Cardiology — MCQs

On this page
A 60-year-old man presents to the clinic for his annual check-up. The patient says that he has occasional leg cramps, and his legs feel heavy especially after standing for long hours to teach his classes. His past medical history is significant for hypertension which is controlled by metoprolol and lisinopril. He has smoked half a pack of cigarettes daily for the past 30 years. He does not drink alcohol. Family history is significant for myocardial infarction (MI) in his father at the age of 55 years. The blood pressure is 130/80 mm Hg and the pulse rate is 78/min. On physical examination, there are tortuosities of the veins over his lower limb, more pronounced over the left leg. Peripheral pulses are 2+ on all extremities and there are no skin changes. Strength is 5 out of 5 in all extremities bilaterally. Sensation is intact. No pain in the dorsiflexion of the foot. The rest of the examination and the laboratory tests are normal. Which of the following best describes the pathophysiology responsible for this patient’s symptoms?
An 18-year-old man is hospitalized after a suicide attempt, his 6th such attempt in the last 4 years. He was diagnosed with depression 5 years ago, for which he takes fluoxetine. He is currently complaining of severe and worsening left knee swelling and pain since he attempted suicide by jumping out of his second-story bedroom window. He sustained minor injuries at the time, primarily lacerations to his arms and knees, and he was admitted to the hospital’s psychiatric unit. His blood pressure is 110/72 mm Hg, heart rate is 88/min, and temperature is 38°C (100.4°F). On examination, the knee is erythematous and edematous, and it feels warm to the touch. The patient’s lab studies reveal a hemoglobin level of 11.9 g/dL, leukocyte count of 11,200/µL, and a platelet count of 301,000/µL. Arthrocentesis yields 15 mL of fluid with a leukocyte count of 61,000/µL, 93% neutrophils, and an absence of crystals under polarized light microscopy. A gram stain of joint fluid is negative; however, mucosal, blood and synovial fluid cultures are still pending. Which of the following is the most appropriate next step in the management of this patient?
A 40-year-old woman with HIV infection presents to the emergency department because of a 4-week history of progressively worsening fatigue and headache. On mental status examination, the patient is somnolent and oriented only to person. Her CD4+ lymphocyte count is 80/mm3 (N = 500). Analysis of this patient's cerebrospinal fluid (CSF) shows a leukocyte count of 30/mm3 (60% lymphocytes), a protein concentration of 52 mg/dL, and a glucose concentration of 37 mg/dL. An India ink stain of the CSF is shown. Which of the following characteristics would also point towards the most likely cause?
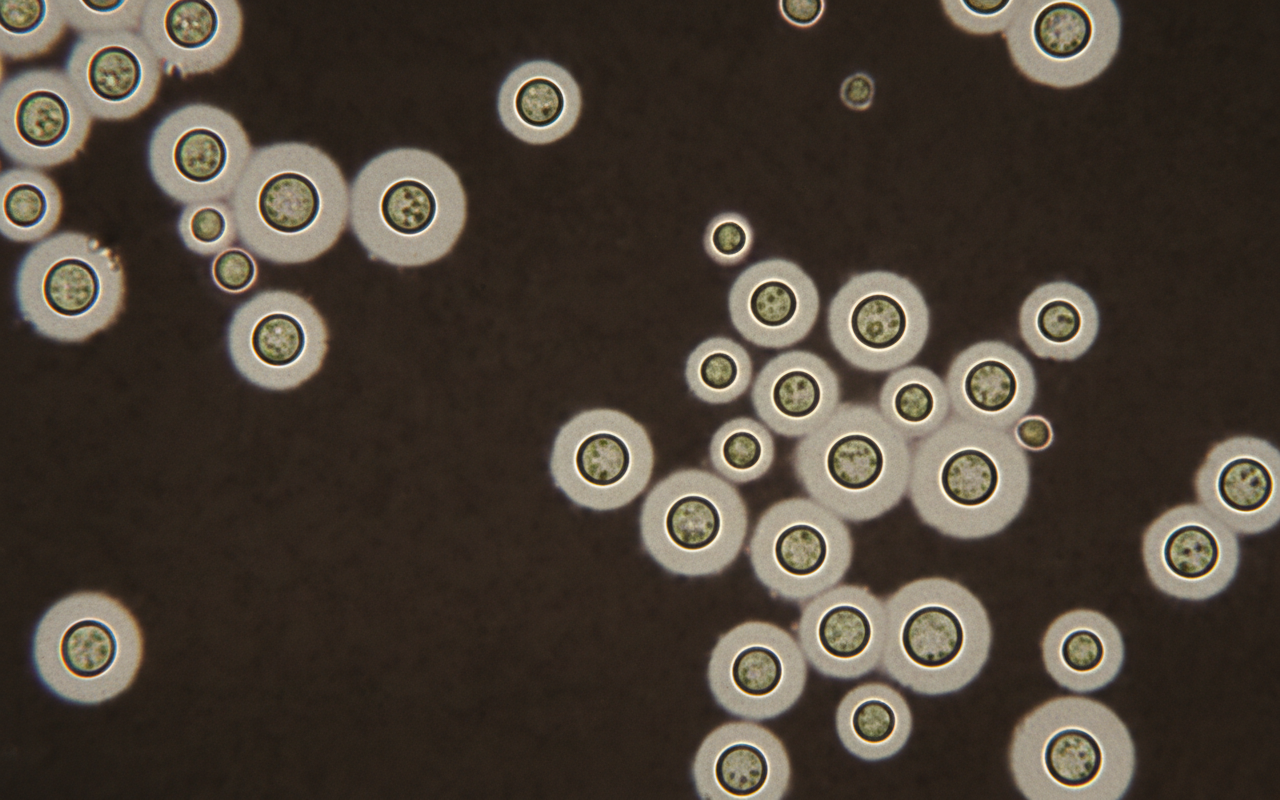
A 45-year-old man presents with 2 weeks of low-grade fever, malaise, night sweats, orthopnea, and shortness of breath. Past medical history is unremarkable. He reports a long-standing history of intravenous drug use for which he has been hospitalized a couple of times in the psychiatry ward. His vital signs upon admission show a blood pressure of 100/80 mm Hg, pulse of 102/min, a respiratory rate of 20/min, and a body temperature of 38.4°C (101.0°F). On cardiac auscultation, there is an S3 gallop and a 3/6 holosystolic murmur heard best along the right sternal border. There are fine rattles present over the lung bases bilaterally. Which of the following tests would be of the greatest diagnostic value in this patient?
A 60-year-old-man presents to his physician with worsening myalgias and new symptoms of early fatigue, muscle weakness, and drooping eyelids. His wife presents with him and states that he never used to have such symptoms. His medical history is significant for gout, hypertension, hypercholesterolemia, diabetes mellitus type II, and pilocytic astrocytoma as a teenager. He denies smoking, drinks a 6-pack of beer per day, and endorses a past history of cocaine use but currently denies any illicit drug use. His vital signs include temperature 36.7°C (98.0°F), blood pressure 126/74 mm Hg, heart rate 87/min, and respiratory rate 15/min. Physical examination shows minimal bibasilar rales, but otherwise clear lungs on auscultation, grade 2/6 holosystolic murmur, 3/5 strength in all extremities, and benign abdominal findings. The Tensilon test result is positive. Which of the following options explains why a chest CT should be ordered for this patient?
A 69-year-old woman is brought to the emergency department by her husband for evaluation of the sudden onset of chest pain and breathlessness 2 hours ago. The pain increases with deep inspiration. She had a total hip replacement 20 days ago. She has hypertension, for which she takes a calcium channel blocker. She has smoked 1 pack of cigarettes daily since adolescence. Her vital signs include a blood pressure of 100/60 mm Hg, pulse of 82/min, and respiratory rate of 30/min. She is cyanotic. Examination of the chest revealed tenderness over the right lower lung with dullness to percussion. A chest CT scan showed a focal, wedged-shaped, pleura-based triangular area of hemorrhage in the right lower lobe of the lung. What is the most probable cause of the pulmonary lesion?
A 9-year-old boy presents with persistent epistaxis. The patient’s mother says that his nosebleed started suddenly 2 hours ago, and has not ceased after more than 20 minutes of applying pressure. She states that he has a history of nosebleeds since he was a toddler, but, in the past, they usually stopped after a few minutes of applying pressure. The patient is otherwise healthy and has been meeting all developmental milestones. The family history is significant for a grandfather and an uncle who had excessive bleeding tendencies. Which of the following is the most likely cause of this patient’s symptoms?
A 55-year-old man presents to his primary care physician for leg pain. The patient works as a mailman but states he has had difficulty completing his deliveries for the past month. He complains of a burning and tingling pain in his legs when he walks that goes away when he sits down and takes a break. The patient has a past medical history of obesity, diabetes, stable angina, and constipation. His current medications include insulin and metformin. The patient has a 22-pack-year smoking history and he drinks 2-3 alcoholic beverages per day. Physical exam reveals a stout man with a ruddy complexion. His gait is stable and he demonstrates 5/5 strength in his upper and lower extremities. Which of the following is the best next step in management?
A 39-year-old woman comes to the physician for worsening fatigue and dyspnea for several months. She has not been seen by a physician in 10 years. She is also concerned about the appearance of her fingernails. A photograph of her hands is shown. Which of the following is the most likely underlying cause for the patient's nail findings?
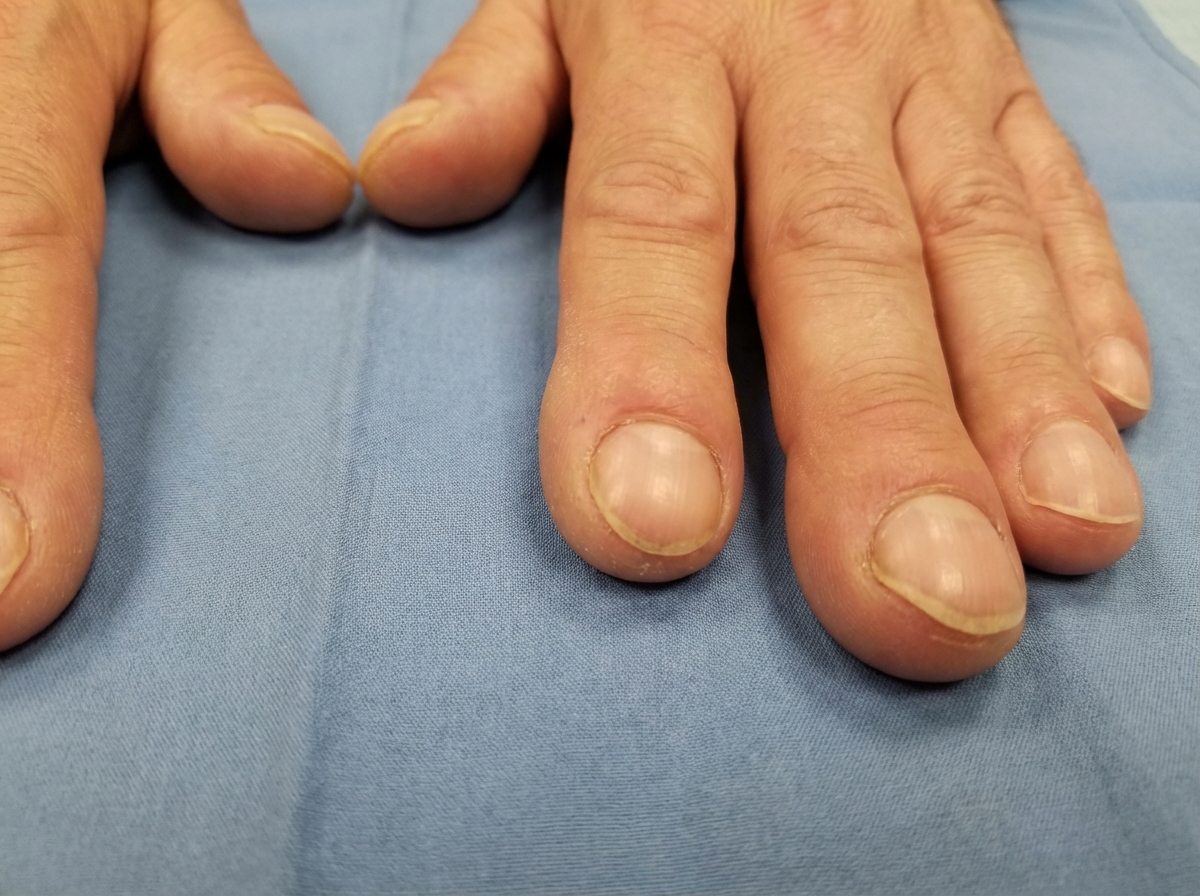
A 58-year-old woman with a history of rheumatic fever has been experiencing exertional fatigue and dyspnea. She has begun using several pillows at night to sleep and occasionally wakes up at night gasping for air. On exam, she appears dyspneic and thin. Cardiac exam reveals a loud S1, opening snap, and apical diastolic rumble. Which of the following is the strongest predictor of the severity of her cardiac problem?
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
