted with limited flexion at the neck. An ophthalmic examination of the retina shows mild papilledema. A noncontrast computed tomography (CT) scan of the head is performed and shown in the exhibit (see image). Which of the following is the next best step in the management of this patient?
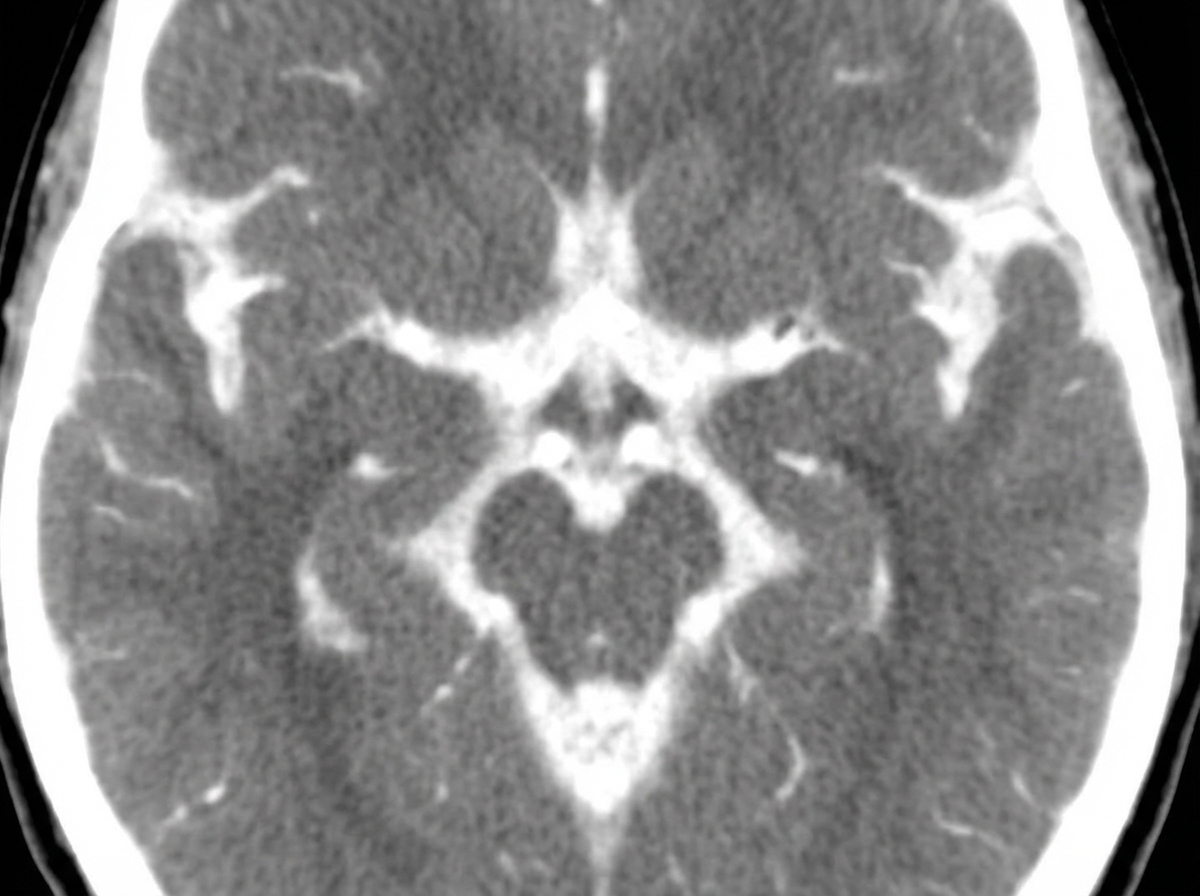
A 58-year-old woman is followed in the nephrology clinic for longstanding chronic kidney disease (CKD) secondary to uncontrolled hypertension. Her glomerular filtration rate (GFR) continues to decline, and she is approaching initiation of hemodialysis. Plans are made to obtain vascular access at the appropriate time, and the patient undergoes the requisite screening to be enrolled as an end stage renal disease (ESRD) patient. Among patients on chronic hemodialysis, which of the following is the most common cause of death?
A 67-year-old man presents with an excruciatingly painful tongue lesion. He says the lesion was preceded by an intermittent headache for the past month that localized unilaterally to the left temple and occasionally radiates to the right eye. The tongue lesion onset acutely and has been present for a few days. The pain is constant. His past medical history is relevant for hypertension and recurrent migraines. Current medications include captopril. On physical examination, multiple knot-like swellings are seen on the left temple. Findings from an inspection of the oral cavity are shown in the exhibit (see image). Laboratory findings are significant for the following: Hemoglobin 12.9 g/dL Hematocrit 40.7% Leukocyte count 5500/mm3 Neutrophils 65% Lymphocytes 30% Monocytes 5% Mean corpuscular volume 88.2 μm3 Platelet count 190,000/mm3 Erythrocyte sedimentation rate 45 mm/h Which of the following is the next best step in the management of this patient?
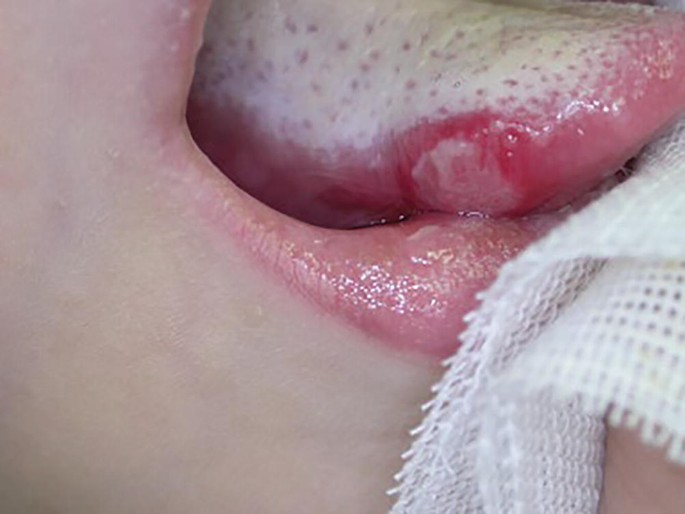
A 67-year-old man presents to his primary care physician for a wellness checkup. The patient states he has been doing well and currently has no concerns. The patient's daughter states that she feels he is abnormally fatigued and has complained of light-headedness whenever he gardens. He also admits that he fainted once. The patient has a past medical history of type II diabetes, hypertension, and constipation. He recently had a "throat cold" that he recovered from with rest and fluids. His temperature is 98.9°F (37.2°C), blood pressure is 167/98 mmHg, pulse is 90/min, respirations are 12/min, and oxygen saturation is 99% on room air. Physical exam reveals a systolic murmur heard best along the right upper sternal border. An ECG is performed and demonstrates no signs of ST elevation. Cardiac troponins are negative. Which of the following is the most likely diagnosis?
A 25-year-old man presents to the emergency department for a fever and abdominal pain. The patient states that his pain has been worsening over the past week in the setting of a fever. He has a past medical history of IV drug abuse and multiple admissions for septic shock. His temperature is 102°F (38.9°C), blood pressure is 94/54 mmHg, pulse is 133/min, respirations are 22/min, and oxygen saturation is 100% on room air. Physical exam is notable for a murmur over the left upper sternal border. Abdominal exam reveals left upper quadrant tenderness. Laboratory values are ordered as seen below. Hemoglobin: 15 g/dL Hematocrit: 44% Leukocyte count: 16,700/mm^3 Platelet count: 299,000/mm^3 Which of the following is the most likely diagnosis?
A 40-year-old woman comes to the physician for a 2-month history of chest pain and heartburn after meals. The patient reports that the pain is worse at night and especially when lying down. She has a history of Raynaud's disease treated with nifedipine. There is no family history of serious illness. She emigrated to the US from Nigeria 5 years ago. She does not smoke or drink alcohol. Vital signs are within normal limits. Cardiopulmonary examination shows no abnormalities. Thickening and hardening of the skin is seen on the hands and face. There are several firm, white nodules on the elbows and fingertips. Further evaluation of this patient is most likely to show which of the following findings?
A 65-year-old woman presents with progressive gait difficulty, neck pain, and bladder incontinence. She also complains of urinary urgency. Past medical history is significant for uncontrolled diabetes mellitus with a previous hemoglobin A1c of 10.8%. Physical examination reveals slightly increased muscle tone in all limbs with brisk tendon reflexes. Sensory examination reveals a decrease of all sensations in a stocking and glove distribution. Her gait is significantly impaired. She walks slowly with small steps and has difficulty turning while walking. She scores 23 out of 30 on a mini-mental state examination (MMSE). A brain MRI reveals dilated ventricles with a callosal angle of 60 degrees and mild cortical atrophy. What is the most appropriate next step in the management of this patient?
A 24-year-old man is running a marathon (42.2 km) on a hot summer day and collapses about halfway through the run. Emergency personnel are called and find him having a seizure. As the seizure subsides, the runner exhibits confusion, dry lips and decreased skin turgor. On the way to the emergency department, he denies taking medication or having a history of seizures. He reports that he drank water, but he admits that it was probably not enough. Which of the following would be the next best step in the management of this patient?
A 55-year-old man comes to the physician because of weight loss and increased urinary frequency for the past month. He has also noticed blood in the urine, usually towards the end of voiding. He emigrated to the U.S. from Kenya 5 years ago. He has smoked one pack of cigarettes daily for 35 years. Physical examination shows a palpable liver edge and splenomegaly. Laboratory studies show a hemoglobin concentration of 9.5 mg/dL and a urine dipstick is strongly positive for blood. A CT scan of the abdomen shows bladder wall thickening and fibrosis. A biopsy specimen of the bladder shows squamous cell carcinoma. Which of the following additional findings is most likely in this patient?
A 40-year-old woman presents with a ‘tingling’ feeling in the toes of both feet that started 5 days ago. She says that the feeling varies in intensity but has been there ever since she recovered from a stomach flu last week. Over the last 2 days, the tingling sensation has started to spread up her legs. She also reports feeling weak in the legs for the past 2 days. Her past medical history is unremarkable, and she currently takes no medications. Which of the following diagnostic tests would most likely be abnormal in this patient?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
