Cardiology — MCQs

On this page
Which of the following flow recording is shown below?
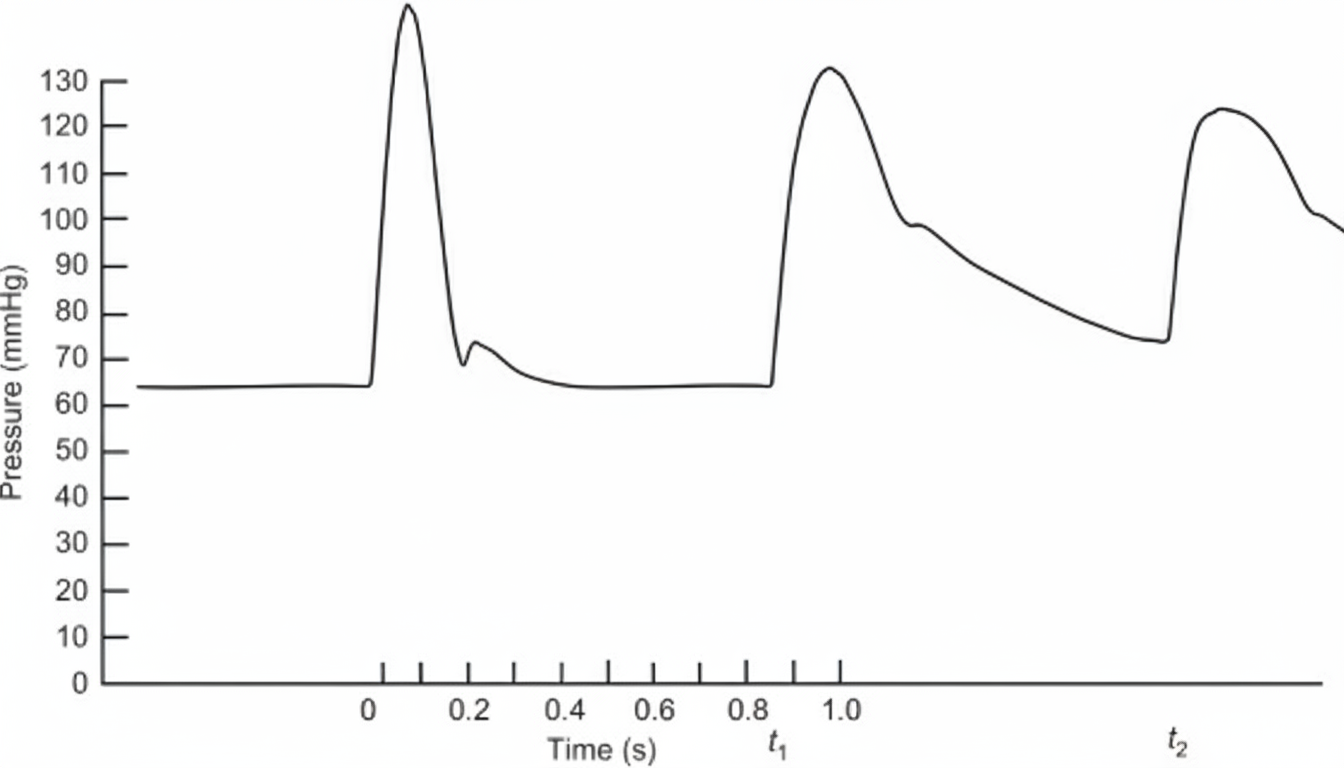
A hypokalemic patient develops syncope with hypotension in ICU. Name the ECG abnormality with preferred drug to be used. (Recent NEET Pattern 2016-17)
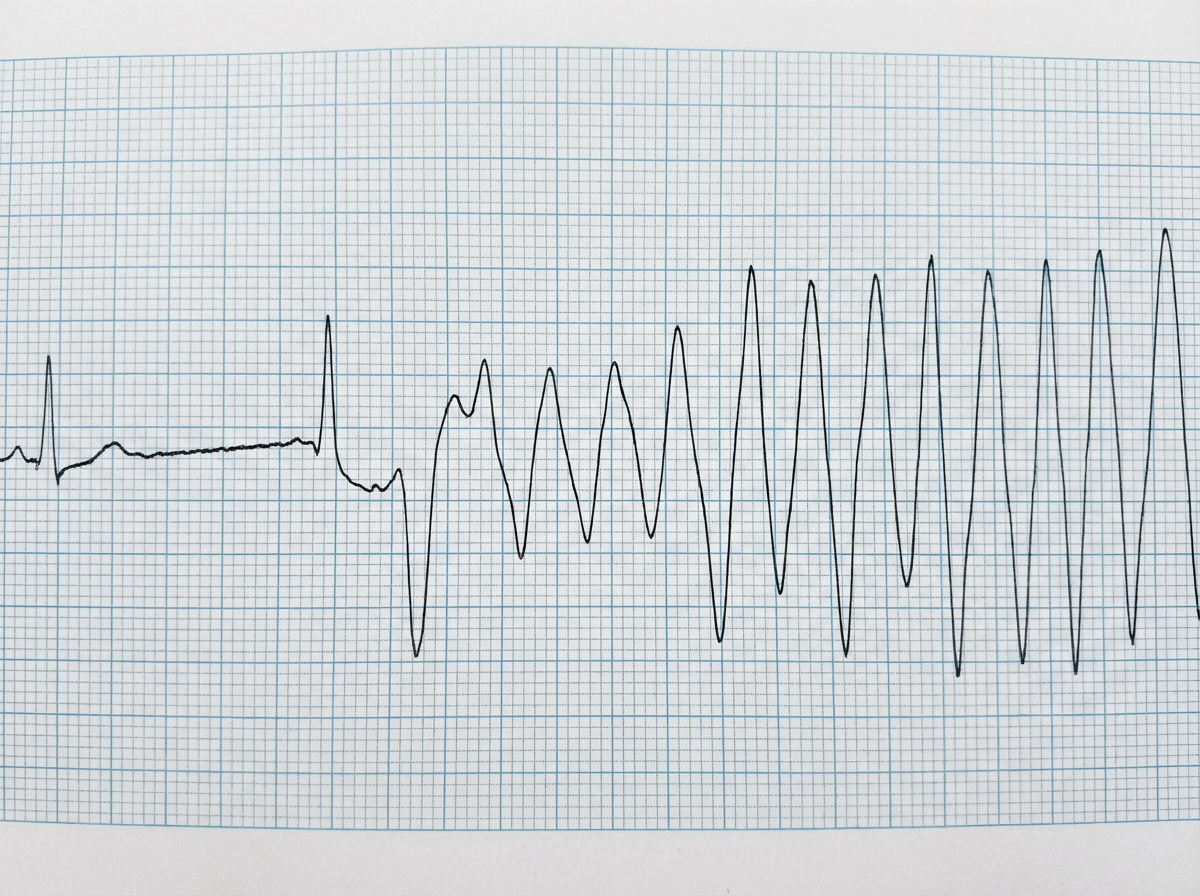
The ECG shows presence of ST elevation from V2-V5. What is the diagnosis?
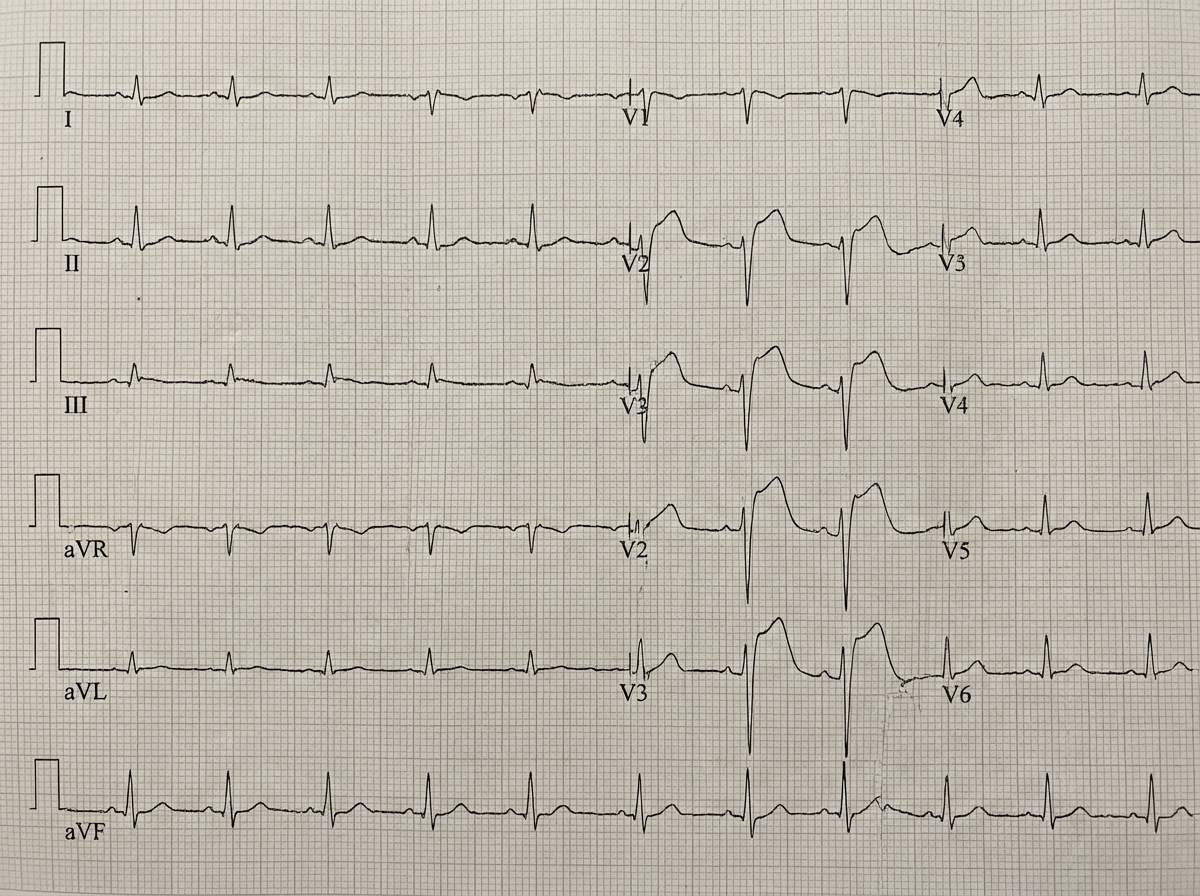
In a patient with the ECG shown below, which drug is not to be given?
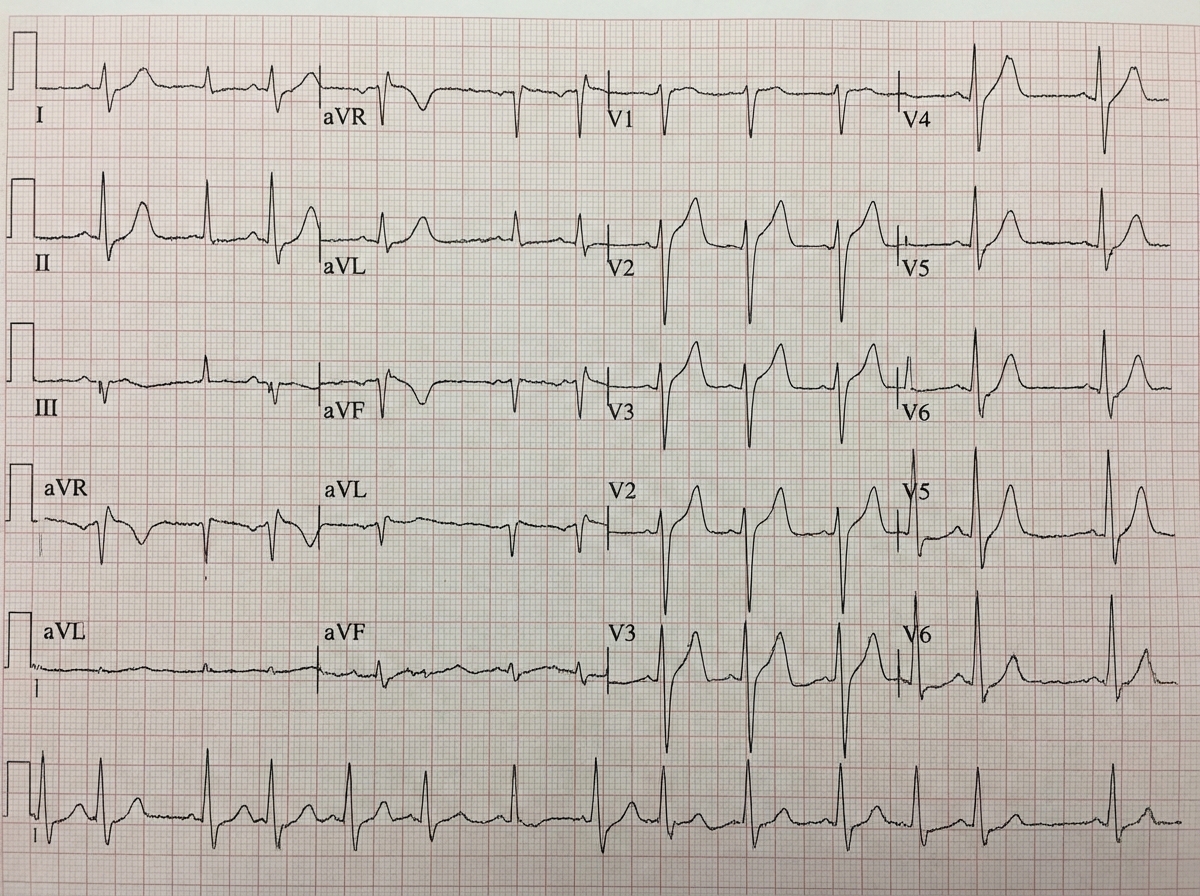
Identify the condition shown in the ECG given below.
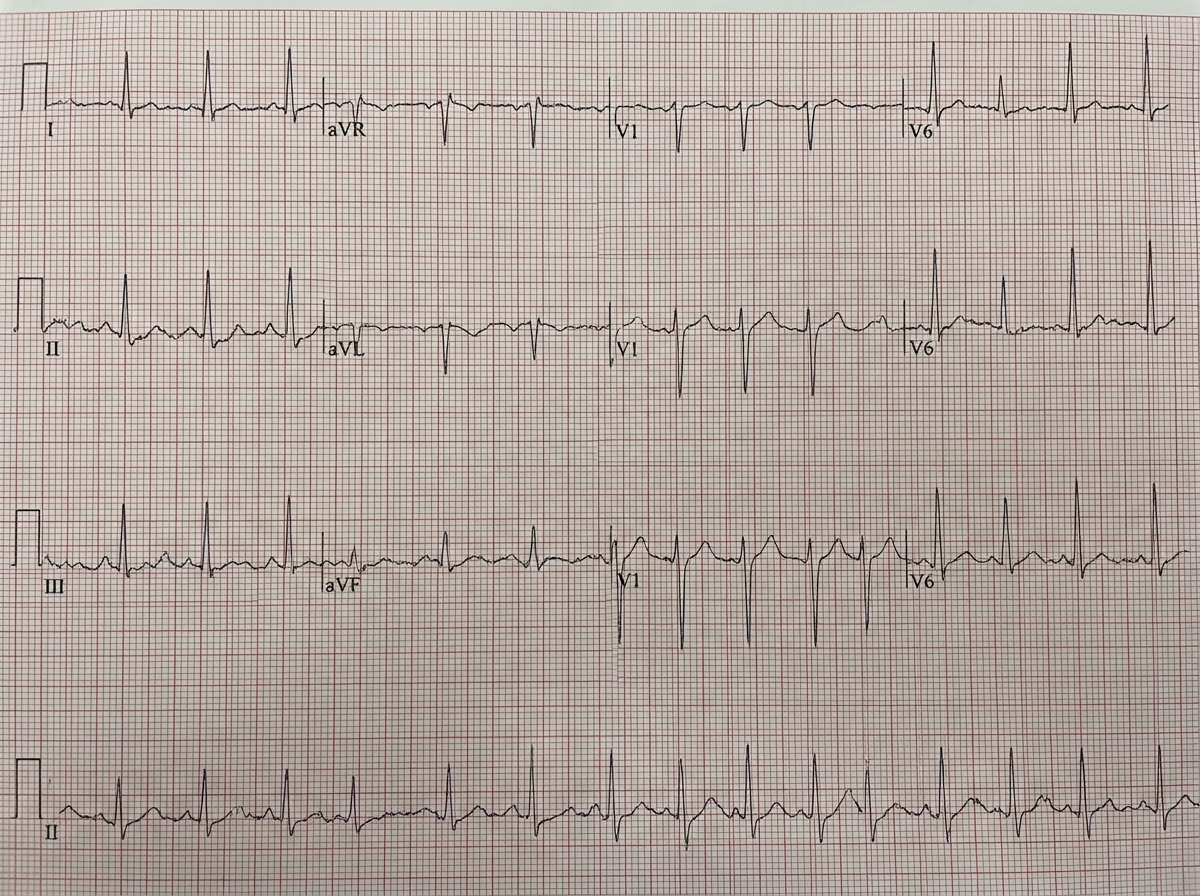
A 65-year-old elderly male with the ECG shown below has a history of sweating and chest pain for the last 24 hrs . Which of the following is not given in managing the patient?
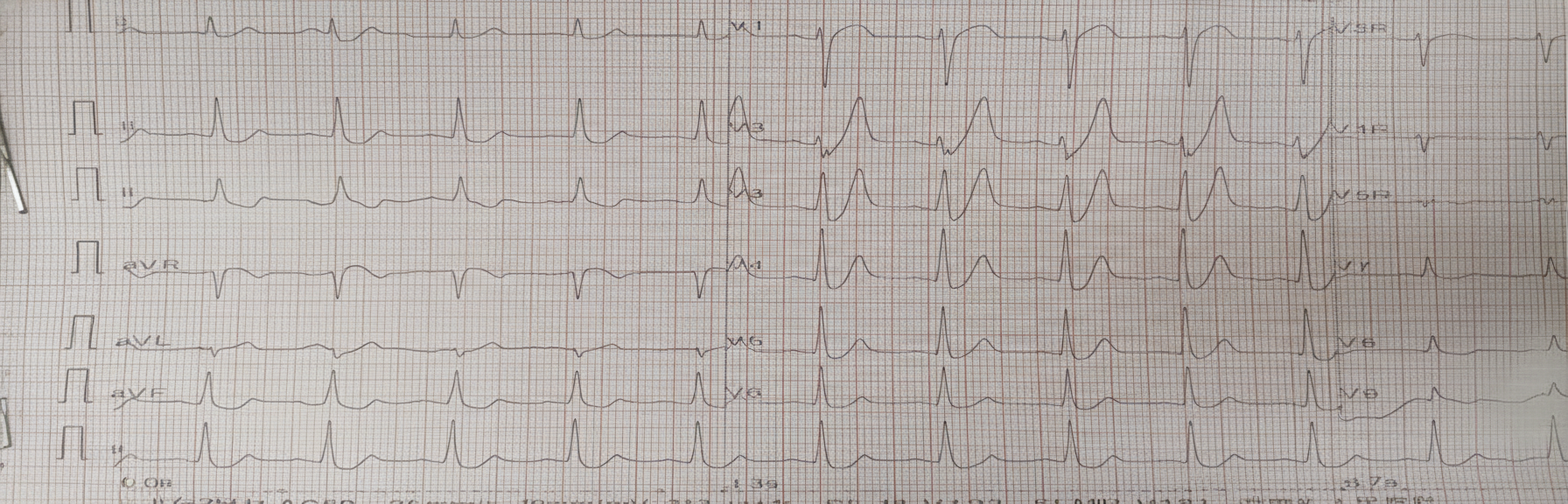
A 52-year-old diabetic patient complains of palpitations. His ECG is given below. The first line of management is:
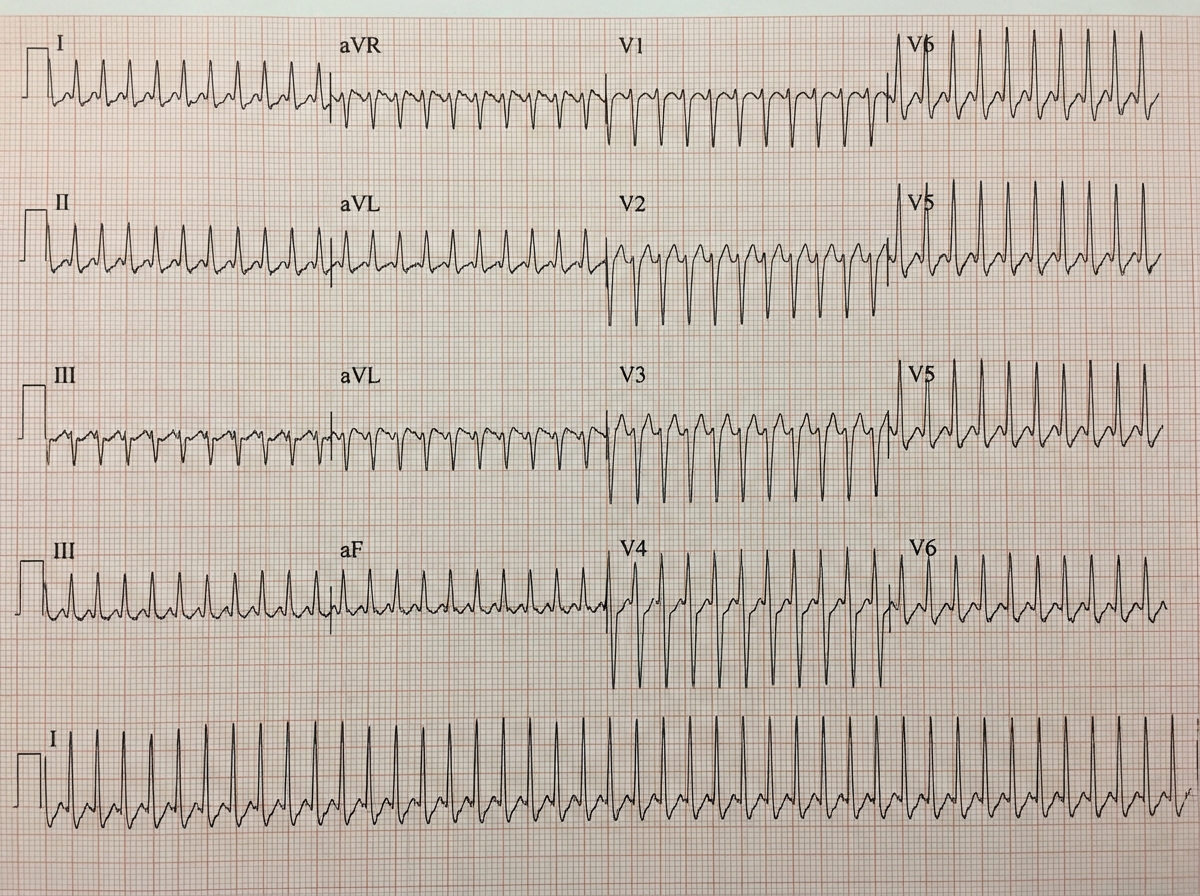
A 76-year-old male came to emergency department with complaints of retrosternal pain for 6 hours. The following is the ECG of the same patient. What is the appropriate next line of management of this patient? (AIIMS May 2016)
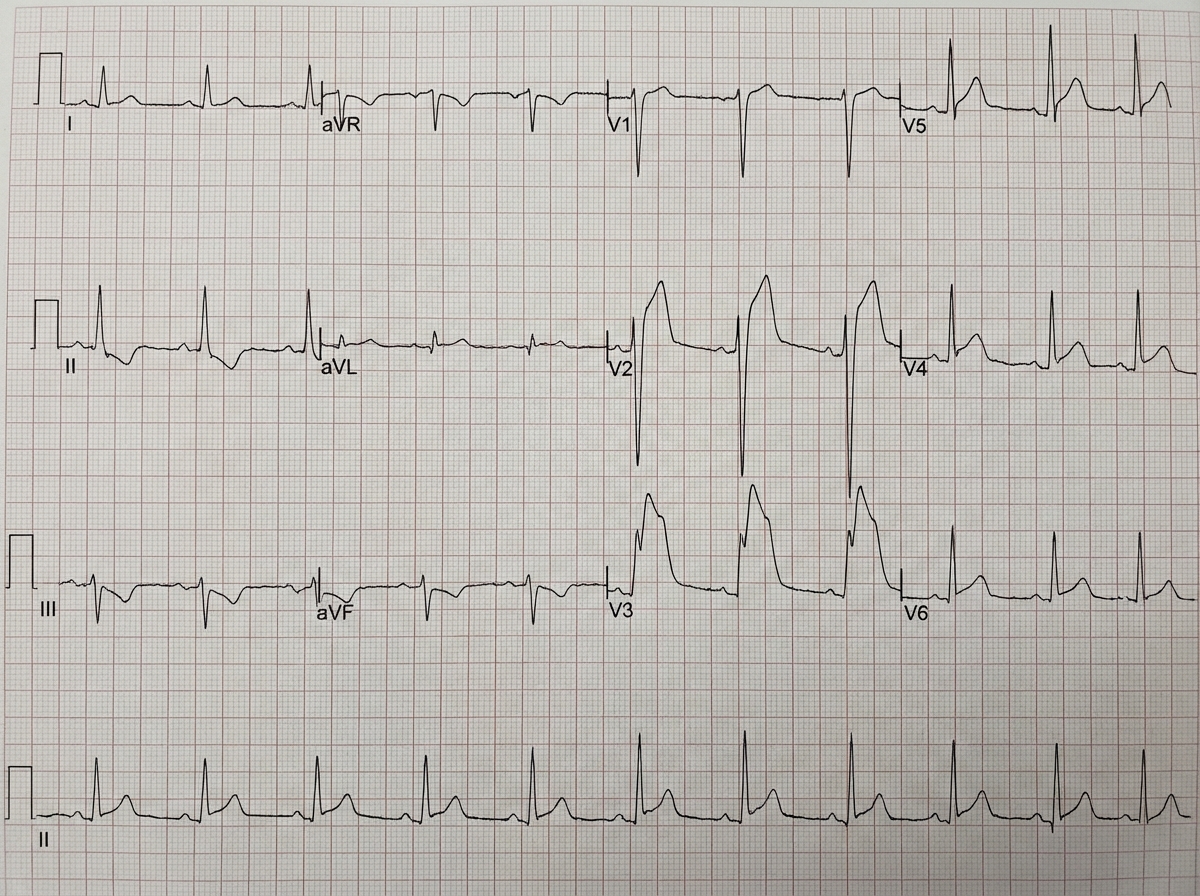
A 16-year-old boy has a history of recurrent episodes of fainting in school assembly. ECG was done. Which is incorrect about the condition?
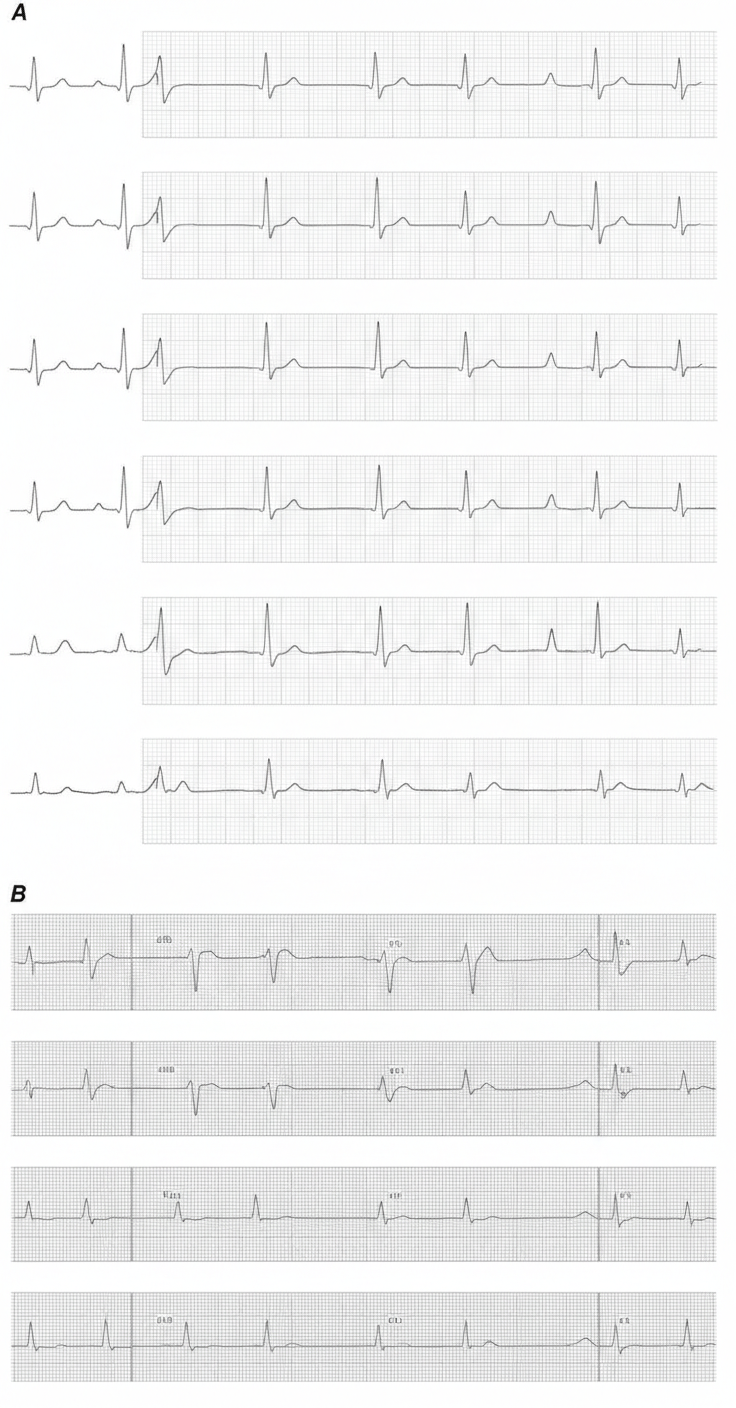
A 65-year-old man presents with crushing chest pain for 2 hours. On examination, BP = 80/60 mm Hg and JVP is elevated 4 cm above the sternal angle. All are true about the condition shown except:
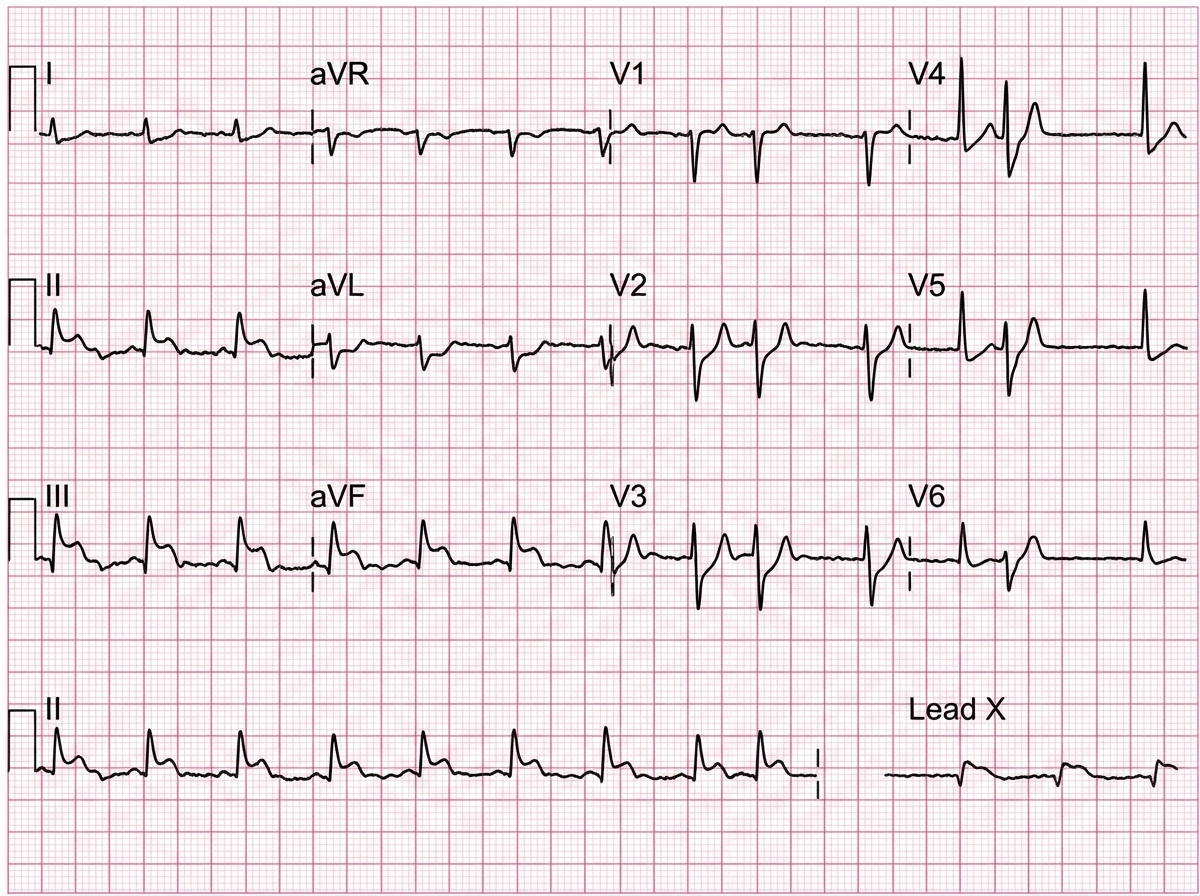
Practice by Chapter
Hypertension diagnosis and management
Practice Questions
Stable coronary artery disease
Practice Questions
Peripheral arterial disease
Practice Questions
Aortic diseases
Practice Questions
Valvular heart disease
Practice Questions
Pericardial diseases
Practice Questions
Adult congenital heart disease
Practice Questions
Cardiac tumors
Practice Questions
Cardiac manifestations of systemic diseases
Practice Questions
Pre-operative cardiac risk assessment
Practice Questions
Cardiac imaging modalities
Practice Questions
Preventive cardiology
Practice Questions
Cardiac rehabilitation
Practice Questions
Want unlimited practice?
Get full access to all questions, explanations, and performance tracking.
Scan to download app
